Slipped Capital Femoral Epiphysis
Original Editor - Juliana Doyle, Roel De Groef as part of the Vrije Universiteit Brussel's Evidence-based Practice project
Top Contributors - Wanda van Niekerk, Roel De Groef, Nicolas D'Hondt, Admin, Juliana Doyle, Kim Jackson, Daphne Jackson, Vidya Acharya, Anouk Toye and Lucinda hampton
Definition/Description[edit | edit source]
Slipped Capital Femoral Epiphysis (SCFE) is the most common hip disorder affecting adolescents.[1] It is a disorder of the immature hip in which anatomic disruption occurs through the proximal femoral physis. It is characterized by a posterior displacement of the epiphysis through the hypertrophic zone with the metaphysis taking on an anterior and superior position.[2]. The injury is a Salter-Harris type 1 physeal fracture and happens when a shearing force in excess of the strength of the growth is applied to the femoral head.[2] The SCFE deformity exposes the anterior metaphysis and edge of neck to the anterolateral rim and labrum and therefor causing impingement.[3] As a result, there is damage to the anterior acetabular cartilage, the labrum and the rim.[3] This damage usually occurs very early.[3] The extent of articular damage is variable and is influenced by the duration of the slip, the severity of the deformity as well as the activity level of the patient.[3] SCFE is associated with a highly variable degree of posterior translation of the epiphysis and simultaneous anterior displacement of the metaphysis. In SCFE, there is a spectrum of each of the following elements: temporal acuity, physical stability of the slipping physis, degree of displacement between the proximal femoral neck and the epiphysis and the amount of deformity that the protruding anterior metaphyseal prominence presents to the anterior acetabular rim with hip flexion.
Fortunately, SCFE can be treated and the complications averted or minimized if diagnosed early. In most of the cases surgery is necessary to stabilize the hip and prevent the situation from getting worse. [4]
Clinically Relevant Anatomy[edit | edit source]
The hip joint, a ball and socket synovial joint at the juncture of the leg (femur) and pelvis (os coxa), is one of the most flexible joints in the human body. In addition to being flexible, the hip joint must be able to support half of the body’s weight along with any other forces acting upon the body. [5] The hip joint must be able to accommodate these extreme forces repeatedly during intense physical activities. In the femur of a growing child, the femoral growth plates are placed between the epiphysis and metaphysis[6]. As we grow, the growth plate builds bone on top of the end of the metaphysis, which assures bone lengthening.
The strength of the cartilage epiphyseal plate itself is inferior to those of its surrounding bone parts. Subsequently, increased force on the hip at a time when the femoral head is not fully ready to support these forces makes the femoral head fail at the weakest point - through the epiphyseal plate. Furthermore, the capital femoral epiphysis is one of the only epiphyses in the body that is inside its joint capsule. The blood vessels that supplies the epiphysis run along the side of the femoral neck and are in real danger of being torn or pinched off if something happens to the growth plate. When this happens, it can result in a loss of the blood supply to the epiphysis which leads to an avascular necrosis and chondolysis. [7]
Epidemiology / Etiology[edit | edit source]
The prevalence of SCFE is 10.8 cases per 100 000 children.[8][9]SCFE presents bilaterally in 18 to 50 percent of patients[9]. The prevalence is more common in boys than girls and varies widely among ethnic groups (higher prevalence rate in blacks, Hispanics, Polynesians, and Native Americans ), geographic locations (higher rates in the north and western parts of the United States), and different seasons (late summer and fall)[8][9].
Eventhough the pathogenesis is most likely multi-factorial, mechanical factors (mainly obesity and growth surges/abnormal morphology of the proximal femur and acetabulum) seem to play a key role. Other factors that either reduce the resistance to shear or that increase the stresses across the proximal femoral physis are endocrine disorders,
There are several factors that can contribute to developing a SCFE:[10]
- Obesity[10]
- Femoral retroversion (>10°)[10]
- Increased physis height[10]
- More vertical slope of the physis[10]
- Metabolic and pathological conditions such as:[10]
- Renal failure osteodystrophy
- Previous radiation therapy
- Endocrine disorders such as[10]
- Hypothyroidism
- Growth hormone deficiency
- Growth hormone excess
- Panhypopituitarism
- Craniopharyngioma
- Hypogonadism
- Hyperparathyroidism
- Multiple endocrine neoplasia
- Turner's syndrome
- Elevation of Leptin levels
Characteristics / Clinical Presentation[edit | edit source]
Typical presentation is a child between the ages of 10 - 20 years. There are some differences found between the literature about the exact age. This has to do with the maturity of the growth plate (epiphysial line). There is an increased prevalence during the period of rapid growth, shortly after puberty. The disorder is more prevalent in male than females (2:1 ratio).
