Lymphoedema
Introduction[edit | edit source]
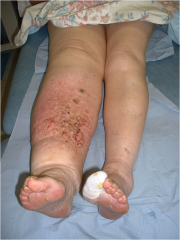
Lymp0hedema is a chronic disease marked by the increased collection of lymphatic fluid in the body, causing swelling, which can lead to skin and tissue changes. The chronic, progressive accumulation of protein-rich fluid within the interstitium (a contiguous fluid-filled space existing between a structural barrier, such as a cell wall or the skin, and internal structures, such as organs, including muscles and the circulatory system) and the fibro-adipose tissue exceeds the capacity of the lymphatic system to transport the fluid.
Swelling associated with lymphoedema can occur anywhere in the body, including the arms, legs, genitals, face, neck, chest wall, and oral cavity.
There are many psychological, physical, and social sequelae related to a diagnosis of lymphedema.
Lymphoedema is classified as either (genetic) primary lymphedema or (acquired) secondary lymphedema[1].
Signs and Symptoms[edit | edit source]
- Distal swelling in the extremities including the arms, hands, legs, feet
- Swelling proximally in the breast, chest, shoulder, pelvis, groin, genitals, face/intraoral tissues
- Restricted range of motion in the joints because of swelling and tissue changes
- Skin discoloration
- Pain and altered sensation
- Limb heaviness;
- Difficulty fitting into clothing[1].
Etiology[edit | edit source]
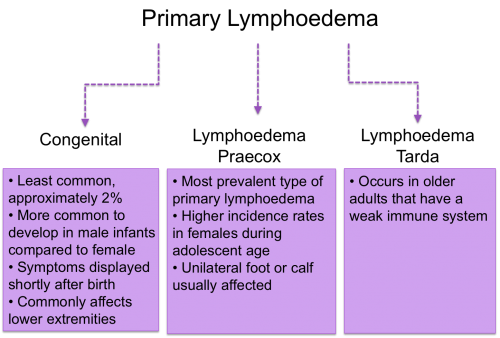
Primary lymphoedema is an inherited or congenital condition that causes a malformation of the lymphatics system, most often because of genetic mutation. Primary lymphedema: subdivided into 3 categories:
- Congenital lymphoedema, present at birth, or recognized within two years of birth;
- Lymphoedema praecox, occurring at puberty or the beginning of the third decade;
- Lymphoedema tarda, which begins after 35 years of age.
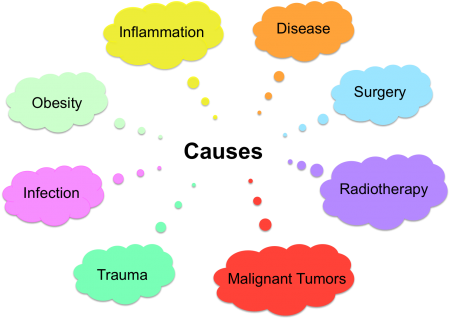
Secondary lymphoedema results from insult, injury, or obstruction to the lymphatic system.
- Most common cause of lymphedema worldwide is filariasis caused by infection by Wuchereria bancrofti.
- In developed countries, most secondary lymphedema cases are due to malignancy or related to the treatment of malignancy. This includes surgical excision of lymph nodes, local radiation treatment, or medical therapy.
- Breast cancer is the most common cancer associated with secondary lymphedema in developed countries[1].
Epidemiology[edit | edit source]
Primary lymphoedema is rare, affecting 1 in 100,000 individuals.
Secondary lymphoedema is the most common cause of the disease and affects approximately 1 in 1000 Americans[1].
The identification of the incidence and prevalence of lymphedema is complex.
- Lymphoedema is remarkably prevalent, but the population implications of lymphatic dysfunction are not well studied. Prevalence estimates for lymphedema are relatively high, yet its prevalence is likely underestimated.
The incidence of lymphoedema is most widely studied in the oncologic population.
- One in 5 women who survive breast cancer will develop lymphoedema.
- In head and neck cancer, lymphatic and soft tissue complications can develop throughout the first 18 months post-treatment, with greater than 90% of patients experiencing some form of internal, external, or combined lymphoedema. Over half of those patients developing fibrosis.
