Physical Activity and Injury Prevention in Adolescents
Top Contributors - Charmene Chaudhry, Zoe Rounding, Chelsea Mclene, Kim Jackson, Ewa Jaraczewska, Simisola Ajeyalemi, Kirsten Dippie, Wanda van Niekerk, 127.0.0.1, Rachael Lowe, Michelle Lee, Fergal O'Reilly, Katie Laverty, Leah Boudreau and WikiSysop
Introduction[edit | edit source]
The regular health benefits of participation in physical activity are well studied[1]; however, physical inactivity remains one of the largest worldwide threats to health and is the leading preventable cause of morbidity and mortality[2]. The worldwide prevalence of obesity nearly tripled between 1975 and [3]. In 2016, over 340 million children and adolescents aged 5-19 were overweight or obese[3]. More than 80% of the world's adolescent population is insufficiently physically active[4]. Physiotherapists are faced with an ever-growing challenge in efforts to promote physical activity in order for people to live healthy lives.
Physical activity has its own risks such as injuries and accidents to participants. Children and adolescents are the largest participants in physical activity and they are at particular risk of these injuries because of a high level of exposure, improper technique, poor proprioception, muscle weaknesses, apparatuses not adjusted to their size, absence of fear and understanding of risks[1][5]. Physical activity is the leading cause of injury and hospital room visits in adolescents[6]. Most injuries or accidents resulting from physical activity are non-life-threatening however they often result in pain, disability, school absence, absence from physical activity, and sometimes in dysfunction in the short and long-term[1]. Injuries to joints can accelerate the development of osteoarthritis and therefore prevention of physical activity-related injuries is essential. Emery showed in a review that injury prevention strategies in children could reduce the risk of physical activity-related injuries[7].
Physical Activity and Health[edit | edit source]
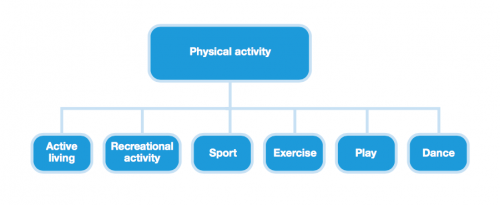
The World Health Organisation (WHO) defines physical activity as 'any bodily movement produced by skeletal muscles that requires energy expenditure'[4]. This broad definition entails that there are various ways in order to be physically active such as play, sport, walking, cycling, housework and gardening.
Regular physical activity is known to have many health benefits including:
- Reduced risk of cardiovascular disease
- Reduced risk of type II diabetes
- Reduced risk of certain types of cancers
- Improved cardiorespiratory and muscular fitness
- Reduced blood pressure
- Improved mental health and well-being
- Improved social and moral development
- Improved ability of academic achievements - e.g. ability to concentrate and better classroom discipline
- A contribution to healthy weight maintenance[4].
The WHO recommends for children and adolescents to accumulate at least 60 minutes of moderate to vigorous-intensity physical activity daily, which should include strengthening activities 3 times per week[4]. All children and young people should minimize the amount of time being sedentary for extended periods of time.
Role of the Physiotherapist[edit | edit source]
The Chartered Society of Physiotherapy (CSP) defines physiotherapy as a ' healthcare profession that works with people to identify and maximize their ability to move and function'[8]. Physiotherapy helps people of all ages to prevent, manage and rehabilitate injury, illness or disability. This could be through education, advice, exercise and manual therapy. It is important to possess the skills required for working within these in-demand services. The National Health Service (NHS) Knowledge and Skills Framework focuses on six core dimensions:
- Communication
- Personal and people development
- Health, safety and security
- Service improvement
- Quality
- Equality and diversity[9].
The CSP emphasizes the need for physiotherapists to encompass these core dimensions in their work[10], and they can be applied to the expanding role of physiotherapists in the prevention of injury and accidents. A physiotherapist must be open to personal and people development, take into account health safety and security while developing new methods of open communication to implement ways of improving safety, be critical when evaluating their services for quality and improvement purposes, and be sensitive to issues of equality and diversity.
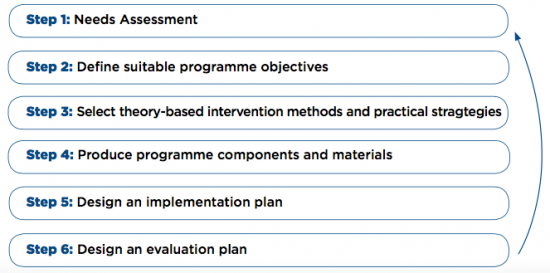
A physiotherapist can develop an injury prevention programme through the use of intervention mapping (IM) protocol. This involves a systematic process that prescribes a series of six steps in order to develop theories and evidence-based health promotion programmes[1]. This six-step process can aid physiotherapists in the development of various prevention programmes such as the prevention of injury and accidents in adolescents as a result of physical activity.
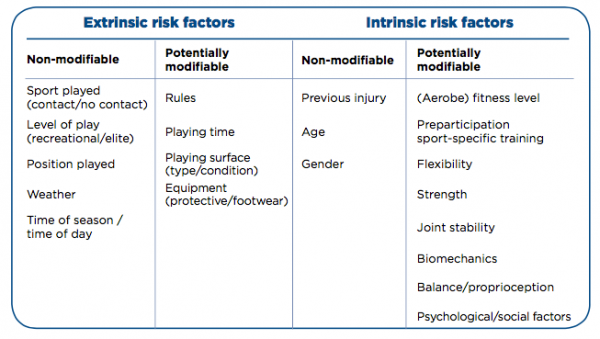
Risk factors are generally the leading guide for preventative measures in physical activity[1]. These risk factors can increase the risk of an injury or accident as a result of physical activity in adolescents and can include both extrinsic and intrinsic factors. Injuries and accidents can also be caused by a combination of these factors. It is important for physiotherapists to identify these risk factors in order to aid in prevention.
Demands on Health Care Services[edit | edit source]
The Health benefits of physical activity are extremely important however physical activity also exposes the participant to a risk of injury or accident. Physical activity such as sport and recreation, cycling, skateboarding and playground use is the most common reason for Australian youths aged 0-16 to be in an emergency department and 14% of these presenting injuries require hospitalization[11]. Similar results have been found worldwide in countries such as Norway, France, New Zealand and the United States[1].
Not only do injuries and accidents related to physical activity affect healthcare services, but they also affect school and work time. A study conducted in the Netherlands showed that school absence occurs in 7% of children and adolescents who sustained a sports injury, and the mean duration of school missed by these children was 8 days[1]. This means that 0.02% of the total population who attend school and participate in physical activity are absent from school one or more days. With a mean duration of 8 days, the total absence due to sports injuries can be calculated at 794,000 days a year. In addition, 22% of people who sustained an injury were also absent from physical activities. The economic consequences of physical activity-related injuries in adolescents are not known, but direct medical costs were estimated to be approximately £145 million and indirect costs (such as school or work absence) were estimated at approximately £360 million[1].
These preventable injuries increase the wait time for people to see a physiotherapist. In the National Health Service (NHS) the average wait time to see a physiotherapist in a musculoskeletal outpatient department is approximately six to eight weeks. Therefore if a plan is put in place to prevent these injuries, fewer persons would require rehabilitation from a physiotherapist. Overall, safety can be improved in many of these activities so that participants are able to continue to enjoy them without their health being compromised.
Current Legislation[edit | edit source]
Sport-Specific Laws[edit | edit source]
All sports have their own legislation when it comes to protective equipment, but there are no specific laws for types of physical activity.
Here is a list of a selection of popular sports and activities with links to their laws which include those on protective equipment:
- Football
- Rugby Union
- Rugby League
- Horse-riding
- Hockey
- Ice Hockey
- Boxing: Technical rules, Open boxing competition rules, World series competition rules.
There is more of a debate around cycling and boxing regarding helmet use so these are discussed in a little more detail.
Cycling[edit | edit source]
Cycling, classified as both, a sport and type of physical activity, is increasing in popularity in the UK as a means of exercise but also of transport. 40% of paediatric hospitalizations and deaths are due to head injury following a bicycle-related trauma[12]. Despite this, it is currently not required by law to wear a helmet in the majority of the UK[13], although there have been many calls by different bodies to make helmet wearing compulsory. It is however stated in the Highway Code (Rule 59) that cyclists should wear a helmet that conforms to the current regulations, is the correct size and is securely fastened.
The arguments of cycling advocates against having a mandatory cycle helmet law as there will be a dramatic decline in the number of people cycling. Consequently, this will lead to an increase in premature deaths and have a greater impact on the populations’ health than the risks of head injuries from not wearing a helmet. Cycling UK reports that 7-8% of head injuries in children admitted to English hospitals are due to cycling, with a small number of these being to areas of the head that a helmet may protect[14].
