Lumbar Assessment
Original Editors - Ben Vandoorne
Top Contributors - Admin, Rachael Lowe, Kim Jackson, Laura Ritchie, Jess Bell, Vandoorne Ben, Carin Hunter, Naomi O'Reilly, Kai A. Sigel, Lucinda hampton, Aminat Abolade, Evan Thomas, Simisola Ajeyalemi, 127.0.0.1, Rishika Babburu, WikiSysop and Wanda van Niekerk
Introduction[edit | edit source]
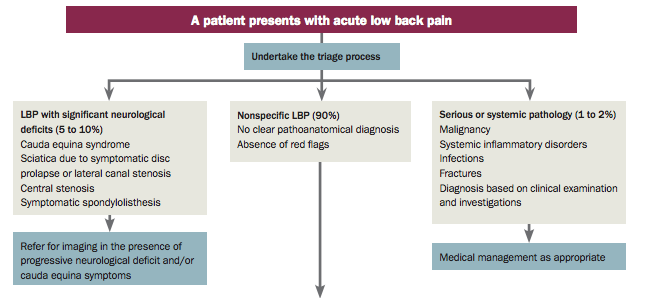
The first aim of the physiotherapy examination for a patient presenting with back pain is to classify them according to the diagnostic triage recommended in international back pain guidelines.[1] Serious conditions (such as fracture, cancer, infection and ankylosing spondylitis) and specific causes of back pain with neurological deficits (such as radiculopathy, caudal equina syndrome) are rare,[2] but it is important to screen for these conditions.[1][3] Serious conditions account for 1-2% of people presenting with low back pain.[4] In around 5-10% of people with low back pain, their pain may be associated with radicular features.[4] When serious and specific causes of low back pain have been ruled out, individuals are said to have non-specific (or simple or mechanical) back pain.
Non-specific low back pain accounts for over 90% of patients presenting to primary care with low back pain[5][6] - these make up the majority of individuals with low back pain who present for physiotherapy. A physiotherapy assessment aims to identify impairments that may have contributed to the onset of the pain, or which increase the likelihood of developing persistent pain. These include biological factors (eg. weakness, stiffness), psychological factors (eg. depression, fear of movement and catastrophisation) and social factors (eg. work environment).[7] The assessment does not focus on identifying anatomical structures (eg. the intervertebral disc) as the source of pain, as might be the case in peripheral joints such as the knee.[7] Previous research and international guidelines suggest it is not possible or necessary to identify the specific tissue source of pain for the effective management of mechanical back pain.[1][3][8]
The subjective assessment (history taking) is a key part of the assessment, with the objective assessment (clinical testing) confirming or refuting the hypothesis formed from the subjective interview.
Triage[edit | edit source]
Lumbar assessment starts with triage.
For this, you'll need knowledge of Red Flags and conditions that can cause neurological deficits:
- Specific Low Back Pain
- Cauda Equina Syndrome
- Lumbar Radiculopathy
- Disc Herniation
- Spinal Stenosis
- Spondylolisthesis
Subjective[edit | edit source]
The subjective examination is one of the most powerful tools a clinician can utilise in the examination and treatment of patients with low back pain. The questions asked during this process can improve the clinician’s confidence that they have identified sinister pathology warranting outside referral. It allows them to screen for yellow flags which may impact specific physiotherapy interventions, and assists in matching physiotherapy interventions with a patient’s symptoms.
A patient history is not only is the record of past and present pain / issues, but also constitutes the basis of future treatment, prevention, and prognosis.
Patient Intake[edit | edit source]
- Self‐report (present complaint (PC), history of present complaint (HPC), past medical history (PMH), drug history (DH), social history (SH))
- Region‐specific questions
- What is the patient’s age?
- What is the patient’s occupation?
- What was the mechanism of injury?
- How long has the problem bothered the patient?
- Where are the sites and boundaries of pain?
- Is there any radiation of pain? Is the pain centralising or peripheralising
- Is the pain deep? Superficial? Shooting? Burning? Aching?
- Is the pain improving? Worsening? Staying the same?
- Is there any increase in pain with coughing? Sneezing? Deep breathing? Laughing?
- Are there any postures or actions that specifically increase or decrease the pain or cause difficulty? Is the pain worse in the morning or evening? Does the pain get better or worse as the day progresses? Does the pain wake you up at night? Which movements hurt? Which movements are stiff?
- Is paresthesia (a “pins and needles” feeling) or anesthesia present?
