Zika Virus
Original Editors - Students from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Nicholas Beckham, Admin, Elaine Lonnemann, Abbey Anderson, 127.0.0.1, Evan Thomas, Kayla Limbert, WikiSysop, Vidya Acharya, Rochelle Dsouza, Kim Jackson, Nupur Smit Shah and April Henderson
Definition/Description[edit | edit source]
Zika virus is in the flavivirus family, which is closely related to Dengue, Yellow Fever, Japanese Encephalitis, and West Nile. It is a disease that is spread primarily through the bite of an infected Aedes species mosquito. Zika was first discovered in 1947 and is named after the Zika forest in Uganda. Outbreaks of Zika have been reported in mostly tropical climates including tropical Africa, Pacific Islands, and Southeast Asia.[1]
Prevalence[edit | edit source]
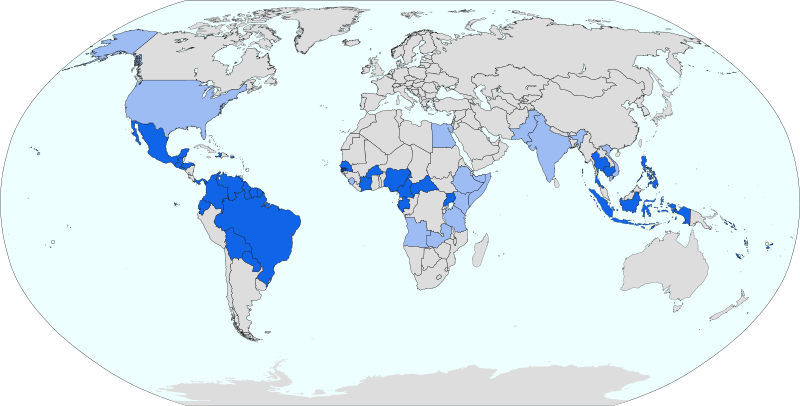
There are currently fewer than 1000 US cases of Zika Virus per year. [3] The below map indicates the prevalence of the Zika virus across the globe, with dark blue indicating confirmed autochthonous infections through biting insects, and light blue indicating only serological evidence.
Since May 2015, the virus has been reported as having been actively transmitted in countries within the Americas. It is predicted that other countries where the mosquito vector is present will also soon begin to report cases of the virus.[4]
Characteristics/Clinical Presentation[edit | edit source]
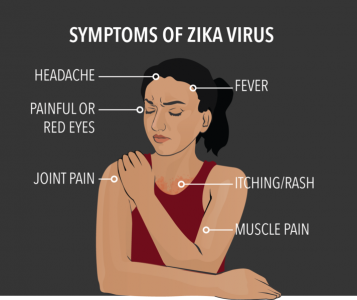
For those infected with the Zika virus, they often will present asymptomatically or with mild symptoms[5]. However, when symptoms do appear, they are very similar to many other diseases. It is probable that many cases of Zika virus have not been reported due to most people infected with the virus not having symptoms. The most common symptoms of Zika are: rash, joint pain, conjunctivitis, muscle pain, stomach pain and diarrhoea[6], and headaches. Illness may last for several days to a week after being infected. Death from the disease is rare, and most victims are not aware of the infection. Zika virus usually remains in the bloodstream for about a week and once infected, the subject is likely to be protected from future infections. [3]
Reports from Brazil indicate an increase in severe foetal birth defects and poor pregnancy outcomes in babies whose mothers were infected with the virus while pregnant.[7] Infection can occur during any trimester, but there is no evidence that pregnancy women are more susceptible than non pregnancy women. [8]Two conditions associated with the Zika virus have made the outbreak more serious. The first is the development of Guillain-Barre syndrome, which manifests as progressive muscle weakness due to damage to the Peripheral Nervous System. The second condition is the surge in congenital microcephaly cases during Zika outbreaks. Further studies are needed to prove a link between microcephaly and Zika virus infection. [1]
Associated Co-Morbidities[edit | edit source]
There is not much current literature on the possibility of associated co-morbidities with the Zika virus. Some reports indicate there may be a link between Zika virus and the onset of Guillain-Barre Syndrome (GBS). There is also much concern of a possible link between Zika virus and microcephaly in the foetuses of women that are infected during pregnancy. [10] Study evaluating the gross motor function of a group of Brazilian children with congenital Zika syndrome (CZS) at 24 months of age showed the presence of CZS symptoms and comorbidities compromising the gross motor functions of children affected with CZS at 24 months[11].