It has been highlighted by Macpherson and Spinks[15] that the following are the reasons people choose not use helmets and therefore could cause the supposed decline in the number of people cycling if a law was put into place:
- The cost of purchasing one
- The discomfort of wearing one
- The lack of the belief that is necessary
- The unpopular image of helmets, e.g. children not looking ‘cool’ in front of their friends.
In 1999 the British Medical Association (BMA) believed in the potential drop in the number of cyclists and recommended there be no law on bicycle helmets but still recommended the use of helmets. In 2004 the BMA changed their position and became in favour of mandatory cycle helmets. This change in stance came about because of their beliefs in the protective effects of cycle helmets in reducing the number and severity of head injuries.
Whilst it is not a legal requirement in the majority of the UK to wear a helmet, Jersey has made it compulsory for children under 13 to wear cycle helmets. You can read about that here. More than 20 countries around the world have made the wearing of cycle helmets compulsory including Finland, Sweden, Australia and some US states and Canadian provinces[12][13].
A study in Canada[16] focused on cycling-related injuries of children admitted to hospital during 1994 and 1998. The rate of head injuries suffered by children when cycling had a significantly greater decline in provinces where legislation regarding a compulsory cycle helmet was adopted when compared to provinces where such legislation was not adopted. This trend was also found in New South Wales, Australia by Walter et al.[17] where there was a large reduction in the rate of head injuries among cyclists following the implementation of legislation. Macpherson et al.[18] discovered there was also a decline in the rate of other types of injuries however this finding was not statistically significant. Macpherson and Spinks found the risk of a cyclist suffering a head or facial injury was reduced by 88% and 65% respectively if they were wearing a helmet[12]. A systematic review looking into injuries and the use of helmets found there to be reductions in the risk of suffering head injuries (51%), serious head injuries (69%), fatal head injuries (65%) and facial injuries (33%)[19].
The introduction of mandatory cycle helmets in Ontario in 1995 does not appear to have an impact on the cycling participation of children in the East York area of Ontario. Changes were noticed in the pattern of cycling but these were related to the location of where children were cycling and factors including weather. This study shows that introducing legislation that makes cycle helmets mandatory does not have a negative impact on the number of children cycling.[20]
In a Cochrane Review, Macpherson and Spinks highlighted that there was not enough evidence to prove or disprove the argument that introducing cycle helmet legislation causes a decline in the cycling population[12]. They did, however, find that the introduction of legislation increased helmet use and reduced the number of head injuries related to bicycle use. Physiotherapists, alongside the BMA, have a role in educating the population that while helmets are not mandatory, they do have protective effects against head and facial injuries. While there is currently no law advocating the compulsory use of helmets, physiotherapists can address the reasons people choose to not wear them; this could be undertaken during one-on-one time with patients and combating these barriers with patients could lead to an increase in those using helmets. With the age group, we are focusing on it could prove beneficial to encourage the use of helmets from an early age so it becomes a habit for them throughout their life.
Boxing[edit | edit source]
Types of Preventative and Protective Equipment[edit | edit source]
Injuries are a common factor among sports people and physical activity which means protective/preventative equipment may be necessary to reduce the risk of injury. The diverse and vast nature of today’s sporting activities has led to the development of various protective equipment for each sport depending on the risk of injury associated with it.
Adolescents aged 12-18 experience a higher risk of accident or injury associated with taking part in sport as their brains and bodies are still developing. There is more concern for safety in physically active adolescents who are often involved in more than one sport and maybe on teams with multiple age groups. This means they can be quite involved in vigorous regular physical activity, which increases the need for them to wear protective equipment at all times to be adequately protected from serious harm[23].
Common Types of Sports Equipment Used in the United Kingdom[edit | edit source]
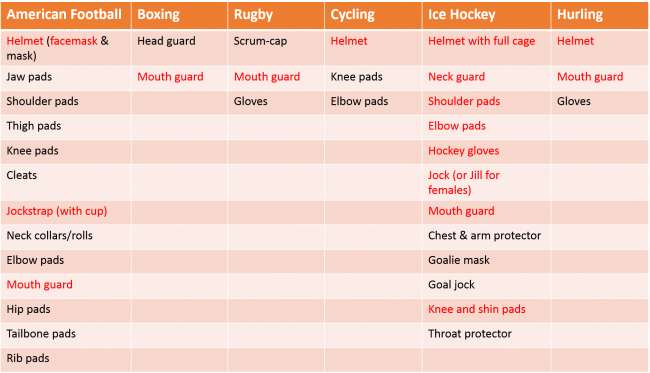
Table 2: Common Types of Sports Preventative Equipment
***Items in red are mandatory for younger adults***
Helmets and Face Guards[edit | edit source]
Helmets are often mandatory or highly advised in a number of sports to reduce the risk of injury from a blow to the head (e.g. American Football, Ice Hockey, Cycling). Face guards are frequently included in many ball games such as hurling or baseball to prevent facial injuries. In cycling specifically, it has been shown that wearing a helmet can reduce the risk of severe injury from an associated blow to the head by approximately 63-88%. Research is less extensive on the use and impact of helmets in other sports but there are many benefits in association with the wearing of helmets in sports such as ice hockey and rugby. Additionally, in other sports such as cricket, in Australia, the compulsory wearing of helmets in younger players reduced facial, neck and head injuries from 35% to 4% with its introduction[25][26].
Knee Braces[edit | edit source]
Knee braces specifically designed to support are made from elastic, foam or plastic which provide assistance to the knee joint during motion and also provide protection against direct blows. They are used throughout the world but their ability to prevent injuries is unclear. There is however evidence to show its protective properties to reducing the risk of ligament sprain and giving a larger resistance to blows to the knee[27].
Ankle Braces and Taping[edit | edit source]
Ankle braces fundamentally provide a carbon copy to that of the knee brace with a focus on the ankle which helps to reduce the range of motion of the ankle. Traditional taping may also be used in a sport that helps to limit ankle movement in order to prevent injury. Ankle ligament sprains are the main preventative area these braces/taping methods aid especially in those who have a history or predisposition to ankle sprains. Evidence suggests braces or taping can reduce the likelihood of ankle sprains by 69%-71% amongst athletes with previous ankle injuries[28][29].
Mouth Guards[edit | edit source]
Mouth guards, also called gum shields are used mainly in contact sports where they act as shock absorbers separating the lower and upper teeth as well as teeth from its surrounding tissue. The specific shock-absorbing characteristics of this sport protective equipment reduce the force transferred to teeth which therefore helps to prevent orofacial or dental injuries which can be caused by blows to the head in sports such as boxing, rugby and ice hockey[30]
Epidemiology/Statistics of Injury[edit | edit source]
Table 3: Prevalence of Injury in Schoolchildren Among Physical Education Class
Adapted from Sreekaarini (2014)[31]
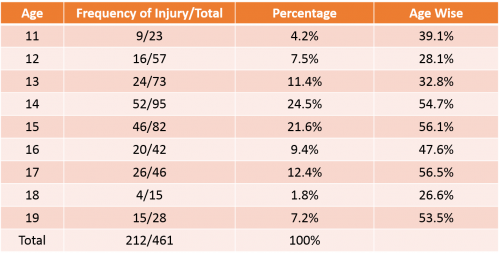
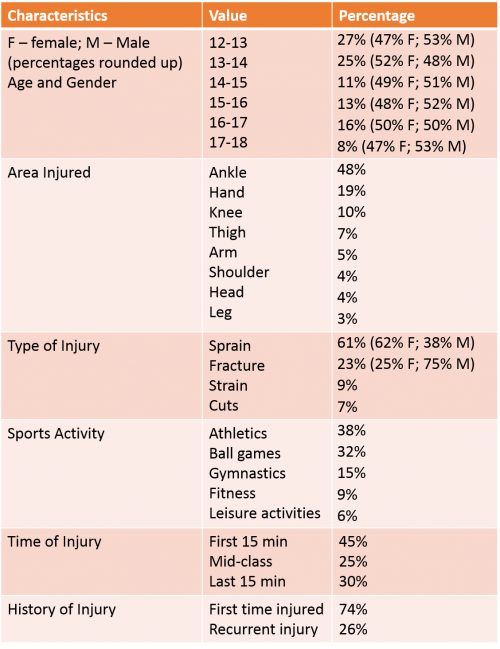
Table 4: Characteristics of Sports Injuries in Students (n=192)
Adapted from Carmeli (2003)[32]
Potential Mechanisms of Injury in Sport[edit | edit source]
- Lack of protection: A lack of protection in contact/high-velocity sports, in particular, may cause injury so protective equipment is necessary to reduce the impact of the level of force exerted on the individual and in turn reduce injury risk.
- Field/Facilities: The terrain/ground may lead to a reduction in grip such as that in ice hockey. Slippery/uneven surfaces can lead to a harder fall during contact.
- Inappropriate footwear: Inappropriate footwear may lead to reduced protection and control of the ankle and foot.
