Rupture Long Head Biceps: Difference between revisions
Leana Louw (talk | contribs) No edit summary |
Leana Louw (talk | contribs) No edit summary |
||
| Line 48: | Line 48: | ||
* Special tests: | * Special tests: | ||
** [[Yergasons Test|Yergason's test]] : Positive if pain is reproduced in the bicipital groove during the test <ref name="p2" /> | ** [[Yergasons Test|Yergason's test]] : Positive if pain is reproduced in the bicipital groove during the test <ref name="p2" /> | ||
{| width="100%" cellspacing="1" cellpadding="1" | |||
|- | |||
|{{#ev:youtube|_Cjahul5yuI|}} | |||
** | ** | ||
Revision as of 17:38, 6 January 2019
Original Editor - Cynthia Meert
Top Contributors - Bianca Geeroms, Leana Louw, Cynthia Meert, Admin, Lucinda hampton, Rachael Lowe, Kim Jackson, Anas Mohamed, WikiSysop, 127.0.0.1, Naomi O'Reilly, Linde Van Droogenbroeck, Claire Knott, Amrita Patro and Wanda van Niekerk
This article or area is currently under construction and may only be partially complete. Please come back soon to see the finished work! (10 June 2024)
Definition/Description[edit | edit source]
Rupture of the biceps tendon often occurs after a sudden contraction of the biceps with resistance to flexion and supination of the forearm. Also intrinsic degeneration of the tendon release and frictional wear of the tendon belly may have an impact.This intrinsic degeneration is caused by improper training or fatigue, inordinate stresses can be placed on the biceps as it attempts to compensate for other muscles. This can lead to attrition and failure, either within the tendon substance or at its origin. [1]
The long head of the biceps has several functions like dynamic stabilizer of the glenohumeral joint and a depressor of the humeral head[2]
Clinically relevant anatomy[edit | edit source]
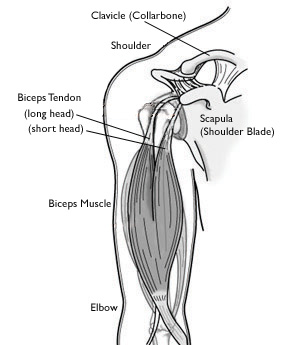
The M. biceps brachii has 2 parts: The long head and the short head. The long head originates at the tuberculum supraglenoidale scapulae and is attached to the dorsal aspect of the tuberositas radii.[3]
The long head biceps starts from the tuberculum subraglenoidale with an intra-articular part. The part passes over the humeral head and then follows the bicipital groove distal to the glenohumeral joint. [4]
There is a strong evidence that the short head is used as more powerful elbow flexor, while the long head is more used as a powerful supinator.[5]
Both parts of the tendon are different in shape. The intra-articular part is wide and flat. The extra-articular part is rounder and smaller. [4]
The articular portion of the Long head Biceps is irrigated by the anterior circumflex artery. [4]
The distal part of LHB is fibrocartilaginous and avascular. The part most vascularized is the proximal tendon. [4]
A soft-tissue stabilizes the extra-articular LHB when it enters the bicipital groove en this is built by fibers of the coracohumeral ligament, superior glenohumeral ligament and parts of the subscapularis tendon.[4]
Epidemiology/Etiology[edit | edit source]
Biceps rupture mainly occurs in individuals between 40 and 60 years who already have a history of shoulder problems. This often happens due overuse: many tears are the result of a wearing down and fraying of the tendon that occurs slowly over time. It can be worsened by repeating the same shoulder motions again and again. Overuse can cause a range of shoulder problems, including tendonitis, shoulder impingement, and rotator cuff injuries. Having any of these conditions puts more stress on the biceps tendon, making it more likely to weaken or tear. [6] Also younger individuals can have this injury but usually after a traumatic fall on an outstretched arm, heavy weightlifting or consistently sport activities such as snowboarding, soccer, ... [5] [7]
Tendon rupture usually results from sudden contraction of the biceps associated with resisted flexion and supination of the forearm, and a predisposing role is possibly played by intrinsic degeneration of the tendon tissue or frictional wear of the tendon belly. [1]
The dominant arm is involved more commonly, probably because it is used more often than is the nondominant arm. [2]
Long head of biceps tendon rupture occurs in 31%-56% of isolated subscapular tears. [2]
No correlation exists between race and the incidence of biceps rupture. [2]
The chance on a tendon tear of the biceps increases with:
- Age. Older people have put more years of wear and tear on their tendons than younger people. [1]
- Heavy overhead activities. [1]
- Shoulder overuse. [1]
- Smoking. Nicotine use can affect nutrition in the tendon. [1]
