Cyclist's Knee
Original Editor - Your name will be added here if you created the original content for this page.
Lead Editors
Cyclist's Knee - Relevant Anatomy[edit | edit source]
Most cyclists experience some knee pain over the course of their riding career. A systematic review and various studies report the incidence of knee pain ranging from 36% to 62%[1] [2]and it is the second most reported overuse injury for cyclists[3] (after Cyclist's Back).
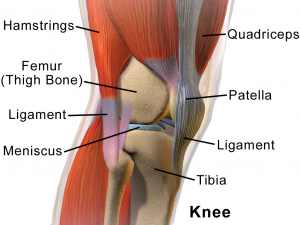
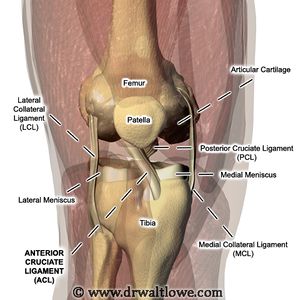
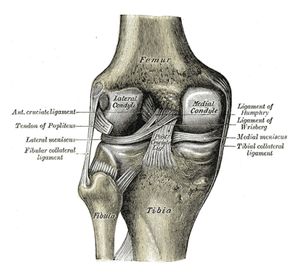
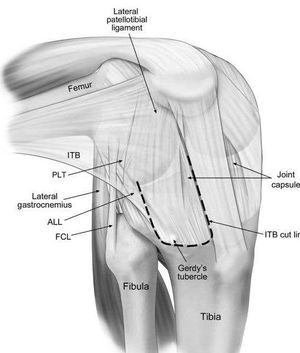
The knee (see the link for comprehensive detail of the knee) sits between the upper and lower leg. If any part of the lower kinematic chain (core, lumbar spine, hip, knee, ankle) gets a problem it can pull on the knee joint changing the way the knee functions and cause knee pain. Due to the repetitive motion of the knee in cycling overuse injuries can occur when these incorrect tensions/torsions are applied to the knee. A 2017 review reported that cycling parameters (i.e., cadence and power output) and bicycle fit settings have differing effects on kinematics, kinetics, and muscle activity around the knee and how biomechanical factors and positioning on the bicycle can increase or decrease stress in specific areas of the knee joint.[4]
The knee joint is a complicated joint with various compartments that can be affected
- Anterior Knee Pain
- Posterior knee pain
- Lateral and medial knee pain
Mechanism of Injury / Pathological Process[edit | edit source]
Four Main Reasons for Knee Pain on the Bike
- Incorrect cleat alignment
- Incorrect saddle position. A 2011 review concluded that correct saddle height (using the knee flexion angle method (25-30°)) reduced the risk of knee injuries and minimised oxygen uptake[1].
- Incorrect cadence
- Poor flexibility and or strength of the core, pelvis, and or flexors or extensors of lower limb kinetic chain[5]
Three Main Regions of Knee Pain
- Anterior Knee PainCaused by increased pressure on the patella ( 2011 systematic review reporting patellofemoral compressive force seems to be inversely related to saddle height) and surrounding soft tissues or incorrect tracking of the patella. This can arise from: saddle too low or positioned too far forward[6]; tight hip or knee flexors causing patella to compress at patellofemoral joint; slow cadence putting much great force through knee; cleats causing tibial torsion resulting in incorrect patella tracking.
- Posterior Knee PainCaused by increased forces applied to posterior knee joint and surrounding soft tissues. This can arise through: saddle too high or too far aft[6]; tight calf, hamstrings or gluteals; cleats positions, foot too far forward on pedal.
- Lateral or Medial Knee Pain.Caused by incorrect pressure applied through lateral or medial knee structures[7] A 2018 systematic review reported that an increased medial projection of their knees causes an altered activation of the vastus medialis and vastus lateralis muscles and was a potential cause of cyclists knee pain[7]. This can arise through: incorrect cleat alignment, toe pointing medially causing lateral stress, toe points lateral causing medial stress; tight medial or lateral structures eg TFL or thigh adductors; insufficient core or pelvic muscle power to stabilise pelvis for lower limb kinetic chain to function efficiently from.[5]
Clinical Presentation[edit | edit source]
Cyclist will complain of pain that arises in the knee when cycling. Be sure to check that the knee has not been recently traumatically injured or the client has any red flags eg medical history, persistent pain on/off the bike. In the above instance,s you should investigate further and consult with GP or specialist.