The child usually presents with some combination of hip, knee, thigh, and groin pain. The leg is typically externally rotated and an antalgic gait is noted. The majority of patients will be able to bear weight and will present with a limp[1][2][11]. When testing hip range of motion, internal rotation, flexion, and abduction are limited. External rotation and adduction are often increased and movement in all directions are painful. Typically, the involved hip will fall into external rotation when the hip is passively flexed beyond 90 degrees[11].
Differential Diagnosis[edit | edit source]
Other conditions to rule out:
- Femoral fractures[9]
- Avascular Necrosis Femoral Head[9]
- Legg-Calve-Perthes Disease[9]
- Osteomyelitis
- Septic Arthritis[9]
- Groin Strain[9]
- Apophyseal avulsion fracture of the anterosuperior and anteroinferior iliac spine[9]
- Apophysitis of the anterosuperior and anteroinferior iliac spine[9]
- Transient synovitis[9]
Diagnostic Procedures[edit | edit source]
Imaging[edit | edit source]
- Plain radiograph (AP and true lateral view)[10]
- Frog lateral review is often requested,but care must be taken as this may displace an unstable slip further. It is also less accurate in assessment of severity because of the variations in positioning of the limbs[10]
- Radiological signs that are used to confirm the diagnosis and assess the severity of the slip include:[10]
- Widening of the growth plate (this is an early sign)[10]
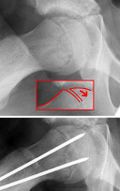
- Trethowan's sign (Klein's line) - On an AP view, a line drawn on the superior border of the femoral neck will intersect less of the femoral head or not at all in a patient with SFCE. This is as a result of the posterior displacement of the femoral epiphysis[10]
- There is a decrease in epiphyseal height , as the femoral head is slipped posteriorly behind the neck[10]
- Resultant remodelling changes are present in the femur neck such as a sclerotic, smooth superior part of the neck and callus formation on the inferior border. (This is not always present in an acute slip)[10]
- There is an increased distance between the tear drop and the femoral neck metaphysis[10]
- Capener's sign - In a patient with SFCE, the whole metaphysis is lateral to the posterior acetabular margin on an AP view of the pelvis. Normally the posterior acetabular margin will cut across the medial corner of the upper femoral metaphysis[10]
- Steel's blanch sign - a crescent shape dense area in the metaphysis as a result of superimposition of the neck and the head[10]
- CT scan[10]
- provides a 3D image helpful in pre-surgical planning[10]
- not always necessary in mild and moderate slips that only requires pinning in situ[10]
- very useful in severe slips in need of corrective surgery[10]
- callus presence can easily be identified by CT scan and this may indicate a chronic slip rather than an acute slip[10]
- helpful to investigate the positioning of wires and screws to prevent joint penetration[10]
- Ultrasound[10]
- MRI[10]
Blood tests[edit | edit source]
Blood tests are necessary to identify or rule out any underlying endocrine problems when the age-weight test is positive. It is also essential as part of the preoperative work up.[10]
Classification of SCFE[edit | edit source]
Classification of the patient and hip affected with SCFE is essential to advance treatment, and the selection thereof, as well as to improve the outcome. Key factors to consider at initial diagnosis are:[3]
- stability of the physis
- degree of slip deformity - seen as substitute for risk of cumulative mechanical damage
- other anatomic and mechanical factors, such as anatomic version, acetabular depth and activity level
Physeal stability[3][edit | edit source]
Previous clinical classifications has often placed untreated SCFE hips into categories such as Acute, Acute-on-Chronic and Chronic. These classifications have limited correlation with the pathomechanics seen in SCFE. The first essential clinical factor to assess is the mechanical stability of the physis. The onset of symptoms in SCFE is usually indefinite and the duration of the symptoms is not closely related to physeal stability. Classification should therefor consider mechanical and morphological parameters.[3]
