Sciatic Nerve
Original Editor - George Prudden
Top Contributors - George Prudden, Manisha Shrestha, Kim Jackson, Lucinda hampton, Candace Goh and Joao Costa
Description[edit | edit source]
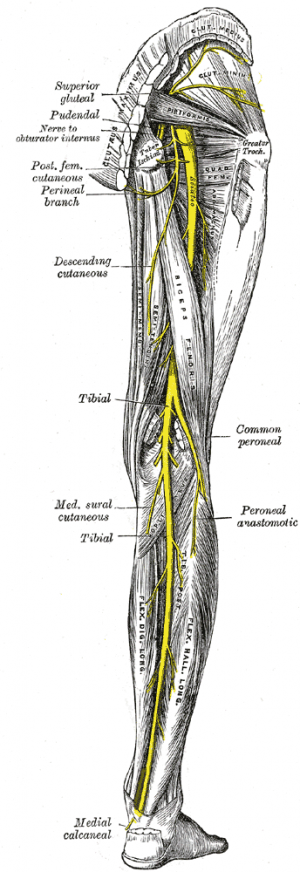
The sciatic nerve is the thickest (approximately 2cm wide) nerve in the body, which travels in the posterior compartment of the thigh and supplies a major part of the lower extremity. At the upper aspect of the popliteal fossa, it branches medially to the Tibial Nerve and laterally to the Common Peroneal Nerve. It is a mixed nerve.[1]
Course[edit | edit source]
It is formed from the ventral rami of the fourth lumbar to third sacral spinal nerves and is a continuation of the upper part of the sacral plexus.[2]
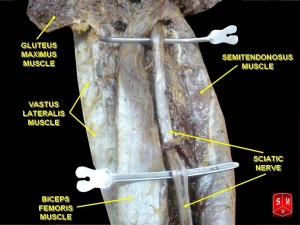
It leaves the pelvis through the greater sciatic foramen, inferior to the Piriformis muscle, and descends between the greater trochanter of the Femur and the ischial tuberosity. Initially deep to piriformis, it runs inferiorly and laterally posterior to the ischium, crossing over the nerve to Quadratus Femoris. Below the piriformis it lies deep to Gluteus Maximus. It passes inferiorly crossing Obturator Internus, the Gemelli Muscles and Quadratus Femoris. The Posterior Femoral Cutaneous Nerve and the Inferior Gluteal Artery lie on its medial side. Descending vertically, it enters the thigh at the lower border of gluteus maximus, where it lies on the posterior surface of Adductor Magnus. Nerves branch off to the hamstring muscles. The nerve is crossed obliquely on its superficial aspect by the long head of Biceps Femoris. The nerve ends at the upper aspect of the popliteal fossa where it branches to distal nerves (tibial and common peroneal nerve).
Prior to diverging, the tibial and common peroneal nerves are structurally separate and only loosely held together as the sciatic nerve. The tibial nerve is derived from the anterior divisions of the sacral plexus, and the common fibular nerve is made up of the posterior divisions of the plexus.
The nerve can be represented on the back of the thigh by a line drawn from just medial to the midpoint of the line from the ischial tuberosity to the apex of greater trochanter down to the apex of popliteal fossa.[3]
Root[edit | edit source]
- L4, L5, S1,S2, S3
Branches[edit | edit source]
- Articular branches arise proximally to supply the hip joint through its posterior capsule, which sometimes may arises from sacral plexus.
- Muscular branches supplies hamstring muscle and ischial part of adductor magnus.
- Distal terminal branches are Tibial nerve and Common peroneal nerve[3]
Blood supply[edit | edit source]
In the gluteal region, the sciatic nerve is supplied by the inferior gluteal artery and cruciate anastomosis (the medial and lateral circumflex femoral arteries, inferior gluteal artery and the first perforating branch of the profunda femoris artery).
Lower in the thigh, arterial branches derived from the perforating branches of the profunda femoris artery or the anastomotic chain between them or, occasionally, from the popliteal artery, enter the nerve on its lateral or anterolateral side.
Function[edit | edit source]
It provides motor innervation to the posterior compartment of the thigh and its terminal branches provide both motor and sensory innervation to leg and foot.