Many presentations are possible to the many structures supporting the knee, some presentations are listed below
- IT band syndrome is a gradual onset injury causing pain on the outside of the knee. The pain may be stabbing and is caused by inflammation and stressed. Over time the pain gets progressively worse
- Patellofemoral pain syndrome (PFPS) is a generic term used to describe patella pain at the front of the knee. Symptoms include an aching pain in the knee joint, at the front of the knee around and under the patella both during activity and while at rest and it may also cause crackling noises and sensations in the knee joint. Malalignment of the patella (kneecap) can also cause or exacerbate issues.
- Hamstring tendinopathy from repeatedly over-stretching the hamstrings insertion (tights hamstrings or high seat position) causing a dull throb or stabbing sensation at or near hamstring insertion(s).
Subjective Examination[edit | edit source]
Should include finding out
- Chronic or acute condition
- Location of pain/injury
- Recent changes in bicycling regime eg duration of cycles, recent increase in kms covered, inclines involved/changed, terrain changes, cadence.
- Recent changes in bike fit, bike shoes, or pedal float ( the degree of mobility the foot has when clicked into pedal cleat)
Objective Examination[edit | edit source]
Make sure to do a good Bike Fit analysis and analysis of shoes and cleats/floats.
Assess the muscle strength and length of the lower limb kinetic chain, and neurodynamic structures. namely
- Anterior Knee Pain: assess lengths of quadriceps, TFL, hip flexors, and femoral nerve tension test- looking for tightness; assess tracking of patella and muscle strength of quadriceps ( VMO and lateral head)
- Posterior Knee Pain; assess lengths of hamstrings, TFL, gluteals, gastrocnemius and soleus and sciatic nerve (slump test)- looking for tightness; assess muscle strength of pelvic stabilisers, gluteals, and hamstrings.
- Medial Knee Pain; assess lengths of semitendinosus, semimembranosus, adductors hip, gluteal muscles- looking for tightness; assess muscle strength of pelvic stabilisers, and knee stabilisers.
- Lateral Knee Pain: assess lengths of biceps femoris, abductors hip, TFL, gluteals, peroneal muscles- looking for tightness; assess muscle strength of pelvic stabilisers, and knee stabilisers.
- Check dynamic stability of knee eg balance tests on balance board
Outcome Measures[edit | edit source]
- Visual Analogue Scale[8]
- LEFS
- Functional Index Questionnaire, see below.
Patient completes items 1-8. The score is out of 24, 24 being least affected by injury score.
Today, do you or would you have any problem in your knee at all? Response options 1.Unable To 2.Can Do With Problem 3.Can do with No Problem
1. walking as far as a mile 2. climbing up 2 flights of stairs (16 steps) 3. squatting 4. kneeling 5. sitting for prolonged periods with your knees bent in one position 6. climbing up 4 flights of stairs (32 steps) 7. running a short distance, say 100 meters.8. walking a short distance(about a city block)[8]
Physiotherapy Management / Interventions[edit | edit source]
Check Bike Fit and correct if needed or consult with Bike Fit specialist
Treat muscle tightness: muscle stretches ( choose between the various types of stretches, see link) for tight muscles; Active Release Techniques eg foam rolling, trigger point release, myofascial release. The below video gives a brief guide to dynamic stretches and foam rolling for cyclists.
Treat Tendon Pathology if appropriate
Kinesiology Taping or Knee Taping (links will give a how to guide)
Balance training to improve the neuromuscular, ligament, and tendon adaptations that the cyclist's knee will be subject to.
Strengthen the core (see Core Stability for a great range of exercises) and gluteals (see this link for treating) if assessed as weak. Remember legs work from the core – the lower back, abs, glutes, and hip flexors are all involved. A cyclist’s core needs to be strong, or smaller and less efficient muscles will be forced to work too hard and become fatigued. eg insufficient gluteals will result in the knee adducting and over-stressing the medial knee structures.[10]
Educate on the importance of Bike Fit, cadence, and how to progress a cycling regime. A 2014 report stated, " Despite both the increasing amounts of research and the popularity of load monitoring in high-performance programs, a single definitive tool that is accurate and reliable is not evident."[11] A often quoted percentage is to only ever add 10% per week to the regime, and monitor for response.
