Bradycardia
Original Editor - Vidya Acharya
Top Contributors - Vidya Acharya, Lucinda hampton, Kim Jackson and Rucha Gadgil
Introduction[edit | edit source]
Bradycardia is defined as a heart rate (HR) of less than 50–60 bpm, and it is seen as a normal phenomenon in young athletic individuals, and in patients as part of normal aging or disease.[1] Research shows there is also a circadian cycle of HR. It varies with the fastest rates between 1400-1700 hours and the slowest rates occurring between 0400-0600 hours. HR decreases by an average of 24 beats in young adults and 14 beats per minute in people over 80 years during sleep. Women have faster HR than men during both waking and sleeping periods, by an average of 10 bpm in young adults[2].
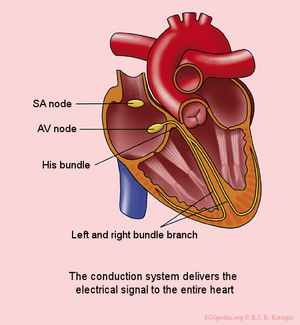
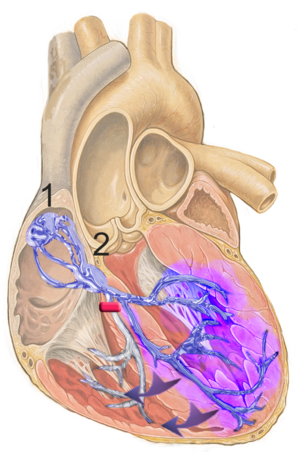
The sinoatrial (SA) node initiates and controls the cardiac rhythm; it is the heart's primary pacemaker. SA node structure consists of clusters of specialized cardiomyocytes enmeshed within strands of connective tissue or fibrosis. The SA conduction pathways electrically connect the SA node to the right atrium and play an important role in regulating the SA node automaticity, thus the maintenance of the HR[2].
Several factors modulating the HR include the autonomic nervous system (dynamic balance between sympathetic and parasympathetic nervous systems), the baroreceptors, the Bainbridge reflex, the intrinsic heart rate, etc. The cardiac conduction system and the SA node are more densely innervated by the autonomic nervous system supporting the central role of the autonomic nervous system in initiating and regulating the cardiac impulse.[2]
Types of Bradycardias[edit | edit source]
Broadly can be defines as 3 main types
- Sinus Bradycardia: Increased vagal tone. It can be physiological in the athletes.[3]
- Atrioventricular Blocks: Atrial impulses are conducted with a delay or not at all when an electrical impulse reaches a tissue that not excitable or is in a refractory period.
- First Degree AV Block: Caused by increased vagal tone or conduction impairment or due to medications.
- Second Degree AV Block: It is further classified into Mobitz I block which has progressive prolongation of the PR interval followed by a skipped beat, and Mobitz II block, where there is a randomly dropped QRS complex on an EKG.
- Third Degree or Complete AV Block: Lack of conduction of atrial impulse to ventricle leading to independent contractions
- Sinus Node Dysfunction: Senescence of the SA node, an ischemic event involving SA node leading to impulse generation at a slower rate[3].
- Sinus Pause: When the SA node has delayed impulse generation.
- Sinus Arrest: Failure of impulse generation.
- SA Nodal Exit Block: Failure of impulse transmission.
Aetiology: Intrinsic Causes[edit | edit source]
Intrinsic causes like aging, ischemic heart disease, infiltrative diseases, or surgery can also result in conduction disorders.
- Athlete: With a heartbeat as low as 50, Bradycardia can be normal in athletes and other physically active people. Regular exercise improves the heart's ability to pump blood efficiently, so fewer heart contractions are required to supply the body's needs[4].
- Aging: Age-induced increase of SA node fibrosis is strongly correlated with slower heart rate and slowed SA node conduction.[2]
- Ischemic heart diseases: Bradyarrhythmias can be due to myocardial ischemia/infarction involving the proximal right and/or circumflex artery or the coronary artery supplying blood flow to the sinus node or to the AV node.
