Low Level Laser Therapy
Introduction[edit | edit source]
The term Laser is the acronym for Light Amplification by Stimulated Emission of Radiation. A laser light is monochromatic, collimated, and coherent. A laser is a device that produces such a light. Low level laser therapy (LLLT) is used by some physiotherapists to treat various musculoskeletal condition. LLLT is a non-invasive light source treatment that generates a single wavelength of light. It emits no heat, sound, or vibration. It is also called photobiology or biostimulation. LLLT is believed to affect the function of connective tissue cells (fibroblasts), accelerate connective tissue repair and act as an anti-inflammatory agent. Lasers with different wavelengths, varying from 632 to 904 nm, are used in the treatment of musculoskeletal disorders.
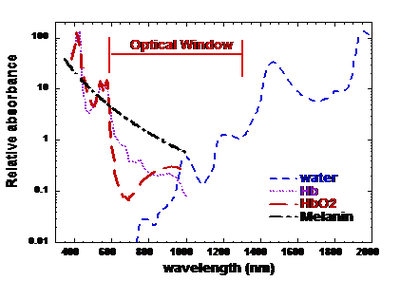
Wavelengths between 660 nm and 905 nm have the ability to penetrate skin, and soft/hard tissues. This light have a good effect on pain, inflammation and tissue repair. [1]
An output power of less than 0.5 Watts is classed as LLLT ( class III in the USA) whereas lasers with an output powers than 500 mW or 0.5 Watts are termed High Power Laser Therapy HPLT (Class IV lasers in the USA). HPLT creates heat on the surface of the skin due to their higher power density (irradiance). LLLT is often referred to as “Cold Lasers” since they do not create a heating sensation during treatment.[2]
Effects of LLLT[edit | edit source]
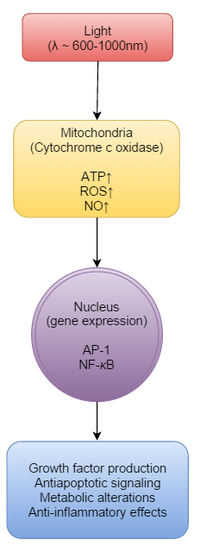
The effects of the LLLT which are significant for physiotherapy, and makes this tool useful to enhance other treatments as therapeutic exercise, are:
- Reduction of inflammation: It can occur within hours to days. [1]
- Pain relief
- Accelerated tissue regeneration: LLLT stimulates cell proliferation of fibroblasts [3], keratinocytes [4], endothelial cells [5] and lymphocytes. [6] [7]
Physiotherapy[edit | edit source]
In physiotherapy LLLT is use for pain relief, accelerated tissue regeneration and reduction of inflammation.
Conditions that are treated include
- Osteoarthritis of the knee, hip and ankle
- Rheumatoid arthritis
- TMD [8],
- Shoulder impingement syndromes
- Hip or shoulder bursitis
- Low back disc degeneration
- Disc herniation
- Sciatica
- neuropathic pain. [9]
- Tendonitis
- Tennis elbow
- Plantar fasciitis
- Reduction of volume and pain in lymphedema[10] [11]
Evidence[edit | edit source]
A 2017 systematic review and meta-analysis found that LLLT is an effective treatment modality to reduce pain in adult patients with musculoskeletal disorders. They also noted that adherence to the World Association of Laser Therapy (WALT) dosages improved effectiveness.[12]
A 2017 review titled "Effective treatment options for musculoskeletal pain in primary care: A systematic overview of current evidence" concluded that the evidence on effectiveness of laser therapy for shoulder pain or acute or chronic neck pain was inconclusive. With regards to knee pain low level laser therapy may confer added benefits to exercise and / or surgical treatment. [13]
Contraindications[edit | edit source]
Contraindication according to The North American Association for Laser Therapy are:
- Eyes: Do not aim laser beams into the eyes and everyone present should wear appropriate safety spectacles.
- Cancer: Do not treat over the site of any known primary carcinoma or secondary metastasis unless the patient is undergoing chemotherapy when LLLT can be used to reduce side effects such as mucositis. LLLT however can be considered in terminally- ill cancer patients for palliative relief.
