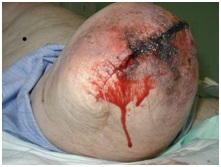
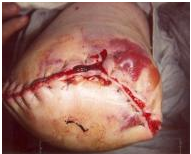
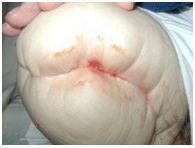
Complications Post Amputation
Original Editor - Lauren Newcombe as part of the World Physiotherapy Network for Amputee Rehabilitation Project
Top Contributors - Sheik Abdul Khadir, Admin, Tarina van der Stockt, Tony Lowe, Kim Jackson, Aicha Benyaich, Lauren Lopez, Olajumoke Ogunleye, Rachael Lowe, Naomi O'Reilly and Andeela Hafeez
Introduction[edit | edit source]
As with any surgery, having an amputation carries a risk of complications. Surgeons will aim to reconstruct the limb to the best of their ability, taking into account soft tissue viability, bone length and other anatomical considerations. However, underlying disease state and post-operative management can result in complications, the most common of which are:
- Oedema
- Wounds and infection
- Pain
- Muscle weakness and contractures
- Joint instability
- Autonomic dysfunction
- Osseointegration specific complications
Low et al.[1] reviewed the data of 2879 patients in the USA who had major lower extremity amputations following trauma injuries to the lower limbs. They discovered a high rate of complications among this patient group and at least 41.8% of these patients had to undergo at least one revision amputation. These patients stayed 5.5 days longer in the hospital when compared to patients who did not undergo a revision. For this population compartment syndrome following the initial trauma was a significant predictor of complications post surgery. [1]
Oedema[edit | edit source]
Stump oedema occurs as a result of trauma and the mishandling of tissues during surgery [2]. After the amputation, there is an imbalance between fluid transfer across the capillary membranes and lymphatic reabsorption [3]. This, in combination with reduced muscle tone and inactivity, can lead to stump oedema. The complications that can arise from stump oedema include wound breakdown, pain, reduced mobility and difficulties with prosthetic fitting.[4]
Numerous interventions are used to manage and prevent post-operative stump oedema, including, compression socks, rigid removable dressings, exercise, wheelchair stump boards, and PPAM aiding. The BACPAR post operative oedema guidance (2012) details the evidence behind these interventions and recommends the use of rigid removable dressings where expertise, time and resources allow. Also according to this guideline the PPAM aid, stump boards, and compression socks have some evidence for oedema control but it is not their main function. [5] See Acute post-surgical management of the amputee for more information.
Wounds and Infection[edit | edit source]
Surgical site infection after amputation is common and as well as increasing patient morbidity, can have negative effects on healing, phantom pain and time to prosthetic fitting [6]. Risk factors for a stump infection include diabetes mellitus, old age and smoking, which are all common denominators amongst the amputee population [7]. The decision to insert a drain and use clips instead of sutures is also associated with increased infection risk.
Literature suggests a post-operative infection rate ranging from 12-70% in the UK [7] but this is widely due to the variation in the classification of stump wounds. The Centre for Disease Control (CDC) Surgical Site Infection (SSI) Criteria (2008) aims to make this classification more standardised[8]:
| Superficial Incisional surgical site infection | Deep Incisional surgical site infection |
|---|---|
|
A Superficial Incisional surgical site infection must meet the following criterion :
|
A Deep Incisional surgical site infection meets the following criterion :
|
The potential consequences of infection include vac therapy, wound debridement and revision surgery. This can increase hospital length of stay and the risk of secondary morbidities such as pneumonia or reduced function. Wounds should be inspected regularly so that any signs of infection can be detected.
The wound may also open up along the surgical line (dehiscence). This happens when the wound is not strong enough to resist the forces placed on it and could result in muscle and bone is exposed. These forces include a direct fall (most common), trauma, or shearing. Other causes may include removing the sutures too soon or swelling of the residual limb. Surgical intervention is usually indicated with total dehiscence. [9]
The following types of wounds may be encountered:
Tissue Necrosis[edit | edit source]
Poor tissue perfusion leads to ischaemia and necrosis. Dusky skin changes, mottled discolouration and slough can be observed. This can lead to subsequent wound breakdown and dehiscence [9]. Depending on the extent of non-viable tissue, wound debridement or revision surgery is often necessary.
Skin Blisters[edit | edit source]
Wound oedema, reduced elasticity or tight stump dressings, and adhesive dressings applied with tension can all increase the friction of the epidermis and cause blistering of the skin. Blisters can also be formed due to infection, traction, and an allergic reaction. [9]
Sinuses and Osteomyelitis[edit | edit source]
A deep, infected sinus can often mask osteomyelitis and delay healing. The sinus can extend from the skin to the subcutaneous tissues and management often includes aggressive antibiotic therapy. Sometimes, surgery is an option, however, this can impact on the shape of the stump and rehabilitation outcomes [9]
More information on wound healing following lower limb amputation from The American Academy of Orthotists & Prosthetists.