Aetiology: Extrinsic causes[edit | edit source]
Medication modifying the heart's excitability, electrolyte, and metabolic disorders may also influence the heart rate directly or indirectly[5].
- Medications:[2]
- β-adrenergic blockers (metoprolol, nebivolol, etc.); non-dihydropyridine calcium-channel blockers (diltiazem, verapamil, etc,); antiarrhythmics, digoxin and other sympathomimetic antihypertensives (clonidine, prazosin, etc.) are known to cause bradycardia.
- Topical ophthalmic medications, such as timolol maleate, used for treating glaucoma and ocular hypertension, may cause bradycardia. The medicine gets absorbed from the eye into the systemic circulation and can cause systemic adrenergic βblocking, leading to AV block and bradycardia.
- Other medications like corticosteroids, donepezil, narcotics, and anesthetics.
- Other conditions[2]: Infection/febrile illnesses (encephalitis, dengue hemorrhagic fever, etc), endocrinologic abnormalities (hypothyroidism), anorexia nervosa, hypothermia, hypoglycemia, electrolyte disturbances (e.g., hyperkalemia), infiltrative disease, collagen vascular disease, trauma to the cardiac conduction system, hypoxia, and other complications
Clinical Presentation[edit | edit source]
A patient with bradycardia can be completely asymptomatic or may present with a diversity of signs and symptoms.
Symptoms[2]:
- dizziness, light-headedness or confusional states,
- episodes of fatigue or muscular weakness,
- exercise intolerance,
- heart failure, or
- palpitations are seen.
Assessment[edit | edit source]
Bradycardia can up as an incidental finding during a routine check-up. In patients with confirmed or suspected bradycardia, a thorough history should be taken. The physical examination should include documentation of associated signs/symptoms of hypoperfusion and precipitating factors, medications (including nasal and ophthalmic routes), personal and family history (coronary artery disease, cardiac arrhythmia, and sudden death).
The clinician should check for[4]:
- pulse rate and rhythm of the heartbeat
- the patient may be asked to do sit-ups/ exercises and check whether the heart rate rises
- signs of other diseases like very dry skin, thin hair, enlarged thyroid, that could be causing the arrhythmia
Investigations[edit | edit source]
Include:
- Basic laboratory tests of electrolytes, glucose, toxicology screening for narcotics, and digitalis level if the patient is on digoxin, and thyroid function is carried out.[2]
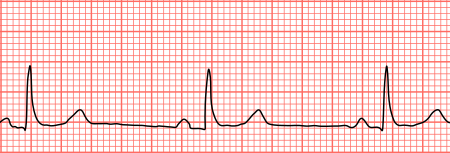
- ECG: A standard 12-lead ECG is used to determine the presence and type of bradyarrhythmia and/or presence of structural cardiac disease, such as prior or acute myocardial ischemia/infarction.[2]
- Holter monitors: Also called ambulatory electrocardiograms are used when bradycardia is intermittent and 12-lead ECG does not yield a diagnosis. They are battery-operated portable devices that record the heart’s activity (ECG) continuously for 24 to 48 hours or longer depending on monitoring requirements. Small electrodes along with wires are attached to the skin.[2]
- Event Recorder: If the Holter monitoring is non-diagnostic and the patient is experiencing intermittent symptoms, longer cardiac monitoring of 1 to 4 weeks is needed, non-invasive mobile cardiovascular telemetry or event monitoring can be used. The event recorder only records when it is activated or when the abnormal heart rhythm is detected.[6][2]
- Invasive electrophysiologic studies: May be used to evaluate sinus node dysfunction and AV blocks in patients with known or suspected bradyarrhythmias
- Stress test, also called treadmill test or an exercise stress test, can help to diagnose chronotropic incompetence by incremental dynamic exercise testing[2][7]
Treatment[edit | edit source]
Medications[edit | edit source]
Atropine Sulfate: is the first-line treatment. It reverses cholinergic-mediated decreases in HR and AV conduction. Atropine improves heart rate and signs/symptoms associated with bradycardia.[2] Atropine should be considered a temporary measure and should not delay the implementation of a pacemaker for patients with symptomatic and/or unstable bradyarrhythmia or sinus arrest. Atropine should be used cautiously in patients with acute coronary syndrome as increased HR may worsen acute ischemia/infarction.