- In one recent study, 37% of women treated for gynecological cancer had measurable evidence of lymphoedema within 12 months post-treatment.
- In the gynecologic oncologic population, more extensive lymph node dissection, receipt of chemotherapy and radiation therapy, increasing body mass index, insufficient levels of physical activity, a diagnosis of vulvar/vaginal cancer, and presence of pre-treatment lymphedema were identified as potential risk factors to lymphoedema development[1].
- Cellulitis is a one of the leading causes in developing lymphoedema. episodes of cellulitis damage the lymphatic vessels and a lymphatic defect predisposes to cellulitis[2]
Pathophysiology[edit | edit source]
Primary lymphoedema[edit | edit source]
- Associated with dysplasia of the lymphatic system and can also develop with conditions of other vascular abnormalities, including Klippel-Trenaunay-Weber syndrome, Milroy Disease, Lymphoedema Distichiasis Syndrome and Turner syndrome.
- Primary lymphoedema is marked by hyperplasia, hypoplasia, or aplasia of the lymphatic vessels.
- Primary lymphoedema has 3 types :1- congenital (before age 2), 2- praecox (between age 2 and 25), 3- tarda (after age 35)[3][4].
Secondary lymphedema[edit | edit source]
- due to damage or dysfunction of the normally functioning lymphatic system.
- Although cancer treatments, including oncologic surgical procedures such as axillary lymph node dissection and excision in breast cancer and radiation treatment, are the most common cause of lymphoedema in the United States, filariasis is the most common cause of secondary lymphedema globally.
- Filariasis is the direct infestation of lymph nodes by the parasite, Wuchereria bancrofti. The spread of the parasite by mosquitos affects millions of people in the tropic and subtropic regions of Asia, Africa, Western Pacific, and Central and South America.
- Oncologic surgical procedures such as sentinel lymph node biopsy and radical dissection that require excision of regional lymph nodes or vessels can lead to the development of secondary lymphoedema.
- Other surgical procedures linked to secondary lymphoedema development include peripheral vascular surgery, burn scar excision, vein stripping, and lipectomy.
- other causes include :
- Recurrent tumors or malignancy that have metastasized to the lymph nodes
- Obstructive lesions within the lymphatic system
- Infected and/or traumatized lymphatic vessels
- Scar tissue obliterating the lumen of the lymphatic vessels.
- Edema from deep venous thrombosis (DVT) or nonobstructive causes of chronic venous insufficiency at the extremities may lead to secondary lymphedema.
Although there is no definitive cure for lymphedema, with proper diagnosis and management, its progression and potential complications can successfully be managed[1].
Characteristics/Clinical Presentation[edit | edit source]
There are both physical and psychological effects of the chronic condition [6] [7]. Early diagnosis is vital to ensure the correct treatment is chosen.
