Medical Complications in Spinal Cord Injury
Original Editor - George Prudden and Naomi O'Reilly
Top Contributors - Naomi O'Reilly, Kim Jackson, Admin, George Prudden, Tarina van der Stockt, Rucha Gadgil and Vidya Acharya
Introduction[edit | edit source]
Spinal cord injury results not only in motor and sensory deficits but also in autonomic dysfunctions as a result of the disruption between higher brain centers and the spinal cord. Autonomic dysfunction can include compromised cardiovascular, respiratory, urinary, gastrointestinal, thermoregulatory, and sexual activities. Maintaining optimal health and well-being after sustaining a spinal cord injury can be a challenge. Common secondary health conditions like pressure sores, spasms, chronic pain, and urinary tract infections often negatively affect quality of life and social participation. [1][2]
Autonomic Dysfunction[edit | edit source]
Autonomic dysfunction is common following a spinal cord injury, particularly in those with a lesion at mid-thoracic levels (T6) and above. During the acute phase of spinal cord injury the main forms of autonomic dysfunction present are neurogenic and spinal shock. Although frequently used interchangeably, true definitions of neurogenic and spinal shock are hard to identify with multiple definition used. Biering-Sørensen et al (2018) suggest that while the symptoms and signs of spinal shock and neurogenic shock may occur simultaneously, it should be noted that these are two distinctly different clinical conditions and should be treated as such. [3] While Autonomic Dysreflexia and thermoregulation dysfunction is more common in the sub-acute and chronic spinal cord injury.
Spinal Shock[edit | edit source]
Spinal shock, first described by Whytt in 1750, is a temporary loss of all neurological activity including motor, sensory and reflex activity below the level of the spinal cord lesion that can occur immediately following the onset of an acute spinal cord injury. Reflexes above the level of the spinal cord injury remain unaffected while those below the level of injury are either depressed (hyporeflexia) or absent (areflexia). The extent of disruption to reflexes is variable, both in terms of reflexes involved and timeframe for recovery, and as a result the precise definition and duration of spinal shock is debated. Appearance of bulbocavernosus reflex, normally within the first few days post injury, is seen by some clinicians as the end point for spinal shock, while others suggest it ends with the recovery of either deep tendon reflexes within a few weeks or much later with the recovery of bladder reflexes within 2 months of injury. [3][4]
Overall there is general agreement that spinal shock resolves in a series of stages lasting anywhere from a few days to a few months, with mean duration around 4 - 6 weeks. The following model consists of four evolving phases for in recovery from spinal shock with both clinical and physiological descriptions. [5]
| Phase | Timeframe | Clinical Description | Underlying Physiological Mechanism |
|---|---|---|---|
| 1 | 0 - 1 Day | Areflexia / Hyporeflexia with Flaccid Paralysis | Spinal Neuron Hyperpolarisation |
| 2 | 1 - 3 Days | Initial Reflex Return | Denervation Supersensitivity / Receptor Upregulation |
| 3 | 4 Days - 1 Month | Early Hypereflexia | Synapse Growth
Short Axons and/or Axon Supplied |
| 4 | 1 - 12 Months | Spasticity / Hypereflexia | Synapse Growth
Long Axons and Soma Supplied |
Gradual development of spasticity in those with an upper motor lesion is evident as spinal shock resolve, which may also be associated with neurophysiological and physical changes, and has important implications for physiotherapy management particularly in relation to contractures. [4][5]
Neurogenic Shock[edit | edit source]
Neurogenic shock, sometimes referred to as vasogenic shock, can occur after damage to the central nervous system, such as an acute spinal cord injury, typically in individuals with a lesion at T6 or above. [7][1][8] Reported incidence of neurogenic shock was 19.3% in cervical injuries, 7% in thoracic injuries and and 3% in lumbar injuries, typically occurring within 24 hours of injury and lasting from one to five weeks and commonly can occur simultaneously with spinal shock. [3][9]
Consequences of neurogenic shock are loss of sympathetic stimulation to the blood vessels and unopposed vagal activity leading to an imbalance of autonomic control, which can mimic or co-exist with Hypovolemic. This results in a haemodynamic triad of severe hypotension with systolic blood pressures of < 90 mmHg in supine position, bradycardia and peripheral vasodilation, which places an individual at risk for secondary neurological injury and pulmonary, renal, and cerebral insults leading to organ dysfunction and death if not promptly recognised and treated. [7][1]
