Chronic Pelvic Pain
Original Editors - Nina Lefeber
Top Contributors - Nina Lefeber, Kim Jackson, Laura Ritchie, Khloud Shreif, Andeela Hafeez, Admin, Nicole Hills, Aminat Abolade, 127.0.0.1, WikiSysop, Vidya Acharya, Rachael Lowe, Evan Thomas and Melissa Coetsee
[See also Pregnancy Related Pelvic Pain]
[See also Chronic Pelvic Pain Syndrome - Male]
Definition/Description[edit | edit source]
Chronic pelvic pain is commonly defined as non-malignant intermittent or continuous pain in the lower abdomen, pelvis or intrapelvic structures, lasting at least 3–6 months.[1] If non-acute and central sensitization pain mechanisms are present, the condition is considered chronic, regardless of the time frame.[2] Central sensitization is characterized by amplification or increased sensory perception, where stimuli that are normally not painful are now perceived as painful.[3] Chronic pelvic pain in women is not exclusively associated with the menstrual cycle, sexual intercourse or pregnancy[1], and is severe enough to cause functional disability and/or to lead to medical care and intervention.[4]
Anatomy Background[edit | edit source]
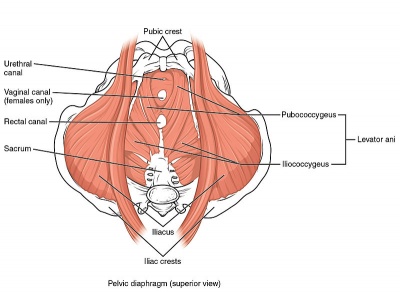
Muscles of pelvic floor muscles divide generally into superficial and deep layers, the superficial is the muscles of the external anal sphincter. Levator ani muscels are the deep pelvic floor muscles and consist of ( puborectalis, pubococcygeus, and iliococcygeus). In addition to pelvic fascia covering all these muscles.
Epidemiology[edit | edit source]
Epidemiologically chronic pelvic pain (CPP) has a greater incidence in women than in men and primarily occurs in individuals between the ages of 36 and 50 years.[2] The etiology of chronic pelvic pain is often not understood[5]. It can be difficult and complex to determine the cause of pain, hence it is very difficult to detect the epidemiology and prevalence of CPP in population facts. It is estimated to be about 25% in reproductive-age women.
Etiology of Chronic Pelvic Pain[edit | edit source]
There is no specific cause for CPP and many women are not able to identify a specific set of problems that can cause symptoms and allow for the diagnosis to be made.[6] CPP may originate from one or more organ systems or pathologies and may have multiple contributing factors.
It usually involves an interaction between the gastrointestinal, urinary, gynecological (endometriosis, adenomyosis, pelvic congestion syndrome, fibroids, and ovarian remnant after surgeries for examples), musculoskeletal such as (tension of pelvic floor muscles, inflammation of the pubic symphysis), neurological and endocrine systems. It can also be influenced by psychological and sociocultural factors.[4]
Characteristics/Clinical Presentation[edit | edit source]
Chronic pelvic pain has numerous presentations, and women with the same problem may exhibit different characteristics. Common symptoms include:
- Constant severe pelvic pain
- Intermittent pain
- Sharp or cramping pain
- Dull aching
- Pressure
Many women miss work, have difficulty doing non-strenuous exercises, and have difficulty sleeping. The level of pain can vary greatly and can contrast from mild to disabling.[6]
Differential Diagnosis[edit | edit source]
| Gastrointestinal | Celiac disease, colitis, colon cancer, inflammatory bowel disease, irritable bowel syndrome |
| Gynaecological | Adhesions, adenomyosis, adnexal cysts, chronic endometritis, dysmenorrhea, endometriosis, gynecologic malignancies, leiomyomata pelvic congestion syndrome, pelvic inflammatory disease |
| Musculoskeletal | Degenerative disk disease, fibromyalgia, levator ani syndrome, myofascial pain, peripartum pelvic pain syndrome, stress fractures |
| Psychiatric/neurological | Abdominal epilepsy, abdominal migraines, depression, nerve entrapment, neurologic dysfunction, sleep disturbances, somatization |
| Urological | Bladder malignancy, chronic urinary tract infection, interstitial cystitis, radiation cystitis, urolithiasis |
| Other | Familial Mediterranean fever, herpes zoster, porphyria |
Examination[edit | edit source]
Musculoskeletal examination to exclude different musculoskeletal disorders such as examination and assessment for pelvic girdle pain, posture assessment, and lumbar for example, assessment if it's neuropathic pain in origin or not is also important.
