Traumatic Paraplegia
Original Editor - Wouter Claesen
Top Contributors - Wouter Claesen, Vanessa Rhule, Blessed Denzel Vhudzijena, Evan Thomas, Naomi O'Reilly, Lucinda hampton, 127.0.0.1, Admin, Wendy Walker, WikiSysop and Kim Jackson
Definition/Description[edit | edit source]
Traumatic paraplegia is caused by a lesion of the spinal cord (SCI) which occurs after a trauma, e.g. vertebral fracture causing a puncture to the spinal cord. The most common causes of SCI in the world are traffic accidents, gunshot injuries, knife injuries, falls and sports injuries. There is a strong relationship between functional status and whether the injury is complete or not complete, as well as the level of the injury. The results of SCI bring damage to independence and physical function and many complications from the injury eg. Neurogenic bladder and bowel, urinary tract infections, pressure ulcers, orthostatic hypotension, fractures, deep vein thrombosis, spasticity, autonomic dysreflexia, pulmonary and cardiovascular problems, and depressive disorders. SCI leads to serious disability in the patient resulting in the loss of work, which brings psychosocial and economic problems.[1]
The treatment and rehabilitation period is long, expensive and exhausting in SCI. Whether complete or incomplete, SCI rehabilitation is a long process requiring patience and motivation of both patient and relatives. Early rehabilitation is important to prevent joint contractures and the loss of muscle strength, conservation of bone density, and to ensure normal functioning of the respiratory and digestive system[1].
An interdisciplinary approach is essential in rehabilitation in SCI, as in the other types of rehabilitation. The team includes the treating doctor, patient and family, physiotherapist, occupational therapist, dietician, psychologist, speech therapist, social worker and other consultant specialists as necessary.
Clinically Relevant Anatomy[edit | edit source]
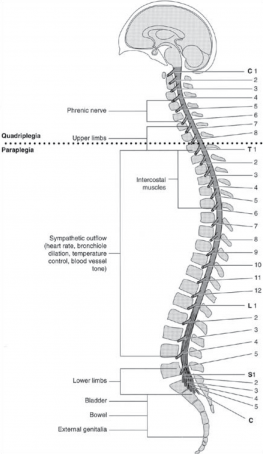
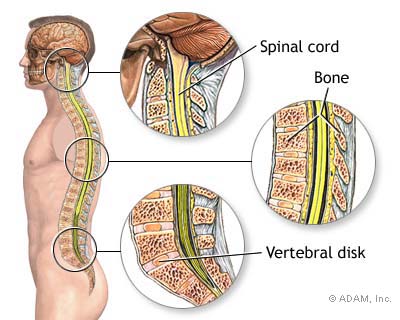
The spinal cord is connected to the brain, where it descends down the middle of the back, surrounded and protected by the bony vertebral column. The spinal cord is surrounded by Cerebral Spinal Fluid (CSF). Its function is to prevent the delicate nerve tissue from the inside of the vertebrae. The spinal cord itself consists of millions of nerve fibers which transmit electrical information to and from the limbs, trunk and organs of the body, to and from the brain. The Central Nervous System (CNS) consists of the brain and spinal cord. The nerves connecting the spinal cord to the body is called the Peripheral Nervous System (PNS).
Epidemiology/Etiology[edit | edit source]
The cause of paraplegia due to a spinal cord injury is most often by a car accident. It can also result from a firearm injury, which is not the case in many countries in the world. Traumatic paraplegia is most prominent in young men between the ages of 21 and 35 years. The more reckless way of driving within the younger population could also be one of the reasons.
This injury has a major effect on the social life of the patient, such as divorce or loss of work. Therefore, it might be important as a physiotherapist to talk with the patient about considering professional psychological help and assist in guiding him/her through this process.
Physical Therapy Management[edit | edit source]
From the very beginning, all efforts should be concentrated on the rehabilitation of the patient.An accurate assessment of the patient is needed so as to be able to institute the appropriate treatment plan. The physiotherapy management of the patient starts from the day patient is admitted in hospital. The management can be discussed under the Acute stage and the Chronic stage:
A. ACUTE STAGE MANAGEMENT: -
The aims of treatment include: -
- avoiding chest complications
- further injury to the spine
- maintaining range of movement
Goal setting:- Realistic goals should be agreed upon with the patient and the relatives and the therapist – compromises should be agreed upon.
Chest Physiotherapy:- Will mainly prophylactic at this stage and depends on the level of injury. If prophylactic involves deep breathing exercises to maintain tidal volume and avoid atelectasis. The higher the level of injury the greater the risk of chest infections due to reduced chest mobility. Reduced vital capacity can lead to atelectasis and infections. This can be prevented by teaching the patient deep breathing exercises, assisted coughing and huffing, and doing percussions to mobilise secretions. If on a ventilator, suctioning together with vibrations and percussions can be done.
