Benign Joint Hypermobility Syndrome
Introduction[edit | edit source]
Joint Hypermobility Syndrome (JHS) was first described in 1967 by Kirk and colleagues as a condition where joint laxity is associated with various musculoskeletal complaints.[1] JHS encompasses various disorders such as Benign Joint Hypermobility Syndrome (BJHS), Ehler-Danlos Syndrome (EDS), Marfan Syndrome and Osteogenesis Imperfecta.[2] All of these disorders are classified as hereditary connective tissue disorders (HCTDs).[2]
Connective tissue is found throughout the body (ligaments, tendons, joints, the digestive tract, heart, eyes), so JHS does not just affect the joints. It can also affect skin extensibility, digestion and in more severe connective tissue disorders like Marfan Syndrome, it can affect heart function.[3]
Unlike other connective tissue disorders, BJHS is a condition which causes musculoskeletal symptoms in hypermobile patients, without other rheumatological features being present.[4] Its primary symptom is symptomatic hypermobility (ie excessive laxity) of multiple joints.[5][6] and it is associated with arthralgia, poor exercise tolerance and potentially recurrent subluxations.[7][5] Links to other conditions such as and mitral valve prolapse in patients with BHJS and fibromyalgia[8] and primary focal hyperhidrosis (i.e. excessive sweating) are also being explored, but further research is required[9].
Epidemiology[edit | edit source]
Generalised joint laxity is often observed in people who do not have any other symptoms.[4] Hypermobility that is not connected with systemic disease is said to occur in 4% to 13% of the population.[4] Prevalence rates vary across ethnicities. Prevalence of BJHS is 5% to 18% in Caucasian populations, and up to 43% in non-Caucasian populations[10] - there are generally higher rates of this condition in Asian, African and Middle Eastern people.[4] In 1973, Beighton and colleagues demonstrated that the number of positive hypermobility tests was age and gender-related - i.e. rates are higher in younger children and women have higher scores than age-matched men (approximately a 2:1 ratio).[11][10]
There have been a number of studies looking at prevalence rates of hypermobility in children. One study by Gedalia and colleagues found that generalised hypermobility occurs in 66% of school children with arthralgia of unknown cause.[4][12] However, while de Inocencio Arocena and colleagues found similar prevalence rates as Gedalia et al (hypermobility prevalence was 55% and 71 % in children aged less than 8 years),[13] they found that there was no association between hypermobility and developing arthralgia.[4][13] Thus, it appears that generalised hypermobility can exist without joint pain.[4]
BJHS has a strong genetic component and appears to be caused by an abnormality in collagen or the ratio of collagen subtypes.[4] Mutations in the fibrillin gene have also been found in families with BJHS.[4]
Signs and Symptoms[edit | edit source]
The most common initial complaint of BJHS is joint pain. One or more joints may be affected and the presentation may be generalised or symmetric. While any joint can be affected, the most commonly involved joints are the knee and ankle.[4]
Symptoms can begin at any age with young children often affected. The pain is often in multiple joints. While BJHS tends to be a self-limiting condition,[4] pain will persist for some patients and can become chronic.[3][14] It has been found that a high proportion of patients diagnosed with chronic pain also have generalised joint hypermobility.[15]
Patients with BJHS are often particularly prone to overuse injury.[16] They may have a subjective history of being very active during the day, which may indicate an imbalance between the tissue capacity and the amount of load being placed on the tissues.[3] The resulting overload can stimulate the central nervous system, causing an increase in pain as the day progresses.[3] Thus, patients may often complain of night pain.[4] As many of these patients are young children, these symptoms can be overlooked as “growing pain". They may also present with sensations of muscle tightness in the evening.[3]
Other signs of connective tissue disorder may be present. These include:[4]
- Scoliosis
- Pes planus
- Genu valgum,
- Lordosis
- Patellar subluxation or dislocation
- Marfanoid habitus
- Varicose veins
- Rectal or uterine prolapse
- Thin skin[4]
There has been some controversy over the association of BJHS with mitral valve prolapse. Early studies appeared to show an association between MVP and BJHS, but this has been questioned in later studies.[4]
Diagnosis[edit | edit source]
The diagnosis of BJHS is made with a clinical examination and it is one of exclusion.[3] If patients present with painful or swollen joints, inflammatory and autoimmune causes need to be excluded, as does infection. Medical tests to exclude these conditions might include: a complete blood cell count, erythrocyte sedimentation rate, rheumatoid factor, antinuclear antibody test, serum complement (C3, C4, CH50) levels, and serum immunoglobulin (IgG, IgM, IgA) levels. If any of these test results are outside normal ranges, a diagnosis other than BJHS is likely.[4]
Because BJHS shares a number of features with other connective tissue disorders like Marfan Syndrome and Osteogenesis Imperfecta, these conditions need to be ruled out.[4] Key distinguishing features may be present to differentiate between these disorders.