Management of Neurogenic Shock[edit | edit source]
Restoration of intravascualar volume is the focus of initial treatment with the goal being to maintain Mean Arterial Pressure (MAP) at 85 to 90mmHg, followed by inotropic supports such as dopamine if symptoms of neurogenic shock do not resolve with initial volume resuscitation to maintain adequate spinal cord perfusion. [1][10][11]
Autonomic Dysreflexia[edit | edit source]
Autonomic dysreflexia, also referred to as autonomic hyperreflexia, is a potentially life-threatening condition that can affect people who have had a spinal cord injury at the level of T6 or above, and occurs more frequently in those with a complete injury over those with an incomplete injury, presenting more commonly during the chronic phase of spinal cord injury, around 3 - 6 months. Often unrecognised by many medical professionals, autonomic dysreflexia should be considered a medical emergency that requires immediate intervention. If not treated promptly and correctly, it can lead to significant complications, including stroke, seizures, myocardial ischaemia, and even death. [12][13]
It is an acute syndrome characterised by a sudden excessive increase in Systolic Blood Pressure triggered by an ascending sensory, usually "noxious” stimuli below the level of the lesion. Noxious stimuli can include bladder infection, urinary stasis, bowel obstruction, pressure on bony areas or pressure sores, improper positioning, tight clothing, catheter blockage, twisted intercostal drainage tubes, after sudden violent hip range of motion, and extreme hot weather with the most common causes resulting from bladder and bowel related problems. [13]
The noxious stimulus sends nerve impulses to the spinal cord, where they travel upward until they are blocked by the lesion at the level of the spinal cord injury. Since the impulses cannot reach the brain, a reflex is activated that increases the activity of the sympathetic portion of the autonomic nervous system. This results in severe vasoconstriction, which causes a sudden rise in blood pressure. Baroreceptors in the heart and blood vessels detect this rise in blood pressure and send a message to the brain. The brain sends a message to the heart, causing the heartbeat to slow down and the blood vessels above the level of injury to dilate. However, the brain cannot send messages below the level of injury, due to the spinal cord lesion, and therefore the blood pressure cannot be regulated. The brain is unable to check the sympathetic response resulting in increased systemic blood pressure. [12]
This overstimulation of the autonomic nervous system is characterised by sudden onset of severe high blood pressure known as paroxysmal hypertension at least 20 to 40 mmHg above normal resting systolic level. (It is important to remember that Blood Pressure for individuals with tetraplegia or high paraplegia is usually low, around 90 to 100/60 mmHg while lying down and possibly lower whilst sitting). This manifests itself with flushing of the skin, pounding headache, blurred vision, spots in visual field, irritability, pilo erection (goose bumps), profuse sweating above the level of the injury, dry and pale skin caused by vasoconstriction below the level of the injury, blurred vision, nasal congestion, bradycardia, cardiac arrhythmias, atrial fibrillation and often associated with anxiety and feelings of apprehension. Silent autonomic dysreflexia can also occur with minimal or no symptoms despite elevated blood pressure. [13][14][15]
Management of Autonomic Dysreflexia[edit | edit source]
A variety of non-pharmacological and pharmacological strategies can be used to treat autonomic dysreflexia. Immediate treatment recommends identification and removal of the triggering stimuli as soon as possible prior to pharmacological strategies since autonomic Dysreflexia tends to resolve once the inciting stimulus is removed. Sitting the individual upright and with legs over the bedside can reduce help to blood pressure levels and provide partial symptom relief. Tight clothing and stockings should be removed. Catheterization of the bladder, or relief of a blocked urinary catheter tube may resolve the problem. The rectum should be cleared of stool impaction, using anaesthetic lubricating jelly. If the noxious precipitating trigger cannot be identified, drug treatment is sometimes needed until further studies can identify the cause. When non-pharmacologic treatment methods are not successful in an acute episode of autonomic dysreflexia, pharmacologic agents are required and may include nifedipine, nitrates, and captopril. Only nifedipine has been supported by controlled trials. [14][13][16]
Thermoregulation[edit | edit source]
