Sternal Pain - Different Causes
Original Editor - Sofie Van Cutsem
Top Contributors - Laura Ritchie, Kim Jackson, Sofie Van Cutsem, Lucinda hampton, Evan Thomas, Blessed Denzel Vhudzijena, Oyemi Sillo and Joao Costa
Introduction[edit | edit source]
Sternum pain is pain or discomfort in the area of the chest that contains the sternum and the cartilage connecting it to the ribs.
- The sternum is located near the heart, so many people experiencing sternum pain may confuse it with more general chest pain.[1]
- Most cases of sternum pain is unrelated to the heart and caused primarily due to problems with the sternum itself or the nearby cartilage[1]
- Approx. 1-3% of annual visits to a primary care provider in the United States is related to chest pain[2]. In a 2009 study by Sik et al 20-30% of hospital admissions were for chest related pain.[3]However, Aalam et al. reported in a retrospective descriptive study that, despite an increase in visits to emergency departments between 2006 and 2016, admissions fell from 19% in 2006 to 3.9% in 2016.[4]
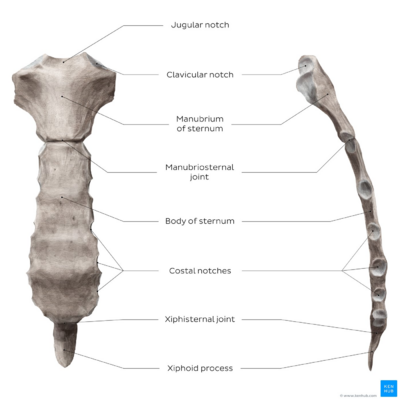
Image: Anatomy of the sternum - anterior and lateral views [5]
Clinical Relevant Anatomy[edit | edit source]
The sternum is a flat bone located in the centre of the anterior thoracic wall.
It consists of three segments;
- Manubrium (uppermost part, see image at R)
- The manubrium articulates with the clavicles, the first ribs and the superior part of the second costal cartilages.[6] The manubrium is quadrangular and lies at the level of the 3rd and 4th thoracic vertebrae. The jugular (suprasternal) notch is the thickest part of the manubrium and is convex anteriorly and concave posteriorly.[6]
- Body (middle part)
- The body of the sternum is longer and thinner than the manubrium. Its margins articulate with the inferior portion of the 2nd costal cartilages, the 3rd to 6th costal cartilages and the superior portion of the 7th costal cartilage.[6]
- Xiphoid process (lowest part).[6]
- The xiphoid process is the lowest and smallest part of the sternum. It articulates with the inferior portion of the 7th costal cartilage and provides attachment for rectus abdominis, transversus abdominis aponeurosis, transversus thoracis and the abdominal diaphragm. [6][7]
Causes of Sternal Pain[edit | edit source]
Sternum pain is usually caused by problems with the muscles and bones near the sternum and not the sternum itself.
Pain felt just behind or below the sternum is called substernal pain and is sometimes caused by gastrointestinal problems[1].
Some of the most common causes of sternum and substernal pain are:
- costochondritis
- clavicular (collarbone) injuries and fractures
- sternoclavicular joint injury
- hernia
- sternal fracture
- acid reflux
- muscular strain or bruise
For more detail on specific causes, see lists below.