- Physical games: Serious injury may result from contact such as a direct blow or as a result of falling to the ground.
- Lack of knowledge/facilities surrounding appropriate equipment use: If particular sports protective equipment, such as a helmet, is not worn correctly/snugly in place it can lead to a reduction in its effectiveness in reducing serious injury.
- Rules/Regulatory bodies: In sports such as ice hockey, there is player contact where one player fends another off the play which can result in serious harm to the individual involved.
- Age: If an individual is much younger than a fellow player it can have a significant influence on the development of injuries for contact sports in particular. A person playing at a young age is also more vulnerable as their bones are still growing until adulthood.
Issues in Specific Sports[edit | edit source]
Hurling[edit | edit source]
Hurling (or Camogie) is an Irish national sport where two teams consisting of 15 players each use a 1-metre long ash stick (hurley) to strike a hard leather ball (sliotar). It is one of the fastest field sports. Due to the nature and rules of the game such as swinging of the hurley and the weight of the sliotar, the likelihood of injury is very high. In previous years helmets were not regularly worn or mandatory. More recently, this rule has changed and wearing helmets have greatly reduced common head injuries. The proportion of hurling-related head injuries among A&E treated players are reduced 10-fold when full head protection is available by wearing both a helmet and face guard.
Evidence of iatrogenic-like consequences was discovered in hand injuries when full head protective equipment was used[33][34].
American Football[edit | edit source]
American Football is arguably one of the most dangerous sports where players of different weights, sizes, speeds, and strengths, depending on their position, face off to tackle the player on the opposition. Because of this, protection is vital especially for smaller players or ones who are playing in quarterback positions where more skill and precision are needed oversize. In 12-18-year-old, there can be huge discrepancies in builds, weights, and sizes when playing against their counterparts and this, therefore, means a vast array of protection must be worn to prevent serious harm[36].
Helmet/Face Mask[edit | edit source]
Due to the unforgiving, aggressive nature of American football, it is necessary to wear a helmet to prevent a serious head injury. Along with this, players may decide to wear other equipment to further protect themselves such as:
- Mouth guard: provides shock absorption separating the lower and upper teeth as well as teeth from their surrounding tissue
- Chin straps: allows the helmet to be secured correctly allowing a snug fit.
- Air-filled interior pockets: design of air-filled pockets works as a preventative measure against serious concussions which are a regular occurrence in the game.
- Face masks: can comprise off a bar that comes down past the nose area and joins 2 or 3 bars from both sides. This 'cage' precludes an opponent from reaching into the facial area with their hand.
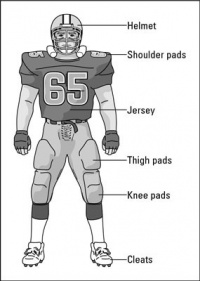
Pads[edit | edit source]
There are many different pads that can be used to absorb blows from another player during contacts such as shoulder pads, thigh pads, elbow pads, hip pads, tail pads, and knee pads. Shoulder pads protect the individual’s shoulder but also give protection to the sternum region where others may also provide protection to the rotator cuff muscles and top of the arm.
Boots/Cleats[edit | edit source]
Football boots/cleats can come with studs of varying sizes from ½ inch to 1 inch. The field may differ in its surface from hard to soft ground. Proper selection of cleats provides traction to the ground, therefore, prevents injury from falls to the ground[37].
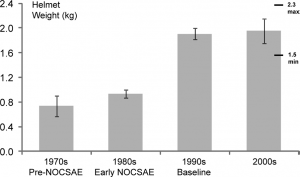
Changes in the design of different sports equipment with particular focus on the helmet have helped to further the protective aspect of players in American Football. Over the years the helmet has changed extensively to provide greater support with added protection with face masks, etc. The size and weight have also been modified with a heavier helmet and air-filled pockets for a preventative capacity especially for preventing concussions from contact[38]. &nbsForbes
Ice Hockey[edit | edit source]
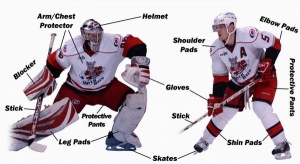
Ice hockey is a game played in many parts of the world and is a high-contact, high-speed team sport where two teams use their individual stick to hit a puck into the other’s net. In this contact, sports injuries are quite common so protective equipment is very important to prevent serious injury. The game focuses on physicality among players and other influences such as hockey pucks, skate blades and hockey sticks all having an impact in causing serious harm to an individual. Injuries that usually occur include concussions, muscle strains, broken bones, contusions, hyperextensions and ligament tears[39].
See IIHF Official Rule Book to read about mandatory and recommended equipment for ice hockey by the International Ice Hockey Federation's Inline Official Rulebook 2018-2022.
Below are two videos illustrating how to put on protective hockey gear and how ice hockey equipment protects you.
Importance of Equipment for Adolescents[edit | edit source]
Protective equipment, in general, is on the rise as it is of vital importance for individuals involved in sport and physical activity. It is even more crucially important for younger adults who are still developing because an injury such as a fall may cause even more damage to a 12-year-old than a 20-year-old.
The reason younger individuals are required to wear more equipment than their adult counterparts is mentioned below. It is important to remember they are still growing and their bones are still developing and as a result, they are more susceptible to injuries [23].
Type of Injuries[edit | edit source]
- Overuse injuries
- Strains
- Contusions
- Dislocations (shoulder)
- Physeal plate injuries
Areas Commonly Affected[edit | edit source]
- Extensor mechanism of the knee from increased stresses when running, jumping and squatting
- Achilles tendon
- Muscles: mainly of lower limb
- Shoulder (labrum-ligament complex)
- Physis
Long-Term Effects on Adolescents[edit | edit source]
- Can affect normal physical growth and maturation
- Osgood-Schlatter disease: traction apophysitis of the tibial tubercle
- Sinding-Larsen-Johansson: occurs at the distal pole of the patella
- Myositis ossifications
- Instability of the shoulder: Bankart lesion
- Physeal plates: causing deformities by affecting normal growth[23]
Causes[edit | edit source]
- Excessive stresses
- Forceful contraction of the muscle
- Improper warm-up before sports, fatigue, previous injury
- Physical contact, falls
- Acute mechanical overload
Possible Role/Treatment of Physiotherapists[edit | edit source]
General Management[edit | edit source]
- Injury management and education to prevent overtraining and exposure to excessive levels of physical activity.
- Rest, ice, hamstring stretching, quadriceps strengthening, patellar tendon taping.
- Achilles and plantar fascia stretching, or cast immobilisation in extreme cases.
- Teams and individuals education about the importance of warm-up and stretch before sporting activities.
- Early initial immobilization of muscle under considerable stretch to reduce oedema and accumulation of scar tissue and earlier recovery of strength.
- Wearing preventative/protective equipment such as helmets, pads, etc.
Specific Examples of Management[23][edit | edit source]
Overuse injuries[edit | edit source]
Repetitive application of submaximal stresses to otherwise normal tissue. This is common among organised sports such as American Football, compared with recreational/backyard games. Overtraining and exposure to excessive levels of physical activity can present an increased risk of injury. If not managed properly and efficiently, overuse injuries can affect normal physical growth and maturation. Prevention is key, gradual rather than sudden increases in intensity can usually avoid physical breakdown.
Strains[edit | edit source]
Occur to the muscle due to forceful contraction of the specific area. Strains are commonly arranged among severity making up 3 degrees of strains with the third being a complete tear of the musculotendinous junction.
Contusions[edit | edit source]
Most commonly occur from contact sports such as ice hockey or hurling.
Dislocations[edit | edit source]
Not very common among younger athletes; however, when shoulder dislocations occur they can be some of the most incapacitating injuries. Approximately 90% of shoulder dislocation patients can experience Bankart lesions, later on, resulting in long-term disability and instability in the labrum-ligament complex.
Physeal plate injuries[edit | edit source]
The most vulnerable part of a younger, immature athlete is that of the physis where physeal plate injuries can have devastating effects on growth. Physeal plate injuries/fractures are often caused by acute mechanical overload often associated with collision/contact sports such as American Football or rugby.
Considerations of Preventative Equipment[edit | edit source]
There are some criticisms of using certain protective equipment in sports. Below are some arguments against the use of protective equipment in sports.
- Players: not used to it, may slow them down or affect vision/performance.
- Regulatory bodies possibly lenient and not wanting a change in the sport which may have been played somewhat successfully for a number of years.
- In skiing, it has been demonstrated that although helmets provide protection, wearing them may also increase the risk of concussion from impact.
Children's Participation in Dangerous Contact Sports[edit | edit source]
A letter published in the Guardian newspaper on 2 March 2016 stated that studies have shown that the risk of injury from rugby (a high-impact collision sport) in under 18's is high and that the injuries are often serious. Currently, many secondary schools in the UK insist on contact rugby as a compulsory part of the physical education (PE) curriculum from age 11. The letter said: 'The majority of all injuries occur during contact or collision, such as the tackle and the scrum. These injuries, which include fractures, ligamentous tears, dislocated shoulders, spinal injuries, and head injuries, can have short-term, life-long, and life-ending consequences for children'[42].
