Patellar Fractures: Difference between revisions
Leana Louw (talk | contribs) No edit summary |
Leana Louw (talk | contribs) No edit summary |
||
| Line 11: | Line 11: | ||
== Clinically relevant anatomy == | == Clinically relevant anatomy == | ||
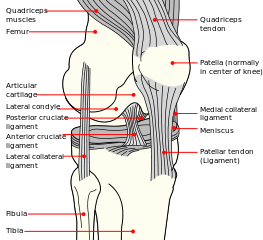
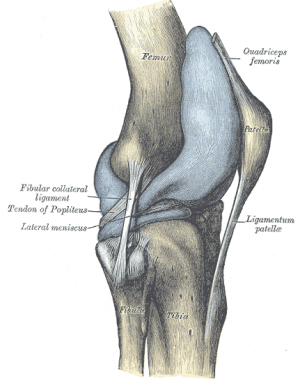
The patella is a triangular bone situated on the anterior surface of the knee at the distal end of the femur. It is the largest sesamoïd bone in the body and makes part of the knee joint.<ref>Cedars-Sinai. Fractured Kneecap. Cedars Sinai organisation. https://www.cedars-sinai.org/health-library/diseases-and-conditions/f/fractured-kneecap.html (accessed 25/07/2018).</ref><ref>Schunke M. Anatomische atlas Prometheus, algemene anatomie en bewegingsapparaat. Bohn Stafieu van Loghum: 2e druk. 2010.</ref><ref>Everett L. Knee and Lower Leg. In: Marx J, Walls R, Hockberger R, editors. Rosen's Emergency Medicine: Concepts and Clinical Practice. 6th ed. Philadelphia: Mosby Elsevier, 2006.</ref> Vastus medialis and lateralis, as part of the quadriceps group, control movement at the patella.<ref>Orthopaedia. Collaborative Orthopaedic Knowledgebase, http://www.orthopaedia.com/display/Main/Patella+fractures (accessed November 10, 2010).</ref> The extensor mechanism as a whole plays a major role in patella fractures. This consists of the quadriceps, quadriceps tendon, retinaculum, patella tendon, tibial tubercle and patellofemoral and patellotibial ligaments | The patella is a triangular bone situated on the anterior surface of the knee at the distal end of the femur. It is the largest sesamoïd bone in the body and makes part of the knee joint.<ref>Cedars-Sinai. Fractured Kneecap. Cedars Sinai organisation. https://www.cedars-sinai.org/health-library/diseases-and-conditions/f/fractured-kneecap.html (accessed 25/07/2018).</ref><ref>Schunke M. Anatomische atlas Prometheus, algemene anatomie en bewegingsapparaat. Bohn Stafieu van Loghum: 2e druk. 2010.</ref><ref>Everett L. Knee and Lower Leg. In: Marx J, Walls R, Hockberger R, editors. Rosen's Emergency Medicine: Concepts and Clinical Practice. 6th ed. Philadelphia: Mosby Elsevier, 2006.</ref> Vastus medialis and lateralis, as part of the quadriceps group, control movement at the patella.<ref>Orthopaedia. Collaborative Orthopaedic Knowledgebase, http://www.orthopaedia.com/display/Main/Patella+fractures (accessed November 10, 2010).</ref> The extensor mechanism as a whole plays a major role in patella fractures. This consists of the quadriceps, quadriceps tendon, retinaculum, patella tendon, tibial tubercle and patellofemoral and patellotibial ligaments.<ref name=":11" /> See the page on the [[patella]] for more details on the anatomy. | ||
{| | {| | ||
| Line 22: | Line 22: | ||
== Epidemiology/Etiology == | == Epidemiology/Etiology == | ||
In a recent study, the average mortality rate at one year after patella fractures was 2.8%, increasing to 6.2% in the geriatric population. Patella fractures are not associated with an increased mortality rate, as the relative risk of death was 0.9.<ref>Larsen P, Elsoe R. [https://www.sciencedirect.com/science/article/pii/S0020138318303590 Patella fractures are not associated with an increased risk of mortality in elderly patients]. Injury 2018.</ref | In a recent study, the average mortality rate at one year after patella fractures was 2.8%, increasing to 6.2% in the geriatric population. Patella fractures are not associated with an increased mortality rate, as the relative risk of death was 0.9.<ref>Larsen P, Elsoe R. [https://www.sciencedirect.com/science/article/pii/S0020138318303590 Patella fractures are not associated with an increased risk of mortality in elderly patients]. Injury 2018.</ref> | ||
