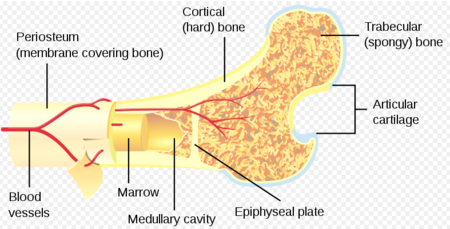
Bone Marrow Lesions
Introduction[edit | edit source]
Bone marrow lesions (BML) are painful alterations in subchondral bone due to repetitive microdamage at the articular surface. BML can be a result of degenerative, metabolic, inflammatory, traumatic and neoplastic processes.[1][2]
Bone marrow lesions (BML) are a clinical finding on MRI.
- BMLs can be found in any bone of the body.
- They may be present in a wide range of conditions.
- They were first discovered in 1988 and were initially called Bone Marrow Edema (BME) [3].
- The term oedema was used as it was thought that there was an increase in fluid in the bone marrow. It was later found that histologically it is not oedema but rather a multitude of different factors. As a result of these findings, the term Bone Marrow Lesion has replaced bone marrow oedema.[4] BME continues to be utilised in radiology circles, and the two terms can be used interchangeably.
Histopathology[edit | edit source]
There is limited research on the exact histopathology of BMLs. Remodelled trabeculae, bone marrow fibrosis, bone marrow bleeding, ingrowth of fibrovascular tissue and lymphocytic infiltrates have been found when investigating BMLs. [5][4]
Findings on Radiological Investigations[edit | edit source]
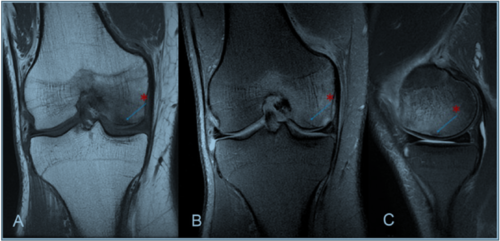
A BML is seen on MRI. A BML on a T1-weighted scan is seen as a hypodense (lighter) area and on a T2-weighted scan as a hyperdense (darker) area. They have no clear margins and cross anatomical boundaries[4]. Fat suppressed T2- weighted scans are often suggested to best identify BMLs [3]
Conditions that present with BMLs[edit | edit source]
BMLs represent a clinical finding on MRI. To diagnose the cause of the bone marrow lesion the patient's clinical history and symptoms must be taken into account[6].
In Eriksen's (2015) article on BMLs, they describe that BMLs are present in the following conditions[4]:
- Trauma
- Fracture (acute, osteoporotic and stress)
- Local transient osteoporosis
- Altered stress/biomechanics (plantar fasciitis, tendinitis/entesitis)
- Bone bruise
- Osteochondral injuries (osteochondritis dissecans)
- Degenerative lesions
- Osteoarthritis (hip, knee, other)
- MODIC lesions (spine)
- Inflammatory lesions
- Inflammatory arthropathies and enthesitis (rheumatoid arthritis (RA), Ankylosing spondylitis, psoriasis)
- Systemic chronic inflammation with fibrosis
- Ischaemic lesions
- Avascular necrosis (AVN)
- Complex regional pain syndrome (Sudeks atrophy of bone)
- Sickle cell anaemia (SCA)
- Infectious lesions
- Osteomyelitis
- Diabetic foot, Charcot's foot
- Sepsis (bone infarcts)
- Metabolic/endocrine lesions
- Hydroxyapatite deposition disease (HADD)
- Gout
- Iatrogenic lesions
- Surgery
- Radiotherapy
- Immunosuppressants (glucocorticoids, cyclosporin)
- Cytostatics
- Neoplastic (and neoplastic-like) lesions
Clinical Significance of BMLS[edit | edit source]
The clinical significance of BMLS is not well understood. Literature is starting to show a potential correlation between BMLs, pain and function[6]. Studies have shown that the presence of BMLs can increase the risk of cartilage loss as well as the development of knee pain[7]. X-ray findings such as osteophytes and loss of joint space are commonly used to diagnose osteoarthritis. Bone marrow lesions are possibly an early clinical finding of OA. It has been proposed that BMLs could potentially be an early indicator for OA and interventions targeted at managing the BMLs could result in the preservation of joint cartilage.[6]
Treatment of BMLs[edit | edit source]
Treatment of BML is complicated as their exact aetiology is not entirely understood. There is no agreement on standard treatment protocols for BMLs. Treatment is often targeted more at the condition, symptoms, functional presentation.[8] Many studies have been conducted looking at the effect on bone marrow lesions using various modalities. They have mostly shown that interventions may produce functional and symptomatic changes but may not always affect the appearance of BMLs on MRI[4].
