Shoulder Osteoarthritis
Introduction[edit | edit source]
Please note this article relates to the glenohumeral joint of the shoulder only.
Osteoarthritis of the shoulder or glenohumeral osteoarthritis (GH OA) is defined as ongoing damage of the glenohumeral cartilage in association with bony erosions, pain and decreased function of the glenohumeral joint[1]. It causes significant pain, functional limitation and disability. The loss of shoulder function can lead to depression, anxiety, activity limitations, and job-performance problems[2].
Watch this informative 2 minute video on GH OA>
Epidemiology[edit | edit source]
The glenohumeral joint is the third most common large joint to be affected following the knee and hip. While the true prevalence of glenohumeral OA is difficult to ascertain, population-based studies have demonstrated that 16.1%–20.1% of adults older than 65 years have radiographic evidence of glenohumeral OA[4]. Primary glenohumeral osteoarthritis is more common in women and in patients over the age of 60[1].
Risk Factors[edit | edit source]
Age is the main risk factor for glenohumeral osteoarthritis. Other risk factors include:
- female sex
- obesity
- caucasian race
- prior trauma
- rotator cuff tears
- glenohumeral instability
- crystalline arthropathy eg gout
- sickle cell disease[1]
.
Mechanism of Injury / Pathological Process[edit | edit source]
GH OA causes a gradual, progressive, mechanical, and biochemical breakdown of the articular cartilage and other joint tissues, including bone and joint capsule. As the articular surface wears, friction within the joint increases, causing progressive loss of the normal load-bearing surfaces with pain and disability.
The below video gives a great rundown of GH OA starting with details of the pathological process and goes on to nicely summarise the management and future directions.
Clinical Presentation[edit | edit source]
The typical presenting symptoms are:
- Progressive, activity-related pain that is deep in the joint and often localized posteriorly.
- As the disease progresses, night pain becomes more common.
- For many patients, the pain is present at rest and interferes with sleep.
- In advanced cases, the stiffness creates significant functional limitations.
- Crepitus on ROM
- Joint effusion
NB. In younger patients, prior trauma, dislocation, or previous surgery for shoulder instability are factors associated with the development of osteoarthritis.
Diagnostic Procedures[edit | edit source]
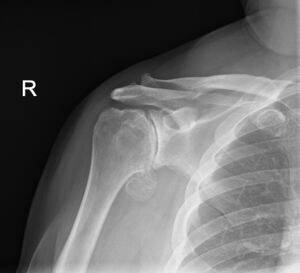
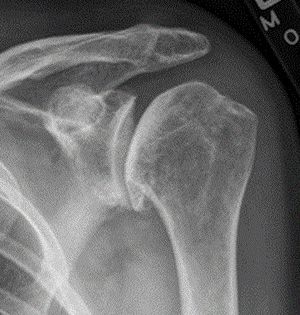
Imaging studies are essential to diagnosing degenerative joint disease. In most cases, conventional xrays demonstrate shoulder osteoarthritis. Early in the disease process, radiographic evidence of degenerative joint disease may include joint-space narrowing (mild), osteophytes (small), subchondral sclerosis, cysts, and eburnation or advanced articular cartilage loss. The axillary view provides the best image to look for joint-space narrowing and helps rule out dislocations. Anteroposterior radiography, with the arm held at 45 degrees of abduction, may also show early joint-space narrowing. Computed tomography arthrograms can localize articular defects, whereas MRI reveals soft-tissue pathologies and subtle changes in articular cartilage. Subchondral edema visible on MRI suggests advanced articular cartilage involvement.[6]
Outcome Measures[edit | edit source]
- DASH Outcome Measure
- Upper Extremity Functional Index
- Constant-Murley Shoulder Outcome Score
- Shoulder Pain and Disability Index (SPADI)
Management / Interventions[edit | edit source]
Treatment of shoulder OA is often controversial and includes both nonoperative and surgical modalities.
- Nonoperative modalities should be offered before operative treatment is considered, particularly for patients with mild-to-moderate OA or when pain and functional limitations are modest despite more advanced radiographic changes.
- If conservative options fail, surgical treatment should be considered. Although different surgical procedures are available, as in other joints affected by severe OA, the most effective treatment is joint arthroplasty.[7]
Physiotherapy[edit | edit source]
Perform a thorough shoulder assessment. This will guide you then your tailored approach to the client.
Education plays an important role. Lifestyle and occupational modifications should be discussed.
Therapy ideally should be initiated before the development of atrophy or contracture, and it should be tailored to the specific needs of the patient.
- Typical programs include gentle range of motion and isometric strengthening of the rotator cuff and scapulothoracic musculature.
- A good home program (HEP) of basic exercises should be given. This could include the following- Pendulum exercise; Passive Internal Rotation; Crossover Arm Stretch; Passive External Rotation; Wall Crawl; Wall Push Up; NB don't give client many exercises in HEP as they are more likely to follow a program that is simple and short. Provide sheet with exercises and dosage.
Rotator Cuff strengthening see link for how to perform and prescribe.