Pain[edit | edit source]
Pain is an inevitable consequence of amputation. There are several types of sensations following an amputation that should be discussed when referring to pain following amputation. Some of them are extremely painful and terribly unpleasant; some are simply weird or disconcerting. In one form or another, they are experienced by most people following an amputation.
Post amputation pain can be isolated to the residual limb or can occur as phantom pain. For many, the pain will not just result from the trauma of the surgery, but will also include a neuropathic presentation known as phantom limb pain (PLP). When amputation has resulted from a traumatic incident, such as in a disaster setting, this can be complicated by co-existing injury to the same limb or other parts of the body. For the physiotherapists involved in the early and post acute stages of rehabilitation, the challenge is determining the nociceptive and neuropathic causes which require attention in order to manage the patient and so enable effective rehabilitation to occur.
- Post-Amputation Pain: Post-amputation pain at the wound site should be distinguished from pain in the residual limb and the phantom limb. After amputation, all three may occur together[10]
- Residual Limb Pain (RLP): Patients can often feel pain or sensations in the areas adjacent to the amputated body part. This is known as residual limb (RLP) or stump pain. It is often confused with and its intensity is often positively correlated with PLP[11].
- Phantom Limb Sensation: This is a normal experience for the majority of amputees, but it is not a noxious sensation, which might be described by the patient as unpleasant. Often it can be described as a light tingling sensation, or in such cases, re-assurance is the key[12].
- Phantom Limb Pain (PLP): Classified as neuropathic pain, whereas RLP and post-amputation pain are classified as nociceptive pain. PLP is often more intense in the distal portion of the phantom limb and can be exacerbated or elicited by physical factors (pressure on the residual limb, time of day, weather) and psychological factors, such as emotional stress. Commonly used descriptors include sharp, cramping, burning, electric, jumping, crushing and cramping.
In addition to these 4 pain types that can be experienced following amputation, clinicians should also be aware of the pain that may be caused by co-existing pathology:
- Vascular pain - such as exercise-induced claudication or pain caused by vascular disease
- Musculoskeletal pain - pain from other injuries suffered during a traumatic amputation, musculoskeletal pain caused by abnormal gait patterns, pain caused by normal ageing processes, or excessive wear and tear on the joints and soft tissue of the residual limb.
- Neuromas - localized pain, sharp/shooting/paraesthesia reproduced by local palpation and Tinel's sign, relieved by LA injection.
Prosthetic pain is also a concern and may be caused by:
- Ill-fitting socket - lack of distal contact, insufficient bony relief, too tight, too loose, pistoning causing friction/blisters
- Incorrect alignment and pressure distribution
- Incorrectly donned prosthesis, including the number/thickness of socks
- Excessive sweating/skin breakdown Verrucous hyperplasia
Treatments[edit | edit source]
A large variety of medical/surgical and non-medical methods exist for the treatment of post-amputation pain:
- Adequate post-op analgesia
- Patient education
- Limit oedema
- Prevent contractures
- Address musculoskeletal weakness and imbalances
- Desensitisation - massage/bandaging
- Get patient moving, distraction helps
- Early prosthetic training
Below Peter Le Feurve, a physiotherapist with an interest in pain talks about pain management in amputees;
Read more about Pain management in amputees
Read about Phantom Limb Pain
Read about Mirror Therapy and Graded Motor Imagery
Muscle Weakness, Contractures and Joint Instability[edit | edit source]
After amputation, it is not uncommon for patients to experience pain, muscle weakness or instability in structures not directly associated with the amputation. These compensatory structures are the muscles and joints that are required to perform additional functions post amputation, often resulting in stiffness, spasm or pain.
The effects of bed rest and reduced mobility are also well documented. Deconditioning results in diminished muscle mass, sarcomere shortening, reduced muscle strength and changes in cartilaginous structures [13]. It is, therefore, crucial, that amputee patients undertake functional rehabilitation and personalised exercise programmes from as early as day 1 post surgery. Hip flexion contractures and knee flexion contractures are common complications post amputation and can impact significantly on prosthetic rehabilitation.
ROM exercises should be incorporated to avoid contractures, as well as prone lying to prevent hip flexion contractures, a sandbag could be placed next to the residuum to prevent a hip abduction contracture. A sandbag could also be placed on the lower part of a transtibial residuum when the patient is prone, to prevent hip flexion contractures.[14].
Physiotherapy regimes should consist of the following elements:
- Range of movement exercises
- Strengthening exercises
- Stretches
- Core stability exercises
- Early mobility practice
- Transfer practice
- Balance exercises
- PPAM aiding and gait re-education
Autonomic Dysfunction[edit | edit source]
Complex regional pain syndromes (CRPS) are neuropathic pain disorders developing as a disproportionate consequence of trauma affecting the limbs [17]. Symptoms include distal pain, allodynia and autonomic and motor dysfunction. The residual limb can appear hot, swollen and trophic due to altered control of the sympathetic nervous system.
