Obturator Nerve
Original Editor - Jin Yoo
Top Contributors - Jin Yoo, Lucinda hampton, Leana Louw, Mariam Hashem and Kim Jackson
Introduction[edit | edit source]
The obturator nerve arises from the lumbar plexus and provides sensory and motor innervation to the thigh. The obturator nerve :
- Provides motor innervation to the medial compartment of the thigh
- Is essential to the adduction of the thigh.
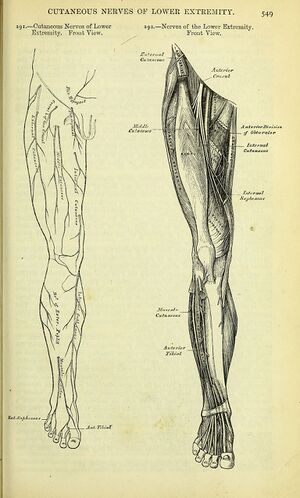
- Provides sensory innervation to the medial upper thigh and provides articular branches to the hip and knee.
- The obturator nerve can become entrapped at the exit of the obturator canal or more distally by fascia, causing exercise-induced medial thigh pain, typically in athletes[1].
Anatomy[edit | edit source]
The obturator nerve arises from the lumbar plexus on the posterior abdominal wall. Root L2-L4
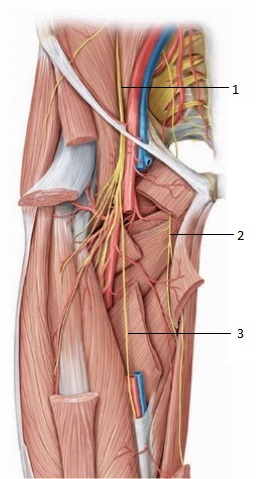
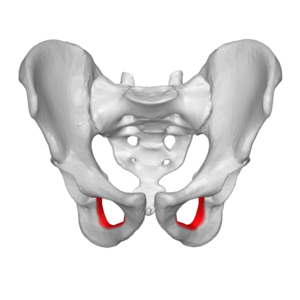
Pelvis: The nerve descends medial to psoas major to the obturator canal where it divides into anterior and posterior divisions. The anterior division exits from the obturator canal to enter the medial compartment of the thigh. The posterior division exits through obturator externus[2].
Medial compartment of thigh: Here the nerve divides into the anterior and posterior branch which are separated by the adductor brevis muscle.
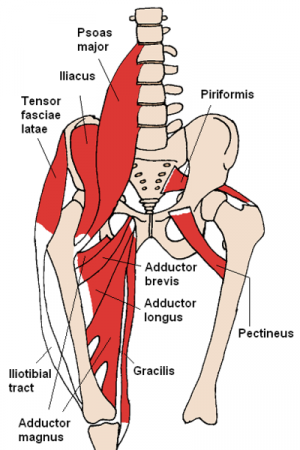
- The posterior branch travels underneath the adductor muscle along the anterior surface of the adductor magnus muscle, innervating the obturator externus, adductor brevis, as well as part of the adductor magnus muscle that is attached to the linea aspera.
- On the anterior surface of the adductor brevis muscle the anterior branch travels underneath the pectineus and adductor longus muscles to innervate the adductor longus, gracilis, and adductor brevis muscles. This branch also often contribute to the pectineus muscle. The cutaneous branches innervate the skin on the medial thigh[3].
Function[edit | edit source]
The Anterior branch provides
- Motor innervation to the adductor brevis, adductor longus, gracilis, and in rare circumstances, the pectineus.
- In terms of cutaneous innervation, the anterior branch of the obturator nerve supplies the medial thigh, and just above the medial knee
The posterior branch of the obturator nerve
- Provides innervation to the adductor magnus, adductor brevis, and occasionally the adductor longus and obturator externus.
- Furthermore, the obturator nerve provides articular branches to the hip and knee joints[1].
Viewing[edit | edit source]
An under 5 minute video on the anatomy of the Obturator nerve
Physiotherapy[edit | edit source]
Injury to the nerve is rare as it lies deep within the pelvis and medial thigh. It can be damaged through direct injury to the nerve or to surrounding muscle tissue. Mild damage to the obturator nerve can be treated with physiotherapy. More severe cases may require surgery[4].