- Pregnancy: Do not treat directly over the developing fetus.
- Epileptics: Be aware that low frequency pulsed visible light (<30Hz) might trigger a seizure in photosensitive, epileptic patients. The adverse effects of LLLT have been reported to be no different from those reported by patients exposed to placebo devices in trials.
(conference of The North American Association for Laser Therapy in 2010)
References[edit | edit source]
- ↑ 1.0 1.1 Cotler HB, Chow RT, Hamblin MR, Carroll J. The Use of Low Level Laser Therapy (LLLT) For Musculoskeletal Pain. MOJ Orthop Rheumatol 2015;2(5): 00068
- ↑ Rehab Management Treating Pain with Low vs High-Power Lasers: What is the Difference? Published on April 4, 2019 Available from: http://www.rehabpub.com/2019/04/treating-pain-low-vs-high-power-lasers-difference/ (last accessed 25.6.2019)
- ↑ Frigo L, Fávero GM, Lima HJ, Maria DA, Bjordal JM, et al. Low-level laser irradiation (InGaAlP-660 nm) increases fibroblast cell proliferation and reduces cell death in a dose-dependent manner. Photomed Laser Surg 2010;28 Suppl 1: S151-S156.
- ↑ Basso FG, Oliveira CF, Kurachi C, Hebling J, Costa CA. Biostimulatory effect of low-level laser therapy on keratinocytes in vitro. Lasers Med Sci 2013 28(2): 367-374.
- ↑ Szymanska J, Goralczyk K, Klawe JJ, Lukowicz M, Michalska M, et al. Phototherapy with low-level laser influences the proliferation of endothelial cells and vascular endothelial growth factor and transforming growth factor-beta secretion. J Physiol Pharmacol 2013;64(3): 387-391.
- ↑ Agaiby AD, Ghali LR, Wilson R, Dyson M. Laser modulation of angiogenic factor production by T-lymphocytes. Lasers Surg. Med 2000;26(4): 357-363.
- ↑ Moore P, Ridgway TD, Higbee RG, Howard EW, Lucroy MD. Effect of wavelength on low-intensity laser irradiation-stimulated cell proliferation in vitro. Lasers Surg Med 2005;36(1): 8-12.
- ↑ Cavalcanti MF, Silva UH, Leal-Junior EC, et.al.Comparative Study of the Physiotherapeutic and Drug Protocol and Low-Level Laser Irradiation in the Treatment of Pain Associated With Temporomandibular Dysfunction. Photomed Laser Surg. 2016 Nov 29. [Epub ahead of print]
- ↑ Chen YT, Wang HH, Wang TJ, Li YC, Chen TJ. Early application of low-level laser may reduce the incidence of postherpetic neuralgia (PHN). J Am Acad Dermatol. 2016;75(3):572-7.
- ↑ Smoot B, Chiavola-Larson L, Lee J, Manibusan H, Allen DD. Effect of low-level laser therapy on pain and swelling in women with breast cancer-related lymphedema: a systematic review and meta-analysis. J Cancer Surviv. 2015;9(2):287-304.
- ↑ Carati CJ, Anderson SN, Gannon BJ, Piller NB. Treatment of postmastectomy lymphedema with low-level laser therapy: A double blind, placebo-controlled trial. Cancer 2003;98(6): 1114-1122.
- ↑ Clijsen R, Brunner A, Barbero M, Clarys P, Taeymans J. Effects of low-level laser therapy on pain in patients with musculoskeletal disorders: a systematic review and meta-analysis. Available from: https://www.ncbi.nlm.nih.gov/pubmed/28145397/ (last accessed 25.6.2019)
- ↑ Babatunde OO, Jordan JL, Van der Windt DA, Hill JC, Foster NE, Protheroe J. Effective treatment options for musculoskeletal pain in primary care: A systematic overview of current evidence. PloS one. 2017 Jun 22;12(6):e0178621. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5480856/ (last accessed 24.6.2019)