Medications[edit | edit source]
Currently, there is, neither vaccine to prevent nor medicine to treat Zika virus. Tylenol can be used to reduce fever or pain but do not take aspirin or NSAIDs until dengue can be ruled out due to risk of bleeding.[3] Other antipyretics may also be used to help treat symptoms of Zika virus.[12]Prevention of mosquito bites is the best means of protection from the virus.[3]
Diagnostic Tests/Lab Tests/Lab Values[edit | edit source]
For pregnant women, reverse-transcriptase PCR (RT-PCR) can be used to detect the Zika virus during the first week in the host’s blood or the first 4 weeks in the host’s urine. Serology is less reliable due to potential cross reaction with antibodies against similar viruses such as dengue.[7]
Additionally, in February 2016, the FDA issued an Emergency Use Authorization (EUA) for a new diagnostic tool, which is to be distributed to certain laboratories within the United States. The test is called the CDC Zika IgM Antibody Capture Enzyme-Linked Immunosorbent Assay (Zika MAC-ELISA). It is intended to be used to detect antibodies the body makes to fight the virus. The antibodies appear in the bloodstream of an infected person beginning 4-5 days after the illness begins, and lasts for about 12 weeks.[3] Blood and urine tests for RNA can also be used based on patient's symptoms and time to exposure. There is evidence of Zika virus detected in the foetus by amniotic fluid, placenta, foetal brain tissue, and products of conception. [13]
Aetiology/Causes[edit | edit source]
Besides bites from the Aedes species mosquitoes, Zika virus can be spread by other methods as well. If a pregnant mother is infected with the virus, it may spread to her newborn near the time of delivery. A pregnant woman can pass Zika virus to her fetus during pregnancy. However, no reports exist of infants getting Zika virus through breastfeeding. Zika virus may also be spread by sexual contact or blood transfusion. In known cases of transmission, the virus can be transmitted before, during, or after symptoms develop. The virus itself is present in semen longer than in blood.[3]
Prevention[edit | edit source]
- Protect yourself from mosquito bites. Use an insect repellant with high percentage of DEET to longer protection. Reapply as label instructs.
- Apply inspect secondary to sunscreen. Wear long sleeve shirts and long pants during the early morning and late afternoons/evening. This will keep the mosquitos from biting the unclothed skin.
- Be aware of Zika when traveling to outside countries.
- Stay in a well air conditioned with windows/ door screened area.
- If you’re pregnant or trying to get pregnant do not travel to areas that have Zika infected mosquitos.
- If sleeping outdoors use a bed net
- Using eucalyptus soaps and shampoos during your stay.
- Plan for travel for Zika prevention [14]
After Your Trip[edit | edit source]
1. For three weeks take steps to prevent from further mosquitos bites so that the mosquito doesn’t transmit it to other people.