Pain assessment[8]:
- QoL questionnaire.
- Visual analogue scale VAS.
- Mc Gill Pain Questionnaire (MPQ).
- Neuropathic Pain Assessment Questionnaires (LANSS Pain Scale for example)
Pelvic Examination[edit | edit source]
A pelvic examination done by a physician may reveal signs of infection, abnormal growths, or tense pelvic floor muscles. During this exam, the physician will check for areas of tenderness and changes in sensation. During pelvic examination, there are two methods; bimanual pelvic examination and speculum examination.
Examination of external genitalia for any signs of infection, inflammation, vulvar malignancy
The patient should let their physician know if they feel any pain during this exam, especially if the pain is similar to the discomfort they have been experiencing.
Diagnostic Procedures[edit | edit source]
Cultures[edit | edit source]
Laboratory analysis of cell samples from the cervix or vagina can detect infections, such as chlamydia, gonorrhoea, or culture studies for Trichomonas infections need to be done.
Imaging Tests[edit | edit source]
Ultrasound scan US: This test uses high-frequency sound waves to produce precise images of structures within the body. It is also used to detect hydrosalpinx, an indicator of pelvic inflammatory disease. Abdominal X-rays, computerized tomography (CT) scans or magnetic resonance imaging (MRI) to help detect abnormal structures or growths.
Laparoscopy[edit | edit source]
During a laparoscopy, the physician makes a small incision in the patient's abdomen and inserts a thin tube attached to a small camera (laparoscope). The laparoscope allows the doctor to view the pelvic organs and check for abnormal tissues or signs of infection in the pelvis. This procedure is especially useful in detecting endometriosis and chronic pelvic inflammatory disease. Laparoscopy is an invaluable tool in the diagnosis of chronic pelvic pain in adolescents and should be performed before starting a psychiatric evaluation or prescribing long-term medical treatment.
Medical Management[edit | edit source]
Treatment of chronic pelvic pain is complex in patients with multiple problems. It generally depends on pain relief medication (NSAID), anti-congestive, antibiotics, or antidepressant medications.[10]
- Initially, pain may respond to simple over-the-counter (OTC) analgesics such as paracetamol, ibuprofen, aspirin, or naproxen. If treatment results are unsatisfactory, the addition of other modalities or the use of prescription drugs is recommended.
- If possible, avoid the use of barbiturate or opiate agonists. Also, discourage long-term use and overuse of all symptomatic analgesics because of the risk of dependence and abuse.
- Tizanidine may improve the inhibitory function in the central nervous system and can provide pain relief. Therapy with tizanidine is not considered the standard of care
- Amitriptyline (Elavil) and nortriptyline (Pamelor) are the tricyclic antidepressants (TCAs) used most frequently for chronic pain.