- Corticosteroid medications. Using corticosteroids has been linked to increased muscle and tendon weakness. [1]
- Gender. Men suffer of biceps rupture more commonly than women, but this difference may result primarily from vocational or avocational factors. [2]
Characteristics/Clinical presentation[edit | edit source]
Patients with a long head biceps rupture report a wide variety of symptoms. [7]
Some patients hear a pop at the time of the trauma, others feel a sharp pain in the anterior shoulder. [5]
This acute pain can be accompanied by snapping sensation [7]
Some patients have a nondescriptive pain while performing overhead activities. [7]
Other patients have a nondescriptive anterior shoulder pain that may get worse at night.[7]
Most LHB pathologies were associated with Rotator Cuff tears of a duration longer then 3 months and an area of 5 cm2. [8]Also shoulder problems like tendonitis or schoulder impingement can cause a rupture of the Long head biceps. [7]
The subscapularis tendon is mostly involved with LHB pathologies.[8]
If there is a rupture of the distal biceps tendon, a Popeye deformity can be seen. [7]
Differential diagnosis[edit | edit source]
Diagnostic procedures[edit | edit source]
Physical examination[edit | edit source]
- Special tests:
- Yergason's test : Positive if pain is reproduced in the bicipital groove during the test [2]
Special investigations[edit | edit source]These studies can create a good image of soft tissues like the biceps tendon. [1] Outcome measures[edit | edit source]Examination[edit | edit source]Diagnosis can be based on clinical examination (grades of recommendation:B) , based on:
- the presence of the classic Popeye sign or a less striking descent of the biceps muscle in the middle part of the arm. (more obvious by contracting the muscle ) [3]
- assesses pain, function, ROM, and strength.[5] - Pain is allotted a maximum of 15 points, activities of daily living (function) 20 points, ROM 40 points, and strength 25 points. The component scores are summated to achieve a maximum possible total score of 100. A maximum score indicates greater shoulder function.[5]
- with the forearm flexed at 90° and the arm adducted to the body, with the hand in full supination
Medical management[edit | edit source]There is no consensus about surgical repair.
There are anti-inflammatory medications that can be used to reduce the underlying inflammatory process that may predispose tendons to rupture. When tendons may be stressed or partially disrupted, anti-inflammatory medications can provide an analgesic effect.(Grades of recommendation = F) [9]
Physiotherapy management[edit | edit source]
- Codman pendulum exercises - Functional exercises
Before the doctor decides to operate, he considered about the advantages and disadvantages. In this situation, the activities of the patiënts , the way of living and the age are important. The operation is often carried out by young people or people who have a hard work, like a carpenter, port worker,… etc. These people need a maximal supination strenght. There will also be operated when some people can’t accept the Popeye malformation. The operation trial ( tenotomy) includes the attaching torn tendon to the bone. The results of the other studies shows us that the function of the muscle fully recovers and that the strength can go back like it was before the rupture. They also see a good cosmetic result. [10] (LoE: 3B) postoperative (tenotomy) rehabilitation [11] (LoE: 5) phase 1: passive
week 1
week 3
Phase 4 : weight training
- Computer after 1-2 weeks
2. conservative treatment Is more used in older patients and who do not need maximal supination strength in their daily life and work. There are some advantages in comparison with the first treatment. Therefore, this treatment is better tolerated and presents fewer complications. The costs are also lower and because there was no operation, the people can get back to work quicker. But with this choice of treatment the strength is 20% lower then before. But it hasn’t have influence at the ADL activities and that maybe is the reason why people hold off an operation. Also doctors recommend this treatment faster when people are afraid or when the injury is too old.
- apply appropriate joint mobilization to restrictive capsular tissues - begin scapular stabilization with instruction in lower trapezius facilitation
- sport cord internal/external rotation in 30° abductee
phase 3: advanced strengthening
- resisted PNF patterns phase 4: return to activities
Resources[edit | edit source]add appropriate resources here Clinical Bottom Line[edit | edit source]add text hereReferences[edit | edit source]
|