Techniques that could be employed include:
- Acupuncture and Dry Needling
- Scapular Stabilisation Exercises and Scapulohumeral Rhythm Exercises
- Rotator Cuff Exercises
- Shoulder Exercises including Strength Exercises and Stretching Exercises
- Biomechanical Analysis
- Proprioception & Balance Exercises
- Soft Tissue Massage
- Electrotherapy & Local Modalities eg TENS Machine. see also Current Concepts in Electrotherapy
- Thermotherapy
- Joint Mobilisation Techniques, see also Shoulder Mobilization and here
- Kinesiology Tape, Supportive Taping & Strapping
- Neurodynamics
Medical Management[edit | edit source]
Includes: salicylates, acetaminophen, and nonsteroidal anti-inflammatory drugs (NSAIDs), which can all be effective in relief of pain and inflammation. In particular randomized trials indicate that NSAIDs are more effective than both paracetamol and placebo for pain relief of OA. See risks of NSAIDs here
Intra-articular Injections[edit | edit source]
May provide pain relief in patients with shoulder OA. Because of the lack of evidence supporting their efficacy, no more than three corticosteroid injections in a single joint are recommendable unless there are special circumstances. Some evidence exists supporting viscosupplementation for shoulder OA. Some evidence reported that glenohumeral viscosupplementation resulted in a significant improvement in shoulder pain and function outcome scores 6 months following injection[7]
Surgical Treatments[edit | edit source]
Shoulder surgery is considered for GH OA pain that does not respond to nonsurgical measures. Improved function is not the goal of surgery and is less predictably achieved than pain relief. The choice of treatment then depends on both patient and disease features. Patient features include age, occupation, activity level, and the expectations for functional recovery. Disease features include the lesion size and the extent of chondral involvement.[7]
Differential Diagnosis[edit | edit source]
- Labral Tear
- Septic Arthritis
- Rotator Cuff Injury
- Cervical Disc Disease with radiculopathy into Shoulder
- Adhesive Capsulitis (Frozen Shoulder)
- Polymyalgia Rheumatica (affects Shoulder in 95% of cases)
- Pseudogout
- Systemic Lupus Erythematosus[9]
Future Directions[edit | edit source]
In the future having a great physiotherapist (up to date on the topic) will continue to be essential. That means having
- A solid background on the pathology of arthritis
- Excellent MSK examination skills
- Knowledge of evidence-based treatments
- Knowledge of exercise prescription for special populations
- Strong communication skills
Research in 2018 reports of a bright spot on the horizon using hyaluronic acid. It is a choice given in the non surgical options for management of OA. Osteoarthritis is a debilitating disease that affects a large portion of the population, and as the population continues towards an older age, the prevalence of the disease is going to go up. Hyaluronic acid potentially helps lower the side effects of OA on joints. Its effectiveness is due to the many methods of actions it deploys, including lubrication, anti-inflammatory and chondroprotective effects. Treatment can be done both orally and through intra-articular injections. New products are continuously being developed that change the composition of the molecule as well as pairing it with other drugs to maximize the effect[10]. However a 2015 report on the effects of these injections versus physiotherapy treatment concluded that physical therapy agents seemed to have greater effects than intra-articular viscosupplementation on disability and pain. In the other cases, both intra-articular viscosupplementation and physical and rehabilitative interventions seemed to be equally effective in improving disability, pain, and quality of life[11].
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Radiopedia Shoulder Osteoarthritis Available: https://radiopaedia.org/articles/osteoarthritis-of-the-shoulder(accessed 22.6.2022)
- ↑ Memel DS, Kirwan JR, Sharp DJ, Hehir M. General practitioners miss disability and anxiety as well as depression in their patients with osteoarthritis. Br J Gen Pract. 2000 Aug 1;50(457):645-8. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1313776/ (last accessed 20.11.2019)
- ↑ Complete physio What is shoulder osteoarthritis (OA)? Available:https://www.youtube.com/watch?v=Wrcp6-LunXk (accessed 22.6.2022)
- ↑ Ansok CB, Muh SJ. Optimal management of glenohumeral osteoarthritis. Orthopedic research and reviews. 2018;10:9. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6209346/ (last accessed 20.11.2019)
- ↑ N Wei The agony of shoulder arthritis Available from: https://www.youtube.com/watch?v=L7x5JA74d1o (last accessed 20.11.2019)
- ↑ Millett PJ, Gobezie R, Boykin RE. Shoulder osteoarthritis: diagnosis and management. Am Fam Physician. 2008 Sep 1;78(5):605-11. Available from: https://www.aafp.org/afp/2008/0901/p605.html (last accessed 20.11.2019)
- ↑ 7.0 7.1 7.2 Chillemi C, Franceschini V. Shoulder osteoarthritis. Arthritis. 2013;2013. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3556427/ (last accessed 21.11.2019)
- ↑ London Pain Clinic Intra Articular injections for the treatment of shoulder pain Available from: https://www.youtube.com/watch?v=JMc213q9EgU&app=desktop (last accessed 21.11.2019)
- ↑ Rheumatological conditions affecting the shoulder. Family Practice Available from: https://fpnotebook.com/Ortho/Rheum/RhmtlgcCndtnsAfctngThShldr.htm (last accessed 21.11.2019)
- ↑ Bowman S, Awad ME, Hamrick MW, Hunter M, Fulzele S. Recent advances in hyaluronic acid based therapy for osteoarthritis. Clinical and translational medicine. 2018 Dec;7(1):6. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5814393/ (last accessed 22.11.2019)
- ↑ Monticone, Marco & Frizziero, Antonio & Rovere, Giancarlo & Vittadini, Filippo & Uliano, Domenico & Bruna, Silvano & Gatto, Renato & Nava, Claudia & Leggero, Vittorio & Masiero, Stefano. (2015). Hyaluronic acid intra-articular Injection and exercise therapy: effects on pain and disability in subjects affected by lower limb joints osteoarthritis. The Italian Society of Physical and Rehabilitation Medicine (SIMFER) systematic review. European journal of physical and rehabilitation medicine. 52. Available from: https://www.researchgate.net/publication/281780420_Hyaluronic_acid_intra-articular_Injection_and_exercise_therapy_effects_on_pain_and_disability_in_subjects_affected_by_lower_limb_joints_osteoarthritis_The_Italian_Society_of_Physical_and_Rehabilitatio/citation/download (last accessed 22.11.2019)