== Complications == | == Complications == | ||
* Injuries (sprain/rupture) to ligaments and tendons attached to the patella | * Injuries (sprain/rupture) to ligaments and tendons attached to the patella | ||
* Avascular necrosis<ref name=":4">Medscape. Patella Fracture Imaging. http://emedicine.medscape.com/article/394270-overview&gt (accessed 25/07/2018). | * Avascular necrosis<ref name=":4">Medscape. Patella Fracture Imaging. http://emedicine.medscape.com/article/394270-overview&gt (accessed 25/07/2018). | ||
</ref> | </ref> | ||
* | * Post-traumatic arthritis | ||
* Osteochondral damage to patella-femoral joint | * Osteochondral damage to patella-femoral joint | ||
* Stiffness | * Stiffness | ||
* Non-union | * Non-union | ||
* Malunion | * Malunion | ||
* <ref name=":1" / | * Concomitant injuries (e.g. injuries to the acetabulum, femur and tibia) | ||
* Long term complications:<ref>Insall JN. Fractured kneecap: treatments. Institute for Orthopaedics and sports medicine 2007.</ref> | |||
** Stiffness | |||
** Extension weakness | |||
** Patellofemoral arthritis. | |||
<ref name=":1" /> | |||
== Characteristics/Clinical Presentation == | == Characteristics/Clinical Presentation == | ||
| Line 47: | Line 49: | ||
** Most common type | ** Most common type | ||
** Proximal blood supply may be compromised | ** Proximal blood supply may be compromised | ||
** Usually as a result of hyper flexion of the knee | ** Usually as a result of hyper-flexion of the knee | ||
* Marginal: As a result of a fall on the knee | * Marginal: As a result of a fall on the knee | ||
* Vertical | * Vertical/longitudinal | ||
* Lower/upper pole | * Lower/upper pole | ||
* Osteochondral | * Osteochondral | ||
| Line 55: | Line 57: | ||
<ref name=":2" /><ref name=":3" /><ref name=":4" /><ref name=":5">Whittle PA. Fractures of the Lower Extremity. In: Canale ST, Beaty JH, editors. Campbell's Operative Orthopaedics. 11th ed. Philadelphia: Mosby Elsevier, 2008.</ref><ref>Melvin SJ, Mehta S. [https://journals.lww.com/jaaos/Abstract/2011/04000/Patellar_Fractures_in_Adults.4.aspx Patellar fractures in adults.] Journal of the American Academy of Orthopaedic Surgeons 2011;19(4):198-207.</ref><ref name=":7">Walters J, editor. Orthopaedics - A guide for practitioners. 4th Edition. Cape Town: University of Cape Town, 2010.</ref> | <ref name=":2" /><ref name=":3" /><ref name=":4" /><ref name=":5">Whittle PA. Fractures of the Lower Extremity. In: Canale ST, Beaty JH, editors. Campbell's Operative Orthopaedics. 11th ed. Philadelphia: Mosby Elsevier, 2008.</ref><ref>Melvin SJ, Mehta S. [https://journals.lww.com/jaaos/Abstract/2011/04000/Patellar_Fractures_in_Adults.4.aspx Patellar fractures in adults.] Journal of the American Academy of Orthopaedic Surgeons 2011;19(4):198-207.</ref><ref name=":7">Walters J, editor. Orthopaedics - A guide for practitioners. 4th Edition. Cape Town: University of Cape Town, 2010.</ref> | ||
The prognosis of the injury depends on the amount of chondral damage at the time of injury. Functional outcome depends on the ability to achieve pain-free and | The prognosis of the injury depends on the amount of chondral damage at the time of injury. Functional outcome depends on the ability to achieve pain-free and stable range of motion in an early stage. <ref name=":6">Mehling I, Mehling A, Rommens PM. [https://www.sciencedirect.com/science/article/pii/S026808900600168X Comminuted patellar fractures.] Current Orthopaedics 2006;20(6):397-404.</ref> | ||