Musculoskeletal Causes[edit | edit source]
| Condition | Information |
|---|---|
| Sternal fractures | See Sternal fractures article |
| Stress fractures of the sternum | This type of fracture represents 0.5% of all sternal fractures and is thought to be caused by repetitive contractions of muscles attaching to that bone.[3] Documented cases include weight lifters, a golfer and military recruits performing tricep dips.[3] |
| Clavicle fractures | These fractures account for 8-15% of all paediatric skeletal injuries and 2-5% of all fractures in adults.[8][9] In adults, over 66% of fractures occur at the diaphysis of the clavicle while in children, up to 90% occur in the mid-shaft.[9] Of all clavicle fractures, around 25% occur in the lateral third and 2-3% occur in the medial third.[9] The most common mechanism of injury is a fall onto the arm when the arm is positioned beside the trunk, such as during contact sports.[10] |
| Stress fractures of the rib[2] | The ribs are affected by stress fractures less frequently than bones in the lower extremities.[11] When they do occur, the mechanism typically involves prolonged activity-related fatigue of muscles involved in breathing and/or upper extremity movement, which then decreases the ability of the muscle to absorb and dissipate forces acting on the rib.[11] The anterolateral aspect of the first rib is commonly affected by this condition in sports involving repetitive overhead activities (e.g. tennis, baseball, javelin, basketball and weightlifting).[3][11] It is most susceptible because of a weakness caused by the groove for the subclavian artery and opposing forces of serratus anterior and the scalene muscles.[3] Ribs 4-8 are commonly affected laterally or posterolaterally with activities such as canoeing, rowing, swimming, ballet, gymnastics and golf.[3][11] The posteromedial aspect of the upper ribs can be affected with golf, particularly in inexperienced players who strike the ground more often, which creates a forceful traction on serratus anterior.[11] Contributing factors include technique, equipment, training volume and gender (since rib stress fractures are more common in women).[3] Repetitive coughing can also results in stress fractures of the ribs, typically the lateral or posterolateral aspect of ribs 4-8 due to the interplay between serratus anterior and external oblique.[11] |
| Joint Subluxations | Costovertebral subluxation can occur with rowing, gymnastics, dancing and butterfly swimming and typically results in posterior pain at the levels of the 6th and 7th ribs.[3] Sternoclavicular and sternocostal subluxations are less common and may be related to trauma or congenital hypermobility.[3] |
| Sternoclavicular joint disorders | See SCJ article |
| Costochondritis[2] | An inflammatory condition affecting costochondral junctions or chondrosternal joints. In 90% of patients, more than one area is affected and the most commonly affected areas are the second to fifth junctions.[3][12] Those affected are typically over the age of 40.[12] Clinical signs include localized pain on palpation which may radiate on the chest wall.[3] No swelling occurs with this condition.[3][12] Recent illness involving coughing and recent strenuous exercise or upper extremity usage can cause this type of inflammation. It has been associated with specific movements in sports including rowing and volleyball.[3] |
| Tietze syndrome[2] | A rare inflammatory condition affecting a single costal cartilage (usually the second or third).[12] Those affected are typically under the age of 40. Localized pain and swelling are found with this condition but no warmth or erythema.[3] It can be caused by infection (particularly from chest wall trauma), neoplasms or rheumatological conditions.[12] It is a diagnosis of exclusion and CT scanning should be considered to rule out differential diagnoses such as lymphoma or skin cancer, particularly if the symptoms of suspected Tietze syndrome are persistent.[3] |
| Inflammatory joint disease | For example, osteoarthritis, rheumatoid arthritis and psoriatic arthritis of the sternoclavicular, sternomanubrial or shoulder joints[12][13] |
| Fibromyalgia[2] | A rheumatological condition that can cause persistent and widespread pain including symmetrical tender points at the second costochondral junction as well as the neck, back hip and extremities.[12] |
| General myalgia | Related to a history of chest trauma or recent onset of strenuous exercise to upper body (e.g. rowing). It may be bilateral and affecting multiple costochondral areas. Local muscle groups may also be tender to palpation.[12] |