Thermoregulation is a process that allows your body to maintain its core internal temperature, with baseline temperature normally between 37°C (98°F) and 37.8°C (100°F). Thermoregulation mechanisms are designed to return your body to homeostasis and maintain a state of equilibrium. A sophisticated thermoregulatory center in the hypothalamus regulates thermogenesis by activating or inhibiting the sympathetic nervous system to maintain core body temperature. When your internal temperature changes, sensors in the central nervous system send messages to the hypothalamus. In response, it sends signals to various organs and systems in the body, which respond with a range of different mechanisms to either cool or heat the body. These mechanisms include: [1][19]
| Cooling Mechanisms | |
|---|---|
| Sweating | Sweat glands release sweat, which cools your skin through evaporation. |
| Vasodilation | Blood vessels under the skin dilate, which increases blood flow to the skin where it is cooler releasing heat through radiation. |
| Heating Mechanisms | |
|---|---|
| Vasoconstriction | Blood vessels under the skin constrict, which decreases blood flow to the skin, enabling heat retention. |
| Thermogenesis | Production of heat by the muscles, organs, and brain e.g. shivering, brown adipose tissue |
| Thyroid gland releases hormones to increase metabolism, which increases the energy your body creates and the amount of heat it produces. | |
Individuals with a spinal cord injury, particularly those with a cervical or high thoracic lesion, have impaired thermoregulation and are unable to respond appropriately to the changing temperatures of their surrounding environments. This is largely as a result of damage to the afferent and efferent pathways of the sympathetic nervous system causing reduced sensory input to the thermoregulatory center and loss of supra spinal control, which lead to dysregulation in vasomotor tone, skeletal muscle shivering and sweating dysfunction below the level of the spinal cord injury. [1][19]
Core temperature and body surface temperature receptors have an effect on body temperature regulation in individuals with a lesion at T7 or below, while the most severe dysfunction in body temperature regulation against external temperature change occurs in individuals with a lesion at T6 or above as their body temperature is controlled by Central Thermoreceptors. Poikilothermia, which is the inability to regulate core body temperature is common among individuals with a spinal cord injury and individuals with a lesion at T6 or above are prone to fluctuating temperature, hypothermia and hyperthermia, which are potentially fatal complications of exposure to environmental extremes. [19]
Cardiovascular Dysfunction[edit | edit source]
Many cardiovascular complications following a spinal cord injury occur as a result of damage to the autonomic nervous system and in individuals with cervical and high thoracic lesions may be life-threatening and may exacerbate the neurological impairment due to the spinal cord injury. In the acute phase many irregularities of the cardiac rhythm may occur including sinus bradycardia and bradyarrhythmias (14%-77%) such as escape rhythm, supraventricular ectopic beats (19%), ventricular ectopic beats (18%-27%), orthostatic hypotension (33%-74%), increased vasovagal reflex, vasodilatation and stasis, [1] while in the chronic phase of spinal cord injury common cardiovascular complications include orthostatic hypotension, autonomic dysreflexia, impaired cardiovascular reflexes, reduced transmission of cardiac pain, loss of reflex cardiac acceleration, cardiac atrophy with tetraplegia due to loss of left ventricular mass and pseudo-myocardial infarction. [2]
Deep Vein Thrombosis and Pulmonary Embolism[edit | edit source]
Deep vein thrombosis (DVT), which refers to the formation of one or more blood clots in one of the body’s large veins and subsequent Pulmonary Embolism (PE), which is blockage of an artery in the lungs by a substance that has moved from elsewhere in the body through the bloodstream (embolism), remains a significant cause of morbidity and mortality in individuals with spinal cord injuries and are particularly vulnerable during the first 2-3 weeks post the injury, followed by a small peak three months after the later. Incidences of deep vein thrombosis and pulmonary embolism are estimated to be 15% and 5%, respectively during the first year post-injury, while the incidence of clinically significant thromboembolism is less than 2% during the chronic stage. [1][2][20] A case report of an individual with acute SCI and COVID-19 showed an increased risk of deep vein thrombosis and pulmonary embolism due to COVID-19 coagulopathy, thus calling for more cautious screening and more aggressive management of individuals with SCI with a concurrent diagnosis of COVID-19.[21].