== Differential diagnosis == | == Differential diagnosis == | ||
* Bipartite patella<ref name=":1" /> | * Bipartite patella<ref name=":1" /> | ||
* [[Multiligament Injured Knee Dislocation|Knee dislocation]] | |||
* Patella dislocation | |||
== Diagnosis == | == Diagnosis == | ||
| Line 94: | Line 98: | ||
=== Special investigations === | === Special investigations === | ||
* X-rays: | * [[X-Rays|X-rays]]: | ||
** AP view: | ** AP view: | ||
*** May be difficult to see patella | *** May be difficult to see patella | ||
** Lateral view: | ** Lateral view: | ||
*** Undisplaced - < 2mm separation | *** Undisplaced - < 2mm separation | ||
*** Displaced - > 2mm separation | *** Displaced - > 2mm separation, step deformity noted | ||
** Sky view | ** Sky view | ||
** | ** Used for regular monitoring of healing process and any possible complications | ||
* CT scan: Usually not needed | * [[CT Scans|CT scan]]: Usually not needed | ||
* MRI: Diagnosis of associated injuries to nearby tendons and ligaments | * [[MRI Scans|MRI]]: Diagnosis of associated injuries to nearby tendons and ligaments | ||
* Bone scans: To identify stress fractures | * Bone scans: To identify stress fractures | ||
<ref name=":7" /><ref name=":8" /><ref name=":9" /><ref name=":11" /> | <ref name=":7" /><ref name=":8" /><ref name=":9" /><ref name=":11" /> | ||
| Line 114: | Line 118: | ||
* [http://www.physio-pedia.com/McGill_Pain_Questionnaire McGill pain questionnaire] | * [http://www.physio-pedia.com/McGill_Pain_Questionnaire McGill pain questionnaire] | ||
== Medical management == | == Medical management == | ||
* In acute cases, local anesthetics can be given to eliminate pain.<ref name="p4" /> This helps to aid in the assessment and diagnosis of the patella fracture. | |||
In acute cases, local anesthetics can be given to eliminate pain.<ref name="p4" /> This helps to aid in the assessment and diagnosis of the patella fracture. | |||
=== Conservative management === | === Conservative management === | ||
Indication: Undisplaced fracture (mostly vertical and | Indication: Undisplaced fracture (mostly vertical, horizontal and comminuted fractures) with extensor mechanism in place <ref name=":1" /><ref name=":6" /> | ||
Management: | Management:<ref name=":7" /><ref name=":6" /><ref name=":11">Duke Orthopaedics. Wheeless’ textbook of Orthopaedics. Fractures of the patella.http://www.wheelessonline.com/ortho/fractures_of_the_patella (accessed November 10 2010).</ref><ref name=":10">American Academy of Orthopaedic Surgeons. Diseases and conditions - Patellar (Kneecap) Fractures. http://orthoinfo.aaos.org/topic.cfm?topic=A00523 (accessed November 10 2010).</ref> | ||
* Fracture immobilized with cast or | * Fracture immobilized with POP cylinder cast or range of motion brace locked in extension (4-6 weeks): | ||
** As healing takes place, knee flexion can gradually be increased | ** As healing takes place, knee flexion can gradually be increased | ||
** | ** Range of motion brace must be worn until union (on X-rays) and clinical signs of healing (not tender on palpation) are present | ||
* Crutch walking 6-8 weeks | * Crutch walking 6-8 weeks | ||
* Rehabilitation | * Rehabilitation | ||
| Line 130: | Line 133: | ||
Indication: Significant displacement with extensor mechanism not intact.<ref name=":1" /> | Indication: Significant displacement with extensor mechanism not intact.<ref name=":1" /> | ||