| Xiphodynia (or painful/hypersensitive xiphoid syndrome) | A condition involving referral of pain to the chest, abdomen, throat, arms and head from an irritated xiphoid process.[2][14] While xiphodynia is usually insidious in nature, trauma may precipitate the syndrome. Acceleration/deceleration injuries, blunt trauma to the chest, unaccustomed heavy lifting and aerobics have been known to lead to the condition.[14] This is a diagnosis of exclusion and serious pathologies should be ruled out before the diagnosis is made.[2][3] It is typically managed using pain medication but in more persistent cases, corticosteroids or lidocaine may be injected and in the most severe cases, the xiphoid cartilage may be surgically excised.[2] |
| Pectoral muscle rupture | A relative uncommon injury that mostly occurs in male athletes between 20 and 40 years of age.[15] Strenuous athletic activity (e.g. football, water-skiing, wrestling) and weight-lifting (particularly the bench press) are the most common activities associated with this injury.[15] Mechanisms of injury are forced abduction against resistance, involuntary contraction and severe traction on the arm. Steroid use may make the muscle more susceptible to rupture. |
| Injuries to muscles other than pec+ (e.g. intercostals, serratus anterior, internal oblique, external oblique)[2] | Typically these strains occur acutely in response to trauma, overuse or when returning to activity after a period of rest.[2][3] |
| Precordial catch syndrome (Texidor’s Twinge)[2] | An uncommon paediatric condition featuring episodes of sharp stabbing pain usually in the region of the left parasternal region or the cardiac apex.[2][16] The pain is typically provoked in slouched positions and is worsened by deep breathing.[2] Episodes typically last from 30 seconds up to three minutes.[3] The condition is thought to be related to spasm of the intercostal muscle(s) but no tenderness is noted on palpation.[2] Management involves reassurance, postural education and pain control as needed.[2] |
| Slipping rib syndrome (aka clicking rib, 12th rib syndrome, rib-tip syndrome)[2][3] | A relatively rare paediatric condition in which hypermobility of a rib causes recurrent focal and unilateral chest pain.[12] [17] Pain referral into the back and a recurrent 'popping' sensation may also be reported.[3][17] Laxity in the sternocostal, costochondral, costovertebral and/or costotransverse ligaments allow for increased mobility and susceptibility to trauma.[17] The hypermobile rib may be able to migrate under the superior rib and can cause intercostal muscle strain, intercostal nerve irritation or sprain of the costal cartilage.[3] In classic SRS, the 8th to 10th ribs are most commonly affected but a rarer variant affects the sternocostal cartilage of one of the 1st to 7th ribs.[17] Pain is reproduced with movement that stresses the affected area as well as palpation and a "hooking" manoeuvre of the affected rib (hooking the fingers under the rib and pulling it anteriorly).[2][3][17] Surgical excision of the affected costal cartilage and anterior rib end is reported to be a curative treatment.[3][17] Non-invasive approaches for less severe presentations include reassurance, analgesics, taping and avoidance of provocative movements.[2][3] A nerve block may also be considered.[3] This condition is rare in adults but may be seen in athletes who perform repetitive trunk movements such as running and swimming.[2][3] |
| Post-surgery | Chronic post-thoracotomy pain syndrome is estimated to occur in 30-60% of patients who have undergone a thoracotomy.[18][19][20] The incidence of post-sternotomy pain is reported to be 35% at three months post-surgery and around 20% at the three year mark (29% in patients over the age of 75 years).[18] Sensory disturbances (e.g. hypersensitivity to touch or pressure) may be more common at around 60-66%.[19][20] However, a smaller subgroup of these patients tend to report severe pain or pain that affects their level of function.[18][21] Thoracotomies and sternotomies may be utilized during surgeries such as thymectomies, Coronary Artery Bypass Graft (CABG), heart valve replacement, lung transplant and lobectomy/pneumonectomy.[20][21][22] Marcassa et al (2015) suggest that inadequate pain management in both the acute post-surgical and the rehabilitation phases may lead to persistent pain in the longer term.[18] In addition, Hetmann et al (2017) supported previous findings suggesting that preoperative pain is also a factor, with most patients who had preoperative pain still reporting pain at 12 months post-surgery whereas most patients who did not have preoperative pain had no pain at the 12 month mark.[19] Patients with this type of pain are more likely to have depression and anxiety.[20]/> |