2. Have protected sex
3. Throw out or tightly cover items in or around your home that hold water due to mosquitos being attracted to them.[15]
Systemic Involvement[edit | edit source]
Some of the more common systemic problems include: arthralgia, fever, skin rashes, and malaise. Retinal abnormalities have also been found within paediatric populations with microcephaly attributed to Zika virus infection during pregnancy.[16]
Other systemic manifestations may include: chills, rigours, retro-orbital pain, anorexia, sore throat, lymphadenopathy (cervical, submandibular, axillary, and/or inguinal), hypotension, and conjunctivitis.[17]
Medical Management[edit | edit source]
Currently, treatment is predominantly supportive and includes drinking fluids, rest, and medication (antipyretics and/or analgesics). Patient's reported symptoms must also be addressed. Patients are advised to not use aspirin or any nonsteroidal anti-inflammatory drug (NSAID) until Dengue virus/infection has been ruled out. Dengue virus infection may result in very serious medical complications, including bleeding and even up to death, which may be reduced significantly secondary to supportive treatment and early detection. Women that test positive for Zika virus, and are pregnant with fever symptoms, can and should be treated with acetaminophen. [18]
It is also important for those infected with Zika to try to prevent mosquito bites for the first week of their illness. The rationale is that during the first week of a Zika infection, the virus is found in the blood and can be passed on from an infected person to a non-infected person through mosquito bites. [3]
Physical Therapy Management[edit | edit source]
Research on the scope of physical therapy management for patients with Zika Virus is currently limited. Physical therapy may potentially be used to provide patient education and/or help manage joint and muscle pain related to the Zika virus. One complication that occurs very rarely is a post-infectious autoimmune temporary paralysis called Guillain-Barre Syndrome. Patients experiencing this will be referred to physical therapy to treat neurological impairments such as symmetrical and bilateral weakness, numbness, respiratory insufficiency, and pain. A more common symptom that patients present with is joint pain. As patients recover, physical therapy would be very beneficial in rehabilitating their strength, decreasing their pain through functional exercises and modalities to return to their pre-illness baseline.[19]
Physical Therapy can also be beneficial for children born with congenital Zika. The world health organization has more nations that to look out for health problems other than microcephaly including: spasticity, seizures, irritability, feeding difficulties, eyesight problems, and severe brain abnormalities.[20] PT’s could play an early role in these children’s life by treating their impairments. Interventions could include treating congenital contractures, hypertonia, and motor control.[21]
Possible treatment ideas include: increasing passive and active range of motion, stretching, modalities, and stability strengthening.[22]
Physical Therapy Management Video[edit | edit source]
Differential Diagnosis [23][edit | edit source]
The following may have symptoms similar to that of the Zika virus, and should be ruled out:
- Dengue
- Chikungunya
- Rubella
- Measles
- Reiter's Syndrome
- Allergic reaction
- Conjunctivitis
- Arthritis
- Gout
Case Reports/Case Studies[edit | edit source]
- Case Report on Zika in a Physical Therapy setting
- Duffy MR, Chen TH, Hancock WT, Powers AM, Kool JL, et al. Zika Virus Outbreak on Yap Island, Federated States of Micronesia. New Engl J Med. June 2009;360(24):2536-43. http://bit.ly/1S176Nj
- Sarno M, Sacramento GA, Khouri R, et al. Zika Virus Infection and Stillbirths: A Case of Hydrops Fetalis, Hydranencephaly and Fetal Demise. PLoS Negl Trop Dis. February 2016;10(2):e0004517. doi: 10.1371/journal.pntd.0004517 http://bit.ly/1R4Z9p7
- Musso D, Roche C, Robin E, Nhan T, Teissier A, Cao-Lormeau VM. Potential Sexual Transmission of Zika Virus. Emerg Infect Dis. March 2015;21(3):552. http://bit.ly/29qVRnq
Resources[edit | edit source]
- Centers for Disease Control and Prevention: http://www.cdc.gov/Zika/hc-providers/diagnostic.html
- New Zealand Ministry of Health: http://www.health.govt.nz/our-work/diseases-and-conditions/Zika-virus?ft=form-oD7hiXimxjhdXsYNzfRv5MooQpW05yleWzEVE4F4rHU
- World Health Organisation: http://www.who.int/emergencies/zika-virus/en/?platform=hootsuite
- European Centre for Disease Prevention and Control: http://ecdc.europa.eu/en/healthtopics/zika_virus_infection/factsheet-health-professionals/Pages/factsheet_health_professionals.aspx
References[edit | edit source]
- ↑ 1.0 1.1 Zika Virus. Virology Blog. http://www.virology.ws/2016/01/28/Zika-virus/. Published January 28, 2016. Accessed March 19th, 2016.
