Traumatic Experiences: Vagus Nerve, Microbiome, Heart Rate Variability (HRV) and Effects of Exercise
Original Editor - Andrea Sturm
Top Contributors - Vidya Acharya, Kim Jackson, Jess Bell, Tarina van der Stockt and Lucinda hampton
The Brain-Gut-Microbiome Axis[edit | edit source]
Biological psychiatry research has long focused on the brain in elucidating the neurobiological mechanisms of anxiety- and trauma-related disorders. However, it has been found that the gut microbiome and its interactome also deserve attention to understand brain disorders and develop innovative treatments and diagnostics in the 21st century. The recent, in-depth characterisation of the human microbiome spurred a paradigm shift in human health and disease. Animal models strongly suggest a role for the gut microbiome in anxiety- and trauma-related disorders. The microbiota–gut–brain (MGB) axis sits at the epicenter of this new approach to mental health. The microbiome plays an important role in the programming of the hypothalamic–pituitary–adrenal (HPA) axis early in life, and stress reactivity over the life span.[1]
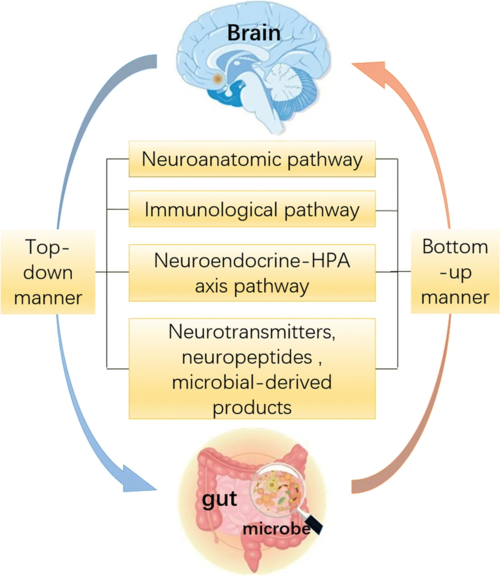
It has been found that there are bidirectional interactions within the brain-gut-microbiome axis.[2][3][4] Gut microbes communicate to the central nervous system through at least 3 parallel and interacting channels involving nervous, endocrine, and immune signalling mechanisms. The brain can affect the community structure and function of the gut microbiota through the autonomic nervous system, by modulating regional gut motility, intestinal transit and secretion, and gut permeability, and potentially through the luminal secretion of hormones that directly modulate microbial gene expression.[5]
A system biological model is proposed that posits circular communication loops amid the brain, gut, and gut microbiome, and in which perturbation at any level can propagate dysregulation throughout the circuit. A series of largely preclinical observations implicate alterations in brain-gut-microbiome communication in the pathogenesis and pathophysiology of irritable bowel syndrome, obesity, and several psychiatric and neurologic disorders. Continued research holds the promise of identifying novel therapeutic targets and developing treatment strategies to address some of the most debilitating, costly, and poorly understood diseases.[5]
The Microbiome in Posttraumatic Stress Disorder[edit | edit source]
Research has explored the relationship of exaggerated inflammatory responses in the development of Post Traumatic Stress Disorder (PTSD).[8][9] Hemmings et al.[8] found that regulatory T cells (Tregs) are altered in individuals with PTSD. Tregs are a subset of CD4+ T cells and are involved in regulating/suppressing cells in the immune system.[8]
- In laboratory conditions, individuals exposed to a stressor have reduced levels of Treg cells.
- Both male and female refugees diagnosed with chronic PTSD show a similar reduction in Treg levels when compared to healthy controls.
- Reduced Treg levels are also associated with autoimmune diseases such as thyroiditis, inflammatory bowel disease, and rheumatoid arthritis.
- Individuals with PTSD have an increased risk for these conditions.[8]
- In addition to this, genome-wide association studies in PTSD cohorts have found an association with ANKRD5.