- Has the patient noticed any weakness or decrease in strength? Has the patient noticed that his/her legs have become weak while walking or climbing stairs?
- What are the patient’s usual activities or pastimes? Before the injury, did the patient modify or perform any unusual repetitive or high-stress activity?
- Which activities aggravate the pain? Is there anything in the patient’s lifestyle that increases the pain?
- Which activities ease the pain?
- What is the patient’s sleeping position? Does the patient have any problems sleeping?
- Does the patient have any difficulty with micturition (i.e. urination)?
- Are there any red flags that the examiner should be aware of, such as a history of cancer, sudden weight loss for no apparent reason, immunosuppressive disorder, infection, fever, or bilateral leg weakness?
- Is the patient receiving any medication?
- Is the patient able to cope during daily activities?
Special Questions[edit | edit source]
Red Flags[edit | edit source]
Although uncommon, serious spinal conditions (such as those listed below) may present as low back pain in approximately 5% of patients presenting to a primary care office:[9]
- Cauda equina syndrome
- Cancer
- Ankylosing spondylitis
- Lumbar stenosis
- Lumbar disc herniations
- Vertebral fracture
- Spinal infection
- Abdominal aortic aneurysm
During your assessment, you must pay attention to any ‘red flags’ that might be present as these can indicate serious pathology. Red flags can be concomitant with mechanical back pain.[10] Koes et al.[11] identified the following ‘red flags’:
- Onset age < 20 or > 55 years
- Non-mechanical pain (unrelated to time or activity)
- Thoracic pain
- Previous history of carcinoma, steroids, HIV
- Feeling unwell
- Weight loss
- Widespread neurological symptoms
- Structural spinal deformity
To learn more aobut red flags, please see: Red Flags in Spinal Conditions and An Introduction to Red Flags in Serious Pathology.
Other Flags[edit | edit source]
It is also important to screen for other (yellow, orange, blue and black) flags as these may interfere with physiotherapy interventions.
To read more about the types of flags, please see: The Flag System.
Outcome Measures[edit | edit source]
There are many outcome questionnaires that can be used for people with back pain to help identify the progress they need to make, have made, and what else you should focus on. It is easy to think you can just get this in your subjective examination. However, a questionnaire is more objective and may elicit information you did not from your objective examination. Further they are a tool to demonstrate more objectively to other entities the efficacy of your treatment.[10]
- Oswestry Disability Index
- Fear Avoidance Belief Questionnaire
- STarT Back Screening Tool
- Acute Low Back Pain Screening Questionnaire
- The Quebec Back Pain Disability Scale
- Hendler 10-Minute Screening Test for Chronic Back Pain Patients
- The Roland-Morris Disability Questionnaire
- Optimal Screening for Prediction of Referral and Outcome (OSPRO)
- Functional Pain Management Society’s Intake questionnaire
Investigations[edit | edit source]
Has the patient had any other investigations such as radiology (X-ray, MRI, CT, ultrasound) or blood tests?
Objective[edit | edit source]
The purpose of the objective examination (clinical testing) is to confirm or refute hypothesis formed from the subjective examination.
Before any objective testing if performed, you need to establish the severity, irritability and nature of the condition.
- Severity relates to the intensity of the symptoms, including subjective pain level
- Irritability can be assessed by establishing the level of activity required to aggravate the symptoms, how severe the symptoms are and how long it then takes for the symptoms to subside. A small movement that causes a large amount of pain that takes a while to subside if known as highly irritable.
- Nature is a broad term relating to the diagnosis, the type of symptoms, personal characteristics/psychosocial factors, red and yellow flags.
For more information, please see Severity, Irritability, Nature, Stage and Stability (SINSS).
When assessing the lumbar spine, the examiner must remember that referral of symptoms or the presence of neurological symptoms often makes it necessary to “clear” or rule out lower limb pathology. Many of the symptoms that occur in the lower limb may originate in the lumbar spine. Unless there is a history of definitive trauma to a peripheral joint, a screening or scanning examination must accompany assessment of that joint to rule out problems within the lumbar spine referring symptoms to that joint.
Examination procedures should be performed from standing-sitting-lying and pain provocation movements saved until last.
Once the subjective and objective examinations are complete, it is important that you identify an asterisk or comparable sign. This can be one of your outcome measures from the subjective examination or a clinical sign that is measurable, reproducible and relevant to the patient's condition. These are used as reassessment tools to measure the progress of a patient's condition.