Aim: Restore extensor function, align articular incongruities, and allow early motion<ref name=":6" /><ref name=":9" /><ref>Shang ZG. Patellar fractures treatment and management. Unbound medline 2013;26(6):445-8.</ref><ref>Strauss J. ORIF Patella Fracture Post-Operative Rehabilitation Protocol, Hospital for Joint Diseases, 2008.</ref> | Aim: Restore extensor function, align articular incongruities, and allow early motion<ref name=":6" /><ref name=":9" /><ref>Shang ZG. Patellar fractures treatment and management. Unbound medline 2013;26(6):445-8.</ref><ref name=":0">Strauss J. ORIF Patella Fracture Post-Operative Rehabilitation Protocol, Hospital for Joint Diseases, 2008.</ref> | ||
Management:<ref name=":1" /><ref name=":7" /> | |||
* Transverse/simple, comminuted mid-patella fracture: Open reduction and internal fixation using tension band wire technique using pins and wires and 'a figure of eight' to press the pieces together | |||
** POP cast in extension for 6 weeks | |||
* Proximal/distal <1/3 - simple or comminuted: Excision of small piece & tendon repair | |||
** POP cast for 6 weeks | |||
* Longitudinal (uncommon): Interfragmentary screw fixation | |||
* Comminuted fracture/irreducible or irreparable fracture or when cartilage too badly damaged: Partial vs complete patellectomy:<ref name="p4" /> | |||
** Quadriceps muscles is is attached to the patellar ligament to ensure function of the extensor apparatus during a complete patellectomy<ref name="p4" /> | |||
** Patellectomy: Relatively old procedure, <u>last treatment of choice</u> | |||
* Repair of bilateral vastus muscles | * Repair of bilateral vastus muscles | ||
* Rehabilitation same as with conservative management<br> | * Rehabilitation same as with conservative management<br> | ||
| Line 145: | Line 154: | ||
== Physiotherapy management == | == Physiotherapy management == | ||
As clinical healing phases do not always correlate with theoretical healing, the surgeon will guide rehabilitation taking X-ray findings into consideration. The following is a guide to be used in the rehabilitation of a patient after a patella fracture, but it is always good to discuss treatment plans with your orthopaedic surgeons. | |||
=== Conservative management === | |||
Conservative management are used when the extensor mechanism is still intact.<ref name=":1" /> | |||
==== Phase 1: 0-6 weeks ==== | |||
* Range of motion (as per surgeon): | |||
** Range of motion brace locked in extension 2-3 weeks | |||
** Controlled motion brace at 2-3 weeks | |||
** Exercises: | |||
*** Open kinetic chain strengthening and knee range of motion at 3-4 weeks - focus on active flexion & extension in inner ranges | |||
*** Quadriceps | |||
*** Hamstring | |||
*** Gluts sets | |||
*** SLR | |||
*** Open and closed kinetic chains hip strengthening exercises | |||
*** Circulatory drills | |||
* Weight-bearing: | |||
** Partial weight-bearing in brace | |||
** May stand tandem | |||
** Weight-bearing restrictions normally apply for 6-8 weeks<ref name=":11" /><ref name=":10" /> | |||
** Duration of crutches/weight-bearing restrictions as per surgeon | |||
* Patella mobilization | |||
* Pain & oedema management using [[cryotherapy]] | |||
<ref name=":1" /><ref name=":0" /> | |||
==== Phase II: 6-12 weeks ==== | |||
* Range of motion knee brace as per surgeon | |||
* Range of motion: | |||
** Progress to full knee flexion & extension | |||
* Exercises: | |||