- ANKRD5 is associated with various autoimmune and inflammatory disorders, including multiple sclerosis, type 2 diabetes mellitus, coeliacs disease, and rheumatoid arthritis.[8]
It is interesting to note that a link between childhood trauma and multiple sclerosis (MS) has also been investigated. A cross-sectional case-control study compared histories of child abuse and neglect between patients with MS and healthy adults.[10]
- 234 patients with MS and 885 healthy adults completed the self-reported Childhood Trauma Questionnaire to assess emotional, physical, and sexual abuse and emotional and physical neglect.
- Patients with MS scored significantly higher in all Childhood Trauma Questionnaire subscales apart from physical abuse and neglect than the control group from the general population.
- Adjusted odds ratios for these types of childhood trauma were higher in the MS group than in controls
- These levels ranged from 2.0 for emotional neglect (95% confidence interval = 1.3-3.2) to 3.4 for emotional abuse (95% confidence interval = 2.0-5.7).[10]
- Childhood trauma was not associated with the degree of disability. However, MS patients who reported a history of physical and/or sexual abuse had significantly higher relapse rates compared with MS patients who did not report such abuse.[10]
A study by Jergovic et al. found an altered Treg phenotype in male combat veterans with PTSD compared to healthy controls.[8]
- PTSD results in up-regulation of interleukin (IL) 6 and proinflammatory cytokines (including interferon gamma (IFN-γ), IL-1β and tumor necrosis factor (TNF).
- Individuals with PTSD have been observed to have elevated levels of C-reactive protein (CRP)
- Pre-existing elevated CRP levels or elevated IL-6 levels (measured within 24 hours of a traumatic event) was found to predict:
- post-deployment CAPS scores in marines
- a diagnosis of PTSD in children six months following trauma[8]
The Human Microbiome[edit | edit source]
The human microbiome is an important factor determining immunoregulation (indicated by a balanced expansion of effector T cell populations and Tregs).[8]
The human microbiota consists of all microorganisms hosted in the human body, including archaea, bacteria, eukaryotes, fungi, and viruses. The human microbiome is made up of all the microbial symbionts and their genes.[8] While humans "share a core intestinal microbiome" the "human microbiome differs by genes, species, enterotypes (ecology), and gene count (microbial diversity)."[11]
- Microbial inputs have been found to be a key factor in maintaining homeostasis and optimum health. They help to:
- Control the blood-brain barrier permeability
- Regulate CNS function.[8]
A bidirectional system of communication exists between the gut microbiome, the gut, and the CNS.[8] Environmental and gut microbial species affect cognition, memory, and fundamental behaviours, such as social interactions and the ability to cope with stress.
Stress can also affect the composition of the gut microbiota; the bidirectional communication between microbiota and the CNS, thus, influences stress reactivity. Alterations in microbiota can alter plasticity-related, serotonergic, and GABAergic signalling systems in the CNS. Thus, any dysregulation of the gut microbiome (known as dysbiosis) could alter an individual’s risk of developing a disease. These could include stress or trauma related conditions.[8]
Exploring the gut microbiota in inpatients with bipolar disorder during a depressive episode[edit | edit source]
Bipolar affective disorder (BD) is one of the top 10 causes of global disability and premature mortality, as well as having a significant socioeconomic impact. BD causes structural brain changes, disturbances in neuroplasticity, as well as chronobiology.[12]
The pathophysiological causes of BD are both genetic and environmental. These include:
- defects in apoptotic, immune‐inflammatory, neurotransmitter, neurotrophin and calcium signalling pathways
- alterations in oxidative and nitrosative stress
- cellular bioenergetics, and membrane or vesicular transport.[12]
Studying the relationship between gut microbiota and BD is a relatively new field of research.[12] Thus, the communication pathways between the microbiota and the brain are not yet fully mapped out. Studying these systems is made more challenging by the fact that the microbial community is ever changing. Moreover, it can be easily modified by external factors including diet and exercise.[12] While it is becoming clear in the research that there is a relationship between diet, the gut microbiota, host immunity and host metabolism, the relationship between exercise and the microbiota has yet to be studied in detail.[12]
What does the current research show?[edit | edit source]
A combination of exercise and diet impacts on gut microbial diversity. In particular, enhanced diversity of the microbiota is correlated with exercise and dietary protein consumption. Diversity is important as it helps to promote stability and performance in all ecosystems.[13]
Considering the psychiatric perspective[edit | edit source]
Research that explores the association between neurotransmitters and gut microbiota has demonstrated that most human neurotransmitters can be produced by gut bacteria:[12]
- Lactobacillus species produce acetylcholine and GABA;
- Bifidobacterium species synthesise GABA;
- Escherichia produces noradrenaline, 5‐HT and dopamine;
- Streptococcus and Enterococcus synthesise 5‐HT
- Bacillus species produce dopamine and noradrenaline.[12]
As well as changes KYN pathway metabolites, TRP (a 5‐HT precursor) is altered in BD. Psychopharmacological agents such as antidepressants and lithium have antibiotic properties, which could affect the gut microbiota.[12] Individuals with BD often have co-morbidities such as inflammatory diseases and obesity - it is possible that the complex interactions between these factors could cause changes in the gut microbiota in BD patients.[12]
Thus, it can be concluded that:
- metabolic syndrome and low-grade inflammation are important characteristics of BD and these may be affected by the gut microbiota.