Physical Changes[edit | edit source]
- Swelling in an arm or a leg. It may be the entire limb or only parts . Most likely unilateral, but can be bilateral
- In the early stages pitting oedema occurs where the skin is pressed leaving an indent in the swelling. Elevating the arm creates a draining effect to reduce swelling
- Can be fibrosis, pitting edema
- Limbs can feel heavy and achy
- There is altered sensation, for example, pins and needles, burning
- Reduced mobility and range of movement of the affected limb/s
- Pain and joint discomfort
- Skin changes, for example redness and increased temperature
- Nail discoloration[8]
- Hyperkeratosis (thickening of the skin) and lymphangiectasia (dilated superficial lymph vessels)
- Reoccurring infections in the involved limb
- Hardening, thickening, or tightness of the skin[9][10]
- Loss of hair
- Loss of sleep[11]
- Symptoms can increase during warm weather, menstruation, and if the limb has been left in its depended position.[4]
- If primary and affecting the intestine signs and symptom include; abdominal bloating, diarrhea, and intolerance of fatty foods.[10]
Psychological effects (associated with the condition as a result of changes to body image).[edit | edit source]
- Swelling and weight gain impact physical appearance that can affect one’s perception of how they look, consequently decreasing their self-confidence [12][7]
- People commonly detach themselves from social events with family and friends leading to social isolation[13]
- Disturbed sleeping pattern
- Some people may feel they have a lack of support
- Financial concerns as a consequence of treatment cost and potential job loss/change[13]
- Some cancer survivors that have acquired secondary lymphoedema feel that it can be a constant reminder of previously having cancer[14]
- For those that experience unilateral lymphoedema, commonly different sizes of garments have to be worn on each side of the body and oversized clothes have to be worn because items such as tight jeans should be avoided.[14]. Psychologically this can largely impact the person because they may not feel comfortable with the way they look and therefore exclude themselves from public situations
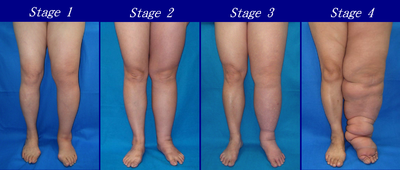
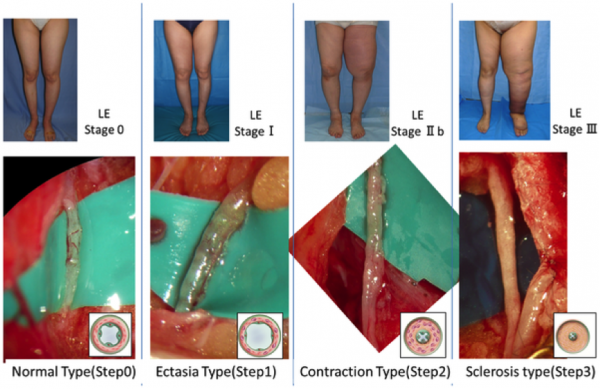
Stages of Lymphoedema[edit | edit source]
Lymphoedema Stages[1]
Stage 0 (Latency stage)[edit | edit source]
- The patient is considered “at-risk” for lymphoedema development due to injury to the lymphatic vessels but does not present with outward signs of edema.
- Includes patients with breast cancer who have undergone sentinel lymph node biopsy and or radiation but have not yet developed swelling.
- Lymphatic transport capacity has been reduced, which predisposes the patient to lymphatic overload and resultant edema.
Stage 1 (Spontaneous)[edit | edit source]
- Reversible
- Has pitting edema
- Swelling at this stage is soft, and may respond to elevation
Stage 2 (Spontaneously irreversible)[edit | edit source]
- Has tissue fibrosis/induration
- Swelling does not respond to elevation
- Skin and tissue thickening occurs as the limb volume increases
- Pitting may be present, but may be difficult to assess due to tissue and or skin fibrosis
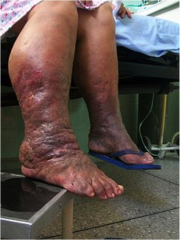
Stage 3 (Lymphostatic elephantiasis)[edit | edit source]
- Show the following:
- Pitting edema
- Fibrosis
- Skin changes
- During this stage papillomas may form, infections/cellulitis may occur, and the skin becomes dry
Evaluation[edit | edit source]
Lymphoedema is often confused with other causes of extremity edema and enlargement.[1]
- Understanding the risk factors and physical examination signs of lymphedema can accurately diagnose patients about 90% of the time.
- Correct diagnosis is imperative so patients can be managed appropriately.
- Diagnosis is suspected by evaluating the history and physical examination.
- Lymphoscintigraphy confirms the diagnosis.
- Imaging is unnecessary to make the diagnosis but can be used as confirmation, assessment of the extent of involvement, and help to determine therapeutic intervention.
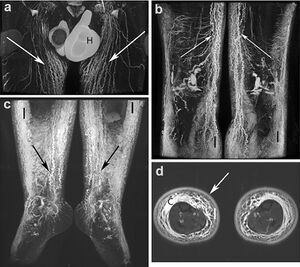
Newer technologies include 3-dimensional magnetic resonance imaging (MRI), computerized tomography (CT), ultrasound, and bioelectrical impedance analysis. Ultrasound is useful to exclude other etiologies like DVT, venous insufficiency and can also help in identifying tissue changes and masses that might be the cause of lymphatic compression. CT and MRI can investigate soft tissue edema with good sensitivity and specificity, but they are relatively expensive.[1]
Treatment/Management[edit | edit source]
- Lymphoedema is a progressive disease, and early diagnosis and treatment are paramount.
