|
|
| Line 21: |
Line 21: |
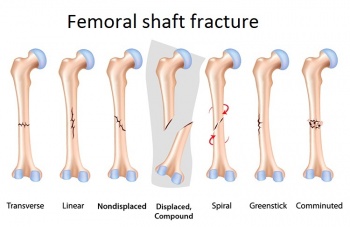
| # Partial fracture: incomplete break of a bone. This type of fracture refers to the way the bone breaks. In an incomplete fracture, the bone cracks but doesn’t break all the way through. In contrast, there is a complete fracture, where the bone snaps into two or more parts.<ref>Cleveland Clinic. Fractures. 2013. (Available at http://my.clevelandclinic.org/services/orthopaedics-rheumatology/diseases-conditions/hic-fractures, assessed 21 December 2014)fckLR</ref><ref>WebMD. Broken bone: types of fractures, symptoms and prevention. 2014. (Available at http://www.webmd.boots.com/a-to-z-guides/bone-fractures-types-symptoms-prevention, accessed on 21 december 2014)fckLR</ref> | | # Partial fracture: incomplete break of a bone. This type of fracture refers to the way the bone breaks. In an incomplete fracture, the bone cracks but doesn’t break all the way through. In contrast, there is a complete fracture, where the bone snaps into two or more parts.<ref>Cleveland Clinic. Fractures. 2013. (Available at http://my.clevelandclinic.org/services/orthopaedics-rheumatology/diseases-conditions/hic-fractures, assessed 21 December 2014)fckLR</ref><ref>WebMD. Broken bone: types of fractures, symptoms and prevention. 2014. (Available at http://www.webmd.boots.com/a-to-z-guides/bone-fractures-types-symptoms-prevention, accessed on 21 december 2014)fckLR</ref> |
| # Completed displaced fracture: breaks into two or more pieces and is no longer correctly aligned. Displacement of fractures is defined in terms of the abnormal position of the distal fracture fragment in relation to the proximal bone. <ref>2.0 2.1 WebMD. Understanding Bone Fractures - the Basics. 2014. (Available at http://www.webmd.com/a-to-z-guides/understanding-fractures-basic-information, accessed 19 December 2014) fckLR</ref> | | # Completed displaced fracture: breaks into two or more pieces and is no longer correctly aligned. Displacement of fractures is defined in terms of the abnormal position of the distal fracture fragment in relation to the proximal bone. <ref>2.0 2.1 WebMD. Understanding Bone Fractures - the Basics. 2014. (Available at http://www.webmd.com/a-to-z-guides/understanding-fractures-basic-information, accessed 19 December 2014) fckLR</ref> |
|
| |
|
| |
|
| |
| ==== Range Of Motion ====
| |
| Improve the range of motion for the hip and the knee joint. In elderly population, the focus is to achieve functional range of motion.
| |
| {| class="wikitable"
| |
| |+
| |
| !Motion
| |
| !Normal
| |
| !Functional
| |
| |-
| |
| |Knee Flexion
| |
| |130 to 140 degrees
| |
| |110 degrees
| |
| |-
| |
| |Hip Flexion
| |
| |125-128 degrees
| |
| |90 to 110 degrees
| |
| |-
| |
| |Hip Extension
| |
| |0-20 degrees
| |
| |0 to 5 degrees
| |
| |-
| |
| |Hip Abduction
| |
| |45 to 48 degrees
| |
| |0 to 20 degrees
| |
| |-
| |
| |Hip adduction
| |
| |40 to 45 degrees
| |
| |0 to 20 degrees
| |
| |-
| |
| |Internal and External Rotation
| |
| |45 degrees
| |
| |0 to 15/20 degrees
| |
| |}
| |
|
| |
| ==== Muscle Strength ====
| |
| The physical therapist has to focus on restoring the strength of the following muscles that are affected by the fracture:
| |
|
| |
| === '''PT management''' ===
| |
| Whilst in hospital, a therapist will teach the patient how to use a walking aid to allow them to mobilise, depending on their weight bearing status. The patient should be taught basic range of movement and strengthening exercises to maintain a degree of strength and reduce the risk of blood clots.