- The selective serotonin reuptake inhibitors (SSRIs) fluoxetine (Prozac), paroxetine (Paxil), and sertraline (Zoloft) also are commonly prescribed. Other antidepressants such as doxepin, desipramine protriptyline, and buspirone also can be used.[11]
Physical Therapy Management[edit | edit source]
The optimal treatment of chronic pelvic pain is based on a biopsychosocial model delivered by a multidisciplinary approach. This multidisciplinary treatment includes oral analgesics and other medications, pain management, pelvic floor rehabilitation, nerve stimulation therapies, teaching cognitive coping strategies, education about the importance of planning and pacing exercise and activities.[3]
Pelvic Floor Rehabilitation[edit | edit source]
Increasing evidence suggests that pelvic floor muscle dysfunction is associated with chronic pelvic pain. Montenegro and colleagues[12] found a significant difference between the prevalence of pelvic floor muscle pain in women with multiple chronic pelvic pain conditions when compared to healthy women. This finding suggests a relationship between the presence of an organic pain condition and pelvic floor pain. A recent (2010) systematic review concluded that myofascial pain in the PFMs is associated with several different CPP conditions that occur in women.[2]
Therefore, pelvic floor rehabilitation is a part of the treatment. Common treatment interventions include:[2]
- Manual therapy of the pelvic floor muscles
- Biofeedback (EMG biofeedback and Kegel perineometer)
- Electrical stimulation (Electro-Acupuncture[13],Percutaneous tibial nerve stimulation[14])
- Myofascial release of painful trigger points of the pelvic floor divided into internal release by Thiele massage techniques and external release.
- Relaxation techniques.
- Pelvic Floor Muscles exercises and core stabilization
- Specific stretches (pelvic floor muscles, adductors, or iliopsoas for example)
- Postural correction.
Physiotherapy and Kegel Exercises[edit | edit source]
Kegel exercises for females and males have been indicated as beneficial in treating CPP, especially where urinary incontinence is one of the symptoms when combined with other physiotherapy modalities[15]. However, there is still no clear evidence that Kegel exercises alone are effective in easing symptoms of Chronic Pelvic Pain[16], In the following presentation Carolyn Vandyken, a physiotherapist who specializes in the treatment of male and female pelvic dysfunction, reviews pelvic anatomy, the history of Kegel exercises, and what the evidence tells us about when Kegels are and aren't appropriate for our patients.
Physiotherapy and Pain Management[edit | edit source]
Pain management and cognitive coping strategies should include education about how psychological factors, such as catastrophizing, pain-related fear, and anxiety, may affect sexual function and the perception of pain during intercourse and other activities for which patients may report pain.[7]
Pain management should also include educating patients about the importance of planning and pacing exercise and activities. The goal is to enable patients to pace their activity to achieve a similar amount each day. Overactive patients may experience constant pain with exacerbations called flare-ups, while others may have constant pain with flare-ups associated with minimal activity.[3]
In addition, therapy can include education about vulvodynia, dyspareunia (painful intercourse), muscle relaxation, Kegel exercises, and vaginal dilation. The goals of the therapy are to reduce the fear of pain and other pain-related cognitions associated with intercourse, increase sexual activity level, and decrease pain.[7]
The longitudinal study by Karen Grinberg et al. suggested that Myofascial Physical Therapy (MPT) intervention (which included myofascial trigger point release and connective tissue manipulation techniques) has a positive effect on the multifactorial pain disorder of Chronic Pelvic Pain Syndrome (CPPS)[18].
Resources[edit | edit source]
| [19] | [20] |
References[edit | edit source]
- ↑ 1.0 1.1 Diaz Mohedo E, Baron Lopez FJ, Pineda Galan C, Dawid Milner MS, Suárez Serrano C, Medrano Sanchez E. Discriminating power of CPPQ‐Mohedo: a new questionnaire for chronic pelvic pain. Journal of Evaluation in Clinical Practice. 2013 Feb;19(1):94-9.
- ↑ 2.0 2.1 2.2 2.3 Alappattu MJ, Bishop MD. Psychological factors in chronic pelvic pain in women: relevance and application of the fear-avoidance model of pain. Physical therapy. 2011 Oct 1;91(10):1542-50.
- ↑ 3.0 3.1 3.2 Cambitzi J. Chronic pelvic pain: causes, mechanisms and effects. Nursing Standard. 2011 Jan 19;25(20).
- ↑ 4.0 4.1 Silva GP, Nascimento AL, Michelazzo D, Alves Junior FF, Rocha MG, Reis FJ, Nogueira AA, Poli Neto OB. High prevalence of chronic pelvic pain in women in Ribeirão Preto, Brazil and direct association with abdominal surgery. Clinics. 2011;66(8):1307-12.