The degree of physeal stability in SFCE can range from a complete disruption of the physis to total stability in the healed slip.[3] The inability to ambulate or weight bear has been the classical definition of the unstable or acute SCFE. [12] Recent evidence, however, suggests that the mechanical stability of the physis in the SCFE hip may be different from what one would assume if the ability to ambulate or weight bear is used as an indicator[13]. Studies reported that 13 of 24 hips in which patients were unable to bear weight before surgery had mechanically stably physis intra-operatively.[13] More significant though, is the fact that 17 of 58 hips in which patients were able to weight-bear before surgery had unstable physis intra-operatively.[13] It is therefor recommended that every SCFE hip with an open physis be considered at risk of acute disruption.[3]
| Slipped capital femoral epiphysis classification by mechanical stability[13] | ||
|---|---|---|
| Status of Physis | Open | Closed |
| Mechanical stability of capital femoral physis and femoral head | Uncertain, regardless of ability to ambulate or duration of symptoms | Stable |
Degree of Deformity[3][edit | edit source]
Morphological classifications have relied on radiographic views using the linear displacement of the femur head on the neck of the femur or the slip angle (angle between the shaft and perpendicular to the physis per Southwick) as parameters.[3]
The degrees of deformity are:
- Pre-slip (widening of the physis, no displacement)
- Mild slip (up to 1/3 displacement, or 30° of femoral head tilt)
- Moderate slip (1/3 to 1/2 displacement or 30° to 60° slip angle)
- Severe slip (> 1/2 displacement or > 60° of slip angle)
Outcome Measures[edit | edit source]
- Diagnostic Imaging
- Radiographs[11][14][10]:
- Anterior/posterior view
- Lauenstein-projection
- Wilson classification system
- Bonescan (MRI, CT)[14][10]:
- slipped femoral epiphysis
- MRI[14][10]:
- Epiphyseal avascular necrosis
- Radiographs[11][14][10]:
- Functional outcome measures
- Patient reported outcome measures (PROM)
Examination[edit | edit source]
With passive movement, there will typically be a restriction with internal rotation, and a remarkably large hip external rotation.[17] Presentation may include a limp or vague pain in the hip, thigh or knee. It is vital to remember that the complaint of knee pain may be present because of referred pain from pathology at the hip. Every child presenting with a complaint of hip, thigh or knee pain must undergo a hip examination. Likewise, a "groin pull" is exceedingly rare in children and must be a diagnosis of exclusion. [18]
On physical examination, the patient may be unable to bear weight with a severe slip. Limited internal rotation of the hip is the most telling sign in the diagnosis of SCFE. Obligatory external rotation is noted in the involved hip of patients with SCFE when the hip is passively flexed to 90 degrees. Sometimes also restricted abduction. Unless the patient has bilateral SCFE, it is helpful to compare range of motion with the uninvolved hip.[19]
Patients usually present with limping and poorly localized pain in the hip, groin, thigh, or knee. Diagnosis is confirmed by bilateral hip radiography, which needs to include anteroposterior and frog-leg lateral views in patients with stable slipped capital femoral epiphysis, and anteroposterior and cross-table lateral views in patients with the unstable form[20]
Medical Management[edit | edit source]
Once the diagnosis of SCFE is made, the patient should be placed on non–weight-bearing crutches or in a wheelchair and quickly referred to an orthopedic surgeon familiar with the treatment of SCFE. The initial goals of treatment are to prevent slip progression and avoid complications.[21]
Prophylactic treatment of the contralateral hip in patients with SCFE is controversial, but it is not recommended in most patients. Prophylactic pinning may be indicated in patients at high risk of subsequent slips, such as patients with obesity or an endocrine disorder, or those who have a low likelihood of follow-up. [22]
Stable SCFE[23][edit | edit source]
The standard treatment of stable SCFE is in situ fixation with a single screw. Case series and animal model studies have shown this to be a simple technique with low rates of recurrence and complications. After closure of the growth plate, progression of athletic activities may be allowed, including running and, eventually, participating in contact sports. Most patients with mild to moderate SCFE who are treated with in situ fixation have well to excellent long-term outcomes.