- Critical to diagnose and treat both mild and early onset cases to halt the progression of this lifelong and often debilitating condition.
- For patients to improve their knowledge base and learn helpful evidence-based management and coping strategies, patients must be referred to a specialist holding certification in lymphedema treatment and management eg. physician, an occupational therapist, or physical therapist.
Drug therapy:
- Adjunctive only for pain control or secondary infection
Surgery :
- Debulking is often ineffective
Microsurgical techniques:
- Vascularized Lymph Node Transfer (VLNT)
- Lymphaticovenous Anastomoses (LVA): VLNT and LVA are microsurgical procedures that can improve the patient's physiologic drainage of the lymphatic fluid and eliminate the need for compression garments in some patient. These procedures have better results when performed when a patient's lymphatic system has less damage.
- Suction-Assisted Protein Lipectomy (SAPL): Is more effective in later stages of lymphedema and allow removal of lymphatic solids and fatty deposits that are poor candidates for conservative lymphoedema therapy, or VLNT or LVA surgeries[1]
Prognosis[edit | edit source]
- A cure is rarely achieved once lymphedema occurs.
- Meticulous treatment and preventive measures can help lessen symptoms, slow or stop disease progression, and prevent complications.
- A systematic review and meta-analyses suggest the need for complete awareness of the factors contributing to the wide variability in lymphedema in order to improve QOL people living with cancer-related lymphoedema in low and middle-income countries[16].
- Patients with chronic lymphedema for ten years have a 10% risk of developing lymphangiosarcoma. This tumor is highly aggressive, requires radical amputation of the involved extremity, and has a very poor prognosis. Five-year survival is less than 10%[1].
Complications[edit | edit source]
Complications of lymphoedema also include[1]:
- Cellulitis: often recurrent
- Lymphangitis
- Superficial bacterial and fungal infections
- Lymphangio-adenitis
- Deep vein thrombosis (DVT)
- Severe functional impairment
- Psychosocial dysfunction
- Cosmetic embarrassment
- Amputation
- Complications following surgery are common and include:
- Partial wound separation
- Seroma
- Hematoma
- Skin necrosis
Physical Therapy Management[edit | edit source]
Education regarding the following points are paramount
- Self MLD
- Infection prevention
- Exercise
- Instruction in proper diet to decrease fluid retention and how to avoid injury and infection, anatomy
- Self bandaging and use of compression garments. Garment fitting.[10][17]
- Weight control
- Avoid venipuncture in the affected extremity
- Avoidance of other constricting items; do not take BP measurements on the affected extremity
- Life long education regarding eg. Rigid adherence to compression stockings is mandatory to obtain relief from the pain and swelling. In addition, skin dryness and pruritus also need to be addressed. All patients should be seen by a wound care nurse if there is tissue breakdown. At this point, the chances of healing are small, and daily wound dressings are necessary[1]
- Use limb as normally as possible
- Avoid any minor injuries such as scratches (may lead to infection- treat with antiseptic).
- Avoid injections on affected side
- Don’t take HOT BATHS (increases swelling), COLD BATHS are allowed.
- Don’t wear tight bands/ jewelry on affected side. [18]
Interventions include:[edit | edit source]
- Short/low stretch Compression garment wear following lymphatic drainage.
- Skin Hygiene and care (such as cleaning the skin of the arm or leg daily and moisten with lotion). Fastidious skin care is essential to prevent secondary skin infections
- Exercise: Light exercise promotes lymph drainage and protein absorption via muscle contraction. A systematic review found that progressive resistance exercise does not appear to increase the risk or severity of developing lymphoedema, and can facilitate volume reduction[19].
- Compression pumps: Helps with drainage but can increase the risk of infection
- Psychological and emotional support
- Decongestive lymphoedema therapy (DLT): Is the primary treatment for moderate-to-severe lymphedema and mobilizes lymph and dissipate fibrosclerotic tissue.