- BD may not simply be an affective disorder, but could also be understood in the context of gut-brain axis dysfunction.[12]
Trauma and mental disorder[edit | edit source]
Being exposed to potentially traumatic events (PTEs) increases the risk of developing a mental disorder.[14]
- Repeated exposure to PTEs (eg in conflict zones) is a strong predictor of PTSD, depression and anger/Intermittent Explosive Disorder (IED). This association is known as the dose-effect relationship.
- Longitudinal studies amongst veterans and groups exposed to trauma have shown that post-traumatic stress symptoms following PTE exposure may precede/contribute to the onset of depression and other anxiety disorders.[14]
Trauma, Heart Rate Variability (HRV) and the Vagus Nerve[edit | edit source]
Reduced heart rate variability (HRV) is a potential psychophysiological marker to various affective responses following trauma as it reflects altered vagal nerve function and impaired emotion regulation capacity.[14]
HRV measures parasympathetic regulation of heart rate via the inhibitory influence of the vagus nerve over the sinoatrial node. Under conditions of safety, the heart rate is slowed, and social engagement is facilitated. In response to an external cue (eg a threat signal), inhibition from the vagal nerve ends, which allows the sympathetic nervous system to dominate and begin defence responses. Ongoing exposure to threat (eg in conflict) may have a long term impact on the functioning of the vagal system, reducing an individual’s ability to adapt to stressful events.[14]
It has been suggested that a higher level of resting-state HRV may be a central indicator of healthy emotion regulation capacity - ie a system that is able to respond effectively to environmental challenges.[14] A healthy vagal system is believed to index:
- psychological flexibility
- emotional self-regulation
- and positive adaptation.[14]
Alternatively, low resting state HRV is an indicator of psychophysiological rigidity - ie decreased capacity for regulating emotional responses to distressing events.[14] Reduced resting HRV has been linked to:
- greater trauma exposure
- mental disorder/symptoms
- physical health status (PTSD; depression and anxiety; aggression and anger; comorbidity, and poor physical health)
- increased vulnerability to distress
- delayed physiological recovery after stress exposure.[14]
Improvements in heart rate variability with exercise therapy[edit | edit source]
As a measure of autonomic nervous system function, HRV is beneficial as it is: noninvasive, practical, and reproducible.[16]
While having a variable and responsive heart rate confers a survival advantage, reduced HRV may be associated with poorer cardiovascular health and outcomes.[16]
The prognostic implications of HRV have been studied in various clinical populations. This research has found that reduced HRV has prognostic significance for people with myocardial infarction, chronic heart failure, unstable angina, and diabetes mellitus.[16]
Interventions designed to increase HRV, such as exercise therapy, have also been explored.[16] The results have been promising in this area. It appears that exercise therapy may improve HRV in myocardial infarction, chronic heart failure, and revascularisation patients by increasing vagal tone and reducing sympathetic activity. It has been theorised that a shift toward greater vagal modulation may have a positive effect on the prognosis of these patients.[16] It is not yet clear how exercise training improves vagal modulation, but angiotensin II and nitric oxide are possible mediators.[16]
Potential mechanism in the modification of HRV by exercise therapy[edit | edit source]
It has been suggested that enhancing cardiac vagal tone may be beneficial for survival. Greater vagal influence results in a reduced oxygen consumption and decreased cardiac work load - due to a reduction in resting heart rate and myocardial contractility. Stimulation of the vagus nerve appears to act directly on the sinus node and the myocardium, and limits sympathetic involvement. Cardiac vagal tone may also reduce the risk of dangerous ventricular dysrhythmias including ventricular fibrillation.[16]
Exercise training may enhance vagal tone. It’s not yet clear how exercise training improves vagal modulation, but angiotensin II and nitric oxide (NO) are potential mediators.[16]
- Angiotensin II inhibits cardiac vagal activity and it has been theorised that exercise training suppresses angiotensin II expression.[16]
- It has also been found that plasma renin activity levels are lower in athletes (long-distance runners) than in untrained individuals/nonathletes/sedentary individuals. This is important because athletes who have lower plasma renin activity would, in theory, have lower angiotensin II and, thus, higher associated levels of cardiac vagal activity.