Prehabilitation[edit | edit source]
Physiotherapists are often involved with the aftercare of an injury or accident. Patients are then usually started on a rehabilitation programme which can vary significantly depending on the circumstances. Alternatively, “prehabilitation” (or prehab) is a current and emerging strategy that is used both in sporting and clinical settings to help reduce injury, help maintain physical status or to improve recovery time after surgery. While there have been many studies discussing the effects of prehabilitation in post-operative patients regarding total knee replacements[43], spinal surgery[44], cardiac procedures[45], and colectomies[46], this part will primarily focus on the effects of prehabilitation to reduce injury occurrence in a sport and physical activity context, particularly in adolescents (aged 12-18).
While there is no actual definition of “prehabilitation”, it is generally recognised as an injury prevention programme that is specific to the individual and chosen sport or activity. Essentially, it is specific training to prevent an injury from occurring. Meir et al. suggest that 'prehabilitation describes a systematic approach to identifying common injuries within a specific sport and then designing an appropriate series of exercises that work toward minimizing their incidence'[47]. This is supported by Brukner[48] who explains that the first step of injury prevention is to understand the incidence and severity of injuries, e.g. when working with a team the physiotherapist should record all injuries within the squad. This may easily be done when working with a specific sports team or club, however, it presents barriers for individuals who participate in sport and physical activity with no club affiliation or access to a physiotherapist. Perhaps if physiotherapists have a more collaborative relationship with schools and other organisations it would be possible to reach those adolescents who do not get prehabilitation/injury prevention programmes elsewhere. This could have a promising impact on injury prevention within this population. Indeed, research by Roach et al.[49]suggested that up to half of all injuries that children sustain in sport are preventable, highlighting the potential role a physiotherapist could play. Furthermore, Meir et al.[50] suggested that common injuries sustained in rugby might be preventable or the severity lessened if the affected area of the body goes through a specific preventative conditioning program.
Prehabilitation programmes usually consist of strength and conditioning training, proprioception exercises, and sport-specific drills. Occasionally psychological skills training may be incorporated. Below explains how these aspects of prehab can help reduce the incidence and severity of injury within adolescents.
Strength and Conditioning Training in Adolescents[edit | edit source]
Strength and conditioning is the most common type of prehabilitation used when working with young athletes. Studies have found that programmes that include strength, flexibility, balance, and sport‐specific fitness and technique training prevent lower limb injury[51]. It is also thought that the benefit is continued when the prehab is performed throughout the playing season. This provides important information regarding physiotherapy practice, as strength and conditioning should be an ongoing “prehab” strategy for young athletes in which the physio should recommend. This agrees with adult studies that used preventive programmes in volleyball resulting in significant reductions in ankle sprains[52][53][54]. Similarly, conditioning programmes in football have shown a 50–75% reduction in injuries in general and a significant decrease in ACL injuries[55]. Given the evidence that strength and conditioning training helps prevent injury, it could have important implications for the role of a physiotherapist. A physio that works directly with a club or team has the opportunity to implement a specific strength and conditioning programme. For adolescents who participate in sport and physical activity, and do not have access to a physiotherapist through a club or organisation, physiotherapists should have a responsibility to work closely with schools to highlight the potential use of strength and conditioning training to prevent injury.
Resistance Training for Adolescents[edit | edit source]
The literature regarding resistance training in adolescents has been conflicted over the last 20 years. Studies have suggested that resistance training in youths can be harmful[56]; however, these programs can benefit children and preadolescents by improving their strength, bone density, balance, lipid profiles, fat-free mass, and personal self-esteem[57][58][59][60][61]. Additionally, strength training can help reduce injury by improving joint integrity, therefore reducing the risk of subluxation, dislocation, and strains. It is within a physiotherapist’s role to ensure that resistance training is completed safely and is in line with the individual's growth. The benefits that can be achieved for adolescents participating in an appropriate resistance training programme are outlined underneath.
Current Guidelines[edit | edit source]
The current guidelines put forward by the National Strength and Conditioning Association (NSCA) for resistance training are[62]:
- A properly designed and supervised resistance training program is relatively safe for youths.
- A properly designed and supervised resistance training program can enhance the muscular strength and power of youths.
- A properly designed and supervised resistance training program can improve the cardiovascular risk profile of youths.
- A properly designed and supervised resistance training program can improve motor skill performance and may contribute to enhanced sports performance of youths.
- A properly designed and supervised resistance training program can increase a young athlete's resistance to sports-related injuries.
- A properly designed and supervised resistance training program can help improve the psychosocial well-being of youths.
- A properly designed and supervised resistance training program can help promote and develop exercise habits during childhood and adolescence.
Stretching[edit | edit source]
It has long been believed that increased flexibility attained through stretching decreases injury incidence[63]. However, recent research by Magnusson et al.[64] has suggested that 'pre-exercise stretching in isolation (with or without warm-up) does not reduce overall injury rates'[65]. Furthermore, a systematic review by Thacker et al.[66]concluded that, while stretching increased flexibility, increased flexibility did not significantly reduce injury (p=9.3).
In the evidence that did show a benefit to pre-exercise stretching, it was found to be in conjunction with a warm-up before the stretching. The conflicting evidence within this area suggests that stretching is not the most important aspect in injury prevention. Rather, it appears that focusing time on strength training, proprioception, and appropriate warm-ups is more effective to reduce the incidence of injury in adolescents. This information is valuable for physiotherapists when constructing a prehabilitation programme for adolescents. Indeed, physiotherapists should recognise that while it is important for individuals to have a good range of motion around joints, stretching is not an essential part of injury prevention. On the contrary, some studies have even suggested that stretching can actually increase injury incidence.
Shrier[67] has put forward five reasons why stretching is not an effective means for injury prevention:
- In animals, immobilization or heating-induced increases in muscle compliance cause tissues to rupture more easily.
- Stretching before exercise should have no effect on activities in which excessive muscle length is not an issue (e.g., jogging).
- Stretching will not affect muscle compliance during eccentric activity when most strains are believed to occur.
- Stretching can produce damage at the cytoskeleton level.
- Stretching appears to mask muscle pain in humans.
It is important for physiotherapists to be aware of the evidence surrounding stretching including the potential risks for injury. It should be within their role to know when to recommend the use of stretching and educate young athletes on the matter.
Proprioceptive Training[edit | edit source]
Proprioception is the term used to describe the sensory information that contributes to the sense of body position and movement. A common example of proprioceptive training is the use of a wobble board to improve sensory input from the ankle or knee. The theory behind proprioception is that human muscles contain specific nerve endings called “mechanoreceptors” that can detect pain, pressure, joint motion and position[68]. These mechanoreceptors send signals to the CNS and give information about what is happening around the body. Visual feedback and the vestibular system (inner ear) also play an important role within proprioception. Visual cue’s help provide the CNS with reference points for orientating the body in space and the vestibular system helps maintain overall body posture and balance[69]. With these important aspects to consider, proprioception is sometimes referred to as a' collection of sensations regarding joint movement and joint position'[70].
It is thought that proprioceptive training can help information of joint motion and position to be sent quicker to the CNS, therefore, leading to faster, stabilising and injury-preventing actions of the joints and muscles. A randomised control trial by Sheth et al.[71] examined muscle reaction time of the anterior tibialis, posterior tibialis, peroneus longus, and flexor digitorum longus in response to a sudden, potentially injury-producing change in ankle position (trap-door). Twenty healthy adults were recruited and were divided into a control group (n=10) and an experimental group (n=10). The experimental group were given proprioceptive training using an ankle disc for 8 weeks and were found to have a significant increase of speed at which the muscles responded to the sudden changes in ankle position. Additionally, it also altered the rate at which force was produced by the posterior tibialis.
Research within this area has been driven by two main things[72]:
- If muscles can react more quickly in response to a postural or joint perturbation, there should be better control of movement and a lower risk of uncontrolled motions which might increase injury.
- If muscles react more quickly, an athlete can function with greater power (more force production per unit time) which could lead to improved performance.
Due to the growing evidence within this area, it is becoming more common to incorporate proprioceptive training in prehabilitation programmes to reduce the incidence of injury. Indeed, there is good evidence supporting its use. A systematic review by Aberneth and Bleakley[73] looked at three studies that examined the effectiveness of various proprioceptive training. A study that investigated a home‐based proprioceptive training programme using a wobble board showed improved static and dynamic balance in healthy adolescents and reduced the incidence of injury over a 6‐month period[74]. Similarly, a study by Wedderkopp et al.[75] found that female handball players who implemented the use of an ankle disc in their training programme were less likely to be injured than a control group.
