Retrocalcaneal Bursitis
Original Editor - Aarti Sareen
Top Contributors - Aarti Sareen, Kim Jackson, Adam Vallely Farrell, Rachael Lowe, Simisola Ajeyalemi, Admin, WikiSysop, Jess Bell, Khloud Shreif, Evan Thomas, Rucha Gadgil, Claudia Karina, Wanda van Niekerk and Lucinda hampton
Introduction[edit | edit source]
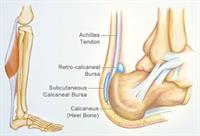
Retrocalcaneal bursitis is the most common heel bursitis. Retrocalcaneal bursitis is the inflammation of the bursa located between the calcaneus and the anterior surface of the Achilles tendon[1].There are two bursae located just superior to the insertion of the Achilles (calcaneal) tendon.[2] Inflammation of either or both of these bursa can cause pain at the posterior heel and ankle region.[3][4][5]
- Anterior or deep to the tendon is the retrocalcaneal (subtendinous) bursa, which is located between the Achilles tendon and the calcaneus[2].
- Posterior or superficial to the Achilles tendon is the subcutaneous calcaneal bursa, also called the Achilles bursa. This bursa is located between the skin and posterior aspect of the distal Achilles tendon.
It is also known as Achilles tendon bursitis. It can often be mistaken for Achilles Tendinopathy or can also occur in conjunction with Achilles tendinopathy.
Clinical Anatomy and pathogenesis[edit | edit source]
A bursa appears at a junction of a tendon on the bone. A bursa is filled with a thin layer of synovial fluid. It protects and brakes the shocks of the joint. The structures nearby the bursa can move with minimal friction due to irritation.
The retrocalcaneal bursa is saddled over the posterior-superior prominence of the calcaneus under the Achilles tendon and its lateral expansions. The Achilles tendon insertion, the fibrocartilaginous walls of the retrocalcaneal bursae that extends into the tendon and the adjacent calcaneum form an "ENTHESIS ORGAN". The key concept is that at this site the tendon insertion, the bursa and the bone are so intimately related that a prominence of the calcaneum will greatly predispose to mechanical irritation of the bursa and the tendon. Also, there is significant strain on the tendon insertion on the posterior aspect of the tendon with dorsiflexion.[6][7]
Epidemiology[edit | edit source]
Retrocalcaneal bursitis is common in both the sporting athlete and the general population. In normal population its incidence is high in individuals who are accustomed to wearing high-heeled shoes on a long-term basis and may experience increased stretch and irritation of the Achilles tendon and its associated bursae when switching to flat shoes.
Causes[edit | edit source]
A retrocalcaneal bursa mat occur traumatically from a fall or a sport related impact contusion or it can also present as a gradual onset due to repetitive trauma to the bursa from activities including running or excessive loading.
- Overtraining in an athlete
- Tight or poorly fitting shoes that produce excessive pressure at the posterior heel
- Haglund deformity
- Altered joint axis
Inflammation of the calcaneal bursae is most commonly caused by repetitive (cumulative) trauma or overuse, and the condition is aggravated by pressure, such as when athletes wear tight-fitting shoes. Retrocalcaneal bursitis may also be associated with conditions such as gout, rheumatoid arthritis, and seronegative spondyloarthropathies. In some cases, retrocalcaneal bursitis may be caused by bursal impingement between the Achilles tendon and an excessively prominent posterosuperior aspect of the calcaneus (Haglund deformity). In Haglund disease, impingement occurs during ankle dorsiflexion.[2]
Sign and Symptoms[edit | edit source]
- Pain at the back of the heel, especially when running uphill
- Pain may get worse when rising on the toes (standing on tiptoes)
- Tenderness at the back of heel
- Swelling at the back of heel
- Increase in pain in activities which load the calf
Clinical Assessment[edit | edit source]
A good clinical practise includes evaluation of the tendon, bursa and calcaneum by, careful history, inspection of the region for bony prominence and local swelling as well as palpation of the area of maximal tenderness. Biomechanical abnormalities, joint stiffness and proximal soft tissue tightening can exacerbate an anatomical predisposition to retrocalcaneal bursitis, they warrant correction when present[7].