Motor[edit | edit source]
- Hamstrings
- Biceps Femoris
- Semitendinosus
- Semimembranosus
- Adductor magnus- ischial head
- Indirectly innervates (via common peroneal and tibial nerves) the all muscles of the leg and foot.
Sensory[edit | edit source]
- Indirectly innervates (via common peroneal and tibial nerves) the skin of the lateral leg, heel, and both the dorsal and plantar surfaces of the foot.
Assessment[edit | edit source]
Neurological examination is crucial for the assessment of sciatic nerve.
Myotomes[edit | edit source]
Myotomes of lower extremities are:
- Ankle dorsiflexion (L4)
- Extension of the big toe (L5)
- Eversion of the ankle, contraction of buttock and knee flexion (S1)
- Knee flexion and toe standing (S2)
- Pelvic floor, bladder and genital function (S3)[5]
Dermatomes[edit | edit source]
Dermatomes of lower extremities are:
- Over the medial malleolus (L4)
- On the dorsum of the foot at the third metatarsophalangeal joint (L5)
- On the lateral aspect of the calcaneus (S1)
- At the midpoint of the popliteal fossa (S2)
- Over the tuberosity of the ischium or infra-gluteal fold (S3)
Reflexes[edit | edit source]
- Knee jerk (L3 and 4)
- Ankle jerk (S1)
Neurodynamic[edit | edit source]
Neurodynamic tests can be used to assess the mobility of the nervous system. Assessments that stress the sciatic nerve include straight leg raise and slump tests. Whilst performing the neurodynamic movement the following qualities should be noted:
- Resting symptoms
- The quality of movement
- Range of movement
- Resistance through the range and at the end of range
- Behaviour of pain (local and referred)[5]
A test is positive if one or more of the following is found:
- All or part of the patients symptoms are reproduced
- Symptoms different from 'normal' response are produced
- Range of movement in the symptomatic limb is different from that of the contralateral limb.
Sensitising and desensitising movements are essential to rule out any other structures that could be implicated as a source of a patient's pain. When assessing the sciatic nerve the hamstrings are also put on stretch during both tests. Once a position of pain reproduction is identified, dorsiflexion or plantarflexion can be added which will increase and decrease symptoms respectively. Adding dorsiflexion increases the tension on the nerves because they form a continuous structure.
Straight leg raise[edit | edit source]
The Straight Leg Raise Test (SLR) test is a neurodynamic test. Neurodynamic tests check the mechanical movement of the neurological tissues as well as their sensitivity to mechanical stress or compression. These tests, along with relevant history and decreased range of motion, are considered by some to be the most important physical signs of disc herniation, regardless of the degree of disc injury.[6]
Slump[edit | edit source]
Slump test is the nerve tension test for sciatic nerve. It is a provocative test in which sciatic nerve is tensed by flexing spines and hips and extending knees. To begin the test, have the patient seated with hands behind back to achieve a neutral spine. The first step is to have the patient slump forward at the thoracic and lumbar spine. If this position does not cause pain, have the patient flex the neck by placing the chin on the chest and then extending one knee as much as possible.
If extending the knee causes pain, have the patient extend the neck into neutral. If the patient is still unable to extend the knee due to pain, the test is considered positive.
If extending the knee does not cause pain, ask the patient to actively dorsiflex the ankle. If dorsiflexion causes pain, have the patient slightly flex the knee while still dorsiflexing. If the pain is reproduced, the test is considered positive.
Then, the test is repeated on opposite side.
Clinical Relevance[edit | edit source]
There is some variability between the relationship of the sciatic nerve, piriformis muscle and short external rotators. In approximately 85% of cases the sciatic nerve exists as described above. In 11% of individuals a portion of the piriformis muscle splits the common peroneal nerve and tibial nerve. [2]
Piriformis Syndrome[edit | edit source]
Youngman described 'Piriformis Syndrome' in 1928 as compression of the sciatic nerve by the piriformis muscle. This is associated with acute trauma to the buttock and occurs when the sciatic nerve exits posterior to the piriformis. The patient's may report that sitting and activities that require hip flexion or internal rotation as aggravate the pain. The pain radiates in a sciatic nerve distribution.[2]
Objective examination reveals tenderness directly over the piriformis or in the gluteal area, and the pain can be replicated by internal rotation of the extended thigh. This finding is called the 'Pace's sign'. There is sometimes weak abduction or external rotation against resistance. The pain may also be reproduced by rectal or vaginal examination.