| |
|
| |
| Surgical fixation and immobilization are followed by extensive physical therapy. Under extensive therapy can be understood that the patients who underwent a femur fracture should receive a treatment by a physiotherapist who will invest time in gait training. Gait training results in increased bone formation. Even if gait training is completed using 30-50% of body weight support, an increase in bone formation could be found. <ref name="Carvalho et al.">Carvalho DC, Garlipp CR, Bottini PV, Afaz SH, Moda MA, Cliquet Jr A. [https://www.scielo.br/j/bjmbr/a/m9NT8PxjVGHMdyJY5nNXtLS/abstract/?lang=en Effect of treadmill gait on bone markers and bone mineral density of quadriplegic subjects]. Brazilian journal of medical and biological research. 2006;39:1357-63.</ref>After a femoral fracture, most of the muscles are much weaker than before so physiotherapy is very important. <br>
| |
|
| |
| The physiotherapist will begin with a range of motion exercises for the hip, knee and ankle because mobility is decreased following immobilization. Mobilization is a very important treatment in the recovery process. The patient can also begin strengthening exercises based on the surgeon's orders (typically six weeks post-op). Patients should also undergo balance and proprioceptive rehab and these abilities are quickly lost with inactivity. <br>
| |
|
| |
| ==== Mobility exercises ====
| |
|
| |
| Knee: flexion and extension, abduction and adduction<br>Hip: flexion and extension, abduction and adduction, rotation <br> Functional quadriceps exercises should be initiated as soon as possible after the surgery because the quadriceps help provides stability in the knee. Flexion exercises also need to start as soon as possible, provided the fracture is adequately supported (i.e. the selected fixation approach allows for weight bearing). Physiotherapy should be continued until an acceptable functional range has been achieved or until a static position has been reached. It is necessary to record the range of movements in the knee with accuracy; first, this should be done at weekly and then at monthly intervals. <br>
| |
|
| |
| During the postoperative treatment of patients with a proximal femoral fracture, physical therapy should focus on increasing the muscle strength, to improve walking safety and efficiency. Allowing the elderly patient to become more independent.
| |
|
| |
| Research indicates that strengthening the abductor and adductor muscles of the hip increase the mediolateral stability during walks. Resulting in an influence on the improvement of the patient’s dynamic balance.<ref name="Carneiro et al.">MCarneiro B, Alves DP, Mercadante MT. Physical therapy in the post-operative of proximal femur fracture in elderly: Literature review. Acta Ortop. Bras. 2013;21:175-8.</ref><br>
| |
|
| |
| ==== Orthopaedic therapy ====
| |
|
| |
| <br>During the immobilisation period, the therapists need to actively mobilise the foot, with or without weight. Another important aspect is the mobilisation through a hole in the plaster of the patellar bone. The use of isometric exercises are also important to train the muscles (quadriceps, hamstring & glutei) of the upper leg. After the immobilisation period, it is necessary to fixate the leg manually or by using a brace. The fixation is needed for the re-education of hip and knee and to secure a progressively verticalisation of the leg and to make the patient independent while walking or during other activities. Also, stabilisation exercises with unilateral support are recommended, but also balneotherapy. After the consolidation therapists need to focus on progressively increased pressure, the revalidation of the gait cycle, more intense mobilisation, strength-training therapy to reverse the muscle atrophy that occurred during the immobilisation period and condition training to increase the loss of endurance during the immobilisation period.<br>
| |
| As non-operative treatment there are 3 alternatives:<br>1. Skin traction: used in adults only for emergency fracture immobilisation in the field for patient comfort and to facilitate patient transport. Main disadvantage is the causing of slippage or skin necrosis when applying sufficient forces to the limb.<br>2. Skeletal traction: used for early fracture care before a definitive operative procedure can be performed. The goal is to restore the femoral length and to limit rotational and angular deformities. Skeletal traction may be applied through the distal femur or proximal tibia. Problems with skeletal traction include knee stiffness, limb shortening, prolonged hospitalisation, respiratory and skin ailments, and malunion. <br>3. Cast Brace: an external support device that permits progressive weight bearing by partially unloading the fracture through circumferential support of the soft tissues. Indications for cast bracing include open fracture, distal third fractures, and comminuted midshaft fractures of the femur. Proximal, simple transverse, or oblique fractures are less amendable to cast bracing due to high stress concentration and a propensity to angulate. The cast brace is best used after an initial period of skeletal traction. Consistently high rates of union, superior to 90%, usually by 13 to 14 weeks, have been reported in numerous studies. Problems with cast bracing include loss of reduction and subsequent malunion, shortening and angulation.<ref name="Keany">Keany, J. et al. Femur fracture. 2013. (Available at http://emedicine.medscape.com/article/824856-overview, accessed 6 November 2014)</ref><br>
| |
|
| |
| ==== Physical Exercise ====
| |
|
| |
| <br>Improving muscle strength is necessary to enhance postoperative walking capacity for rehabilitation and to diminish the risks of falls. Physical activity will help:
| |
|
| |
| *Preventing other fractures
| |
| *Increasing gait speed & balance
| |
| *Increasing ADL Performance
| |
| *Regaining walking capacity as early as possible after immobilization to avoid respiratory complications<ref>MCarneiro B, Alves DP, Mercadante MT. Physical therapy in the post-operative of proximal femur fracture in elderly: Literature review. Acta Ortop. Bras. 2013;21:175-8. </ref>
| |
|
| |
| Aerobic fitness is useful to include in a physical therapy plan for an improved cardiorespiratory capacity will lead to a better walking capacity. <br>Physical exercises are not only crucial for rehabilitation after fracture but for ongoing reinforcing of the mineral bone density, especially in vulnerable populations like elder fragile patients, osteoporotic post-menopausal women or people suffering from osteoporosis or osteopenia. Long-term odd-impact exercise-loading, is associated, similar to high-impact exercise-loading, with a 20% thicker cortex around the femoral neck <ref>Nikander R, Kannus P, Dastidar P, Hannula M, Harrison L, Cervinka T, Narra NG, Aktour R, Arola T, Eskola H, Soimakallio S. [https://link.springer.com/article/10.1007/s00198-008-0785-x Targeted exercises against hip fragility]. Osteoporosis International. 2009 Aug;20(8):1321-8.</ref>. In aerobic fitness, these type of movements are most frequently used.