Intravenous infusion of β-adrenergic agonists with HR accelerating effects (e.g., dopamine. epinephrine, isoproterenol) can be effective if the bradycardia is unresponsive to atropine.
Cardiac Pacing[edit | edit source]
Patients with severe bradyarrhythmias should be considered for permanent or temporary pacing therapy.[5]
Temporary Pacing[edit | edit source]
Temporary pacing should be initiated immediately in patients suffering from severe or clinically significant episodes of bradyarrhythmia and asystole, if there is no response to atropine. Temporary pacing is an emergency measure to provide temporary ventricular rate support, thus cardiac output, for adequate perfusion of the vital organs until permanent pacing can be arranged.[2]
Several forms of temporary pacing[2]:
- transcutaneous (done by applying adhesive pads to the chest in anterioposterior or anteroapical configuration),
- esophageal (rarely used),
- epicardial or percutaneous transvenous (the procedure is painful in conscious patients and requires sedatives or anesthetics) is used to stabilize patients suffering from hemodynamic unstable bradyarrhythmia
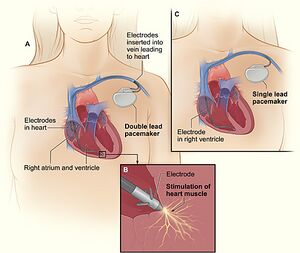
Permanent Pacing[edit | edit source]
Implantable pacemakers activate the cardiac myocardium with electrical stimulation, leading to muscle contraction. Due to a pacemaker's nature, the activation is different from the physiological conduction system; there are electrical and mechanical consequences. It is, therefore, vital to adjust the pacemaker setting to the individual patient[5]. The indications for pacemaker implantation in patients with bradyarrhythmias are atrioventricular blocks, Sinus node dysfunction.
Physiotherapy relevance[edit | edit source]
Change in blood pressure, drop in oxygen saturation, arrhythmias esp. bradycardia may occur during physiotherapy interventions. It is imperative to carry out a detailed multisystem assessment before starting intervention that evaluates the benefits, adverse effects, and patient stability so that physiotherapy intervention is safe and effective.[8] Heart rate, blood pressure, and 12 lead ECG must be constantly assessed during interventions and the recovery period.
Conclusion[edit | edit source]
Bradycardia is common clinical findings, and it may be physiologic or because of pathological conditions (sinus node dysfunction and AV conduction disturbances). Medications and pacing are used to manage unstable or symptomatic bradyarrhythmia.
Resources[edit | edit source]
Physiotherapy and cardiac rhythm devices: a review of the current scope of practice
References[edit | edit source]
- ↑ Sidhu S, Marine JE. Evaluating and managing bradycardia. Trends in cardiovascular medicine. 2020 Jul 1;30(5):265-72.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 Wung SF. Bradyarrhythmias: clinical presentation, diagnosis, and management. Critical Care Nursing Clinics. 2016 Sep 1;28(3):297-308.
- ↑ 3.0 3.1 Desai DS, Hajouli S. Arrhythmias. StatPearls [Internet]. 2020 Jun 25.
- ↑ 4.0 4.1 What is it? Bradycardia. Harvard Health Publishing. Accessed on 31/03/21
- ↑ 5.0 5.1 5.2 Textbook of Cardiology.org.BradycardiaSébastien Krul, MD
- ↑ John Hopkins Medicine, Health, Event Monitor. Accessed on 30/3/2021 fromhttps://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/event-monitor
- ↑ Brubaker PH, Kitzman DW. Chronotropic incompetence: causes, consequences, and management. Circulation. 2011 Mar 8;123(9):1010-20.
- ↑ Pathmanathan N, Beaumont N, Gratrix A. Respiratory physiotherapy in the critical care unit. Continuing Education in Anaesthesia, Critical Care & Pain. 2015 Feb 1;15(1):20-5.