Initial medical management is oral anti-inflammatory medication. Steroid injection and surgical exploration may be considered for chronic cases.
Hamstring Syndrome[edit | edit source]
This pathology commonly affects athletes who present with localised and radiating pain near the ischial tuberosity. The pathophysiology is thought to be that of insertional tendinopathy at the ischium but there may also be involvement of sciatic nerve compression. The pain in hamstring syndrome radiates down the posterior thigh or popliteal region and is exacerbated when the hamstrings are in tension.[2] This is often seen in sprinters or hurdlers. On examination there is exquisite tenderness over the ischial tuberosity and percussion in that region may reproduce the sciatic distribution of pain. Treatment involves rest, anti-inflammatory agents and steroid injections.
Hip Dislocation[edit | edit source]
Hip dislocations are most commonly associated high-energy trauma and therefore are often associated with multi-system injuries. It is important to examine for sciatic nerve injuries. The common peroneal division of the sciatic nerve is most commonly involved. Care is needed during assessment as a femoral fracture can mask otherwise obvious hip dislocation.[2]
Surgical Approach for viewing of sciatic nerve injury post hip dislocation[edit | edit source]
Kocher-Langenbeck Approach (Posterior Approach)
- 'Kocher-Langenbeck' approach is the standard posterior approach to the hip joint.
- Performed in a lateral decubitus position without use of a traction table.
- To access the sciatic nerve the gluteus maximus muscle is split, where the nerve can be identified and examined.
- After identifying the sciatic nerve, the tendinous insertions of the piriformis muscle and the obturator internus are identified.
- When surgeons perform capsulotomies they take care not to injure the acetabulum labrum. The joint can then be assessed, any fracture fragments removed or stabilised and the entire area thoroughly washed out.[2]
Anterior Approach
- The anterior approach to the hip for injuries can be performed through the 'Smith Peterson' or 'Watson Jones' approaches.
- These can be performed with the patient in the semi-lateral or lateral decubitus position.[2]
Intramuscular Injections[edit | edit source]
The path of the sciatic nerve must be considered when administering intramuscular injections into the gluteal region. The region can be divided into quadrants using two lines, marked by bony landmarks:
- One line descends vertically from the highest point on the iliac crest.
- The other horizontal line passes through the vertical line half way between the highest point on the iliac crest and ischial tuberosity.
The sciatic nerve passes through the lower medial quadrant. To avoid damaging the sciatic nerve therefore, intramuscular injections are given only in the upper lateral quadrant of the gluteal region.[8]
References[edit | edit source]
- ↑ Giuffre BA, Jeanmonod R. Anatomy, sciatic nerve.[Updated 2020 Apr 23]. StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing. 2020.
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 2.6 Anatomy.tv | 3D Human Anatomy | Primal Pictures [Internet]. Anatomy.tv. 2018 [cited 1 May 2018]. Available from: http://www.anatomy.tv/
- ↑ 3.0 3.1 Gray's anatomy- The anatomical basis of clinical practice. Forty-first edition.
- ↑ Sciatic Nerve - Anatomy Tutorial.Available from: https://www.youtube.com/watch?v=pWl3s6X9cSk
- ↑ 5.0 5.1 Petty NJ, editor. Neuromusculoskeletal Examination and Assessment, A Handbook for Therapists, 4: Neuromusculoskeletal Examination and Assessment. Elsevier Health Sciences; 2011.
- ↑ David J. Magee;Orthopaedic Physical Assessment; Chapter 9-Lumbar Spine;Fifth Edition: Pg 558-564.
- ↑ Slump test for Sciatic Nerve pain. Available from: https://www.youtube.com/watch?v=zdbIa96e-pk lasted accessed: 24th July 2022
- ↑ The Sciatic Nerve [Internet]. TeachMeAnatomy. 2018 [cited 10 May 2018]. Available from: http://teachmeanatomy.info/lower-limb/nerves/the-sciatic-nerve/