[76]Sport Specific Drills[edit | edit source]
- Help prepare the body for the specific skills performed in the sport.
- Help psychologically prepare the athlete which can help reduce injuries.
Common Injuries in Children Aged Between 12-18[edit | edit source]
- Osgood-Schlatters disease - Preventative strategies
- Stretching
- Controlled loading
- Minimize plyometrics
- Sever's Disease - Preventative Strategies
- Stretching
- Identifying podiatry imbalances
Education[edit | edit source]
A physiotherapist can use many approaches within their role to treat individuals. Some of these approaches include manual therapy, exercises, physical activity advice and educational advice[79]. The CSP states that a physiotherapist looks at the person as a whole, including the patient in their own care through education, awareness, empowerment, and participation in their own treatment[80]. As a physiotherapist, one of the main roles is to educate patients during the treatment process. Patient education is so important because:
- Develops credibility: by educating patients you will demonstrate your knowledge and reveal yourself as the best resource for information and treatments.
- Develops trust: by providing information to the patient that is specific to their problem you will aid in developing trust and making them feel better.
- Increases understanding: if education is provided patients will have a better understanding of their problem and how your treatment is going to help them.
- Improve compliance: when a patient is discharged, it is normal practice to provide educational materials that are informative and specific. This will leave the patient with a positive reaction to the treatment as a whole making them more likely to follow through.
Hydration[edit | edit source]
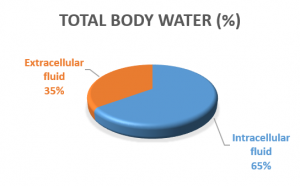
Staying hydrated is essential as your body is composed of 60% water on average[81]. The water is distributed between extracellular (between cells and in the blood) and intercellular (inside cells) and is the main component of body fluids such as blood and synovial fluid[81]. A breakdown of fluid is represented in the figure to the right. The concentration of body fluids is controlled by stimulating thirst or by adapting urinary output; however, if the water loss is not replaced, dehydration can set in.
Dehydration can occur if you lose as little as 2% body mass. The individual can develop impaired cognitive function, headaches, decreases in physical performance and develop symptoms of fatigue[81][82][83]. When an individual becomes fatigued or not able to perform at his best there is an increased risk of injury whether the individual is an adult or child. In some rare cases, the over-drinking can result in hyponatraemia, and low levels of sodium[81].
The volume of water required can depend on the individual and a few factors:
- Intensity of physical activity
- Age
- Weather
- Body composition
In summary, the need for physiotherapists to educate their patients to stay hydrated is a must. It can help to prevent dehydration which could reduce injury occurrences.
Nutrition[edit | edit source]
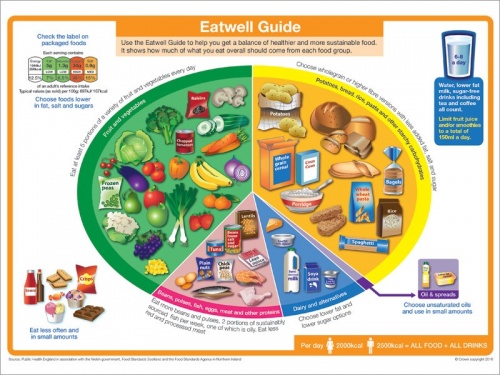
Good nutrition is important to anyone taking part in physical activity. It may not be the first common effect that you think of but your diet can help with muscle recovery. A good diet is what helps to build a strong body structure. The Eat well Guide demonstrates how to maintain a well-balanced diet focusing on the five main food groups [86][87]. Within the guide it is recommended to:
- Eat at least 5 portions of fruit and vegetables a day.
- Base meals on starchy carbohydrates, whole grain preferably.
- Eat small amounts of dairy.
- Consume protein: aiming for fish two times a week.
- Use unsaturated oils and spreads in small amounts.
- Keep foods high in fat, salt and sugar to a minimum.
- Drink plenty of water: six to eight glasses a day.
To look at the Eat well Guide in more detail use the picture with link below.
In order to prevent injuries during physical activity, health professionals should be providing adolescents with information about diet. In adolescents, healthy diets and physical activity have been proven to provide many short and long term health benefits[88][89]. Despite the known benefits of eating regular well-balanced meals, adolescents are more likely to skip breakfast than any other meal[90][89]. According to data from the Health Behaviour in school-aged children nearly three-fifths of young people don’t meet the required fruit intake and only ⅓ will eat vegetables[89] This is less than the recommended intake and if these adolescents were to take part in physical activity they could be increasing their chance of injury due to the body not being prepared with the adequate requirements. There are three eating habits that have been suggested to help prevent injuries in adults[91] taking part in physical activity however these habits can also relate to adolescents:
- Eat enough: if you are taking part in regular physical activity it is important to make sure that calorie intake is sufficient. If not, your body’s ability to repair tissue damage and muscle recovery will decrease.
- Keep fat in the diet: fat is required to keep cells healthy and some fats are essential for the inflammation process.
- Calcium intake: calcium is needed to keep bones healthy and strong. Especially in adolescents, the need for calcium is important to reduce the risk of bone strains or stress fractures.
Skill Acquisition[edit | edit source]
Skill acquisition can aid in the prevention of injuries in adolescents. This method of learning involves three stages of learning.
[92]
Studies have found that including skill acquisition in training programs have reduced the injury rate in children and adolescents. A study by Scase et al.[93] looked into the effects of teaching landing and falling skills on improving landing skills and preventing injuries in young football players. They used two groups where one was provided with the specific landing training and the other group was the control with no additional landing training. Between the groups, the intervention group had a lower rate of injuries and the onset of injuries was later in the season. Studies by Powers and Fisher[94] and Myer et al.[95] also concluded from research that the involvement of skill acquisition in exercise helps prevent injuries. Powers and Fisher[96]go on to explain that the changes in brain neuroplasticity are what underlies the behaviours associated with injury prevention. They say that the decrease in corticomotor excitability may be because of this change as control is reallocated to the subcortical motor regions after specific skill training[97]. Although these studies focused on specific sports this can be relevant to all physical activities.
Therefore, the need for physiotherapists to educate adolescents on basic skills such as landing, balance, running or catching is important. Most of these skills are used within a number of physical activities and if young individuals are not able to master these then they will be increasing their chance of injury occurring.
Posture[edit | edit source]
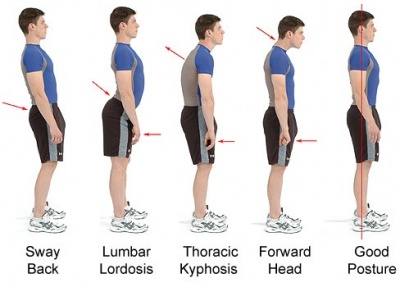
Posture can have a big effect on the prevalence of injuries in physical activity. Teenagers are growing at different rates and these changes can put pressure on the body through changes in posture[98]. Most adolescents are still at school where they are required to sit in a chair for periods of time resulting in slouching in a chair. Although this is not directly related to physical activity the same rules apply and what someone does when they are not taking part in physical activity can affect them when they do.
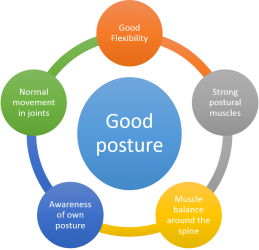
Good posture involves being able to train your body to lie, sit, walk and stand in positions where the least amount of strain is placed on ligaments and muscles[99]. The Mayfield Clinic has created a document that provides a detailed overview of good posture for sitting, standing and even driving. You can access that document here. They suggest that in order to maintain a good posture you need to meet certain requirements and benefits from having a good posture include:
Examples of different postures are illustrated below. The arrows on the picture show where the change in posture has occurred. Poor posture can lead to changes in muscle balance and length, decrease in sports performance, altered biomechanics, reduced flexibility and an increased risk of developing an injury[100]. Therefore, it would be beneficial if physiotherapists can educate patients on how to maintain a good posture. When students are studying to be a physiotherapist, they are taught how to identify good posture, key points to look out for and provide advice on and thus educating patients about how to maintain posture should be routinely incorporated into treatments when appropriate.
Rest[edit | edit source]
Many children and adolescents take part in games, training, and sports on a daily basis because of this the body doesn’t get enough time to fully rest[101]. It is well known that they need to rest between bouts of physical activity as a lack of rest and muscle fatigue will increase an individual’s risk of obtaining an injury[102]. The NHS[103] advise that adolescents need between 8 to 9 hours of good sleep to be well-rested. In order to achieve this, they need to reduce caffeine intake, not eat late at night, limit time spent on electronics and get into a routine[104]. If a teen is not meeting the required amount of rest they are not preparing themselves well for any physical activity that they plan to take part in.