Ehlers–Danlos Syndrome (EDS)[edit | edit source]
EDS has a very similar presentation to BJHS. EDS is a group of connective tissue disorders that cause gross joint laxity, as well as symptoms such as purple papyraceous scars, skin hyperelasticity, and fragile skin, meaning patients are prone to bruising. The most common types of EDS are Types I, II and III.[4] Ross and Grahame note that BHJS can not be distinguished from the hypermobility type of EDS (Type III).[5] Symptoms associated with EDS Type III are joint pain, hypermobility, mild extra-articular involvement, and mild skin changes without scarring.[4] It has therefore been proposed that BJHS may indeed be a mild form of EDS - and that the two conditions are really a continuum.[15][17][10] Both BJHS and EDS are inherited disorders and are due to problems with collagen.[4]
Marfan Syndrome[edit | edit source]
Marfan Syndrome is an autosomal dominant disorder. Patients with Marfan's tend to have a family history of the disorder. Cardiac and ocular features are often present. Patients have a tall, thin build (marfanoid habitus), generalised joint hypermobility, elongated fingers (arachnodactyly), myopia, and lens dislocation.[4]
Osteogenesis Imperfecta[edit | edit source]
Osteogenesis Imperfecta is another disorder associated with a defect in collagen. Patients present with excessive joint laxity, thin blue sclera, and bone fragility, which results in multiple fractures and bony deformities.[4]
Juvenile Rheumatoid Arthritis[edit | edit source]
Juvenile rheumatoid arthritis should be considered in children who present with hypermobility and joint pain. However, the onset of arthritis must occur before 16 years and will involve inflammation of one or more joints. Other rheumatic disorders may also be considered.[4]
Beighton Scale of Hypermobility[edit | edit source]
Once the above conditions have been excluded, a diagnosis of BJHS can be considered. The key assessment measure for BJHS is the Beighton Scale of Hypermobility. The Beighton Scale is a measure of generalised joint laxity and was developed to establish diagnostic criteria for BJHS. It is used to help distinguish BJHS from other connective tissue disorders.[4]
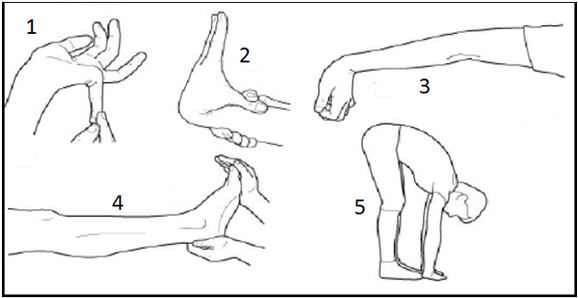
The patient is asked to do five simple movements (see figure 1). Scoring is as follows:
| LEFT | RIGHT | |
| 1. Passive dorsiflexion and hyperextension of the fifth MCP joint beyond 90° | 1 | 1 |
| 2. Passive apposition of the thumb to the flexor aspect of the forearm | 1 | 1 |
| 3. Passive hyperextension of the elbow beyond 10° | 1 | 1 |
| 4. Passive hyperextension of the knee beyond 10° | 1 | 1 |
| 5. Active forward flexion of the trunk with the knees fully extended so that the palms of the hands rest flat on the floor | 1 | |
| TOTAL | / 9 | |
The scoring criteria changes based on age as people become stiffer over time.