Due to the lack of understanding about the pathophysiological abnormalities underlying CRPS, treatment should be multi-disciplinary and comprise of neurologists, physiotherapists and psychologists to name but a few. Anti-depressants are proven to be beneficial in reducing neuropathic pain [18] alongside nerve blocks, TENS, graded exercise and mobilisation.
Osseointegration Specific Complications in Trans Femoral Patients[edit | edit source]
Rare major complications
Common minor complications:
Resources[edit | edit source]
Musculoskeletal Complications in Amputees: Their Prevention and Management
References[edit | edit source]
- ↑ 1.0 1.1 Low EE, Inkellis E, Morshed S. Complications and revision amputation following trauma-related lower limb loss. Injury. 2017 Feb 1;48(2):364-70. (abstract)
- ↑ Elizabeth Bouch, Katie Burns, Elizabeth Geer, Matthew Fuller and Anna Rose. Guidance for the multi disciplinary team on the management of postoperative residuum oedema in lower limb amputees. BACPAR
- ↑ Airaksinen, O., Kolari, P.J., Herve, R. and Holopainen, R. (1988) Treatment of post- traumatic oedema in lower legs using intermittent pneumatic compression. Scandinavian Journal of Rehabilitation Medicine, 20(1), pp.25-28
- ↑ Engstrom, B and Van de Ven, C (1999). Therapy for Amputees. Churchill Livingstone.
- ↑ Bouch E, Burns K, Geer E, Fuller M, Rose A. Guidance for the mulfi-disciplinary team on the management of post-operafive residuum oedema in lower limb amputees. BACPAR post operative oedema guidance (2012) [Accessed 10 Oct 2017]
- ↑ Coulston, J E, Tuff V, Twine C P, Chester J F, Eyers P S and Stewart A H R (2012) Surgical Factors in the Prevention of Infection Following Major Lower Limb Amputation. European Journal of Vascular and Endovascular Surgery, 43 (5), pp.556-560
- ↑ 7.0 7.1 Mcintosh J and Earnshaw J J (2009) Antibiotic Prophylaxis for the Prevention of Infection after Major Limb Amputation. European Journal of Vascular and Endovascular Surgery. 37 (6) pp.696-703
- ↑ http://www.cdc.gov/HAI/ssi/ssi.html
- ↑ 9.0 9.1 9.2 9.3 Harker J. Wound healing complications associated with lower limb amputation. World Wide Wounds. 2006 Sep;9. Available at: www.worldwidewounds.com [Accessed 10 Oct 2017]
- ↑ CM, Kooijmana Dijkstra PU, Geertzena JHB, et al. Phantom pain and phantom sensations in upper limb amputees: an epidemiological study. Pain 2000;87:33–41
- ↑ MacIver K, Lloyd DM, Kelly S, et al. Phantom limb pain, cortical reorganization and the therapeutic effect of mental imagery. Brain 2008;131:2181–91.
- ↑ Le Feuvre P, Aldington D. Know Pain Know Gain: proposing a treatment approach for phantom limb pain. J R Army Med Corps 2014; 160(1):16-21
- ↑ Gillis A and Macdonald B (2005) Deconditioning in the hospitalised elderly. Canadian Nurse. Vol 101 (6)pp. 16-20
- ↑ Pasquina PF, Miller M, Carvalho AJ, Corcoran M, Vandersea J, Johnson E, Chen YT. Special considerations for multiple limb amputation. Current physical medicine and rehabilitation reports. 2014 Dec 1;2(4):273-89. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4228106/ (Accessed 11 Nov 2017)
- ↑ Ottobock. Muscle contractures after amputation. Jan 2019.
- ↑ Ottobock. How to prevent muscle contractures after amputation with stretching exercises? Jan 2019
- ↑ Wasner G, Schattsneider J, Binder A and Baron R (2003) Complex regional pain syndrome-diagnostic mechanisms, CNS involvement and therapy. Spinal Cord. Vol 41. pp. 61-75
- ↑ Max MB et al. Effects of desipramine, amitriptyline, and fluoxetine on pain in diabetic neuropathy. N Engl J Med 1992; 326: 1250
- ↑ 19.0 19.1 Li Y, Brånemark R. Osseointegrated prostheses for rehabilitation following amputation. Der Unfallchirurg. 2017 Apr 1;120(4):285-92.
- ↑ 20.0 20.1 Atallah R, Leijendekkers RA, Hoogeboom TJ, Frölke JP. Complications of bone-anchored prostheses for individuals with an extremity amputation: A systematic review. PloS one. 2018 Aug 9;13(8):e0201821.