| Osteomyelitis | An inflammation due to infection of the bone or bone marrow. Osteomyelitis of the sternum is rare and may stem from cardiac surgery, immunodeficiency, chest trauma (e.g. compressions during CPR), IV drug use, tuberculosis or abscess, although some cases have no precipitating factor identified.[23] Osteomyelitis of the rib is also rare (less than 1% of all osteomyelitis[24]) and may stem from chest trauma, thoracic or breast surgery, pneumonia, empyema, immunosupression or fungal infections (which typically as part of multi-system disease in immunocompromised patients).[25][26][24] Mastectomy and radiotherapy for cancer may increase the risk of any infection following breast implant surgery but specific rib osteomyelitis as a complication is extremely rare.[25] |
Cardiovascular Causes[edit | edit source]
- Heart valve disease
- Hypertrophic cardiomyopathy
- Coronary artery disease
- Myocarditis: Caused by infectious agents (e.g. viral) and non-infectious (e.g. lithium, cocaine).[3] Fifty-two percent of cases occur in patients aged 20-39 years old.[3] Symptoms may include chest pain, difficulty breathing, fatigue and palpitations. [3] The patient may report recent flu-like symptoms.[3]
- Pericarditis: Can be caused by infection, sarcoidosis, rheumatoid arthritis and systemic lupus erythematosus.[3] Symptoms present as pleuritic chest pain which is improved by sitting forward and worse with lying down.[3]
- Aortic dissection
- Amyloidosis
Respiratory Causes[edit | edit source]
- Asthma
- Exercise-induced Asthma/Bronchoconstriction[3]
- Bronchitis
- Bronchiectasis
- Chronic Obstructive Pulmonary Disease (COPD)
- Tracheitis
- Tuberculosis
- Pulmonary embolism
- Pleurisy
- Pneumothorax
- Pulmonary hypertension
- Pulmonary sarcoidosis
- Lower Respiratory Infections (e.g. bronchitis, influenza, pneumonia): Chest pain is caused by overuse of chest muscles with coughing or pleural inflammation.[3] Return to intense physical activity should be done with caution to limit risk of complications; the patient should be afebrile and any residual symptoms should be above the neck.[3]
Abdominal and Gastrointestinal Causes[edit | edit source]
- Gastroesophageal reflux disease (GERD): This presents as a burning pain behind the sternum and may occur with a asthma-like symptoms, dry cough and a sore throat.[3]
- Pancreatitis: This condition causes pain in the upper abdomen and lower chest[3]
- Peptic ulcers
- Referred pain from the esophagus:[2] Esophageal spasm could be triggered by anxiety or drinking cold water.[23]
- Boerhaave's Syndrome: This is a rare condition involving an esophageal rupture caused by a sudden increase in intraluminal pressure.[3] Such a rise in pressure may occur as a result of heavy lifting, although a report exists of one case stemming from a spinal manipulation for back pain.[3] Profound retching associated with alcoholism is also linked to this syndrome.[23] Symptoms include pleuritic chest pain and painful swallowing.[3]
Referred Pain[edit | edit source]
From the;[2]
- Shoulders
- Cervical spine
- Thoracic spine including thoracic disc herniation (which is rare given the relative immobility of this region),[2] discitis or a lesion of the spinal cord or vertebral body (e.g. neoplasm).[3]
- Structures below the diaphragm
Cancer[edit | edit source]
- Breast cancer
- Lung cancer
- Lymphoma
- Bone cancer
- Skin cancer[2]
Diagnostic Procedures[edit | edit source]
- A patient who is older than 35 years of age, has a history or risk of coronary artery disease or presents with cardiovascular symptoms should have electrocardiography and possibly a chest x-ray.[12] Cardiac stress testing may also be required to fully rule in or rule out a cardiac dysfunction.[2]
- A patient with fever, cough, chest wall swelling or other respiratory findings on history or examination should also have a chest x-ray.[12]
- X-rays are also used to rule in/out fractures, as are bone scans (since x-rays are negative in 60% of all stress fractures).[11]
- CT scans and MRIs may be indicated with suspected bony injury if further information is required.[2][3]
- CT scans should be done when neoplasms are strongly suspected.[12]