** Stationary bike with seat elevated and no resistance | |||
** Progress closed kinetic chain exercises: Mini squats, step up, retro step, etc | |||
** Progress resistance on hip exercises | |||
** Proprioception | |||
** Lunges from weeks 8-10 | |||
<ref name=":0" /> | |||
=== Post-operative rehabilitation === | |||
Surgical intervention are done in cases where there are significant displacement and the extensor mechanism is not intact. Open reduction and internal fixation using the tension band wire technique is normally the treatment of choice.<ref name=":1" /> | |||
==== Phase I: 0-2 weeks ==== | |||
* Range of motion brace set at 0-30° | |||
** Only to be taken off for physiotherapy sessions | |||
* <br> | |||
ignificant displacement, extensor mechanism not intact. ORIF tension band wire technique. Repari or bilater. vastus. same rehab as with no-operative-SPORT<br> | ignificant displacement, extensor mechanism not intact. ORIF tension band wire technique. Repari or bilater. vastus. same rehab as with no-operative-SPORT<br> | ||
| Line 194: | Line 243: | ||
(Strauss J. (MD)(level of evidence : 5), Elizabeth Arendt(MD) ( level of evidence: 5) ) | (Strauss J. (MD)(level of evidence : 5), Elizabeth Arendt(MD) ( level of evidence: 5) ) | ||
<br> | <br> | ||
== Resources <br> == | == Resources <br> == | ||
Revision as of 22:12, 29 July 2018
***Editing in process***
Definition/Description[edit | edit source]
Patella fractures are caused by directly by trauma or a compressive force, or indirectly as the result of quadriceps contractions or excessive stress to the extensor mechanism.[1][2][3] Indirect injuries are commonly associated with tears of the retinaculum and vastus muscles.[1] Patella fractures make up about 1% of all skeletal injuries.[4][5]
Clinically relevant anatomy[edit | edit source]
The patella is a triangular bone situated on the anterior surface of the knee at the distal end of the femur. It is the largest sesamoïd bone in the body and makes part of the knee joint.[6][7][8] Vastus medialis and lateralis, as part of the quadriceps group, control movement at the patella.[9] The extensor mechanism as a whole plays a major role in patella fractures. This consists of the quadriceps, quadriceps tendon, retinaculum, patella tendon, tibial tubercle and patellofemoral and patellotibial ligaments.[10] See the page on the patella for more details on the anatomy.
Epidemiology/Etiology[edit | edit source]
In a recent study, the average mortality rate at one year after patella fractures was 2.8%, increasing to 6.2% in the geriatric population. Patella fractures are not associated with an increased mortality rate, as the relative risk of death was 0.9.[11]
Complications[edit | edit source]
- Injuries (sprain/rupture) to ligaments and tendons attached to the patella
- Avascular necrosis[12]
- Post-traumatic arthritis
- Osteochondral damage to patella-femoral joint
- Stiffness
- Non-union
- Malunion
- Concomitant injuries (e.g. injuries to the acetabulum, femur and tibia)
- Long term complications:[13]
- Stiffness
- Extension weakness
- Patellofemoral arthritis.
Characteristics/Clinical Presentation[edit | edit source]
Types of fractures[edit | edit source]
Patella fractures are classified as either displaced or non-displaced. Displaced fractures are unstable and can be further classified as:[14]
- Comminuted: As a result of direct trauma (mostly due to blows or falls on flexed knee)
- Can cause damage to the articular cartilage of patella and femoral condyles.
- Tansverse/stellate: As a result of muscle contraction/extensive stress on the extensor mechanism, e.g. explosive quadriceps contraction after jumping from height.