- Pre-pubertal girls and boys - a score of six or more is considered positive for joint hypermobility
- Pubertal men and women up until the age of 50 years - a score of five or more is considered positive
- Adults aged over 50 - a score over four is considered positive[3]
It is important to remember when using this measure that BJHS refers to pain associated with hypermobility - not hypermobility alone.[3]
Management[edit | edit source]
Education[edit | edit source]
Education is a key component in the management of BJHS. It should cover a number of areas, including education about the condition, as well as pain education.[3] It should be highlighted to patients and their families that BJHS is a non-progressive connective tissue disorder that can be successfully managed with changes in lifestyle, exercise and joint protection.[4]
Load management is key for these patients, thus it is important to include a discussion about activity/ sport schedules when educating patients and their families. Vigorous or repetitive activities are considered to be aggravating factors.[4] Overtraining or a focus on joint flexibility rather than stability can increase joint pain and increase the risk of injury.[4]
Points to consider when discussing a patient’s schedule with his / her family:[3]
- Ascertain the level of load and potentially discuss the need to reduce activity levels. It is important to highlight that this is likely a short term solution to allow the tissues to accommodate/ recover and for the pain system to desensitise
- Once pain levels have decrease / stabilised, a managed return to loaded activities can be appropriate[3]
- Ascertain the amount of formal sport vs free play - play enables a child’s nervous and musculoskeletal systems to become adaptive and resilient.[3] Formal sports are often loaded and included many repetitive activities, which increases strain on specific tissues
- A general rule is that children should match the amount of formal sport with their age - i.e. if they are 7 years old, they should not do more than 7 hours of sport per week[3]
Exercise[edit | edit source]
Exercise is an essential component in the management of BJHS.[10] Specific joint strengthening programmes for children experiencing pain associated with BJHS has been found to be beneficial[3] although there is currently limited evidence to indicate which form of exercise is best.[18]
Initially, it is important to protect the joint and decrease pain levels. In the early stages of rehabilitation, braces or crutches may be helpful as a short term solution when there are high levels of pain. Similarly, orthotics or strapping might have a positive effect.[3]
Targeted graded exercise programmes appear to be useful for these patients.[3] Isometric exercises could be a good starting point to increase resilience and to desensitise the nervous system.[3]
Options for strengthening include:
As the patient progresses, it is important to start loading the joint in the hyper-extensive range to help build resilience in these end-range positions.[3] Pacey and colleagues found that when young patients exercise in this range, their parents report improvements in their psychosocial health. Exercising in a neutral range was perceived as affecting only physical health.[19] The exercises included in Pacey and colleague's eight week programme included:[19]
- Isometric exercises of the hamstrings and quadriceps in supine
- Theraband and joint control exercises in standing
- Prone eccentric hamstring exercises
- Side lying gluteus medius exercises
- Standing hip abductor exercises
In the later stage of an exercise programme, variability in terms of exercise type and speed is important.[3] There should also be a focus on proprioceptive and balance activities as they have been found to decrease pain and improve function in patients with BJHS.[20]
The following video includes exercises that can be useful for children under 8 years.
Children aged over 8 years can benefit from a range of theraband exercises, including quadriceps strengthening (see below) and inner range brachialis exercises.
Additional Exercise Resources[edit | edit source]
The following resources include various games and exercises that may be useful for children with BJHS:
- PhysiFun Physical Fundamentals
- Hypermobility Exercises from Ashford and St Peter's Hospitals, NHS Foundation Trust
- Hypermobility exercises for under 5’s from the Royal Berkshire NHS Foundation Trust
Medication[edit | edit source]
As BJHS is not associated with inflammation, non-steroidal anti-inflammatory drugs (NSAIDs) will have little benefit.[3][4] Paracetamol is more likely indicated,[3] as well as rest and joint protection.[4]
Summary[edit | edit source]
- BJHS is a non-progressive, non-inflammatory connective tissue disorder that results in hypermobility and pain[4]
- As laxity and symptoms tend to decrease with age, patients with BJHS often have good outcomes[4]
- They can, however, be at risk for longer-term pain conditions, as well as acute soft tissue injuries, overuse injury, joint instability and uterine/rectal prolapse[4]
- BJHS can often be managed with appropriate education and exercise therapy[3]
References[edit | edit source]
- ↑ Kirk JA, Ansell BM, Bywaters EG. The hypermobility syndrome: musculoskeletal complaints look for more recent sources associated with generalized joint hypermobility. Ann Rheum Dis. 1967; 26(5): 419–25.
- ↑ 2.0 2.1 Neki NS, Chhabra A. Benign Joint Hypermobility Syndrome. Journal of Mahatma Gandhi Institute of Medical Sciences. 2016; 21(1): 12-18
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 Prowse, T. Benign Joint Hypermobility Syndrome Course. Plus. 2020.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 4.16 4.17 4.18 4.19 4.20 4.21 4.22 4.23 4.24 4.25 4.26 4.27 4.28 4.29 4.30 4.31 4.32 Simpson MMR. Benign Joint Hypermobility Syndrome: Evaluation, Diagnosis, and Management. J Am Osteopath Assoc. 2006;106(9): 531–536.
