Cellulitis
Original Editors - Students from Bellarmine University's Pathophysiology of Complex Patient Problems project.
Top Contributors - Kacie McClendon, Elaine Lonnemann, Erica Shelley, Kim Jackson, Lucinda hampton, Fasuba Ayobami, 127.0.0.1, Evan Thomas, WikiSysop, Karen Wilson, Vidya Acharya and Claire Knott
Introduction[edit | edit source]
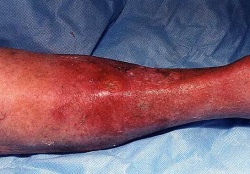
Cellulitis is a common infection of the dermis and subcutaneous tissues. Cellulitis typically presents with pain, erythema, oedema, and warmth. Cellulitis is not transmitted by person-to-person contact as the epidermis is not involved.[1] If correctly identified and treated promptly with appropriate antibiotic treatment is usually resolves.[2]
Etiology[edit | edit source]
The skin is a protective barrier that stops normal skin flora and other microbial pathogens reaching the subcutaneous tissue and lymphatic system. If a skin breakage occurs normal skin flora and other bacteria can enter the dermis and subcutaneous tissue, leading potentially to an acute infection affecting the deep dermis and subcutaneous tissue. Cellulitis most commonly results from infection with group A beta-hemolytic streptococcus (i.e., Streptococcus pyogenes).[2]
Risk factors for cellulitis include: skin injuries; surgical incisions; intravenous site punctures; fissures between toes; insect and animal bites; other skin infections; patients with comorbidities such as diabetes mellitus, venous insufficiency, peripheral arterial disease, and lymphedema.[2]
Epidemiology[edit | edit source]
Cellulitis is relatively common, occurring often in middle-aged and older adults. Men and women, have a similar incidence of cellulitis. There are approximately 50 cases per 1000 patient-years[2]
Pathophysiology[edit | edit source]
Cellulitis takes place after the skin is disrupted and microorganisms invade the subcutaneous tissues. Most commonly the infective agent is beta-haemolytic streptococci (most often) or staphylococcus aureus (including methycillin-resistant). [1]
Clinical Presentation[edit | edit source]
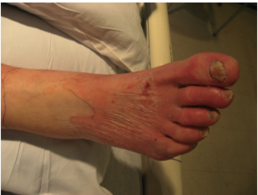
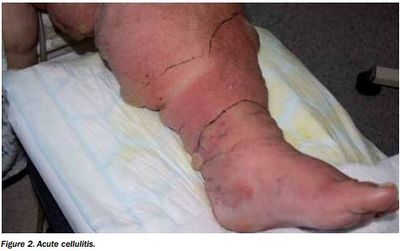
Typical symptoms of cellulitis include acute poorly demarcated and spreading erythema along with pain, swelling, and warmth. Commonly affects a lower limb but can occur on any area of skin or underlying subcutaneous tissue.[4][5] Regional lymphadenopathy and lymphangitis may be present alongside systemic features such as fevers and rigors.[1]
Examination[edit | edit source]
Patients with cellulitis will reveal an affected skin area typically with a poorly demarcated area of erythema. The erythematous area is often warm to the touch with associated swelling and tenderness to palpation. The patient may present with constitutional symptoms of generalized malaise, fatigue, and fevers.
- Ask for a complete history of the presenting illness, focusing on the context in which the patient noticed the skin changes or how the cellulitis began to occur.
- It is essential to ask patients if they: recently traveled, experienced any trauma or injuries, have a history of intravenous drug use, and/or have had insect or animal bites to the affected area.
- A complete and thorough past medical history should additionally be conducted to evaluate for possible chronic medical conditions that predispose patients to cellulitis, such as diabetes mellitus, venous stasis, peripheral vascular disease, chronic tinea pedis, and lymphedema. Diabetes Mellitus is one of most common comorbidities among those hospitalized for acute bacterial infections including cellulitis. Following a cellulitis infection, those with diabetes require a longer course of antibiotic therapy and are more likely to have an outpatient follow-up visit.[6].[7]
- Inspected area to look for any area of skin breakdown. The area should be demarcated with a marker to monitor for continuous spread. The area should be palpated to feel for fluctuance that could indicate the formation of a possible abscess.
- Gently palpate the affected area, be sure to note any presence of warmth, tenderness, or purulent drainage.
- Cellulitis can present on any area of the body, but most often affects the lower extremities. It is rarely bilateral.
- In lower extremity cellulitis, careful examination between interspaces of the toes should take place.
- Check for proper sensation and verify pulses are intact to monitor closely for compartment syndrome.
- Note if there are developing vesicles, bullae, or the presence of peau d'orange and lymphadenopathy.[8]
Diagnosis[edit | edit source]
Cultures is most commonly diagnosed by history and physical examination alone. Two of the four criteria (warmth, erythema, edema, or tenderness) are needed for diagnosis.[2]
Medical Management[edit | edit source]
Patients presenting with mild cellulitis and no systemic signs of infection require antibiotics. The duration of oral antibiotic therapy should be for a minimum duration of 5 days.