- Most common type
- Proximal blood supply may be compromised
- Usually as a result of hyper-flexion of the knee
- Marginal: As a result of a fall on the knee
- Vertical/longitudinal
- Lower/upper pole
- Osteochondral
- Sleeve (only in paediatric patients)
The prognosis of the injury depends on the amount of chondral damage at the time of injury. Functional outcome depends on the ability to achieve pain-free and stable range of motion in an early stage. [17]
Differential diagnosis[edit | edit source]
- Bipartite patella[1]
- Knee dislocation
- Patella dislocation
Diagnosis[edit | edit source]
Interview[edit | edit source]
- Details regarding accident
- Mechanism of injury
- Pain at knee
- Complaints of difficulty standing or snapping sensation at knee
Physical examination[edit | edit source]
- Observation:
- Whole extremity
- Swollen, bruised knee
- Deformity around knee
- Possible wounds (open fracture)
- Palpation (often done after local anesthetics to eliminate pain):
- Tenderness around patella
- Palpable gap (for displaced fractures)
- Rule out concomitant injuries:
- e.g. fractures of the acetabulum, femur and tibia
- Haemarthrosis
- Range of motion:
- Acute:
- Limited knee and painful knee flexion and extension
- Often unable to do straight leg raise
- Chronic:
- Full knee flexion with extension lag
- Acute:
- Distal pulses
- Assess compartment of the leg
- Neurological assessment
Special investigations[edit | edit source]
- X-rays:
- AP view:
- May be difficult to see patella
- Lateral view:
- Undisplaced - < 2mm separation
- Displaced - > 2mm separation, step deformity noted
- Sky view
- Used for regular monitoring of healing process and any possible complications
- AP view:
- CT scan: Usually not needed
- MRI: Diagnosis of associated injuries to nearby tendons and ligaments
- Bone scans: To identify stress fractures
Outcome measures[edit | edit source]
- Knee injury and osteoarthritis outcome score
- Knee outcome survey
- Lower extrimity function scale
- McGill pain questionnaire
Medical management[edit | edit source]
- In acute cases, local anesthetics can be given to eliminate pain.[18] This helps to aid in the assessment and diagnosis of the patella fracture.
Conservative management[edit | edit source]
Indication: Undisplaced fracture (mostly vertical, horizontal and comminuted fractures) with extensor mechanism in place [1][17]
- Fracture immobilized with POP cylinder cast or range of motion brace locked in extension (4-6 weeks):
- As healing takes place, knee flexion can gradually be increased
- Range of motion brace must be worn until union (on X-rays) and clinical signs of healing (not tender on palpation) are present
- Crutch walking 6-8 weeks
- Rehabilitation
Surgical intervention[edit | edit source]
Indication: Significant displacement with extensor mechanism not intact.[1]
Aim: Restore extensor function, align articular incongruities, and allow early motion[17][20][23][24]
- Transverse/simple, comminuted mid-patella fracture: Open reduction and internal fixation using tension band wire technique using pins and wires and 'a figure of eight' to press the pieces together
- POP cast in extension for 6 weeks
- Proximal/distal <1/3 - simple or comminuted: Excision of small piece & tendon repair
- POP cast for 6 weeks
- Longitudinal (uncommon): Interfragmentary screw fixation
- Comminuted fracture/irreducible or irreparable fracture or when cartilage too badly damaged: Partial vs complete patellectomy:[18]
- Quadriceps muscles is is attached to the patellar ligament to ensure function of the extensor apparatus during a complete patellectomy[18]
- Patellectomy: Relatively old procedure, last treatment of choice
- Repair of bilateral vastus muscles
- Rehabilitation same as with conservative management
Later stages:
Manipulation under anesthesia or the arthroscopic releasing of adhesions is required when athrofibrosis occurs.[17]
Physiotherapy management[edit | edit source]
As clinical healing phases do not always correlate with theoretical healing, the surgeon will guide rehabilitation taking X-ray findings into consideration. The following is a guide to be used in the rehabilitation of a patient after a patella fracture, but it is always good to discuss treatment plans with your orthopaedic surgeons.