Thought to be caused by altered haemostasis with reduced fibrinolytic activity and increased factor VIII activity as a result of physical inactivity from paralysis, lack of movement and exacerbated by bedrest and reduced of vasomotor control in individuals with lesions involving the sympathetic nervous system, DVT’s tend to begin in the calf muscle. The signs and symptoms of DVT include;
- Low Grade Fever
- Localised swelling of the lower limb, usually unilateral
- Increased Leg Spasms
- Heat and Discolouration/Erythema of Skin
- Pain sometimes present in individuals with intact sensation
- Autonomic Dysreflexia if Lesion Above T6
Additionally the following signs and symptoms are more characteristic of a PE;
- Shortness of Breath
- Hypoxia
- Sweating
- Haemoptysis
- Tachycardia
- Confusion
- Chest Pain
- Loss of Consciousness
It was initially though there was an increased risk of dislodging a DVT during passive movement, although this is now disputed. If suspected or diagnosed, movement of the individual should be kept to a minimum and passive movements of the legs should cease until adequate therapeutic management with thrombolytic agents or low molecular weight heparin. Anticoagulation medication ,compression stockings, regularly screening, and early mobilisation as soon as feasible are routinely used to prevent DVT during the acute phase post injury. External pneumatic compression devices and electrical stimulation have also been advocated.[2][4][20]
Orthostatic Hypotension[edit | edit source]
Orthostatic Hypotension, also referred to as Postural Hypotension, is defined as a decrease in systolic blood pressure of 20 mmHg or more, or a reduction in diastolic blood pressure of 10 mmHg or more, when the body position changes from supine to upright, regardless of whether symptoms occur and occurs both during the acute and chronic stages of spinal cord injury. Reported prevalence is 21%, with greater prevalence in individuals with cervical and then high thoracic lesions above T6 secondary to a loss of supraspinal control of the sympathetic nervous system. It is exacerbated by poor venous return secondary to lower limb paralysis and the loss of the lower limb ‘muscle pump’, causing blood pooling in the legs and abdomen, resulting in a drop in blood pressure. Several other factors including low plasma volume, hyponatremia, and cardiovascular deconditioning due to prolonged bed-rest may also may predispose individuals with a spinal cord injury to orthostatic hypotension. [1][2][4][22]
Symptoms include dizziness, light headedness, headache, pallor, yawning, sweating, muscle weakness, fatigue and occasionally syncope and tend to be more pronounced when individuals first start to sit up and mobilize after injury, especially if there has been an extended period of prior bedrest and as such graduated gradual progressive daily head-up tilt is important. Over time individuals adjust and ‘acclimatize’ to the upright position and better tolerate the transition from lying to sitting, this is thought to be due to an increased tolerance to feelings of lightheadedness with lower blood pressure. [2][4][22]
Management of Orthostatic Hypotension[edit | edit source]
Management of orthostatic hypotension consists of both pharmacological and non-pharmacological treatments, although very few have been evaluated for use specifically in spinal cord injury. Immediate treatment is to lie the patient down and raise the feet or tilt the wheelchair backwards. Other management strategies include application of graduated compression stockings pressure stockings and abdominal binders, adequate hydration, and in some cases administration of pharmacological agents such as midodrine, although evidence of the effectiveness of these strategies is conflicting. [2][4][22]
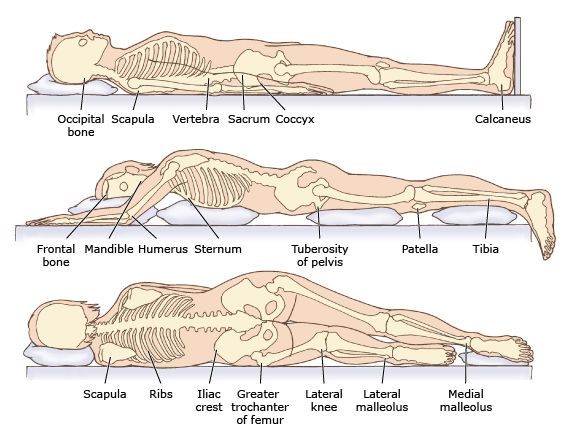
Pressure Sores[edit | edit source]
Individuals with a Spinal Cord injury are at high risk of developing pressure ulcers with an incidence of 25 - 66%, with higher level injuries more susceptible than those with a lower level injury. [23] The National Pressure Ulcer Advisory Panel, U.S (NPUAP) defines a pressure ulcer as an area of unrelieved pressure over a defined area, usually over a bony prominence, resulting in ischemia, cell death, and tissue necrosis. [24] A pressure ulcer is localized injury to the skin and/or underlying tissue usually over a bony prominence, as a result of pressure, or pressure in combination with shear. [25] A pressure sore can develop in a few hours, but the results can last for many months and even cause death. A number of contributing or confounding factors are associated with pressure ulcers; but the significance of these factors is yet to be elucidated. Tissue injury is related to both extrinsic and intrinsic factors. Extrinsic factors include pressure, shear, friction, immobility, and moisture, while Intrinsic factors relate to the condition of the patient, such as sepsis, local infection, decreased autonomic control, altered level of consciousness, increased age, vascular occlusive disease, anemia, malnutrition, sensory loss, spasticity, and contracture.[23]