- Hospitalization for systemic antibiotics may be requires for patients with systemic signs of infection, have failed outpatient treatment, are immunocompromised, exhibit worsening erythema, are unable to tolerate oral medications, or have cellulitis overlying or near an indwelling medical device.[2]
- It is beyond a physiotherapists scope to know the individual antibiotics and best choices. The pharmacist ideally will have a board specialty in infectious disease to assist and work with the clinician on the best antibiotic selection.[8]
Physical Therapy Management[edit | edit source]
While there is lack of evidence that discusses specific physical therapy interventions for cellulitis, therapists should be aware of the signs and symptoms in order to refer the patient appropriately. Physical therapists should have awareness of risk factors and various causes of cellulitis, in addition to signs and symptoms.
Modalities that physical therapists can use for a patient with cellulitis include
- Rest and elevation of the affected limb is important and can help alleviate pain.
- The application of cool, wet, sterile bandages is also recommended for pain relief, and ice can be used as well.
Preventative Measures: Compression stockings; Exercise promotion and specific exercises eg calf pumps whilst standing in lines etc.[9]; Educate patient re the importance of maintaining good hand hygiene and adequately clean any future abrasions in their skin.[8]
Differential Diagnosis[edit | edit source]
Many and include:
- Necrotising soft tissue infections
- Deep vein thrombosis
- Myriad of non-infective erythematous rashes
- Dermatitis
- Thermal injury[1]
Complications[edit | edit source]
Without prompt diagnosis and treatment, cellulitis could lead to several complications. Cellulitis that leads to bacteremia, endocarditis, or osteomyelitis will require a longer duration of antibiotics and possibly surgery.[8] Cellulitis can spread systemically through the lymphatics and blood stream, which can lead to further complications.[10] If cellulitis does spread systemically through one of these systems, it can cause flu-like symptoms such as fever, rigors, nausea, and vomiting.[11][7] Though rare, there is a risk for severe sepsis, gangrene, or necrotizing fasciitis if cellulitis spreads systemically and is left untreated.[11]
Prognosis[edit | edit source]
Overall, cellulitis has a good prognosis
- If promptly diagnosed cellulitis with correct antibiotic treatment, patients can expect to notice an improvement in signs and symptoms within 48 hours.
- Annual recurrence of cellulitis occurs in about 8 to 20% of patients, with overall reoccurrence rates reaching as high as 49%
- Recurrence is preventable with prompt treatment of cuts or abrasions, proper hand hygiene, as well as effectively treating any underlying comorbidities.
- There is approximately an 18% failure rate with initial antibiotic treatment. [8]
Resources[edit | edit source]
A video link by dermatologist Dr. Noah Craft MD, PhD, DTMH discusses Cellulitis from the provider point of view and includes case studies, differential diagnosis, and treatment approaches.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 Radiopedia Cellulitis Available:https://radiopaedia.org/articles/cellulitis (accessed 29.1.2023)
- ↑ 2.0 2.1 2.2 2.3 2.4 2.5 Brown BD, Watson KL. Cellulitis. InStatPearls [Internet] 2022 Aug 8. StatPearls Publishing.Available:https://www.ncbi.nlm.nih.gov/books/NBK549770/ (accessed 29.1.2023)
- ↑ Bailey E, Kroshinsky D. Cellulitis: Diagnosis and Management. Dermatologic Therapy. 2011;24:229–39.http://onlinelibrary.wiley.com/doi/10.1111/j.1529-8019.2011.01398.x/full (accessed 15 Mar 2017).
- ↑ Tsai C-YL, Calvin MK, Chung C, Susan Shin-Jung L, Yao-Shen C, Hung C. Development of a prediction model for bacteremia in hospitalized adults with cellulitis to aid in the efficient use of blood cultures: a retrospective cohort study. BMC Infectious Diseases. 2016;16(1):581.
- ↑ Raff AB, Kroshinsky D. Cellulitis: A Review. JAMA. 2016;316(3):325-37. http://jamanetwork.com/pdfaccess.ashx?url=/data/journals/jama/935437/ (accessed 27 Feb 2017).
- ↑ Jenkins TC. Comparison of the Microbiology and Antibiotic Treatment among Diabetic and Non-Diabetic Patients Hospitalized for Cellulitis or Cutaneous Abscess. J Hosp Med. 9ADADDec12;:788–94.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4256165/ (accessed 28 Feb 2017).
- ↑ 7.0 7.1 Riches K, Keeley V. Cellulitis in patients with chronic oedema. Nursing & Residential Care [serial on the Internet]. (2012, Mar), [cited March 31, 2017]; 14(3): 122-127. Available from: CINAHL with Full Text.
- ↑ 8.0 8.1 8.2 8.3 8.4 Brown BD, Watson KL. Cellulitis. InStatPearls [Internet] 2019 Nov 6. StatPearls Publishing. Available from:https://www.ncbi.nlm.nih.gov/books/NBK549770/ (last accessed 12.2.2020)
- ↑ University of Maryland Medical Center. http://umm.edu/health/medical/altmed/condition/cellulitis (accessed 25 March 2017).
- ↑ Medscape. Cellulitis. http://emedicine.medscape.com/article/214222-overview (accessed 27 Feb 2017).
- ↑ 11.0 11.1 Kilburn SA, Featherstone P, Higgins B, Brindle R. Interventions for cellulitis and erysipelas. (Cochrane review). Cochrane Database Syst Rev. 2010(6):CD004299.