Conservative management[edit | edit source]
Conservative management are used when the extensor mechanism is still intact.[1]
Phase 1: 0-6 weeks[edit | edit source]
- Range of motion (as per surgeon):
- Range of motion brace locked in extension 2-3 weeks
- Controlled motion brace at 2-3 weeks
- Exercises:
- Open kinetic chain strengthening and knee range of motion at 3-4 weeks - focus on active flexion & extension in inner ranges
- Quadriceps
- Hamstring
- Gluts sets
- SLR
- Open and closed kinetic chains hip strengthening exercises
- Circulatory drills
- Weight-bearing:
- Patella mobilization
- Pain & oedema management using cryotherapy
Phase II: 6-12 weeks[edit | edit source]
- Range of motion knee brace as per surgeon
- Range of motion:
- Progress to full knee flexion & extension
- Exercises:
- Stationary bike with seat elevated and no resistance
- Progress closed kinetic chain exercises: Mini squats, step up, retro step, etc
- Progress resistance on hip exercises
- Proprioception
- Lunges from weeks 8-10
Post-operative rehabilitation[edit | edit source]
Surgical intervention are done in cases where there are significant displacement and the extensor mechanism is not intact. Open reduction and internal fixation using the tension band wire technique is normally the treatment of choice.[1]
Phase I: 0-2 weeks[edit | edit source]
- Range of motion brace set at 0-30°
- Only to be taken off for physiotherapy sessions
ignificant displacement, extensor mechanism not intact. ORIF tension band wire technique. Repari or bilater. vastus. same rehab as with no-operative-SPORT
Treatment procedure Post-Operative :
Phase
I:
0-2
Weeks
Knee
Immobilizer:
Worn
at
all
times
(taken
off
only
for
physical
therapy
sessions
converted
to
hinged
knee)
brace is worn
at
first
post‐op
visit
- Weight bearing: with the knee locked in extension
- Range of Motion: 0‐30 degrees
- Therapeutic Exercises:
•
Isometric
quadriceps/hamstring/adductor/abductor
strengthening,
• Ankle
theraband exercises
Phase
II:
2-6
Weeks
Knee
Brace:
Worn
with
weight bearing
activities
still
locked
in
full
extension,
may
be
removed
at
night
- Weightbearing:
- Range of Motion: add 15 degrees of flexion each week –
- Goal is 90 degrees by post‐op week 6
- Therapeutic Exercises:
• Isometric
quadriceps/hamstring/adductor/abductor
strengthening,
• Ankle
theraband
exercises,
• Initiate
straight
leg
raises
Phase
III:
6-10
Weeks
Knee
Brace:
Unlocked,
worn
with
weight bearing
activities
- Weightbearing: Full
- Range of Motion: progress to full ROM by post‐operative week 10
- Therapeutic Exercises: Isometric quadriceps/hamstring/adductor/abductor strengthening, Ankle theraband exercises, Initiate straight leg raises
Phase
IV:
10-12
Weeks
Knee
Brace:
Discontinue
- Weightbearing: Full
- Range of Motion: Full
- Therapeutic Exercises: Isometric quadriceps/hamstring/adductor/abductor strengthening, Ankle theraband exercises, Initiate straight leg raises, Start stationary bicycle
Phase
V:
36
Months: return
to
full
activities
as
tolerated
(Strauss J. (MD)(level of evidence : 5), Elizabeth Arendt(MD) ( level of evidence: 5) )
Resources
[edit | edit source]
http://www.physioroom.com/injuries/knee/patella_fracture_full.php
http://www.summitmedicalgroup.com/library/adult_health/smapatellarfractureexecises_references/
http://www.mdguidelines.com/fracture-patella
http://www.ncbi.nlm.nih.gov/pubmed/?term=patellar%20fracture
http://www.healthline.com/human-body-maps/knee
References
[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 1.8 1.9 Frobell R, Cooper R, Morris H, Arendt, H. Acute knee injuries. In: Brukner P, Bahr R, Blair S, Cook J, Crossley K, McConnell J, McCrory P, Noakes T, Khan K. Clinical Sports Medicine: 4th edition. Sydney: McGraw-Hill. p.626-683
- ↑ 2.0 2.1 Schuett DJ, Hake ME, Mauffrey C, Hammerberg EM, Stahel PF, Hak DJ. Current treatment strategies for patella fractures. Orthopedics. 2015;38(6):377-84.