[108]
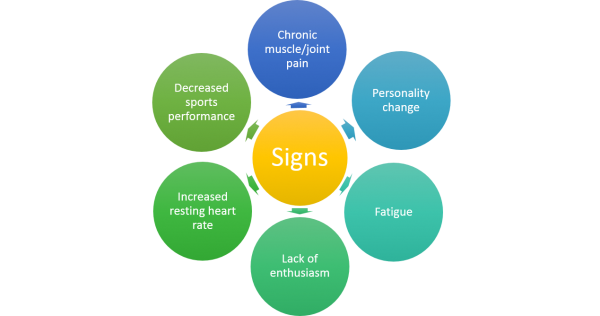
Overtraining syndrome is a condition where reduced rest results in maladapted physiology following excessive exercise[109][110]. Some common signs of overtraining are:
Kreher and Schwatz[111] suggested that overtraining can be caused by systemic inflammation and consequent changes in the central nervous system, neurohormonal changes and decrease in mood. For more in-depth information about changes that occur read the following article by Kreher[112]. Brenner[113] provides some guidelines to follow to prevent overtraining/burnout:
As a healthcare practitioner providing education on taking rest is important. During education, individuals should be made aware of the risks of overtraining and advising them on the common signs to look for as this can give them the responsibility of their own wellbeing[114]. During sessions, it would be a good idea to ask adolescents how their training is going and whether they have increased their workload recently as this can give you an indication of how they are doing and feeling[115]. Therefore, as a physiotherapist, it is important to provide education about the importance of rest as it can help to prevent injuries from occurring.
Conclusion[edit | edit source]
With the increasing demand from the NHS to maintain future healthy populations, physiotherapists will have to increase their scope of practice to include helping with the prevention of injury and accidents, especially in adolescents. This would be in addition to the current job description which involves treating injuries amongst other roles. With this in mind, the physiotherapists can help prevent injury and accident by:
- Encouraging and enforcing current legislation.
- Educating patients on the importance of protective equipment and prehabilitation in the prevention of injury and accident.
- Having an input into the law system due to the workload physiotherapists have due to injuries and accidents.
Looking into the future, physiotherapists have an advantage over other Allied Health Professionals due to the time spent with patients during assessments and treatment sessions. They can utilize this time to educate patients and use research, some of which has been provided in this resource, to highlight the importance of protective equipment in preventing injuries and accidents. This opportunity to educate the general public would hopefully lead to a reduction in the number of injuries.
References[edit | edit source]
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 1.7 Collard D, Paw C, Van Mechelen W, Verhagen R. Design of iplay study: systematic development of a physical activity injury prevention program for primary school children. Sports Medicine 2009;39(11):889-901. (last accessed 18 Nov 2021).
- ↑ Hall G, Laddu DR, Phillips SA, Lavie CJ, Arena R. A tale of two pandemics: How will COVID-19 and global trends in physical inactivity and sedentary behaviour affect one another? Prog Cardiovasc Dis. 2021 Jan-Feb;64:108-110. DOI: 10.1016/j.pcad.2020.04.005. Epub 2020 Apr 8. PMID: 32277997; PMCID: PMC7194897.
- ↑ 3.0 3.1 World Health OrganizatiLon. Obesity and Overweight-Key Facts (2020). Available from https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight [last accessed 18/11/2021]
- ↑ 4.0 4.1 4.2 4.3 World Health Organisation (WHO). Physical activity. Available from https://www.who.int/news-room/fact-sheets/detail/physical-activity [last assessed 18/11/2021]
- ↑ Habelt S, Hasler CC, Steinbrück K, Majewski M. Sports injuries in adolescents. Orthopaedic reviews. 2011 Nov 7;3(2):18.
- ↑ Brussoni M, Brunelle S, Pike I, Sandseter EB, Herrington S, Turner H, Belair S, Logan L, Fuselli P, Ball DJ. Can child injury prevention include healthy risk promotion?. Injury prevention. 2014 Dec 22:injuryprev-2014.
- ↑ Emery CA. Injury prevention and future research. Med Sport Sci. 2005;48:179-200. DOI: 10.1159/000084289. PMID: 16247258.
- ↑ CSP. Physiotherapy Framework: putting physiotherapy behaviours, values, knowledge & skills into practice. Available from file:///C:/Users/Charmene/Downloads/physiotherapy_framework_condensed_updated_sept_2013.pdf [last accessed 19 /11/2021]
- ↑ NHS. The NHS Knowledge and Skills Framework - a short guide to KSF dimensions. [last accessed 19/11/2021]
- ↑ CSP. Professional Frameworks. Available fromhttp://www.csp.org.uk/professional-union/careers-development/career-development/professional-frameworks [last accessed 19/11/2021]
- ↑ Spinks AB, Macpherson AK, Bain C, McClure RJ. Injury risk from popular childhood physical activities: results from an Australian primary school cohort. Injury Prevention. 2006 Dec 1;12(6):390-4.
- ↑ 12.0 12.1 12.2 12.3 Macpherson A, Spinks A. Bicycle helmet legislation for the uptake of helmet use and prevention of head injuries. Cochrane Database Syst Rev. 2008 Jul 16;2008(3): CD005401. DOI: 10.1002/14651858.CD005401.pub3. PMID: 18646128; PMCID: PMC6823199.
- ↑ 13.0 13.1 Gleave J, Bedford: Transport Planning Society. Cycle helmets: the impacts of cycle helmet legislation on cyclist fatalities and premature deaths in the UK. [last accessed 19/11/2021]
- ↑ Cycling UK. Campaign with us. Available fromhttp://www.cyclinguk.org/campaigning/views-and-briefings/cycle-helmets [last accessed 19/11/2021]
- ↑ Macpherson A, Spinks A. Bicycle helmet legislation for the uptake of helmet use and prevention of head injuries (Review). Cochrane Database of Systematic Reviews. 2007 Feb;2.
- ↑ Macpherson AK, To TM, Macarthur C, Chipman ML, Wright JG, Parkin PC. Impact of mandatory helmet legislation on bicycle-related head injuries in children: a population-based study. Paediatrics. 2002 Nov 1;110(5):e60-.
- ↑ Walter SR, Olivier J, Churches T, Grzebieta R. The impact of compulsory cycle helmet legislation on cyclist head injuries in New South Wales, Australia. Accident Analysis & Prevention. 2011 Nov 30;43(6):2064-71.
- ↑ Macpherson AK, To TM, Macarthur C, Chipman ML, Wright JG, Parkin PC. Impact of mandatory helmet legislation on bicycle-related head injuries in children: a population-based study. Paediatrics. 2002 Nov 1;110(5):e60-.
- ↑ Olivier J, Creighton P. Bicycle injuries and helmet use: a systematic review and meta-analysis. International journal of epidemiology. 2016 Jul 22:dyw153.
- ↑ Macpherson AK, Parkin PC, To TM. Mandatory helmet legislation and children's exposure to cycling. Injury prevention. 2001 Sep 1;7(3):228-30
- ↑ James Cracknell. A personal appeal from James Cracknell - Use your head. Use your helmet. Available from https://www.youtube.com/watch?v=nu4QzAIayTU [last accessed 12 Nov 2021]
- ↑ AIBA. AIBA Open Boxing (AOB): Competition Rules. http://aiba.s3.amazonaws.com/2015/02/AOB-Competition-Rules-2015-09-11.pdf (accessed 15 Nov 2016).
- ↑ 23.0 23.1 23.2 23.3 Merkel DL, Molony JT Jr. Recognition and management of traumatic sports injuries in the skeletally immature athlete. Int J Sports Phys Ther. 2012 Dec;7(6):691-704. PMID: 23316432; PMCID: PMC3537461.
- ↑ Hockeyhurlingshinty2. The hits collection - hockey v hurling. Available fromVox. The NFL's concussion crisis, explained. Available from https://youtu.be/tnAmddi52Y8 [last accessed 12 Nov 2021]
- ↑ Thompson DC, Rivara FP, Thompson R. Helmets for preventing head and facial injuries in bicyclists. Cochrane database of systematic reviews. 2000;4.
- ↑ Thompson DC, Rivara FP, Thompson R. Helmets for preventing head and facial injuries in bicyclists. Ann Emerg Med. 2003 May;41(5):738-40.
- ↑ Thacker SB, Stroup DF, Branche CM, Gilchrist J. Prevention of knee injuries in sports: A systemic review of the literature. Journal of Sports Medicine and Physical Fitness. 2003 Jun 1;43(2):165.
- ↑ Handoll HH, Rowe BH, Quinn KM, de Bie R. Interventions for preventing ankle ligament injuries. The Cochrane Database of Systematic Reviews. 2001;3(3):CD000018.
- ↑ Handoll HH, Rowe BH, Quinn KM, de Bie R. Interventions for preventing ankle ligament injuries. The Cochrane Library. 2011.