- ↑ Cleary E. Zika Virus explained simply. Available from: https://www.youtube.com/watch?v=cGdwix0zYGs [last accessed April 7, 2016]
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and fckLRPrevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Accessed April 7, 2016.
- ↑ Lupton K. Zika Virus disease: a public health emergency of international concern. Brit J Nurs. February 2016;25(4):198-202.
- ↑ Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and Prevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Updated March 23,2017. Accessed March 23, 2017.
- ↑ Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and Prevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Updated March 23,2017. Accessed March 23, 2017.
- ↑ 7.0 7.1 Zika Virus. New Zealand Government Ministry of Health Web site. http://www.health.govt.nz/our-work/diseases-and-conditions/Zika-virus?ft=form-oD7hiXimxjhdXsYNzfRv5MooQpW05yleWzEVE4F4rHU. Updated April 5, 2016. Accessed April 5, 2016.
- ↑ Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and Prevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Updated March 23,2017. Accessed March 23, 2017.
- ↑ Marshall T, Desai R. Zika Virus - definition, symptoms, and complications. Available from: https://www.youtube.com/watch?v=oGNxGlltnOs [last accessed April 7, 2016]
- ↑ Stagg D. Zika Virus and Pregnancy. Nurs Women Health J. 2016;doi: 10.1016/j.nwh.2016.03.001
- ↑ Frota LM, Sampaio RF, Miranda JL, Brasil RM, Gontijo AP, de Melo Mambrini JV, de Brito Brandão M, Mancini MC. Children with congenital Zika syndrome: symptoms, comorbidities and gross motor development at 24 months of age. Heliyon. 2020 Jun 1;6(6):e04130.
- ↑ Sikka V, Chattu VK, Popli RK, et al. The Emergence of Zika Virus as a Global Health Security Threat: A Review and a Consensus Statement of the INDUSEM Joint working Group (JWG). J Glob Infect Dis. 2016;8(1):3-15.
- ↑ Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and Prevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Updated March 23,2017. Accessed March 23, 2017.
- ↑ Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and Prevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Updated March 23,2017. Accessed March 23, 2017.
- ↑ Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and Prevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Updated March 23,2017. Accessed March 23, 2017.
- ↑ Fontes BM. Zika virus-related hypertensive iridocyclitis. Arquivos Brasileiros de Oftalmologia. Published January 2016. Accessed March 2016.
- ↑ Chan JFW, Choi GKY, Yip CCY, Cheng VCC, Yuen KY. Zika fever and congenital Zika syndrome: An unexpected emerging arboviral disease. J Infection. March 2016;doi:10.1016/j.jinf.2016.02.011
- ↑ Oduyebo T, Petersen EE, Rasmussen SA, et al. Update: Interim Guidelines for Health fckLRCare Providers Caring for Pregnant Women and Women of Reproductive Age with Possible Zika Virus Exposure – United States, 2016. Morbidity and Mortality Weekly Report. 2016; 65(5): 122-127.
- ↑ The Latest News on Zika. APTA. http://www.apta.org/PTinMotion/News/2016/7/1/ZikaUpdateJune2016/. Published July 1, 2016. Accessed March 23, 2017.
- ↑ The Latest News on Zika. APTA. http://www.apta.org/PTinMotion/News/2016/7/1/ZikaUpdateJune2016/. Published July 1, 2016. Accessed March 23, 2017.
- ↑ Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and Prevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Updated March 23,2017. Accessed March 23, 2017.
- ↑ Zika Virus Disease in the United States, 2015-2016. Centers for Disease Control and Prevention Web site. http://www.cdc.gov/zika/geo/united-states.html. Published February 4, 2016. Updated March 23,2017. Accessed March 23, 2017.
- ↑ Whelan P, Hall J. Zika virus disease. The Northern Territory Disease Control Bulletin. 2008; 15(1): 19-21.