- ↑ 3.0 3.1 Archdeacon, Michael T., and Roy W. Sanders. Chapter 54 - Patella Fractures and Extensor Mechanism Injuries. In: Browner BD, Jupiter JB, Krettek C, Anderson PA, editors. Skeletal Trauma, 4th edition. Elsevier Health Sciences, 2008.
- ↑ Crowther MA, Mandal A, Sarangi PP. Propagation of stress fracture of the patella. British journal of sports medicine 2005;39(2):e6.
- ↑ Sweetnam R. Patellectomy. Postgraduate medical journal 1964 Sep;40(467):531.
- ↑ Cedars-Sinai. Fractured Kneecap. Cedars Sinai organisation. https://www.cedars-sinai.org/health-library/diseases-and-conditions/f/fractured-kneecap.html (accessed 25/07/2018).
- ↑ Schunke M. Anatomische atlas Prometheus, algemene anatomie en bewegingsapparaat. Bohn Stafieu van Loghum: 2e druk. 2010.
- ↑ Everett L. Knee and Lower Leg. In: Marx J, Walls R, Hockberger R, editors. Rosen's Emergency Medicine: Concepts and Clinical Practice. 6th ed. Philadelphia: Mosby Elsevier, 2006.
- ↑ Orthopaedia. Collaborative Orthopaedic Knowledgebase, http://www.orthopaedia.com/display/Main/Patella+fractures (accessed November 10, 2010).
- ↑ 10.0 10.1 10.2 10.3 Duke Orthopaedics. Wheeless’ textbook of Orthopaedics. Fractures of the patella.http://www.wheelessonline.com/ortho/fractures_of_the_patella (accessed November 10 2010).
- ↑ Larsen P, Elsoe R. Patella fractures are not associated with an increased risk of mortality in elderly patients. Injury 2018.
- ↑ 12.0 12.1 Medscape. Patella Fracture Imaging. http://emedicine.medscape.com/article/394270-overview> (accessed 25/07/2018).
- ↑ Insall JN. Fractured kneecap: treatments. Institute for Orthopaedics and sports medicine 2007.
- ↑ 14.0 14.1 Whittle PA. Fractures of the Lower Extremity. In: Canale ST, Beaty JH, editors. Campbell's Operative Orthopaedics. 11th ed. Philadelphia: Mosby Elsevier, 2008.
- ↑ Melvin SJ, Mehta S. Patellar fractures in adults. Journal of the American Academy of Orthopaedic Surgeons 2011;19(4):198-207.
- ↑ 16.0 16.1 16.2 16.3 16.4 Walters J, editor. Orthopaedics - A guide for practitioners. 4th Edition. Cape Town: University of Cape Town, 2010.
- ↑ 17.0 17.1 17.2 17.3 17.4 Mehling I, Mehling A, Rommens PM. Comminuted patellar fractures. Current Orthopaedics 2006;20(6):397-404.
- ↑ 18.0 18.1 18.2 18.3 18.4 Günal I, Karatosun V. Patellectomy: an overview with reconstructive procedures. Clinical Orthopaedics and Related Research 2001;389:74-8.
- ↑ 19.0 19.1 McRae R, Esser M. Practical fracture treatment E-book. Churchill Livingstone/ Elsevier; 2002.
- ↑ 20.0 20.1 20.2 Fourati MK. Reeducation du genou après fracture de la rotule. Ann. Kinésitherapie 1986.
- ↑ Scolaro J, Bernstein J, Ahn J. In brief: patellar fractures. 2011;1213-1215.
- ↑ 22.0 22.1 American Academy of Orthopaedic Surgeons. Diseases and conditions - Patellar (Kneecap) Fractures. http://orthoinfo.aaos.org/topic.cfm?topic=A00523 (accessed November 10 2010).
- ↑ Shang ZG. Patellar fractures treatment and management. Unbound medline 2013;26(6):445-8.
- ↑ 24.0 24.1 24.2 Strauss J. ORIF Patella Fracture Post-Operative Rehabilitation Protocol, Hospital for Joint Diseases, 2008.