Read more here about the prevention and management of Pressure Ulcers
Respiratory Dysfunction[edit | edit source]
Impaired respiratory function is common following a spinal cord injury. Respiratory function of people with is primarily determined by neurological level of the injury. Paralysis or partial paralysis of key muscles has a marked impact on respiratory function. Respiratory complications in spinal cord injury are common with complications directly correlated with mortality, and both are related to the level of neurologic injury. Pulmonary complications of spinal cord injury include the following: [1][2][4]
- Atelectasis secondary to decreased vital capacity and decreased functional residual capacity
- Ventilation-perfusion (V/Q) mismatch due to sympathectomy and/or adrenergic blockade
- Increased work of breathing secondary to decreased compliance
- Decreased cough, which increases the risk of retained secretions, atelectasis, pneumonia and respiratory infections
- Breathing Pattern Disorders e.g. Hypoventilation
- Muscle Paralysis
- Muscle Fatigue
Read more about Respiratory Management in Spinal Cord Injury
Gastrointestinal Dysfunction[edit | edit source]
Gastrointestinal dysfunction including constipation, straining, diarrhea, distention, abdominal pain, Urinary Incontinence, rectal bleeding, hemorrhoids, and autonomic dysreflexia during bowel movements occur in 27% to 62% of individuals with a spinal cord injury. During the acute stage of spinal cord injury there is an increased risk of gastrointestinal complications within the first few days post injury, including gastrointestinal hemorrhage, perforation, and paralytic ileus, while neurogenic bowel, affecting almost half of those with a spinal cord injury (46.9%) is a major problem long term both in terms of physical and psychological wellbeing. [1][2][27]
Paralytic Ileus[edit | edit source]
Paralytic Ileus, often associated with spinal shock post an acute spinal cord injury, is an obstruction of the intestine secondary to paralysis of the intestinal muscles with no evidence of mechanical obstruction, which like spinal shock can last from a few days to a few weeks. The paralysis does not need to be complete to cause ileus, but the intestinal muscles must be so inactive that it prevents the passage of food, and leads to a functional blockage of the intestine, which causes abdominal distension. A distended abdomen increases the work of breathing but also may cause vomiting, which increase the risk for aspiration pneumonia and further respiratory complications. Individuals with a paralytic ileus are typically managed Nil by Mouth (NPO) with nasogastric suction to regularly aspirate the stomach contents. [1][4][27]
Neurogenic Bowel[edit | edit source]
Neurogenic bowel dysfunction with changes to bowel motility, sphincter control, coupled with impaired mobility and hand dexterity, is a major physical and psychological problem for many individuals with a spinal cord injury, as well as major source of morbidity. Neurogenic bowel occurs secondary to a lack of central nervous control of the bowel resulting in dysfunction of the colon, with two distinct clinical presentations. [2][28]
Upper Motor Neuron (UMN) Bowel Syndrome, occurring in a spinal cord injury above the conus medullaris results in a hyperreflexic bowel, characterised by increased colonic wall and anal tones, with disrupted voluntary external anal sphincter control. Typically associated with constipation and fecal retention at least in part due to external anal sphincter activity. [2][28]
Lower Motor Neuron (LMN) Bowel Syndrome, occurring in a spinal cord injury at the injury at the conus medullaris or cauda equina results in an areflexic bowel, characterised by loss of spinal cord-mediated peristalsis and slow stool propulsion with an atonic external anal sphincter. Typically associated with constipation and a significant risk of incontinence due to flaccid paralysis of the external anal sphincter and reduced motor control of levator ani. [2][28]
The three main implications of disruption to motor, sensory and autonomic pathways post spinal cord injury on bowel function are an inability to:
- feel when the bowel is full
- voluntarily control muscles to defecate
- voluntarily contract muscles to prevent defecating
Management[edit | edit source]