- ↑ Vercellini P, Somigliana E, Viganò P, Abbiati A, Barbara G, Fedele L. Chronic pelvic pain in women: etiology, pathogenesis and diagnostic approach. Gynecological Endocrinology. 2009 Jan 1;25(3):149-58.
- ↑ 6.0 6.1 Paulson JD, Paulson JN. Anterior vaginal wall tenderness (AVWT) as a physical symptom in chronic pelvic pain. JSLS: Journal of the Society of Laparoendoscopic Surgeons. 2011 Jan;15(1):6.
- ↑ 7.0 7.1 7.2 Ortiz DD. Chronic pelvic pain in women. American family physician. 2008 Jun 1;77(11):1535-42.
- ↑ Passavanti MB, Pota V, Sansone P, Aurilio C, De Nardis L, Pace MC. Chronic pelvic pain: assessment, evaluation, and objectivation. Pain research and treatment. 2017;2017.
- ↑ Lecturio Medical. Chronic Pelvic Pain – Gynecology | Lecturio. Available from: https://www.youtube.com/watch?v=7Kdy2fgaih4 [last accessed 1/6/2022]
- ↑ Mathias SD, Kuppermann M, Liberman RF, Lipschutz RC, Steege JF. Chronic pelvic pain: prevalence, health-related quality of life, and economic correlates. Obstetrics & Gynecology. 1996 Mar 1;87(3):321-7.
- ↑ Medscape. Chronic Pelvic Pain in Women Treatment & Management. https://emedicine.medscape.com/article/258334-treatment [accessed 1 June 2022]
- ↑ Montenegro ML, Vasconcelos EC, Candido Dos Reis FJ, Nogueira AA, Poli‐Neto OB. Physical therapy in the management of women with chronic pelvic pain. International journal of clinical practice. 2008 Feb;62(2):263-9.
- ↑ Chong OT, Critchley HO, Williams LJ, Haraldsdottir E, Horne AW, Fallon M. The impact of meridian balance method electro-acupuncture treatment on chronic pelvic pain in women: a three-armed randomised controlled feasibility study using a mixed-methods approach. British Journal of Pain. 2018 Nov;12(4):238-49.
- ↑ Istek A, Gungor Ugurlucan F, Yasa C, Gokyildiz S, Yalcin O. Randomized trial of long-term effects of percutaneous tibial nerve stimulation on chronic pelvic pain. Archives of gynecology and obstetrics. 2014 Aug;290(2):291-8.
- ↑ Masterson TA, Masterson JM, Azzinaro J, Manderson L, Swain S, Ramasamy R. Comprehensive pelvic floor physical therapy program for men with idiopathic chronic pelvic pain syndrome: a prospective study. Translational andrology and urology. 2017 Oct;6(5):910.
- ↑ Ferreira PH, Ferreira ML, Maher CG, Herbert RD, Refshauge K. Specific stabilisation exercise for spinal and pelvic pain: a systematic review. Australian Journal of Physiotherapy. 2006 Jan 1;52(2):79-88.
- ↑ Physiopedia. Pelvic Physiotherapy - to Kegel or Not?. Available from: http://www.youtube.com/watch?v=w08iCzxnQBU [last accessed 1/6/2022]
- ↑ Grinberg K, Weissman-Fogel I, Lowenstein L, Abramov L, Granot M. How does myofascial physical therapy attenuate pain in chronic pelvic pain syndrome?. Pain Research and Management. 2019 Dec 12;2019.
- ↑ Stanford Health Care. Pelvic Pain Causes and Treatment. Available from: http://www.youtube.com/watch?v=xnJc-3M9NRQ [last accessed 1/6/2022]
- ↑ innova fisioterapia. Chronic Pelvic Pain Syndrome - AUA 2015. Available from: http://www.youtube.com/watch?v=4dP_jtZvz9w [last accessed 1/6/2022]