Plain radiographs of the calcaneus may reveal a Haglund deformity (increased prominence of the posterosuperior aspect of the calcaneus). However, on weight-bearing lateral radiographs, the retrocalcaneal recess often appears normal even in patients with retrocalcaneal bursitis, limiting its usefulness in making this diagnosis.Radiographs may be used as a diagnostic measure to support a clinician’s diagnosis of retrocalcaneal bursitis. Individuals with retrocalcaneal bursitis may have an absence of the normal radiolucency (ie, blunting) that is seen in the posteroinferior corner of the Kager fat pad, known as the retrocalcaneal recess or bursal wedge. This may occur with or without an associated erosion of the calcaneus.[8][9]
Magnetic resonance imaging (MRI) may demonstrate bursal inflammation, but this modality probably does not offer much more information than that found by careful physical examination. Theoretically, MRI could help the physician to determine whether the inflammation is within the subcutaneous bursa, the subtendinous bursa, or even within the tendon itself; however, such testing is generally not necessary.
Ultrasonography may be a potentially useful tool for diagnosing pathologies of the Achilles tendon.[10]
Differential Diagnosis[11][edit | edit source]
- Posterior ankle impingement
- Haglund deformity
- Achilles tendonitis
- Partial rupture Achilles tendon
- Plantar fasciitis
Treatment[edit | edit source]
Physical Therapy[edit | edit source]
In the acute phase, ice can be applied to the posterior heel and ankle several times a day.
The patient with retrocalcaneal bursitis should be instructed to apply ice to the posterior heel and ankle in the acute period of the bursitis. Icing can be performed several times a day, for 15-20 minutes each. Some clinicians also advocate the use of contrast baths.
Gradual progressive stretching of the Achilles tendon may help relieve impingement on the subtendinous bursa and can be performed in the following manner:
- Stand in front of a wall, with the affected foot flat on the floor. Lean forward toward the wall until a gentle stretching is felt within the ipsilateral Achilles tendon.
- Maintain the stretch for 20-60 seconds and then relax.
- Perform the stretches with the knee extended and then again with the knee flexed.
- To maximize the benefit of the stretching program, repeat the above steps for several stretches per set, several times daily. Avoid ballistic (i.e, abrupt, jerking) stretches.
Other treatment options are microcurrent therapy and corticosteroid injection into the retrocalcaneal bursa
Patient Education[edit | edit source]
It is important to educate the patient on their foot wear
Surgical[edit | edit source]
Whilst rare, in un-resolving cases of retrocalcaneal bursitis may result in a bursectomy where the bursae is removed from the back of the ankle.
Resources[edit | edit source]
References[edit | edit source]
- ↑ Fauci, Anthony (2010). Harrison's Rheumatology, Second Edition. McGraw-Hill Professional Publishing; Digital Edition. p. 271
- ↑ 2.0 2.1 2.2 Brinker MR, Miller MD. The adult foot. Fundamentals of Orthopaedics. Philadelphia, Pa: WB Saunders Co; 1999:342-63.
- ↑ McGee DJ. Lower leg, ankle, and foot. Orthopedic Physical Assessment. 2nd ed. Philadelphia, Pa: WB Saunders Co; 1992:448-515.
- ↑ Snider RK, ed. Foot and ankle. Essentials of Musculoskeletal Care. 2nd ed. Rosemont, Ill: American Academy of Orthopedic Surgeons; 1997:366-489.
- ↑ Young JL, Olsen NK, Press JM. Musculoskeletal disorders of the lower limbs. In: Braddom RL, ed. Physical Medicine and Rehabilitation. Philadelphia, Pa: WB Saunders Co; 1996:783-812.
- ↑ Lyman J, Weinhold PS, Almekinders LC. Strain behaviour of the distal Achilles tendon: Implications for insertional Achilles tendinopathy. Am J Sports Med 2004; 32(2):457-61.
- ↑ 7.0 7.1 Brukner P, Khan Karim. Clinical Sports Medicine. Ch.32. 3rd edition.
- ↑ van Sterkenburg MN, Muller B, Maas M, Sierevelt IN, van Dijk CN. Appearance of the weight-bearing lateral radiograph in retrocalcaneal bursitis. Acta Orthop. Jun 2010;81(3):387-90. [Medline].
- ↑ Ly JQ, Bui-Mansfield LT. Anatomy of and abnormalities associated with Kager's fat Pad. AJR Am J Roentgenol. Jan 2004;182(1):147-54.
- ↑ Blankstein A, Cohen I, Diamant L, et al. Achilles tendon pain and related pathologies: diagnosis by ultrasonography. Isr Med Assoc J. Aug 2001;3(8):575-8.
- ↑ Cook JL, Khan KM, Purdam C. Achilles tendinopathy. Manual Therapy 2002;7(3):121-130.