- Nuclear scintigraphy (organ scanning) may be positive with costochondritis but the test is not specific to that condition.[12]
- Blood testing for rheumatoid factor and C-reactive protein (CRP) may be indicated if a rheumatological condition is suspected.[13]
- Elevated white blood cell counts, fever, increased heart rate and increased respiratory rate are likely indicative of an infectious process.[23] MRI is considered the gold standard for identifying osteomyelitis.[25]
- MR imaging and/or ultrasound can help to assess the extent of a muscle rupture and if surgical repair is indicated.[2][15]
Examination[edit | edit source]
- Cardiopulmonary scan - observation (e.g. sweating, skin pallor, skin redness, shortness of breath), breathing rate, heart rate, blood pressure
- Chest pain persisting longer than 12 hours and tenderness on palpation of the anterior chest wall are strong clinical indicators of a musculoskeletal cause of sternal pain.[13]
- Active movements such as deep breathing (to expand the thorax) and elevation of the upper extremities may reinforce a musculoskeletal diagnosis.[12][15]
- Pain during inspiration would be expected in the presence of a rib or sternal fracture, along with painful chest and upper extremity movements and pain on palpation and/or gentle percussion.[2][3]
- If the fracture was a stress fracture, the pain might be difficult to localize at first but may become more prominent and debilitating over time.[3] A bony callous may be palpated over the site of the injury with persistent stress fractures.[11]
- In cases of tubercular osteomyelitis, a palpable abscess or discharging sinus may be observed in addition to chest pain and fever.[26] Swelling from rib osteomyelitis typically occurs near the costochondral junction or the costovertebral angle.[24]
- Resisted testing may pick up true muscular weakness or neurogenic weakness.[2][15] Altered sensory testing and peripheral reflexes in addition to neurogenic weakness may be indicative of thoracic or lower cervical nerve root involvement.
- Questions regarding morning stiffness and other areas of pain or dysfunction as well as general observation of joints may raise the index of suspicion of a rheumatological cause.[12]
- Asymmetry, swelling and bruising (either on the chest or into the axilla and arm) may be observed in the presence of severe muscle injuries such as a pectoralis major rupture and the patient may have felt a 'pop' at the moment of onset.[15]
- For more minor strains, the following information can help to differentiate between structures;[2]
| Muscle | Mechanism | Presentation & Examination |
|---|---|---|
| Intercostal(s) | Excessive exertion of untrained muscles in activities such as coughing, chopping wood or overhead painting and in sports with a lot of upper body exertion such as rowing. | Pain/tenderness on palpation of intercostal(s).
Pain with deep inspiration and coughing. |
| Pectoralis major and/or minor | Direct blow.
Indirect trauma e.g. forceful eccentric contraction when muscle is already under full tension (more common in sports such as weight lifting and rugby), or forced abduction with external rotation or extension (such as in a fall or recreational weight-lifting). |
Sudden arm or shoulder pain reported, possibly with a 'pop.'
+/- Swelling and bruising. +/- Loss of axillary fold, asymmetry, palpable defect in muscle belly. +/- Loss of arm adduction |
| Internal and External Oblique | Muscle lengthening followed by sudden eccentric contraction.
Uncommon injury but when present, typically associated with swimming, javelin throwing, rowing and ice hockey. It is also seen in the non-bowling arm of a cricket fast bowler. |
Pain on palpation of lower four costal cartilages.
Increased pain with resisted trunk side bend towards the injured side. |
| Serratus Anterior | Overuse in activities such as weight lifting and rowing | Pain at medial border of scapula radiating anteriorly.[3]
Pain is reproduced on resisted scapular protraction |
Physical Therapy Management[edit | edit source]
In taking patients history be aware of red flags
While sternum pain is not usually serious, there are some causes of sternum pain that require immediate medical attention. For example;
- Started as a result of direct trauma
- Is accompanied by heart attack symptoms
- Is persistent and does not improve over time
- Is accompanied by intense vomiting or vomiting blood[1]
A brief description of the more common causes and treatment is provided, see links also.