| |
|
| |
| Moderate magnitude impacts from Odd-exercise loading is mechanically less demanding and makes the body work in all directions, retraining the biomechanical qualities and properties of the bone structure and impacting positively the bone mineral density. Fitness aerobics, dance fitness, dance, ball games, gymnastics involving rapid turns and movements are good examples of odd-impact exercises.<br>Furthermore, duration, frequency and intensity are important and should be customized to the different age-groups.
| |
|
| |
| Strengthening exercises seem to be key for the functional improvement. <ref>MCarneiro B, Alves DP, Mercadante MT. Physical therapy in the post-operative of proximal femur fracture in elderly: Literature review. Acta Ortop. Bras. 2013;21:175-8.</ref> These strength exercises may as well produce advantages in the psychosocial area which tends to be altered in elder patients that suffered a fracture. Weight-bearing exercises will reinforce the dynamic balance and functional performance <ref>Yang SD, Ning SH, Zhang LH, Zhang YZ, Ding WY, Yang DL. [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5370805/ The effect of lower limb rehabilitation gymnastics on postoperative rehabilitation in elderly patients with femoral shaft fracture: a retrospective case-control study]. Medicine. 2016 Aug;95(33). </ref>, especially exercises in standing position since they are more challenging for the postural control <ref>MCarneiro B, Alves DP, Mercadante MT. Physical therapy in the post-operative of proximal femur fracture in elderly: Literature review. Acta Ortop. Bras. 2013;21:175-8. </ref>.<br>
| |
|
| |
| ==== Home Rehabilitation Training ====
| |
|
| |
| <br>Home Rehabilitation Training leads towards better rehabilitation and better performance in daily activities. Home physiotherapy training is suitable for all elder patients, including those suffering from cognitive or psychological impairment. The literature stresses the importance of home physiotherapy, in combination with day-to-day activities like going to the shop, for gaining confidence, balance, functionality and reducing as such the number of falls. Therefore it can also be seen as a way to prevent falls. <ref>Giusti A, Barone A, Oliveri M, Pizzonia M, Razzano M, Palummeri E, Pioli G. [https://www.sciencedirect.com/science/article/pii/S0003999306001663 An analysis of the feasibility of home rehabilitation among elderly people with proximal femoral fractures]. Archives of physical medicine and rehabilitation. 2006 Jun 1;87(6):826-31.</ref>Fall prevention programmes are important for the elder population that already suffers a femoral fracture. The literature indicates that elder people often fall again following a previous hip or femoral fracture and that this constitutes a major health problem <ref>Berggren M, Stenvall M, Olofsson B, Gustafson Y. [https://link.springer.com/article/10.1007/s00198-007-0507-9 Evaluation of a fall-prevention program in older people after femoral neck fracture: a one-year follow-up]. Osteoporosis international. 2008 Jun;19(6):801-9. </ref>. The study of Berggren et al. concludes that fall-prevention must be part of everyday life in fall-prone elderly. Prevention and treatment of fall-risk factors are key. These programs should include gait training with advice on assistive devices and medication, exercise programmes for balance training, treatments for cardiovascular problems, environmental modifications and hypotension.<ref>Stenvall M, Olofsson B, Lundström M, Englund U, Borssén B, Svensson O, Nyberg L, Gustafson Y. [https://link.springer.com/article/10.1007/s00198-006-0226-7 A multidisciplinary, multifactorial intervention program reduces postoperative falls and injuries after femoral neck fracture]. Osteoporosis international. 2007 Feb;18(2):167-75.</ref>.
| |
|
| |
| <br>
| |
|
| |
| == References == | | == References == |
|
| |
|