- Manual lymph drainage (MLD): Light lymph massage designed to increase lymph flow. MLD benefits remain inconclusive, in one study, MLD significantly reduced arm oedema volume, yet did not improve subjective symptoms or arm function[20]. Despite this, MLD is well tolerated and safe in combination with compression therapy and may benefit women with mild to moderate lymphoedema[21].
- Intermittent Pneumatic Compression Devices (IPCD): It can be used to reduce oedema volume in conjunction with DLT, particularly in patients with compromised mobility or physical exercise [22].
- see also The Role of the Physiotherapist in Palliative Care for People With Lymphoedema
Complex Decongestive Therapy: the primary treatment for moderate-to-severe lymphoedema and mobilizes lymph and dissipate fibrosclerotic tissue. One study showed a 53% mean reduction of lymphedema volume after 4 weeks of complex decongestive physiotherapy, consisting of manual lymph drainage, extremity elevation, multilayer compression bandage, remedial exercises and skin care[23].
- Phase 1:
- Skin care
- Light manual massage (manual lymph drainage)
- ROM
- Compression (multi-layered bandage wrapping, highest level tolerated 20-60 mm Hg)
- Phase 2:
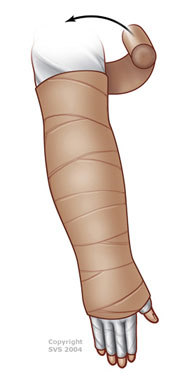

- Compression by low-stretch elastic stocking or sleeve
- Skin care
- Exercise
- Light massage as needed
Contraindications for compression includes arterial disease, painful postphlebitic syndrome, and occult visceral neoplasia.[17]
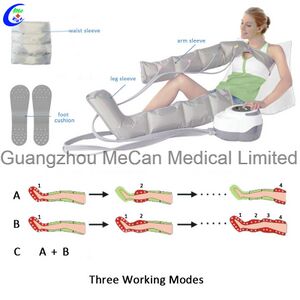
Pneumatic compression therapy (PCT):
- Machine- Consist of pneumatic pump & sleeves
- Pneumatic pump consists of: Pressure control (unit- mmHg/ kilopascal)- scale by deflection of needle or knob round scale, On/Off switch and Time control (ratio of inflation/deflation)
- Sleeves consisting of double layer of sealed polyurethane. Available for full upper limb (UL) (straight) or full lower limb(LL) (foot shaped at end) or below knee only with Zip/ velcro fastening
- Sleeves with more air entry holes give more even pressure.
- Pneumatic compression may be given either Intermittent – whole sleeve alternately inflate & deflate or Sequential – sections of sleeve inflate & deflate in turn giving compression to limb distal to proximal.
- Application: •Remove all clothing & jewelry •Limb should be well supported & elevated •If circulation is restricted by sleeve patient may feel pins & needles sensation. It should be avoided.
- Assessment prior to PCT: •Joint ROM •Muscle strength •Palpation of Edema •Check tissue mobility •Limb measurements for oedema - Check bilaterally Before treatment, just after treatment, 1 hour later & in evening
- Pressure are same for UL & LL:
- 1.Fixed – 30-40 sec inflation 15 sec deflation
- 2.Variable – inflation time can be increased up to 60 sec. Machine should provide same physiological condition as normal muscle contraction.
- Plan of treatment with PCT :
- •1st week – •Begin with 40mmHg for 30 min twice a day. •Assess immediately & 1 hour later. •Pressure is kept same & time is gradually increased until end of a week the dosage is 40 mmHg for 1 hour. •Treatment given 7 days/week
- •2nd week – •Increase pressure by 5 mmHg per day until 65 mmHg (max) •Time - 1 hour twice daily •If pain is complain use lower pressure & treat more frequently e.g. 45 mmHg 3 times/day Or 30 mmHg 4 times/day. Treatment can be given as in IPD /OPD by physiotherapist or at home.[18]
The 5 videos below are informative therapy viewing.