Successful bowel management is multi-dimensional and needs to be specific to each individual requiring careful assessment for accurate diagnoses and prescription of treatments for bowel management following spinal cord injury, recognising that completeness of injury also has a significant impact on bowel function. Key strategies for bowel management include a high-fibre diet although further research to examine the optimal level, adequate fluid intake and a regular routine for bowel evacuation, which may incorporate digital stimulation or manual evacuation. Transanal irrigation is also now seen as a promising technique to reduce constipation and fecal incontinence. Prokinetic agents such as cisapride, prucalopride, metoclopramide, neostigmine, and fampridine are supported by strong evidence for the treatment of chronic constipation in individuals with a spinal cord injury in those where conservative management is not effective. [2][4][28]
| Bowel Management Options | Considerations for Appropriate Bowel Management Options |
|---|---|
| High Fibre Diet | Presence or Absence of Bowel Reflexes
Hand Function Patients’ Preference Other Complex Factors |
| Adequate Fluid Intake | |
| Regular Bowel Emptying Routine | |
| Digital Stimulation Bowel Reflexes | |
Medication
|
Read more about Bowel Management in Spinal Cord Injury
Urological Dysfunction[edit | edit source]
Urological dysfunction occurs in up to 80% of individuals with a spinal cord injury including urinary retention, urinary tract infection (UTI), upper and lower urinary tract deterioration, bladder or renal stones, incontinence, neurogenic bladder. During the acute stage of spinal cord injury there is an increased risk of urological complications secondary to spinal shock. The bladder becomes atonic, with no conscious awareness of bladder filling. The micturition reflex is interrupted and leads to urinary retention, which needs to be managed with clean intermittent catheterisation or with an indwelling catheter, while neurogenic bladder, is a major problem long term both in terms of physical and psychological wellbeing.[1][2][4]
Neurogenic Bladder[edit | edit source]
Neurogenic bladder dysfunction with changes to micturition, sphincter control, coupled with impaired mobility and hand dexterity, is a major physical and psychological problem for many individuals with a spinal cord injury. Neurogenic bladder, as with neurogenic bowel occurs secondary to a lack of central nervous control of the bladder with two distinct clinical presentations. [1][2][31]
Upper Motor Neuron Bladder occurring in a Suprasacral Lesion results in a reflex bladder, characterised by loss of cortical inhibition of sacral reflex arcs due to disturbance of descending spinal tracts, leading to detrusor hyperactivity often in combination with detrusor sphincter dyssynergia. Typically associated with recurrent, spontaneous voiding secondary to the detrusor hyperactivity with high voiding pressure and residual urine volume secondary to the Detrusor Sphincter Dyssynergia. [31][32]
Lower Motor Neuron Bladder occurring in a Sacral Lesion at S2 - S4 results in an areflexic bladder characterised by diminished motor stimulation of the bladder and reduced or absent contractility of the detrusor, meaning the bladder will not contract no matter how much it fills up.. Typically associated with bladder distension and Hydronephrosis, when an over-distended bladder causes a reflux of urine into the kidney. Overflow urinary incontinence and urinary tract infections are also not uncommon. [31][32]
Depending on the extent and location of nerve damage it is possible to have a mixed bladder pattern with elements of upper motor neuron and lower motor neuron bladder i.e. increased tone in external urethral sphincter as seen in UMN Bladders with detrusor hyporeflexia as seen in LMN Bladders or reduced sphincter tone with detrusor overactivity. [31][32]
Management[edit | edit source]
Management of neurogenic bladder dysfunction needs to be individualised according to the patient, the classification of their bladder dysfunction, and their symptoms with the overall goal of bladder management programs to develop predictable and effective patterns of elimination by emptying the bladder and preventing potential complications including urinary incontinence, urinary tract infections, detrusor overdistension, and progressive upper urinary tract damage due to chronic, excessive detrusor pressures.
Bladder training with patient education is an essential component of neurogenic bladder dysfunction management to ensure regular and adequate emptying of the bladder either with a voiding schedule, clean self intermittent catheterization, which is the preferred method of bladder emptying in spinal cord injury or indwelling catheterization i.e. suprapubic where they have difficulty with self-catheterization.