Conclusion[edit | edit source]
Remind cyclists to listen to their body, as it is designed to let you know something is wrong before it is a chronic problem. Advocate seeking help early on and seriously consider a bike fit.
Remember getting on the bike has many health benefits too as a 2011 systematic review that looked precisely at this found
"the strength of evidence was strong for fitness benefits, moderate for benefits in cardiovascular risk factors, and inconclusive for all-cause mortality, coronary heart disease morbidity and mortality, cancer risk, and overweight and obesity"[12]
References[edit | edit source]
- ↑ 1.0 1.1 Bini R, Hume PA, Croft JL. Effects of bicycle saddle height on knee injury risk and cycling performance. Sports medicine. 2011 Jun 1;41(6):463-76. Available from: https://www.ncbi.nlm.nih.gov/pubmed/21615188 ( last accessed 28.8.2019)
- ↑ Johnston TE, Baskins TA, Koppel RV, Oliver SA, Stieber DJ, Hoglund LT. The influence of extrinsic factors on knee biomechanics during cycling: a systematic review of the literature. International journal of sports physical therapy. 2017 Dec;12(7):1023. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5717478/ (accessed 28.8.2019)
- ↑ Clarsen, Benjamin & Krosshaug, Tron & Bahr, Roald. (2010). Overuse Injuries in Professional Road Cyclists. The American journal of sports medicine. 38. 2494-501. 10.1177/0363546510376816. Available from: https://www.researchgate.net/publication/46288399_Overuse_Injuries_in_Professional_Road_Cyclists (last accessed 29.8.2019)
- ↑ Johnston TE, Baskins TA, Koppel RV, Oliver SA, Stieber DJ, Hoglund LT. The influence of extrinsic factors on knee biomechanics during cycling: a systematic review of the literature. International journal of sports physical therapy. 2017 Dec;12(7):1023. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5717478/ (last accessed 29.8.2019)
- ↑ 5.0 5.1 SickBiker Bike Fitting - 4 Main Knee Pain Syndromes Of Cyclists. Saddle / cleats position... Available from: https://www.youtube.com/watch?v=Xk0zaFyJXbg&app=desktop (last accessed 29.8.2019)
- ↑ 6.0 6.1 Bini RR, Hume PA, Lanferdini FJ, Vaz MA. Effects of moving forward or backward on the saddle on knee joint forces during cycling. Physical Therapy in Sport. 2013 Feb 1;14(1):23-7. Available from: https://www.ncbi.nlm.nih.gov/pubmed/23312729 ( last accessed 29.8.2019)
- ↑ 7.0 7.1 Bini RR, Bini AF. Potential factors associated with knee pain in cyclists: a systematic review. Open access journal of sports medicine. 2018;9:99. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5973630/ (last accessed 29.8.2019)
- ↑ 8.0 8.1 BERT M. CHESWORTHl. Validation of Outcome Measures in Patients with Patellofemoral Syndrome. JOSPT February 1989 [last accessed 30.8.2019]. Available from: https://www.jospt.org/doi/pdf/10.2519/jospt.1989.10.8.302
- ↑ UCHealth Mountain Bike Stretches | UCHealth MTB Training Available from: https://www.youtube.com/watch?v=tGi8o3_FMc0&app=desktop (last accessed 31.8.2019)
- ↑ Cycling Weekly Cycling knee pain: everything you need to know. Available from: https://www.cyclingweekly.com/fitness/cycling-knee-pain-everything-you-need-to-know-329957 (last accessed 31.8.2019)
- ↑ Halson SL. Monitoring training load to understand fatigue in athletes. Sports medicine. 2014 Nov 1;44(2):139-47. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4213373/ (last accessed 31.8.2019)
- ↑ Oja P, Titze S, Bauman A, De Geus B, Krenn P, Reger‐Nash B, Kohlberger T. Health benefits of cycling: a systematic review. Scandinavian journal of medicine & science in sports. 2011 Aug;21(4):496-509. Available from: https://www.ncbi.nlm.nih.gov/pubmed/21496106 (last accessed 1.9.2019)