1. Complete Decongestive Therapy ( 109 seconds)
2. Manual Lymphatic Drainage 3 minutes 51 seconds
3. Self care - Lymphoedema (3 minutes 20 seconds)
4. A 9 minute video on monitoring limb measurements, objective assessments.
5. This 3 minute video is on bandaging techniques
Differential Diagnosis[edit | edit source]
- Lipedema
- Cellulitis
- Dermatologic Manifestations of Cardiac Disease
- Dermatologic Manifestations of Renal Disease
- Erysipelas
- Filariasis
- Lymphangioma
- Thrombophlebitis
- Venous Insufficiency[24]
Evidence[edit | edit source]
Courneya K, Mackey J, Bell G.Randomized Controlled Trial of Exercise Training in Postmenopausal Breast Cancer Survivors: Cardiopulmonary and Quality of Life Outcomes. Journal of Clinical Oncology, Vol 21, Issue 9 (May), 2003: 1660-1668. http://171.66.121.246/content/21/9/1660.full Accessed on 4/5/2011.
Badger C, Peacock J, Mortimer P. A Randomized, Controlled, Parallel-Group Clinical Trial Comparing Multilayer Bandaging Followed by Hosiery versus Hosiery Alone in the Treatment of Patients with Lymphedema of the Limb. Cancer 2000;88:2832–7.© 2000 American Cancer Society.https://www.cebp.nl/media/m1159.pdf Accessed on 4/5/2011.
McNeely M, Magee D, Lees A, Bagnall K. The Addition of Manual Lymph Drainage to Compression Therapy For Breast Cancer Related Lymphedema: a Randomized Controlled Trial. Volume 86, Number 2, 95-106. http://resources.metapress.com/pdf-preview.axd?code=pm25575l0765836l&size=largest Accessed on 4/5/2011.
Resources[edit | edit source]
National Cancer Institute http://www.cancer.gov/cancertopics/pdq/supportivecare/lymphedema/Patient/Page2#Section_69
Northwest Medical Center http://northwestmed.com/our-services/lymphedema-management.dot
http://www.vascularweb.org/vascularhealth/Pages/lymphedema.aspx
http://www.medicinenet.com/breast_cancer_and_lymphedema/louisville-ky_city.htm
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 Sleigh BC, Manna B. Lymphedema. InStatPearls [Internet] 2019 Dec 5. StatPearls Publishing.Available from:https://www.ncbi.nlm.nih.gov/books/NBK537239/ (last accessed 28.7.2020)
- ↑ Rodriguez JR, Hsieh F, Huang C-T, Tsai T-J, Chen C, Cheng M-H. Clinical features, microbiological epidemiology and recommendations for management of cellulitis in extremity lymphedema. J Surg Oncol [Internet]. 2020;121(1):25–36. Available from: http://dx.doi.org/10.1002/jso.25525
- ↑ 3.0 3.1 Antignani PL, Puppo F, Tomczak H, Cormier J, Andrade M, Boccardo F, et al. Diagnosis and treatment of primary lymphedema. Consensus document of the International Union of Phlebology (IUP) [Internet]. Cloudfront.net. [cited 2022 May 28].
- ↑ 4.0 4.1 The Merck Manuals: The Merck Manual for Healthcare Professionals. Lymphedema. http://www.merck.com/mmpe/sec07/ch081/ch081h.html#sec07-ch081-ch081h-1866. (accessed 5 April 2011)
- ↑ Oremus M, Dayes I, Walker K, Raina P. Systematic review: conservative treatments for secondary lymphedema. BMC Cancer [Internet]. 2012;12(1):6. Available from: http://dx.doi.org/10.1186/1471-2407-12-6
- ↑ Cancer Research UK. Symptoms of lymphoedema. http://www.cancerresearchuk.org/about-cancer/coping-with-cancer/coping-physically/lymphoedema/lymphoedema-symptoms (accessed 1 April 2014).
- ↑ 7.0 7.1 McCallin M, Johnston J, Bassett S. How effective are physiotherapy techniques to treat established secondary lymphoedema following surgery for cancer? A critical analysis of literature. NZ Journal of Physiotherapy 2005;33:101-112. (accessed May 28 2022).