- Rib fracture: Pain management, deep breathing exercises to maintain appropriate lung function and relative rest for the first three weeks post-injury are recommended followed by gradual return to activity (particularly overhead activities).[2] With stress fractures, correction of biomechanics and sport technique may be required to prevent recurrence.[3][11] Delayed or malunion can occur but are typically asymptomatic.[3][11]
- Joint subluxation: Conservative treatment involving pain management and joint manipulation.[3] Surgical debridement may be considered if conservative treatment fails.[3]
- Costochondritis: Reassurance, pain management, mobilization/manipulation and taping as appropriate.[3] This condition typically resolves within one year.[3]
- Acute Myalgia: Relative rest[12]
- Fibromyalgia: Graded exercise[12]
- Muscle strain: Reassurance, pain control (e.g. analgesics, heat) and avoidance of aggravating activities as required in the acute stage. A progressive strengthening program and gradual return to activity in the subacute stage. Consider referral for injections of lidocaine or corticosteroids for persistent cases that do not respond to conservative treatment.[2]
- Pectoralis major rupture:[15] In the initial stage, a sling for comfort, analgesics and rest are required. Early shoulder mobilization and gentle stretching are also recommended. Once pain improves and mobility is back to normal (typically around six to eight weeks), strengthening can be added. Education on weight lifting techniques to reduce further stress on pectoralis major are also recommended (e.g. lowering the weight to no more than 4-6cm above chest wall, using a narrower grip no more than 1.5 times the biacromial width).[15]
- Slipping Rib Syndrome: Typically treated with rest, physiotherapy and intercostal nerve blocks. If chronic and severe, surgical removal of the hypermobile cartilage segment may be performed.[12]
- Sternal Fracture
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Medical news today Causes of sternal pain Available from:https://www.medicalnewstoday.com/articles/320185 (last accessed 4.5.2020)
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 2.24 2.25 2.26 2.27 2.28 2.29 2.30 Ayloo A, Cvengros T, Marella S. Evaluation and treatment of musculoskeletal chest pain. Prim Care. 2013 Dec;40(4):863-87.
- ↑ 3.00 3.01 3.02 3.03 3.04 3.05 3.06 3.07 3.08 3.09 3.10 3.11 3.12 3.13 3.14 3.15 3.16 3.17 3.18 3.19 3.20 3.21 3.22 3.23 3.24 3.25 3.26 3.27 3.28 3.29 3.30 3.31 3.32 3.33 3.34 3.35 3.36 3.37 3.38 3.39 3.40 3.41 3.42 3.43 3.44 3.45 3.46 3.47 3.48 3.49 3.50 Sik EC, Batt ME, Heslop LM. Atypical Chest Pain in Athletes. Curr Spor Med Rep. 2009;8(2):52-58.
- ↑ Aalam AA, Alsabban A, Pines JM. National trends in chest pain visits in US emergency departments (2006–2016). Emergency Medicine Journal. 2020 Nov 1;37(11):696-9.
- ↑ Sternum anatomy image - © Kenhub https://www.kenhub.com/en/library/anatomy/sternum
- ↑ 6.0 6.1 6.2 6.3 6.4 Grant JCB. Grant's Atlas of Anatomy. 6th ed. Baltimore: The Williams and Wilkins Co; 1972.
- ↑ Broyles R. The location and purpose of the Xiphoid process [Internet]. Troy: Bright Hub Inc; 2009 [updated 7 March 2017; cited 24 January 2018]. Available from:http://www.brighthub.com/science/medical/articles/57775.aspx
- ↑ Adamich J, Howard A, Camp M. Do All Clavicle Fractures in Children Need To Be Managed by Orthopedic Surgeons? Pediatr Emerg Care. 2017 Sep 18. doi: 10.1097/PEC.0000000000001269. [Epub ahead of print]
- ↑ 9.0 9.1 9.2 van der Meijden OA, Gaskill TR, Millett PJ. Treatment of clavicle fractures: current concepts review. J Shoulder Elbow Surg. 2012;21(3):423-9.
- ↑ Pecci M, Kreher J. Clavicle fractures. Am Fam Physician. 2008;77(1):65-70.
- ↑ 11.0 11.1 11.2 11.3 11.4 11.5 11.6 11.7 11.8 11.9 Connolly LP, Connolly SA. Rib stress fractures. Clin Nucl Med. 2004;29(10):614-6.
