Wilms Tumor
Original Editors - Students from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Rachel Flaherty and Allison Hafele
Introduction[edit | edit source]
Wilms tumour is a malignant paediatric renal tumour. Also known as nephroblastoma.[1]
Epidemiology[edit | edit source]
Wilms tumours are the most common paediatric renal cancer (reportedly 85% of cases) and 7% of all childhood cancers are Wilms tumours. They are most common in children ages 3 to 4 and becomes much less common after the age of 5.[2] Wilms’ tumor affects boys and girls equally, and can also be found in adults, though it is very rare.[3]
Etiology[edit | edit source]
The cause of Wilms tumor is not precisely known, but genetic alterations that deal with the normal embryological development of the genitourinary tract are thought to be causative. Wilms patients with a relative with the disease (typically not a parent) number less thyan 1%.[4]
Watch this 1 minute video on Wilms tumour.
Characteristics/Clinical Presentation[edit | edit source]
Wilms’ tumor is often hard to find early because the tumor can grow large without any signs or symptoms. These children may look and act normally.[6] The most common first clinical sign is swelling or a hard mass in the abdomen. It is often firm and large enough to be palpated on both sides of the abdomen, and is usually not painful.[6] Haematuria occurs in ~20% of cases. Hypertension, due to excessive renin production, is found in up to 1/4 of patients. Acquired von Willebrand disease occurs in 8% of cases. [1]
Diagnosis[edit | edit source]
Diagnosis includes:
- A physical exam looking for possible signs of Wilms' tumor.
- Blood and urine tests to see how the kidneys are working.
- Imaging tests may include an ultrasound, computerized tomography (CT) or magnetic resonance imaging (MRI).[2][6]
Management[edit | edit source]
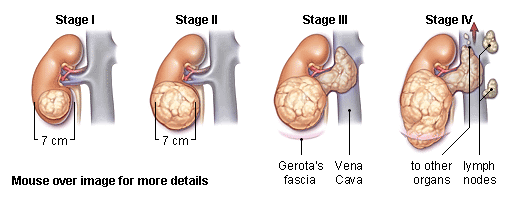
Management of Wilms’ tumor involves surgery, chemotherapy, and radiation therapy. Most children will receive more than one type of treatment. Treatment is based on both the stage and histology of the Wilms’ tumor.[7]
- Unilateral Wilms tumours are, usually, treated by a combination of nephrectomy and chemotherapy.
- Radiotherapy has a small role, but may be used if peritoneal spread or incomplete resection occurs.
Cure today is possible ~90% of the time. Recurrence can occurs within the tumour area, or distally within the lungs or liver.[1]
Physical Therapy Management[edit | edit source]
There are several long-term side effects of chemotherapy. Childhood cancers tend to respond better to chemotherapy than adult cancers. [6]Children’s bodies also tend to tolerate it better than adults do. Side effects of chemotherapy can include fatigue or extreme tiredness from having too few red blood cells.
Musculoskeletal complications that can occur due to radiation therapy include growth abnormalities and hypoplasia. [6]Mild scoliosis and mild asymmetry of all musculoskeletal structures can occur due to reduced growth of bone and paravertebral muscles. These effects are more pronounced the younger the patient is at the time of radiation therapy. [6]
Physical therapy interventions may include strengthening postural muscles and also increasing endurance to promote a higher quality of life. Patients should avoid heavy lifting due to the decreased bone density and risk of osteoporosis.[6]
Alternative/Holistic Management[edit | edit source]
Complementary medicine is treatment used in combination with regular medical care. Alternative treatments are used instead of the traditional medical treatment.[6] Although there are not any alternative medicines to surgery, radiation or chemotherapy, there are complementary treatments including art therapy or play therapy to reduce stress, peppermint tea to relieve nausea, and acupuncture to help relieve pain. [6]
Differential Diagnosis[edit | edit source]
- - Clear cell sarcoma
- - Malignant rhaboid tumor
- - Autosomal recessive polycystic kidney disease (ARPKD)
- - Autosomal dominant polycystic kidney disease (ADPKD)
- - Hydronephrosis
- - Renal carbuncles
- - Hemorrhage
- - Neuroblastoma, an embryonal malignancy of the adrenal gland, usually affect the same age group and commonly arise in the same general region of the abdomen [8]
Case Reports/ Case Studies[edit | edit source]
WT1 mutation as a cause of 46 XY DSD and Wilm's tumour a case report and literature review
Wilms' Tumor Metastatic to Bilateral Testes at Presentation Case and Review of the LiteratureExtrarenal Wilms' Tumor of the Ovary- A Case Report and Short Review of the Literature
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Radiopedia Wilms tumour Available:https://radiopaedia.org/articles/wilms-tumour?lang=gb (accessed 27.1.2023)
- ↑ 2.0 2.1 Mayo Clinic: Wilms Tumor. Available from: http://www.mayoclinic.org/diseases-conditions/wilms-tumor/basics/definition/con-20043492. Accessed 29 October 2022.
- ↑ St. Jude’s Children Research Hospital: Wilms Tumor. Available from:http://www.stjude.org/stjude/v/index.jsp?vgnextoid=5ceb061585f70110VgnVCM1000001e0215acRCRD. Accessed 29 October 2022.
- ↑ Leslie SW, Sajjad H, Murphy PB. Wilms tumor.Available:https://www.ncbi.nlm.nih.gov/books/NBK442004/ (accessed 27.1.2023)
- ↑ UCSFPediatricSurgery. What is Wilms Tumor? Available from: https://www.youtube.com/watch?v=5Jfh3AxUHz0
- ↑ 6.0 6.1 6.2 6.3 6.4 6.5 6.6 6.7 6.8 6.9 American Cancer Society: Wilms Tumor. Available from: http://www.cancer.org/cancer/wilmstumor/index. Accessed 29 October 2022.
- ↑ Dome JS, Huff V. Wilms Tumor Overview. 2003 Dec 19 [Updated 2022]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK1294/. (accessed 29 October 2022).
- ↑ Huszno J, Starzyczny-Slota D, Jaworska M, Nowara E. Adult Wilms’ tumor-diagnsis and current therapy. Cent Eur J Urol. 2013:39-44 Available from:http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3921847/pdf/CEJU-66-00262.pdf. (accessed 29 October 2022)