Unstable SCFE[24][edit | edit source]
Unstable SCFE is a much more severe injury than stable SCFE. The rate of osteonecrosis is as high as 20 to 50 percent in patients with the unstable form. Treatment goals are similar to those of stable SCFE with in situ fixation, but there is controversy as to the specifics of treatment, including timing of surgery, value of reduction, and whether traction should be used.
Physical Therapy Management[edit | edit source]
Once the patient is diagnosed with SCFE, the patient should seize to bear weight on this leg. The first goal of treatment is to prevent the further slipping and avoid complications.[12][25]
Conservative treatment can include Spica Casting, easy range of motion exercises and hydrotherapeutic exercises. This method consists of a period of immobilization that is much longer than when undergoing surgical treatment. A long immobilization phase is associated with a lot of complications like atrophy and strength loss of the muscles, reduced bone mineral density and it is unfavorable to prevent chondrolysis. However, Pinheiro et al[26] suggest that whatever treatment you use the chances for chondrolysis are 7%. As soon as the risk of femoral head slippage is reduced the therapist can use partial weight bearing with the help of crutches and an exercise program. Strenghth exercises are implemented to regain power in all leg muscles as well as proprioception and coordination exercises to regain full control and stability of the hip.
When pinning-in-situ surgery is performed the first goal is to is decrease the pain. Modalities such as ice, ultrasound and electrical current may be used. Continuous passive motion of the hip to maintain range of motion is recommended after surgery[27]. The patient can also weight bear up to 20kg but should always be assisted by the therapist. Cryotherapy can be used to relief the pain. After surgery an exercise program to improve range of motion of the hip, augment muscle strength and coordination can be prescribed. Up to 3 weeks the patient has to limit himself to the 20kg of weight bearing. After this, if the patient is pain free, full range of motion is achieved and six weeks have passed, the patient can fully weight-bear.. If not,partial weight bearing must be advised.[28][29]
Resources[edit | edit source]
References[edit | edit source]
- ↑ 1.0 1.1 Perry DC, Metcalfe D, Costa ML, Van Staa T. A nationwide cohort study of slipped capital femoral epiphysis. Arch Dis Child 2017;102:1132–1136 (accessed 22 October 2018)
- ↑ 2.0 2.1 2.2 Chang AL, Cirino C, Anthony SG. Orthopaedic sports injuries in youth: the hip. Ann Joint 2018;3:36 (accessed 22 October 2018)
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 Millis MB. SCFE: clinical aspects, diagnosis, and classification. J Child Orthop 2017;11:93-98. (accessed 22 October 2018).
- ↑ Kauer JMG., Rutten - Dobber CE, Kapandji IA. Bewegingsleer aan de hand van tekeningen van de werking van de menselijke gewrichten deel II De onderste extremiteit, Scheltema & Boltema, Utrecht, 1984, 233 pagina’s (L.O.E. 5)
- ↑ Van Roy P et al. Compendium Artrologie vakgroepen experimentele anatomie en menselijke anatomie, Dienst Uitgaven Vrije Universiteit Brussel, Brussel, 64 pagina’s (L.O.E. 5)
- ↑ Kahle W, Leonhardt H, en Platzer W. Sesam atlas van de anatomie, Bosh & Keuning NV, Baarn, 1981, 433 pagina’s (L.O.E. 5)
- ↑ Kauer JMG, Rutten-Dobber CE, Kapandji IA. Bewegingsleer aan de hand van tekeningen van de werking van de menselijke gewrichten deel II De onderste extremiteit, Scheltema & Boltema, Utrecht, 1984, 233 pagina’s (L.O.E. 5)
- ↑ 8.0 8.1 Chang AL, Cirino C, Anthony SG. Orthopaedic sports injuries in youth: the hip. Ann Joint 2018;3:36.
- ↑ 9.00 9.01 9.02 9.03 9.04 9.05 9.06 9.07 9.08 9.09 9.10 Peck DM, Voss LM, Voss TT. Slipped Capital Femoral Epiphysis: Diagnosis and Management.Am Fam Physician. 2017 Jun 15;95(12):779-784.