Pharmacological therapies may also be used for bladder management. Anticholinergic (Antimuscarinic) treatment is the first-line therapy for neurogenic detrusor overactivity, which works by blocking cholinergic transmission at muscarinic receptors and not only result in an increased bladder capacity, but reduced bladder pressure and delay the urge to void. [2][4][31]
Sexual Dysfunction[edit | edit source]
Sexual health is a significant component of an individuals overall health and wellbeing and this continues to be the case following a spinal cord injury, with 87% engaging in some form of sexual relationship post-injury. Sexual function can be affected by a spinal cord injury either directly or indirectly including the ability to engage in sexual activities; sexual intimacy and relationships; sexual self-view, and fertility and reproductive health. Associated physical sexual responses during sexual activity in both males and females are affected following a spinal cord injury dependent on the level and completeness of injury. Individuals with an upper motor neuron lesions retain reflexive but not psychogenic responses, while those with a lower motor neuron lesion lose reflexive but may retain psychogenic responses, while all retain some ability for non-genital sexual arousal. [4][35]
Erectile Dysfunction[edit | edit source]
Depending on the level and completeness of injury most men can attain an erection following a spinal cord injury through either the psychogenic pathway at T11- L2 or the reflexogenic pathway at S2-S4. However, these erections are often unreliable or inadequate for sexual intercourse with difficulties experienced in maintaining an erection. The use of Phosphodiesterase-5 Inhibitors (PDE-5I e.g. Viagra®, Cialis®) is the first line of management for erectile dysfunction in men with spinal cord injury and can be used safely, although up to 13% of men report adverse events occur including headache, flushing, hypotension, nasal congestion and dyspepsia. Intracavernosal injections of vasoactive medications such as papaverine and phentolamine may be used for those where PDE-5I are ineffective. [4][35]
Fertility[edit | edit source]
Although sperm production is usually normal, male fertility post a spinal cord injury may be affected secondary to impaired ejaculation and reduced sperm quality, which can result in complete infertility or impaired fertility. Symptoms and degree of infertility will vary depending on the type and severity of the spinal cord injury. Various techniques can be used for sperm retrieval including vibration and electro-ejaculation techniques, or microsurgical epididymis sperm aspiration or testicular sperm extraction where an individual is unable to ejaculate to obtain sperm for use with Intra-uterine Insemination (IUI) or In-vitro Fertilization (IVF).
Female fertility and menstruation are largely unchanged following spinal cord injury though women may briefly cease ovulating after an injury for between 1 - 3 months. Pregnancy for women with a spinal cord injury are associated with increased risks, particularly in those with spinal cord injuries at T6 or above. [4][35]
Bone Metabolism Dysfunction[edit | edit source]
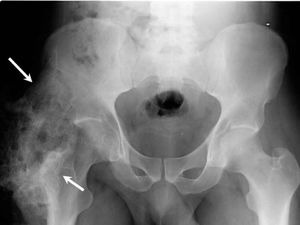
Heterotopic Ossification[edit | edit source]
Heterotopic ossification, also referred to as ectopic ossification and myositis ossificans, is the formation of pathological bone in muscle or soft tissue, which if severe can lead to ankylosis and impaired function. It usually presents around the joint, predominantly in the hip, with the first signs including swelling around the joint, reduced range of motion, with or without fever, spasticity and pain, which are similar clinical signs to those of fracture and deep venous thrombosis. Ultrasound, CT Scan or Bone Scan are used to provide a definitive diagnosis of heterotopic ossification, although blood tests may also give some indication.[4] In spinal cord injury the incidence has been reported between 10% - 78%, occurring most commonly below the level of the lesion in the hip joint and first noted during the first two months following injury, but can occur many years post injury. It is suggested that males and individuals with a complete spinal cord injury (AIS A) are at increased risk, as are individuals with high thoracic and cervical level injuries, although both gender and injury severity as risk factors have been disputed in the literature. Other factors including spasticity, pneumonia, thoracic trauma, tracheostomy, nicotine use, and urinary tract infection increase patients’ risk for heterotopic ossification with evaluation for these factors, in combination with early intervention and diagnosis, likely to reduce incidence or improve a patient’s recovery post-operatively. [2][36]
In spinal cord injury it appears to be initiated by metaplasia of mesenchymal cells in the peri articular hematoma and micro-hematoma into bone precursor cells but the mechanism is not yet fully understood, which creates a challenge in early diagnostic and therapeutic interventions. [37] It has been observed that repeated and aggressive passive movements of immobilized joints in animals led to development of heterotopic ossification and as a result has been suggested that physiotherapy may increase the risk, although a causal relationship between physiotherapy and heterotopic ossification has not been demonstrated in the research, but as such aggressive manual therapy interventions are not encouraged. There is some evidence though, albeit low quality, to suggest that gentle passive movements maintain range of motion during the acute inflammatory stage of heterotrophic ossification. [2][4][36] Pharmacological management, including non-steroidal anti-inflammatory and Warfarin, is the main treatment for heterotopic ossification with varying degrees of success. Occasionally, excessive bone can be removed surgically but this is not without risk and can exacerbate the condition, and as a result is generally only performed once heterotopic ossification has stabilized, typically 1-2 years after onset, and primarily in situations where function and quality of life are adversely affected. [4][36]