- ↑ Knapik JJ, Marshall SW, Lee RB, Darakjy SS, Jones SB, Mitchener TA, dela Cruz GG, Jones BH. Mouthguards in sports activities history, physical properties and injury prevention effectiveness. Sports Medicine. 2007 Feb 1;37(2):117-44.
- ↑ Sreekaarini I, Eapen C, Zulfeequer CP. Prevalence of Sports Injuries in Adolescent Athletes. J Athl Enhancement 3. 2014;5:2.
- ↑ Carmeli E, Azencot S, Wertheim M, Coleman R. Sports injuries in students aged 12-18 during physical education classes in Israel. Biology of Sport. 2003 Jan 1;20(4):271-80.
- ↑ Crowley PJ, Crowley MJ. Dramatic impact of using protective equipment on the level of hurling-related head injuries: an ultimately successful 27-year programme. British journal of sports medicine. 2014 Jan 1;48(2):147-50.
- ↑ O'Connor S, McCaffrey N, Whyte EF, Moran KA. Epidemiology of injury in male adolescent Gaelic games. Journal of Science and Medicine in Sport. 2016 May 31;19(5):384-8.
- ↑ UNESCO. Hurling. Available from https://www.youtube.com/watch?v=pnOnc91W0KE. [last accessed 12 Nov 2021]
- ↑ Wiley. The American Football Player's Uniform. http://www.dummies.com/sports/football/the-american-football-players-uniform/ (accessed 9 Nov 2016).
- ↑ Wiley. The American Football Player's Uniform. http://www.dummies.com/sports/football/the-american-football-players-uniform/ (accessed 9 Nov 2016).
- ↑ Lundberg GD, Metzner D. How to Rescue American Football. Cureus. 2016 Apr;8(4).
- ↑ Council on Sports Medicine and Fitness, Brenner JS, Brooks A, Demorest RA, Halstead ME, Kelly AK, Koutures CG, LaBella CR, LaBotz M, Martin SS, Moffatt K. Reducing Injury Risk From Body Checking in Boys’ Youth Ice Hockey. Pediatrics. 2014 Jun 1;133(6):1151-7.
- ↑ Marycate givs. Ice hockey protective equipment. Available from https://youtu.be/qq7s6JzMdFc [last accessed 12 Nov 2021]
- ↑ ChillerIceRinks. Hockey Gear- How to outfit your players haead to toe. Available from https://youtube/fid_y0VVQtE&t=25s [last accessed 12 Nov 2021]
- ↑ O’Dowd A. Experts seek a ban on tackling in school rugby to prevent child injuries. BMJ. 2016 Mar 3;352:i1289.
- ↑ Swank AM, Kachelman JB, Bibeau W, Quesada PM, Nyland J, Malkani A, Topp RV. Prehabilitation before total knee arthroplasty increases strength and function in older adults with severe osteoarthritis. The Journal of Strength & Conditioning Research. 2011 Feb 1;25(2):318-25.
- ↑ Nielsen PR, Jørgensen LD, Dahl B, Pedersen T, Tønnesen H. Prehabilitation and early rehabilitation after spinal surgery: a randomized clinical trial. Clinical Rehabilitation. 2010 Feb 1;24(2):137-48.
- ↑ Alkarmi A, Thijssen DH, Albouaini K, Cable NT, Wright DJ, Green DJ, Dawson EA. Arterial Prehabilitation. Sports Medicine. 2010 Jun 1;40(6):481-92.
- ↑ Gillis C, Li C, Lee L, Awasthi R, Augustin B, Gamsa A, Liberman AS, Stein B, Charlebois P, Feldman LS, Carli F. Prehabilitation versus RehabilitationA Randomized Control Trial in Patients Undergoing Colorectal Resection for Cancer. The Journal of the American Society of Anesthesiologists. 2014 Nov 1;121(5):937-47.
- ↑ Meir R, Diesel W, Archer E. Developing a Prehabilitation Program in a Collision Sport: A Model Developed Within English Premiership Rugby Union Football. Strength & Conditioning Journal. 2007 Jun 1;29(3):50-62.
- ↑ Brukner P. Brukner & Khan's clinical sports medicine. North Ryde: McGraw-Hill; 2012.
- ↑ Roach R, Maffulli N. Childhood injuries in sport. Physical Therapy in Sport. 2003 May 31;4(2):58-66.
- ↑ Meir R, Diesel W, Archer E. Developing a Prehabilitation Program in a Collision Sport: A Model Developed Within English Premiership Rugby Union Football. Strength & Conditioning Journal. 2007 Jun 1;29(3):50-62.
- ↑ Abernethy L, Bleakley C. Strategies to prevent injury in adolescent sport: a systematic review. British journal of sports medicine. 2007 Oct 1;41(10):627-38.
- ↑ Bahr R, Lian Ø, Bahr IA. A twofold reduction in the incidence of acute ankle sprains in volleyball after the introduction of an injury prevention program: a prospective cohort study. Scandinavian journal of medicine & science in sports. 1997 Jun 1;7(3):172-7.
- ↑ Stasinopoulos D. Comparison of three preventive methods in order to reduce the incidence of ankle inversion sprains among female volleyball players. British journal of sports medicine. 2004 Apr 1;38(2):182-5.
- ↑ Verhagen E, Van der Beek A, Twisk J, Bouter L, Bahr R, Van Mechelen W. The effect of a proprioceptive balance board training program for the prevention of ankle sprains a prospective controlled trial. The American journal of sports medicine. 2004 Sep 1;32(6):1385-93.
- ↑ Ekstand J, Gillquist J. Prevention of sports injuries in football players. International journal of sports medicine. 1984 Nov;5(S 1):S140-4.
- ↑ Pearce PZ. Prehabilitation: preparing young athletes for sports. Current sports medicine reports. 2006 Jun 1;5(3):155-60.
- ↑ Webster DA, Bayliss GV, Spadaro JA. Head and face injuries in scholastic women's lacrosse with and without eyewear. Medicine and science in sports and exercise. 1999 Jul;31(7):938-41.
- ↑ Olsen OE, Myklebust G, Engebretsen L, Holme I, Bahr R. Exercises to prevent lower limb injuries in youth sports: cluster randomised controlled trial. Bmj. 2005 Feb 24;330(7489):449.
- ↑ Wedderkopp N, Kaltoft M, Lundgaard B, Rosendahl M, Froberg K. Prevention of injuries in young female players in European team handball. A prospective intervention study. Scandinavian journal of medicine & science in sports. 1999 Feb 1;9(1):41-7.
- ↑ Kaminski TW, Perrin DH. Effect of prophylactic knee bracing on balance and joint position sense. Journal of athletic training. 1996 Apr;31(2):131.
- ↑ Caraffa A, Cerulli G, Projetti M, Aisa G, Rizzo A. Prevention of anterior cruciate ligament injuries in soccer. Knee surgery, sports traumatology, arthroscopy. 1996;4(1):19-21.
- ↑ Faigenbaum AD, Kraemer WJ, Blimkie CJ, Jeffreys I, Micheli LJ, Nitka M, Rowland TW. Youth resistance training: updated position statement paper from the national strength and conditioning association. The Journal of Strength & Conditioning Research. 2009 Aug 1;23:S60-79.
- ↑ Brukner P. Brukner & Khan's clinical sports medicine. North Ryde: McGraw-Hill; 2012.
- ↑ Magnusson SP, Simonsen EB, Aagaard P, Dyhre-Poulsen P, McHugh MP, Kjaer M. Mechanical and physiological responses to stretching with and without preisometric contraction in human skeletal muscle. Archives of physical medicine and rehabilitation. 1996 Apr 30;77(4):373-8.
- ↑ Brukner P, Khan K, Agosta T. Biomechanics of common sporting injuries. Clinical sports medicine. Sydney (Australia): McGraw-Hill. 2001:56-8.
- ↑ Thacker SB, Gilchrist J, Stroup DF, Kimsey Jr CD. The impact of stretching on sports injury risk: a systematic review of the literature. Medicine & Science in Sports & Exercise. 2004 Mar 1;36(3):371-8.
- ↑ Shrier I. Stretching before exercise does not reduce the risk of local muscle injury: a critical review of the clinical and basic science literature. Clinical Journal of Sports Medicine. 1999 Oct 1;9(4):221-7.
- ↑ Anderson O. Proprioceptive training and injury prevention. http://www.sportsinjurybulletin.com/archive/proprioceptive-exercises.html (accessed 16 Nov 2016).
- ↑ Anderson O. Proprioceptive training and injury prevention. http://www.sportsinjurybulletin.com/archive/proprioceptive-exercises.html (accessed 16 Nov 2016).
- ↑ Anderson O. Proprioceptive training and injury prevention. http://www.sportsinjurybulletin.com/archive/proprioceptive-exercises.html (accessed 16 Nov 2016).
- ↑ Sheth P, Yu B, Laskowski ER, An KN. Ankle disk training influences the reaction times of selected muscles in a simulated ankle sprain. The American journal of sports medicine. 1997 Jul 1;25(4):538-43.