- ↑ 10.00 10.01 10.02 10.03 10.04 10.05 10.06 10.07 10.08 10.09 10.10 10.11 10.12 10.13 10.14 10.15 10.16 10.17 10.18 10.19 10.20 10.21 10.22 10.23 10.24 10.25 10.26 10.27 10.28 10.29 10.30 10.31 10.32 Adam J, Austin S, Alshryda S.Treatment of Slipped Capital Femoral Epiphysis-What is new? New Iraqi J Med 2018;4:72 -79.
- ↑ 11.0 11.1 11.2 Campbell S, Vander Linden D, Palisano R. Physical therapy for children. St. Louis, MO:Elsevier Inc, 2006.
- ↑ 12.0 12.1 Loder RT, Richards BS, Shapiro PS, Reznick LR, Aronson DD. ‘Acute slipped capital femoral epiphysis: the importance of physeal stability.’ J Bone Joint Surg Am. 1993;75(8):1134–1140. (L.O.E. 2A
- ↑ 13.0 13.1 13.2 13.3 Ziebarth K, Domayer S, Slongo T, Kim YJ, Ganz R. Clinical stability of slipped capital femoral epiphysis does not correlate with intraoperative stability. Clin Orthop Relat Res 2012;470:2274-2279
- ↑ 14.0 14.1 14.2 Koos van Nugteren. De kwetsbaarheid van het jeugdige skelet. Bohn Stafleu Van Loghum, 2005:44-48.
- ↑ B. Herngren, M. Stenmarker, K. Enskär, and G. Hägglund. Outcomes after slipped capital femoral epiphysis: a population-based study with three-year follow-up. J Child Orthop. 2018 Oct 1; 12(5): 434–443.
- ↑ 16.0 16.1 16.2 De Poorter J, Beunder TJ, Gareb B, Oostenbroek HJ, Bessems GHJM, van der Lugt JCT, Maathuis PGM,van der Sande MAJ. Long-term outcomes of slipped capital femoral epiphysis treated with in situ pinning. J Child Orthop. 2016 Oct; 10(5): 371–379.
- ↑ Koos van Nugteren. ‘De kwetsbaarheid van het jeugdige skelet.’, Bohn Stafleu Van Loghum, 2005:44-48. (L.O.E. 5)
- ↑ Department of Orthopedic Surgery, SUNY Upstate Medical University, Syracuse, NY, USA. ‘Slipped capital femoral epiphysis: the importance of early diagnosis.’ (L.O.E 5)
- ↑ Peck D., ‘Slipped Capital Femoral Epiphysis: Diagnosis and Management.’, AM Fam Physician, 2010-08, nr. 3, p. 258-262 (L.O.E. 2A)
- ↑ Maximilian F. ‘Reiser,Andrea Baur-Melnyk. Musculoskeletal Imaging.’ P. 173, 174 (L.O.E. 5)
- ↑ Nonoperative treatment of slipped capital femoral epiphysis: a scientific study (L.O.E 2B)
- ↑ Nonoperative treatment of slipped capital femoral epiphysis: a scientific study (L.O.E 2B)
- ↑ Nonoperative treatment of slipped capital femoral epiphysis: a scientific study (L.O.E 2B)
- ↑ Nonoperative treatment of slipped capital femoral epiphysis: a scientific study (L.O.E 2B)
- ↑ Aronsson DD, Loder RT. ‘Treatment of the unstable (acute) slipped capital femoral epiphysis.’ Clin Orthop Relat Res. 1996;(322):99–110. (L.O.E 2B)
- ↑ Pedro Carlos MS Pinheiro, Nonoperative treatment of slipped capital femoral epiphysis: a scientific study 2011 (L.O.E 2B)
- ↑ Capital Realignment for Moderate and Severe SCFE Using a Modified Dunn Procedure, Kai Ziebarth MD, (L.O.E 2B)
- ↑ Loder RT, Richards BS, Shapiro PS, Reznick LR. Acute slipped capital femoral epiphysis: the importance of physeal stability. J bone joint surg 1993;75A:1134-1140. (L.O.E. 2A)
- ↑ Loder RT, Richards BS, Shapiro PS, Reznick LR. Acute slipped capital femoral epiphysis: the importance of physeal stability. J bone joint surg 1993;75A:1134-1140. (L.O.E. 2A)
- ↑ Slipped Capital Femoral Epiphysis - Michael Millis, MD | Grice Lecture. Available from https://www.youtube.com/watch?v=SGATdIL7pX0