Observation[edit | edit source]
Movement Patterns[edit | edit source]
- How does the patient enter the room?
- A posture deformity in flexion or a deformity with a lateral pelvic tilt, possibly a slight limp, may be seen.
- How does the patient sit down and how comfortably/ uncomfortably do they sit?
- How does the patient get up from the chair? A patient with low back pain may splint the spine in order to avoid painful movements.
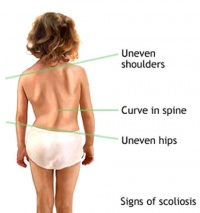
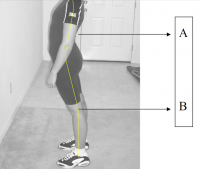
Posture[edit | edit source]
Other observations[edit | edit source]
- Body type
- Attitude
- Facial expression
- Skin
- Hair
- Leg length discrepancy (functional, structural)
Functional Tests[edit | edit source]
- Functional demonstration of pain provoking movements
- Squat test - to highlight lower limb pathologies. This test should not be selected for patients suspected of having arthritis or pathology in the lower limb joints, pregnant patients, or older patients who exhibit weakness and hypomobility. If this test is negative, there is no need to test the peripheral joints (peripheral joint scan) with the patient in the lying position.[12]
Movement Testing[edit | edit source]
- Active range of motion (AROM) (flexion 40-60, extension 20-35, side flexion 15-20 - looking for willingness to move, quality of movement, where movement occurs, range, pain, painful arc, deviation)
- Overpressure (at the end of all AROM if they are pain-free, normal end-feel should be tissue stretch)
- Sustained positions (if indicated by the subjective history)
- Combined movements (if indicated by the subjective history)
- Repeated movements (if indicated by the subjective history)
- Muscle strength (resisted isometrics in flexion, extension, side flexion, rotation; core stability, functional strength tests)
Movement Control Tests[edit | edit source]
Movement control tests[13][14] are a range of tests that can assess lumbar movement control.[15] Individuals who have low back pain and reduced movement control often also demonstrate poor lumbar movement control.[16] A battery of six movement control tests have been found to be a reliable means of assessing lumbopelvic control.[13] These tests are discussed in detail here.
Neurologic Assessment[edit | edit source]
Neurologic assessment is indicated when there is suspicion of neurologic deficit or with any symptoms below the gluteal fold.
- Myotomes
- L2: Hip flexion
- L3: Knee extension
- L4: Ankle dorsiflexion
- L5: Great toe extension
- S1: Ankle plantar flexion, ankle eversion, hip extension
- S2: Knee flexion
- Dermatomes
- Reflexes
- Patellar (L3–L4) (commonly used in clinical practice)
- Medial hamstring (L5–S1) (rarely used in clinical practice)
- Lateral hamstring (S1–S2) (rarely used in clinical practice)
- Posterior tibial (L4–L5)(rarely used in clinical practice)
- Achilles (S1–S2) (commonly used in clinical practice)
- Neurodynamic testing - slump, straight leg raise, prone knee bend and modified versions where appropriate
Circulatory Assessment[edit | edit source]
If indicated, it may be necessary to perform a haemodynamic assessment.
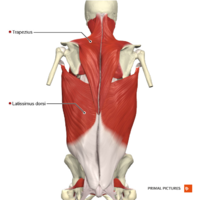
Palpation[edit | edit source]
| [17] |
An important part of the diagnosis of low back pain includes palpation of the lumbar spinous processes. This is commonly performed centrally and unilaterally when using Maitland's techniques in assessment.