- In summary, it may be that the suppression of angiotensin II via exercise could mediate the enhancement of cardiac vagal tone.[16]
- NO may also be involved in increasing cardiac vagal control and, as a result, indirectly inhibit sympathetic influences.[16]
- Exercise training improves endothelial function and NO bioavailability among individuals with coronary risk or coronary atherosclerosis.
- It is therefore possible that the relationship between exercise and cardiac vagal activity is affected to some degree by NO.
- More research is still needed to determine the potential role of NO in autonomic control as well as possible influence on the relationship between exercise and cardiac vagal tone.[16]
Some research exists to suggest that exercise training (particularly endurance training) can increase cardiac vagal tone and reduce sympathetic cardiac influences.[16]
- Improvements in HRV occur in Myocardial Infarct (MI) patients who participate in unsupervised low-intensity walking programs as well as more intensive supervised exercise programs.[16]
- MI patients who participated in a two-week exercise program (consisting of two 30 min daily sessions of cycle ergometry at the anaerobic threshold) had faster parasympathetic nervous system activity recovery than patients who participating in a walking cardiac rehabilitation program.[16]
- However, the exact mechanisms leading to changes in HRV by exercise therapy are not yet known.[16]
The ANS and stress[edit | edit source]
The ANS is highly adaptable. It enables individuals to maintain balance during stressful events. However, when the system lacks flexibility, various somatic and psychological pathologies can develop. A number of studies have found a link between reduced HRV in post-myocardial infarction patients and increased risk for adverse cardiovascular events (such as ventricular arrhythmias and sudden death).[17] More recent research has found that patients with depression and anxiety disorders have abnormally low HRV when compared with non-psychiatric controls.[17] Reduced HRV appears to indicate the decreased cardiac vagal tone and elevated sympathetic activity in anxious and depressive patients and would reflect a lack of flexibility of emotional physiological mechanisms.[17]
References[edit | edit source]
- ↑ Martin CR, Osadchiy V, Kalani A, Mayer EA. The brain-gut-microbiome axis. Cellular and molecular gastroenterology and hepatology. 2018 Jan 1;6(2):133-48.
- ↑ Margolis KG, Cryan JF, Mayer EA. The microbiota-gut-brain axis: from motility to mood. Gastroenterology. 2021 Apr;160(5):1486-1501.
- ↑ Chudzik A, Orzyłowska A, Rola R, Stanisz GJ. Probiotics, prebiotics and postbiotics on mitigation of depression symptoms: modulation of the brain-gut-microbiome axis. Biomolecules. 2021 Jul 7;11(7):1000.
- ↑ Person H, Keefer L. Psychological comorbidity in gastrointestinal diseases: Update on the brain-gut-microbiome axis. Prog Neuropsychopharmacol Biol Psychiatry. 2021 Apr 20;107:110209.