Proper turning to patients:- will help prevent further spinal cord damage together with prevention of pressure sores
Proper positioning:- is essential to prevent further patient injury, to prevent spinal deformities, prevent pressure sores, prevent contractures
Active assisted exercises:- to facilitate recovery of affected muscle groups and also to maintain range of movement in the partially involved muscles. To maintain and increase muscle strength in the partially involved muscle groups.[5]
Passive movements:- to prevent contractures and should be assisted where applicable. Precautions with passive movements:-
- avoid extreme range of movement – the joints are paretic
- hip flexion to be done with knee flexion – avoid lumbar or lower thoracic movement if lesion low.
- Avoid straight leg raising – stretches damaged neural tissue.
- Do not give combined wrist and finger flexion – trauma to the extensor tendons.
Counseling and psychological support:- can be given to the patient with lots of input from the psychologist and or the social worker. Relatives should be included as well.
B. SUBACUTE TO CHRONIC STAGE PHYSIOTHERAPY MANAGEMENT:-
Bed mobility:- This involves teaching the patient how to roll , come from lying to sitting and vice-versa, bridge and relieve pressure when in bed
Outside bed mobility:- Involves teaching the patient sitting balance, standing and standing balance, walking where applicable.
Wheelchair use and selection:- Is done with help of the Occupational Therapists – involves teaching the patient transfers from wheel chair to bed, toilet seat, car, bathroom and also to floor. Wheelchair maneuvering is also taught for e.g. ramps and kerbs. The Occupational Therapists also teaches a lot of ADLs with the patient in a wheelchair in preparation for discharge. Pressure care is also included.
Continue with Chest physiotherapy as in acute stage.
Aid selection and use training:- If they are a low level paraplegia and will be able to walk with the use of calipers or orthosis, they will be helped with the selection and training on the use of the aid. Backslabs/callipers can also be used to help with walking and standing.
Standing:- can be done using a tilt-table at first and then move to backslabs and other devices.
Muscle strengthening:- As is appropriate - to try and compensate for the affected muscle groups and to strengthen those with partial innervation.[6]
Home adjustments:-usually done with the help of the Occupational Therapists. A home assessment will have to be done and advice on the necessary changes and adjustments to be undertaken given before the patient is discharged from hospital.
Sexual education:- Emphasis should be on the utilisation of the areas still with sensation to get sexual gratification. Clinician can also suggest the use of other assistive devices e.g. sex toys
Social services;- Will be needed to help with processing of pension etc. and also social support to the patient and family. Psychological support from the Psychologist will be required throughout the rehabilitation process until the patient and relatives have accepted the disability.
Vocational training and job placement:- Can be done with help of Physios, OTs and the Social Worker.
Follow-up – at home or during workshops to continue with support and address any problems that may arise.
GAIT RE-EDUCATION AND SPINAL CORD INJURY:-
1. T1 –T8 – swing to callipers with rollator. Can try crutches if spasticity not a big problem.
2. T8 – T10- swing to and swing through gait with full callipers and crutches. Walking not functional.
3. T10- L2- swing through and four point gait with calipers and crutches. Requires wheelchair for part of day. Walking can be functional.
4. L2 –L4- below knee calipers with crutches or sticks. Wheelchair not required.
5. L4 – L5 may or may not require calipers. Wheelchair not required. May need stick or other walking aid.
General Lower Limb Neuological Examination[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Nas K, Yazmalar L, Şah V, Aydın A, Öneş K. Rehabilitation of spinal cord injuries. World journal of orthopedics. 2015 Jan 18;6(1):8. Available from:https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4303793/ (last accessed 5.1.2020)
- ↑ PATHOLOGICAL OSSIFICATION IN TRAUMATIC PARAPLEGIA*; A. G. HARDY, SHEFFIELD, and J. W. DICKSON, IPSWICH, ENGLAND ; 1963
- ↑ Initial Treatment of Traumatic Paraplegia; By L. GUTTMANN, O.B.E., M.D., M.R.C.P.;1953
- ↑ Spinal cord potentials in traumatic paraplegia and quadriplegia; E M SEDGWICK, E EL-NEGAMY, AND H FRANKEL; 1980
- ↑ Spastic Paraplegia 3A , SPG3A; Peter Hedera ; 2010
- ↑ Aravind N, Harvey L, Glinsky J. Physiotherapy interventions for increasing muscle strength in people with spinal cord injuries: a systematic review. Spinal Cord. 2019; 57: 449–460.
- ↑ Bahaa Mostafa Kamel. https://www.youtube.com/watch?v=VG8Uzt87gko [last accessed 10/02/2016]