- ↑ Lyons OTA, Modarai B. Lymphoedema. Surgery (Oxford). 2013;3:218-223. http://www.sciencedirect.com/science/article/pii/S0263931913000355 (accessed 12 January 2016).
- ↑ Mayo Clinic. Lymphedema. http://www.mayoclinic.com/health/lymphedema/DS00609/DSECTION=symptoms (accessed 5 April 2011)
- ↑ 10.0 10.1 10.2 Goodman C, Fuller K. Pathology: Implications for the Physical Therapist. 3rd ed. St. Louis, MO: Saunders Elsevier: 2009.
- ↑ National Cancer Institute: U.S National Institutes of Health. Lymphedema PDQ. http://www.cancer.gov/cancertopics/pdq/supportivecare/lymphedema/Patient/page1. (acceessed 5 April 2011)
- ↑ Harmer V. Breast cancer-related lymphoedema: risk factors and treatment. Br J Community Nurs. 2009;18:166-172. (accessed 10 October 2015).
- ↑ 13.0 13.1 Ridner SH. The Psycho-Social impact of Lymphedema. Lymphat Res Biol 2009;7:109-112. http://www.ncbi.nlm.nih.gov/pubmed/19534633 (accessed 12 January 2016).
- ↑ 14.0 14.1 Greene AK. Epidemiology and morbidity of lymphedema. In: Lymphedema. Cham: Springer International Publishing; 2015. p. 33–44.
- ↑ Overview of magnetic resonance lymphography for imaging lymphoedema https://parjournal.net/article/view/4173
- ↑ Torgbenu E, Luckett T, Buhagiar MA, Chang S, Phillips JL. Prevalence and incidence of cancer related lymphedema in low and middle-income countries: A systematic review and meta-analysis.
- ↑ 17.0 17.1 Piller N, Carati C. The diagnosis and treatment of peripheral lymphedema. Lymphology [Internet]. 2009 [cited 2022 May 28];42(3):146–7. Available from: https://journals.uair.arizona.edu/index.php/lymph/article/viewFile/17084/16876
- ↑ 18.0 18.1 Thomson, A., Skinner, A., & Piercy, J. (1994). Tidy's physiotherapy. Oxford: Butterworth Heinemann. 12th ed.
- ↑ Olsson Möller U, Beck I, Rydén L, Malmström M. A comprehensive approach to rehabilitation interventions following breast cancer treatment - a systematic review of systematic reviews. BMC Cancer. 2019 May 20;19(1):472. doi: 10.1186/s12885-019-5648-7. PMID: 31109309; PMCID: PMC6528312.
- ↑ Shao Y, Zhong DS. Manual lymphatic drainage for breast cancer-related lymphoedema. Eur J Cancer Care (Engl). 2017 Sep;26(5). doi: 10.1111/ecc.12517. Epub 2016 May 11. PMID: 27167238.
- ↑ Ezzo J, Manheimer E, McNeely ML, Howell DM, Weiss R, Johansson KI, Bao T, Bily L, Tuppo CM, Williams AF, Karadibak D. Manual lymphatic drainage for lymphedema following breast cancer treatment. Cochrane Database Syst Rev. 2015 May 21;(5):CD003475. doi: 10.1002/14651858.CD003475.pub2. PMID: 25994425; PMCID: PMC4966288.
- ↑ Tran K, Argáez C. Intermittent Pneumatic Compression Devices for the Management of Lymphedema: A Review of Clinical Effectiveness and Guidelines [Internet]. Ottawa (ON): Canadian Agency for Drugs and Technologies in Health; 2017 May 12. PMID: 29553689.
- ↑ Dіdem K, Ufuk YS, Serdar S, Zümre A. The comparison of two different physiotherapy methods in treatment of lymphedema after breast surgery. Breast cancer research and treatment. 2005 Sep;93:49-54.
- ↑ Medscape reference. Dermatological Manifestations of Lymphedema Differential Diagnosis. http://emedicine.medscape.com/article/1087313-differential. (accessed 5 April 2011)