- ↑ 5.0 5.1 Malan-Muller S, Valles-Colomer M, Raes J, Lowry CA, Seedat S, Hemmings SM. The gut microbiome and mental health: implications for anxiety-and trauma-related disorders. Omics: a journal of integrative biology. 2018 Feb 1;22(2):90-107.
- ↑ DavidPerlmutterMD Gut Bacteria Change Your Brain Available from https://www.youtube.com/watch?v=RXh4u03lM3w Accessed on 28/09/19
- ↑ Zhao L, Xiong Q, Stary CM, Mahgoub OK, Ye Y, Gu L, Xiong X, Zhu S. Bidirectional gut-brain-microbiota axis as a potential link between inflammatory bowel disease and ischemic stroke. Journal of neuroinflammation. 2018 Dec;15(1):339.
- ↑ 8.00 8.01 8.02 8.03 8.04 8.05 8.06 8.07 8.08 8.09 8.10 8.11 Hemmings SM, Malan-Muller S, van den Heuvel LL, Demmitt BA, Stanislawski MA, Smith DG, Bohr AD, Stamper CE, Hyde ER, Morton JT, Marotz CA. The microbiome in posttraumatic stress disorder and trauma-exposed controls: an exploratory study. Psychosomatic medicine. 2017 Oct;79(8):936.
- ↑ Brenner LA, Stearns-Yoder KA, Stamper CE, Hoisington AJ, Brostow DP, Hoffmire CA, et al. Rationale, design, and methods: A randomized placebo-controlled trial of an immunomodulatory probiotic intervention for Veterans with PTSD. Contemp Clin Trials Commun. 2022 Jun 28;28:100960.
- ↑ 10.0 10.1 10.2 Spitzer C, Bouchain M, Winkler LY, Wingenfeld K, Gold SM, Grabe HJ, Barnow S, Otte C, Heesen C. Childhood trauma in multiple sclerosis: a case-control study. Psychosomatic medicine. 2012 Apr 1;74(3):312-8.
- ↑ Malard F, Dore J, Gaugler B, Mohty M. Introduction to host microbiome symbiosis in health and disease. Mucosal Immunol. 2021 May;14(3):547-54.
- ↑ 12.0 12.1 12.2 12.3 12.4 12.5 12.6 12.7 12.8 12.9 Painold A, Mörkl S, Kashofer K, Halwachs B, Dalkner N, Bengesser S, Birner A, Fellendorf F, Platzer M, Queissner R, Schütze G. A step ahead: Exploring the gut microbiota in inpatients with bipolar disorder during a depressive episode. Bipolar disorders. 2019 Feb;21(1):40-9.
- ↑ Clarke SF, Murphy EF, O'Sullivan O, Lucey AJ, Humphreys M, Hogan A, Hayes P, O'Reilly M, Jeffery IB, Wood-Martin R, Kerins DM. Exercise and associated dietary extremes impact on gut microbial diversity. Gut. 2014 Dec 1;63(12):1913-20.
- ↑ 14.0 14.1 14.2 14.3 14.4 14.5 14.6 14.7 Liddell BJ, Kemp AH, Steel Z, Nickerson A, Bryant RA, Tam N, Tay AK, Silove D. Heart rate variability and the relationship between trauma exposure age, and psychopathology in a post-conflict setting. BMC psychiatry. 2016 Dec;16(1):133.
- ↑ Owen Epstein Heart rate variability Available from https://www.youtube.com/watch?v=B6Id6Jl7_HU Accessed on 28/09/19
- ↑ 16.00 16.01 16.02 16.03 16.04 16.05 16.06 16.07 16.08 16.09 16.10 16.11 16.12 16.13 16.14 16.15 Routledge FS, Campbell TS, McFetridge-Durdle JA, Bacon SL. Improvements in heart rate variability with exercise therapy. Canadian Journal of Cardiology. 2010 Jun 1;26(6):303-12.
- ↑ 17.0 17.1 17.2 Servant D, Logier R, Mouster Y, Goudemand M. Heart rate variability. Applications in psychiatry. L'Encephale. 2009 Oct;35(5):423-8.