There has been debate about the use of palpation in lumbar assessments due to concerns about inter-therapist reliability in identifying each spinous process.[18] However, Snider et al.[19] found that using various landmarks to identify lumbar spinous processes is more accurate than previously suggested. Differences in accuracy were associated with "examiner experience, presence of anatomical anomalies, and participant characteristics."[19] Philips et al.[20] found that when combined with verbal feedback from the participant, manual examination is an accurate method of detecting a patient's affected lumbar segmental level.[20]
Factors that hinder palpation include:
- increased body mass index (BMI)[21]
- anatomical abnormalities (e.g. of the 12th rib leads to decreased accuracy of palpation in the region L1-L4)[22]
Passive Intervertebral Motion[edit | edit source]
Passive Physiological Intervertebral Motion - PPIVM video provided by Clinically Relevant
Passive Accessory Intervertebral Motion-PAIVM video provided by Clinically Relevant
Clear Adjacent Joints[edit | edit source]
| [23] |
- Thoracic spine - seated rotation with combined movements and overpressure
- Sacroiliac joints (SIJ) - various tests have been described to clear the SIJ such as Gillet test, sacral clearing test, cluster tests
- Hips - passive range of motion (PROM) with overpressure
- Knees and ankles - should also be cleared for restrictions that may affect movement patterns
Special Tests[edit | edit source]
For neurological dysfunction:
- Centralisation/ peripheralisation
- Crossed straight leg raise test
- Femoral nerve traction test
- Prone knee bend test or variant
- Slump test variant
- Straight leg raise or variant
For lumbar instability:
- H and I test - demonstrated in video [24]
- Passive lumbar extension test
- Prone segmental instability test
- Specific lumbar torsion test
- Test for anterior lumbar spine instability
- Test for posterior lumbar spine instability
For joint dysfunction:
- Bilateral straight leg raise test
- One-leg standing (stork standing) lumbar extension test
- Quadrant test
For muscle tightness:
- 90–90 straight leg raise test
- Ober's test
- Rectus femoris test
- Thomas test
Other tests:
Brief Examination[edit | edit source]
If you only have a short amount of time, a brief examination of patients with back pain has two basic purposes.
- Firstly it will help screen patients for possible serious spinal pathology even though taking a good history is much more important.
- Secondly, it will improve patient satisfaction and effectiveness of the consultation.
It is suggested that the following be performed as a bare minimum:
- Inspect – general appearance, gross structural deformities
- Active movements – flexion (significant limitation often pathological), extension, side flexion
- Myotomes– rise from a knee squat (L3/4), walk on heels (L4/5) and walk on toes (S1/2)
- Straight leg raise (if there is leg pain or if you feel it is needed for reassurance) +/- slump test
Obviously, if the history raises concerns that there may be non-spinal pain, structural deformity, widespread neurological disorder or serious spinal pathology, it is appropriate to examine the patient more fully as per normal clinical practice.
What Next?[edit | edit source]
Lumbopelvic disorders are not a homogeneous group of conditions, and subgrouping or classification of patients with back pain has been shown to enhance treatment outcomes.[25][26] Classification of lumbopelvic disorders should adequately define the primary signs and symptoms and guide therapeutic interventions. The examination allows us to arrive at a diagnosis and impairment classification for the condition. These classification systems help us to avoid the pitfalls of attempts to identify the pathoanatomic cause of the patient’s symptoms.
Psychosocial Assessment[edit | edit source]
Look out for flags, particularly yellow flags. See The Flag System and General Physiotherapy Assessment for more information.
Psychosocial screening tools such as the STarT Back Screening Tool and Orebro Screening Tool can be useful.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Koes BW, van Tulder M, Lin C-WC, Macedo LG, McAuley J, Maher C. An updated overview of clinical guidelines for the management of non-specific low back pain in primary care. Eur Spine J 2010;19:2075–94
- ↑ Henschke N, Maher CG, Refshauge KM, Herbert RD, Cumming RG, Bleasel J, York J, Das A, McAuley JH. Prevalence of and screening for serious spinal pathology in patients presenting to primary care settings with acute low back pain. Arthritis & Rheumatism: Official Journal of the American College of Rheumatology. 2009 Oct;60(10):3072-80.
- ↑ 3.0 3.1 Van Tulder M, Becker A, Bekkering T, Breen A, del Real MT, Hutchinson A, Koes B, Laerum E, Malmivaara A, COST B13 Working Group on Guidelines for the Management of Acute Low Back Pain in Primary Care. European guidelines for the management of acute nonspecific low back pain in primary care. European spine journal. 2006 Mar;15(Suppl 2):s169.
- ↑ 4.0 4.1 O'Sullivan, P. and Lin, I. Acute low back pain Beyond drug therapies. Pain Management Today, 2014, 1(1):8-14
- ↑ Koes BW, Van Tulder M, Thomas S. Diagnosis and treatment of low back pain. Bmj. 2006 Jun 15;332(7555):1430-4.
- ↑ Traeger A, Buchbinder R, Harris I, Maher C. Diagnosis and management of low-back pain in primary care. CMAJ. 2017 Nov 13;189(45):E1386-E1395.