Surgical
Surgical procedures, such as core decompression have been used in the hip with varying results[3] [4]. Newer techniques such a subchondroplasty where calcium phosphate bone substitute is injected into the trabeculae is showing promise but needs to be further researched[3]
Extracorporeal shock wave therapy
ESWT has shown to reduce the appearance of BMLs in both the hip and knee [4][9]
An RCT published in 2018 has shown promising evidence that ESWT may be an effective management strategy to help with pain relief and functional improvement in people with OA of the knee.[9]
Physical offloading
The idea behind physical offloading is that if repetitive microtrauma has caused a BML then, by offloading the joint, the BMLs should recover. This has not been supported by literature yet. A recent study looked at the use of a cane to potentially offload the knee in patients with medial tibiofemoral OA. Their findings concluded that the use of a cane did not reduce BML volumes compared to not using a cane.[10]
Exercise
A study looked at BMLs and exercise in knee OA. Their end findings concluded that exercise benefited both groups, those with BMLs and those without BMLs, and there was no significant difference between the groups. They did find that strength training may be more effective at reducing pain in patients with BMLs. This could be used to help create individuals treatment plans for patients. Their sample size was very small, and further research into this is required.[8]
Pharmaceutical
Bisphosphonates and prostacyclins have both shown to be somewhat beneficial with improvement in pain in conditions that present with BMLs. The results from various studies are conflicting and often show more promise in early disease stages. To date, there is no consensus on the mechanism of action of these drugs, and more research is needed.
Additional Resources[edit | edit source]
BML as seen on MRI due to migratory osteoporosis
BML as seen on MRI due to Osteochondritis Dissecans Lesion
References[edit | edit source]
- ↑ Munsch MA, Safran MR, Mai MC, Vasileff WK. Bone marrow lesions: etiology and pathogenesis at the hip. Journal of Hip Preservation Surgery. 2020 Aug;7(3):401-9.
- ↑ Gobbi A, Dallo I, Frank RM, Bradsell H, Saenz I, Murrel W. A review of bone marrow lesions in the arthritic knee and description of a technique for treatment. Journal of Cartilage & Joint Preservation. 2021 Sep 1;1(3):100021.
- ↑ 3.0 3.1 3.2 3.3 Bonadio MB, Ormond Filho AG, Helito CP, Stump XM, Demange MK. Bone marrow lesion: image, clinical presentation, and treatment. Magnetic resonance insights. 2017 Apr 12;10:1178623X17703382.
- ↑ 4.0 4.1 4.2 4.3 4.4 4.5 4.6 Eriksen EF. Treatment of bone marrow lesions (bone marrow edema). BoneKEy reports. 2015;4.
- ↑ Xu L, Hayashi D, Roemer FW, Felson DT, Guermazi A. Magnetic resonance imaging of subchondral bone marrow lesions in association with osteoarthritis. InSeminars in arthritis and rheumatism 2012 Oct 1 (Vol. 42, No. 2, pp. 105-118). WB Saunders.
- ↑ 6.0 6.1 6.2 Marcacci M, Andriolo L, Kon E, Shabshin N, Filardo G. Aetiology and pathogenesis of bone marrow lesions and osteonecrosis of the knee. EFORT open reviews. 2016 May;1(5):219-24.
- ↑ Alliston T, Hernandez CJ, Findlay DM, Felson DT, Kennedy OD. Bone marrow lesions in osteoarthritis: what lies beneath. Journal of Orthopaedic Research®. 2018 Jul;36(7):1818-25.
- ↑ 8.0 8.1 Beckwée D, Vaes P, Raeymaeckers S, Shahabpour M, Scheerlinck T, Bautmans I. Exercise in knee osteoarthritis: do treatment outcomes relate to bone marrow lesions? A randomized trial. Disability and rehabilitation. 2017 Aug 28;39(18):1847-55.
- ↑ 9.0 9.1 Kang S, Gao F, Han J, Mao T, Sun W, Wang B, Guo W, Cheng L, Li Z. Extracorporeal shock wave treatment can normalize painful bone marrow edema in knee osteoarthritis: a comparative historical cohort study. Medicine. 2018 Feb;97(5).
- ↑ Van Ginckel A, Hinman RS, Wrigley TV, Hunter DJ, Marshall CJ, Duryea J, Melo L, Simic M, Kasza J, Robbins SR, Wallis JA. Effect of cane use on bone marrow lesion volume in people with medial tibiofemoral knee osteoarthritis: randomized clinical trial. Osteoarthritis and cartilage. 2019 May 21.