- ↑ 12.00 12.01 12.02 12.03 12.04 12.05 12.06 12.07 12.08 12.09 12.10 12.11 12.12 12.13 12.14 12.15 12.16 12.17 Proulx AM, Zryd TW. Costochondritis; diagnosis and treatment. Am Fam Physician. 2009;80(6):617-20.
- ↑ 13.0 13.1 13.2 How J, Volz G, Doe S, Heycock C, Hamilton J, Kelly C. The causes of musculoskeletal chest pain in patients admitted to hospital with suspected myocardial infarction. Eur J Intern Med. 2005;16(6):432-6.
- ↑ 14.0 14.1 Simpson JK, Hawken E. Xiphodynia: A diagnostic conundrum. Chiropr Osteopat. 2007, 15:13.
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 15.6 15.7 Petilon J, Carr DR, Sekiya JK, Unger DV. Pectoralis major muscle injuries: evaluation and management. J Am Acad Orthop Surg. 2005;13(1):59-68.
- ↑ Gumbiner CH. Precordial catch syndrome. South Med J. 2003;96(1):38-41.
- ↑ 17.0 17.1 17.2 17.3 17.4 17.5 Bonasso PC, Petrus SN, Smith SD, Jackson RJ. Sternocostal slipping rib syndrome. Pediatr Surg Int. 2017 Dec 6. doi: 10.1007/s00383-017-4221-1. [Epub ahead of print]
- ↑ 18.0 18.1 18.2 18.3 Marcassa C, Faggiano P, Greco C, Ambrosetti M, Temporelli PL. A retrospective multicenter study on long-term prevalence of chronic pain after cardiac surgery. J Cardiovasc Med (Hagerstown). 2015;16(11):768-74.
- ↑ 19.0 19.1 19.2 Hetmann F, Kongsgaard UE, Sandvik L, Schou-Bredal I. Post-thoracotomy pain syndrome and sensory disturbances following thoracotomy at 6- and 12-month follow-ups. J Pain Res. 2017;10:663-668.
- ↑ 20.0 20.1 20.2 20.3 Springer JS, Karlsson P, Madsen CS, Johnsen B, Finnerup NB, Jensen TS, Nikolajsen L. Functional and structural assessment of patients with and without persistent pain after thoracotomy. Eur J Pain. 2017;21(2):238-249.
- ↑ 21.0 21.1 Kalso E, Mennander S, Tasmuth T, Nilsson E. Chronic post-sternotomy pain. Acta Anaesthesiol Scand. 2001;45(8):935-9.
- ↑ Meyerson J, Thelin S, Gordh T, Karlsten R. The incidence of chronic post-sternotomy pain after cardiac surgery--a prospective study. Acta Anaesthesiol Scand. 2001;45(8):940
- ↑ 23.0 23.1 23.2 23.3 Vacek TP, Rehman S, Yu S, Moza A, Assaly R. Another cause of chest pain: Staphylococcus aureus sternal osteomyelitis in an otherwise healthy adult. Int Med Case Rep J. 2014;7:133-7.
- ↑ 24.0 24.1 24.2 Idrissa S, Tazi M, Cherrabi H, Souley A, Mahmoudi A, Elmadi A, Khattala K, Bouabdallah Y. Multifocal rib osteomyelitis in children: a case report and literature review. J Surg Case Rep. 2017 Jul 31;2017(7):rjx142.
- ↑ 25.0 25.1 25.2 Watson L, Dunn D, Fraser-Kirk G. Indolent Rib Osteomyelitis Following Breast Implant Reconstruction: An Unusual Case and Review of the Literature. Aesthetic Plast Surg. 2017 Oct 12. doi: 10.1007/s00266-017-0975-z. [Epub ahead of print]
- ↑ 26.0 26.1 Kashyap NK, Jindal A, Borkar NK, Wasnik M. Primary Tuberculotic Osteomyelitis of Rib in a Child. J Clin Diagn Res. 2017 Jul;11(7):PD08-PD09.
- ↑ Trevor Minor. Hooking Maneuver - Test for Slipping Rib Syndrome. Available from: http://www.youtube.com/watch?v=PiLZ5cVP5bA[last accessed 21/03/23]