- ↑ 7.0 7.1 M.Hancock. Approach to low back pain. RACGP, 2014, 43(3):117-118
- ↑ Hancock MJ, Maher CG, Latimer J, Spindler MF, McAuley JH, Laslett M, Bogduk N. Systematic review of tests to identify the disc, SIJ or facet joint as the source of low back pain. European Spine Journal. 2007 Oct 1;16(10):1539-50.
- ↑ Deyo RA, Rainville J, Kent DL. What can the history and physical examination tell us about low back pain?. Jama. 1992 Aug 12;268(6):760-5.
- ↑ 10.0 10.1 Rainey N. Considerations for Lumbar Assessment Course. Plus, 2023.
- ↑ Koes BW, Van Tulder M, Thomas S. Diagnosis and treatment of low back pain. Bmj. 2006 Jun 15;332(7555):1430-4.
- ↑ Magee, D. Lumbar Spine. Chapter 9 In: Orthopedic Physical Assessment. Elsevier, 2014
- ↑ 13.0 13.1 Meier R, Emch C, Gross-Wolf C, Pfeiffer F, Meichtry A, Schmid A, Luomajoki H. Sensorimotor and body perception assessments of nonspecific chronic low back pain: a cross-sectional study. BMC Musculoskeletal Disorders. 2021 Dec;22(1):1-0.
- ↑ Tsunoda Del Antonio T, José Jassi F, Cristina Chaves T. Intrarater and interrater agreement of a 6-item movement control test battery and the resulting diagnosis in patients with nonspecific chronic low back pain. Physiotherapy Theory and Practice. 2022 Mar 4:1-1.
- ↑ Adelt E, Schöttker-Königer T, Luedtke K, Hall T, Schäfer A. Dataset for the performance of 15 lumbar movement control tests in nonspecific chronic low back pain. Data in brief. 2022 Jun 1;42:108063.
- ↑ Khodadad B, Letafatkar A, Hadadnezhad M, Shojaedin S. Comparing the effectiveness of cognitive functional treatment and lumbar stabilization treatment on pain and movement control in patients with low back pain. Sports Health. 2020 May;12(3):289-95.
- ↑ tsudpt11's channel. Maitland Lumbar PAIVM (skeletal model). Available from: http://www.youtube.com/watch?v=t0OCzavA6SY[last accessed 19/08/15]
- ↑ McKenzie AM, Taylor NF. Can physiotherapists locate lumbar spinal levels by palpation?. Physiotherapy. 1997 May 1;83(5):235-9.
- ↑ 19.0 19.1 Snider KT, Snider EJ, Degenhardt BF, Johnson JC, Kribs JW. Palpatory accuracy of lumbar spinous processes using multiple bony landmarks. Journal of manipulative and physiological therapeutics. 2011 Jun 1;34(5):306-13.
- ↑ 20.0 20.1 Phillips DR, Twomey LT. A comparison of manual diagnosis with a diagnosis established by a uni-level lumbar spinal block procedure. Manual therapy. 1996 Mar 1;1(2):82-7.
- ↑ Ferre RM, Sweeney TW. Emergency physicians can easily obtain ultrasound images of anatomical landmarks relevant to lumbar puncture. The American journal of emergency medicine. 2007 Mar 1;25(3):291-6.
- ↑ Snider KT, Snider EJ, Degenhardt BF, Johnson JC, Kribs JW. Palpatory accuracy of lumbar spinous processes using multiple bony landmarks. Journal of manipulative and physiological therapeutics. 2011 Jun 1;34(5):306-13.
- ↑ Physical Therapy Nation. Lumbar and SIJ Examination. Available from: http://www.youtube.com/watch?v=EL5tXj81Q8M[last accessed 19/08/15]
- ↑ PTY621 H and I test Available from: https://www.youtube.com/watch?v=P_N_Sg07XR0 (last accessed 26.11.2019)
- ↑ Brennan GP, Fritz JM, Hunter SJ, Thackeray A, Delitto A, Erhard RE. Identifying subgroups of patients with acute/subacute “nonspecific” low back pain: results of a randomized clinical trial. Spine. 2006 Mar 15;31(6):623-31.
- ↑ Childs JD, Fritz JM, Flynn TW, Irrgang JJ, Johnson KK, Majkowski GR, Delitto A. A clinical prediction rule to identify patients with low back pain most likely to benefit from spinal manipulation: a validation study. Annals of internal medicine. 2004 Dec 21;141(12):920-8.
[[Category:Neurological -