Injury may be caused by:
- Nerve being stretched during surgery
- The nerve can become entrapped at the exit of the obturator canal or more distally by fascia. Entrapment of the obturator nerve causes exercise-induced medial thigh pain, typically in athletes. Athletes may present with pain that may be brought on by exercise, often sports involving a lot or running and twisting.[5]Hip abduction and extension aggravate the pain, and resisted adduction does not elicit pain. Conservative treatment includes stretching and strengthening exercises, cognitive behavioral education, neural gliding, and manual therapy. Neurolysis or neurectomy may merit consideration if symptoms are refractory to treatment[1]
- Compression during pregnancy
- Car or household accident
- Abdominal surgery[6]
Obturator Neuropathy[edit | edit source]
Symptoms
- Pain & paresthesias may extend from hip to knee along the medial aspect of the thigh
- Extension or lateral leg movement can increase pain
- May have trouble walking or experience leg weakness due to problems adducting the ipsilateral hip
Signs
- Weak hip adductors on affected side
- Wasting of medial thigh
- Abnormal abduction of hip during ambulation resulting in a circumduction, wide-based gait
- Area of sensory loss or alteration in the mid and lower third of the medial thigh which sometimes may extend below the knee
- Ipsilateral loss of the hip adductor tendon reflex (test against asymptomatic leg as is not always present in healthy population)
Assessment[edit | edit source]
- Needle EMG to confirm acute/chronic denervation of hip adductors excluding other lower extremity muscles such as iliopsoas or quadriceps
- CT, MRI, or ultrasound imaging when intra-pelvic mass lesions are suspected of entrapping the nerve[4]
Treatment[edit | edit source]
| Tipton JS, 2008[7] |
|
| Sorenson EJ. Chen JJ. Daube JR. 2002[8] |
|
| Bradshaw C. McCrory P. Bell S. Brukner P. 1997[9] |
|
Techniques[edit | edit source]
- Copenhagen Adductor Exercise
A simple adductor strengthening exercise (Copenhagen Adductor Exercise ) with three progression levels, three times per week during the preseason (6-8 weeks), and once per week during the competitive season (28 weeks). For elaboration see Groin Strain
2. This 6 minute video is on Obturator Nerve Flossing
References[edit | edit source]
- ↑ 1.0 1.1 1.2 Koh M, Markovich B. Anatomy, abdomen and pelvis, obturator nerve. StatPearls [Internet]. 2021 Jul 26.Available: https://www.statpearls.com/articlelibrary/viewarticle/26089/(accessed 18.1.2022)
- ↑ Radiopedia Obturator nerve Available:https://radiopaedia.org/articles/obturator-nerve-1 (accessed 18.1.2022)
- ↑ Drake RL, Vogl AW, Mitchell AWN. Gray's Anatomy for Students. 3rd Edition. Philadelphia: Churchill Livingstone/Elsevier. 2015.
- ↑ 4.0 4.1 Busis NA. Femoral and obturator neuropathies. Neurologic Clinics 1999;17:633-53.
- ↑ Tipton JS. Obturator neuropathy. Current reviews in musculoskeletal medicine 2008;1(3-4):234-7.
- ↑ Healthline. Obturator nerve. Available from: https://www.healthline.com/human-body-maps/obturator-nerve#1 (accessed 19/03/2019).
- ↑ Tipton JS. Obturator neuropathy. Current Reviews in Musculoskeletal Medicine 2008;1:234-7.
- ↑ Sorenson EJ. Chen JJ. Daube JR. Obturator neuropathy: causes and outcome. Muscle & Nerve 2002;25:605-7.
- ↑ Bradshaw C. McCrory P. Bell S. Brukner P. Obturator neuropathy: a cause of chronic groin pain in athletes. American Journal of Sports Medicine 1997;25:402-8.
- ↑ Brian Ableson. Flossing the Obturator Nerve - Amazing Results. Available from:https://www.youtube.com/watch?v=VEbVmzcIiv8 (accessed 22/02/2019).