- ↑ Anderson O. Proprioceptive training and injury prevention. http://www.sportsinjurybulletin.com/archive/proprioceptive-exercises.html (accessed 16 Nov 2016).
- ↑ Abernethy L, Bleakley C. Strategies to prevent injury in adolescent sport: a systematic review. British journal of sports medicine. 2007 Oct 1;41(10):627-38.
- ↑ Emery CA, Cassidy JD, Klassen TP, Rosychuk RJ, Rowe BH. Effectiveness of a home-based balance-training program in reducing sports-related injuries among healthy adolescents: a cluster randomized controlled trial. Canadian Medical Association Journal. 2005 Mar 15;172(6):749-54.
- ↑ Wedderkopp N, Kaltoft M, Lundgaard B, Rosendahl M, Froberg K. Prevention of injuries in young female players in European team handball. A prospective intervention study. Scandinavian journal of medicine & science in sports. 1999 Feb 1;9(1):41-7.
- ↑ 66Fit TV. Foot, Ankle, Knee, Hip, Back and Core Exercises using the 66fit Wobble Board - Part 1. Available from https://www.youtube.com/watch?v=J5vebLWclf4 [last accessed 12 Nov 2021]
- ↑ Nabil Ebraheim. Osgood Schlatter Disease - Everything You Need To Know - Dr. Nabil Ebraheim. Available from https://www.youtube.com/watch?v=V6QROj9EMaU [last accessed 18/11/2021]
- ↑ HealThatPain. Severs Disease and Heel Pain in Children. Available from https://www.youtube.com/watch?v=bRccMxPPId8 [last accessed 18/11/2021]
- ↑ NHS. Physiotherapy. http://www.nhs.uk/conditions/Physiotherapy/pages/introduction.aspx (accessed 16 November 2016).
- ↑ Chartered Society of Physiotherapy (CSP). What is physiotherapy? http://www.csp.org.uk/your-health/what-physiotherapy (accessed 16 Nov 2016).
- ↑ 81.0 81.1 81.2 81.3 81.4 Benelam B, Wyness L. Hydration and health: a review. British Nutrition Foundation Nutrition Bulletin. 2010;35:3-25.
- ↑ Ritz P, Berrut G. The importance of good hydration for day-to-day health. Nutrition reviews. 2005 Jun 1;63(suppl 1):S6-13.
- ↑ Shirreffs SM. The importance of good hydration for work and exercise performance. Nutrition reviews. 2005 Jun 1;63(suppl 1):S14-21.
- ↑ Healthy Kids. Drinks for hydration. https://www.healthykids.nsw.gov.au/kids-teens/stats-and-facts-teens/teens-nutrition/drinks-for-hydration.aspx (accessed 12 Nov 2016).
- ↑ Forsythe C. Your biggest hydration questions were answered. https://www.girlsgonestrong.com/blog/nutrition/water-hydration/ (accessed 8 Nov 2016).
- ↑ Gov.uk. The Eatwell guide. https://www.gov.uk/government/publications/the-eatwell-guide (accessed 9 Nov 2016).
- ↑ NHS. The Eatwell guide. http://www.nhs.uk/Livewell/goodfood/Pages/the-eatwell-guide.aspx (accessed 17 Nov 2016).
- ↑ Biddle SJ, Gorely T, Stensel DJ. Health-enhancing physical activity and sedentary behaviour in children and adolescents. Journal of sports sciences. 2004 Aug 1;22(8):679-701.
- ↑ 89.0 89.1 89.2 Pearson N, Atkin AJ, Biddle SJ, Gorely T, Edwardson C. Patterns of adolescent physical activity and dietary behaviours. International Journal of Behavioral Nutrition and Physical Activity. 2009 Jul 22;6(1):1.
- ↑ Dwyer JT, Evans M, Stone EJ, Feldman HA, Lytle L, Hoelscher D, Johnson C, Zive M, Yang M. Adolescents’ eating patterns influence their nutrient intakes. Journal of the American Dietetic Association. 2001 Jul 31;101(7):798-802.
- ↑ Triathlete. Eat to prevent injury. http://www.triathlete.com/2011/01/nutrition/eat-to-prevent-injury_18271 (accessed 16 Nov 2016).
- ↑ QuickTeach PE. Classification of Motor Skills: Skill Acquisition (Fine/Gross..Serial..). Available from https://www.youtube.com/watch?v=MyJzoXqfVx4 [last accessed 18/11/2021]
- ↑ Scase E, Cook J, Makdissi M, Gabbe B, Shuck L. Teaching landing skills in elite junior Australian football: evaluation of an injury prevention strategy. British journal of sports medicine. 2006 Oct 1;40(10):834-8.
- ↑ Powers CM, Fisher B. Mechanisms underlying ACL injury-prevention training: the brain-behaviour relationship. Journal of athletic training. 2010 Sep;45(5):513.
- ↑ Myer GD, Faigenbaum AD, Chu DA, Falkel J, Ford KR, Best TM, Hewett TE. Integrative training for children and adolescents: techniques and practices for reducing sports-related injuries and enhancing athletic performance. The Physician and Sports Medicine. 2011 Feb 1;39(1):74-84.
- ↑ Powers CM, Fisher B. Mechanisms underlying ACL injury-prevention training: the brain-behaviour relationship. Journal of athletic training. 2010 Sep;45(5):513.
- ↑ Powers CM, Fisher B. Mechanisms underlying ACL injury-prevention training: the brain-behaviour relationship. Journal of athletic training. 2010 Sep;45(5):513.
- ↑ Cahirphysio. Pilates for teenagers. http://cahirphysiotherapy.com/category/injury-prevention/ (accessed 19 Nov 2016).
- ↑ Mayfield Clinic. The posture of a healthy back. http://www.mayfieldclinic.com/PE-POSTURE.htm (accessed 28 Oct 2016).
- ↑ Donaldson-Barron. Strategies to prevent injury in adolescent sport. http://www.kidslink.co.nz/strategies-to-prevent-injury-in-adolescent-sport/ (accessed 18 Nov 2016).
- ↑ Sippel K. Prevention and Treatment of Pediatric and Adolescent Overuse Injuries. Undergraduate Research Journal for the Human Sciences. 2013 Apr 9;12(1).
- ↑ Johns Hopkins Medicine. 10 tips for preventing injuries in kids and teens. http://www.hopkinsmedicine.org/health/articles-and-answers/prevention/10-tips-for-preventing-sports-injuries-in-kids-and-teens (accessed 19 Nov 2016).
- ↑ NHS. Sleep tips for teenagers. http://www.nhs.uk/Livewell/Childrenssleep/Pages/teensleeptips.aspx (accessed 19 Nov 2016).
- ↑ NHS. Sleep tips for teenagers. http://www.nhs.uk/Livewell/Childrenssleep/Pages/teensleeptips.aspx (accessed 19 Nov 2016).
- ↑ Brenner JS. Overuse injuries, overtraining, and burnout in child and adolescent athletes. Pediatrics. 2007 Jun 1;119(6):1242-5.
- ↑ Brenner JS. Overuse injuries, overtraining, and burnout in child and adolescent athletes. Pediatrics. 2007 Jun 1;119(6):1242-5.
- ↑ Brenner JS. Overuse injuries, overtraining, and burnout in child and adolescent athletes. Pediatrics. 2007 Jun 1;119(6):1242-5.
- ↑ The Natural Athletes Clinic. Overtraining Syndrome Symptoms, Signs, Testing and Treatment. Available from https://www.youtube.com/watch?v=dbdh6sY-f6s [last accessed 18/11/2021]
- ↑ Kreher JB, Schwartz JB. Overtraining syndrome a practical guide. Sports health: a multidisciplinary approach. 2012 Mar 1;4(2):128-38.
- ↑ Kreher JB. Diagnosis and prevention of overtraining syndrome: an opinion on education strategies. Open Access Journal of Sports Medicine. 2016;7:115.
- ↑ Kreher JB, Schwartz JB. Overtraining syndrome a practical guide. Sports health: a multidisciplinary approach. 2012 Mar 1;4(2):128-38.
- ↑ Kreher JB. Diagnosis and prevention of overtraining syndrome: an opinion on education strategies. Open Access Journal of Sports Medicine. 2016;7:115.
- ↑ Brenner JS. Overuse injuries, overtraining, and burnout in child and adolescent athletes. Pediatrics. 2007 Jun 1;119(6):1242-5.
- ↑ Kreher JB, Schwartz JB. Overtraining syndrome a practical guide. Sports health: a multidisciplinary approach. 2012 Mar 1;4(2):128-38.
- ↑ Kreher JB, Schwartz JB. Overtraining syndrome a practical guide. Sports health: a multidisciplinary approach. 2012 Mar 1;4(2):128-38.