- ↑ 5.0 5.1 5.2 Ross J, Grahame R. Joint hypermobility syndrome. BMJ. 2011; 342: c7167.
- ↑ Russek LN. Hypermobility Syndrome, Physical Therapy. 1999; 79(6): 591-9.
- ↑ Magnusson SP, Julsgaard C, Aagaard P, Zacharie C, Ullman S, Kobayasi T et al.Viscoelastic properties and flexibility of the human muscle-tendon unit in benign joint hypermobility syndrome. The Journal of Rheumatology. 2001; 28(12): 2720-5.
- ↑ Kozanoglu E, Coskun Benlidayi I, Eker Akilli R, Tasal A. Is there any link between joint hypermobility and mitral valve prolapse in patients with fibromyalgia syndrome?. Clin Rheumatol. 2016; 35(4):1041-1044.
- ↑ Parvaneh VJ, Shahvaladi H, Rahmani K, et al. Correlation between benign joint hypermobility syndrome and primary focal hyperhidrosis in children: a novel concept. BMC Musculoskelet Disord. 2020;21(1):268.
- ↑ 10.0 10.1 10.2 10.3 Boudreau PA, Steiman I, Mior S. Clinical management of benign joint hypermobility syndrome: a case series. J Can Chiropr Assoc. 2020;64(1):43-54.
- ↑ Remvig L, Jensen DV, Ward RC. Epidemiology of general joint hypermobility and basis for the proposed criteria for benign joint hypermobility syndrome: review of the literature. The Journal of Rheumatology. 2007; 34(4): 804-9.
- ↑ Gedalia A, Brewer EJ Jr. Joint hypermobility in pediatric practice--a review. The Journal of Rheumatology.1993. 20(2): 371-374.
- ↑ 13.0 13.1 de Inocencio AJ, Ocaña CI, Benito OL. Laxitud articular: prevalencia y relación con dolor musculosquelético [Joint hypermobility: prevalence and relationship with musculoskeletal pain]. An Pediatr (Barc). 2004; 61(2):162-166.
- ↑ Kumar B, Lenert P. Joint Hypermobility Syndrome: Recognizing a Commonly Overlooked Cause of Chronic Pain. The American Journal of Medicine. 2017; 130(6): 640-7.
- ↑ 15.0 15.1 Scheper MC, de Vries JE, Verbunt J, Engelbert RH. Chronic pain in hypermobility syndrome and Ehlers-Danlos syndrome (hypermobility type): it is a challenge. J Pain Res. 2015; 8:591-601.
- ↑ McCormack M, Briggs J, Hakim A, Grahame R. Joint laxity and the benign joint hypermobility syndrome in student and professional ballet dancers. The Journal of Rheumatology. 2004; 31(1): 173-178.
- ↑ Tinkle BT, Bird HA, Grahame R, Lavallee M, Levy HP, Sillence D. The lack of clinical distinction between the hypermobility type of Ehlers–Danlos syndrome and the joint hypermobility syndrome (a.k.a. hypermobility syndrome). Am J Med Genet Part A. 2009. 149A: 2368-70.
- ↑ Palmer S, Bailey S, Barker L, Barney L, Elliott A. The effectiveness of therapeutic exercise for joint hypermobility syndrome: a systematic review. Physiotherapy. 2014; 100(3): 220-7.
- ↑ 19.0 19.1 Pacey V, Tofts L, Adams RD, Munns CF, Nicholson LL. Exercise in children with joint hypermobility syndrome and knee pain: a randomised controlled trial comparing exercise into hypermobile versus neutral knee extension. Pediatr Rheumatol. 2013; 11(1): 30.
- ↑ Sahin N, Baskent A, Cakmak A, Salli A, Ugurlu H, Berker E. Evaluation of knee proprioception and effects of proprioception exercise in patients with benign joint hypermobility syndrome. Rheumatol Int. 2008; 28(10): 995–1000.
- ↑ Physifun. Physifun Physiball Demo Part 1. Available from: https://www.youtube.com/watch?v=b91bo4rsIP0 [last accessed 14/5/2021]
- ↑ Rehab My Patient. VMO Single leg inner range quadriceps with band. Available from: https://www.youtube.com/watch?v=cxN01SEa8aM [last accessed 14/5/2021]