Read more here about the prevention and management of Heterotopic Ossification
Osteoporosis[edit | edit source]
Osteoporosis, meaning porous bone, is a disease characterized by a decrease in bone density, both mass and quality. It is a disorder in which bones become increasingly porous and brittle, leading to increased risk of fracture. [38] Osteoporosis is a common long-term complication of spinal cord injury, primarily thought to be due to the lack of weight bearing and axial loading, with a 25 - 50% reduction in bone mineral content of the lower limbs over a lifetime, with most bone mineral loss is in the first year following injury. The mechanism involved in the development of spinal cord injured-induced osteoporosis is complex and multifactorial. Disuse may play an important role in the pathogenesis of osteoporosis but non-mechanical factors also appear to be important, which may include insufficient nutritional support, disordered vasoregulation, hypercortisolism, alterations in gonadal function and other endocrine disorders. [2][4][39]
There is a significant risk for fragility fractures, in particular low impact fracture, following a spinal cord, with further increased risk for women, motor complete injuries (AIS A and B), longer duration of injury, and with use of benzodiazepines, heparin, or opioid analgesia. The most common fracture sites appear to be those around the knee, such as the distal femur or proximal tibia. Although their effectiveness is yet to be clearly demonstrated, early standing, weight-bearing and electrical stimulation programmes have been advocated but pharmacological management, focused on reversing bone resorption, including use of bisphosphonates is the main treatment. Early assessment and ongoing monitoring of bone health are essential elements of spinal cord injury care. [2][4][39]
Read more here about the management of Osteoporosis.
Spasticity[edit | edit source]
Spasticity is a motor disorder characterized by a velocity-dependent increase in tonic stretch reflexes (muscle tone) with exaggerated tendon jerks, resulting from hyper-excitability of the stretch reflex, as one component of the upper motor neuron syndrome [40], or more recently defined as disordered sensorimotor control, resulting from an upper motor neuron lesion, presenting as an intermittent or sustained involuntary activations of muscles. [41] Present in up to 80% of individuals with a spinal cord injury, characterized by hypertonus, increased intermittent or sustained involuntary somatic reflexes (hyperreflexia), clonus and painful muscle spasms, it can cause significant impairment for many individuals and may contribute to increased functional impairment, contractures, pressure ulcers, posture disorders and pain. [1][2][4]
Many factors or stimuli can elicit spasticity with stretch and touch being the most common, with acute increases often indicative of illness or injury, or an over-distended bladder or bowel.
Management[edit | edit source]
Management options for spasticity involve the elimination of exacerbating factors (such as urinary tract infection, constipation, pressure ulcers, etc.), and pharmacological agents, which act either on the central nervous system (e.g. baclofen, diazepam, gabapentin, clonidine, tizanidine) or the peripheral nervous system, either within the muscle or at the neuromuscular junction (e.g. dantrolene and Botulinum Toxin). Intrathecal administration of medication directly to the spinal cord may be utilized in individuals with more severe spasticity. Transient relief from spasticity may be provided with physiotherapy interventions such as hydrotherapy, stretch, heat, cold, TENS, electrical stimulation, therapeutic exercise techniques, passive movements, standing and vibration, but there is no evidence that any of these interventions produce lasting reductions in spasticity. [1][2][4]
Read more here about the management of Spasticity.
Pain[edit | edit source]
Up to 80% of individuals with a spinal cord injury report chronic pain, which pain may lead to functional impairment and reduced community participation and quality of life. The most widely accepted and current definition of pain, established by the International Association for the Study of Pain (IASP), is "An unpleasant sensory and emotional experience associated with, or resembling that associated with, actual or potential tissue damage.[42]" Although several theoretical frameworks have been proposed to explain the physiological basis of pain, not one theory has been able to exclusively incorporate the entirety of all the aspects of pain perception. [43][44]
There are many different types of pain that occur in association with spinal cord injury, and the characteristics, patterns of presentation, intensity and location are highly variable. When classifying pain specifically in a spinal cord injury the IASP has proposed a taxonomy of pain divided into two main groups: Nociceptive (Musculoskeletal or Visceral) and Neuropathic (either above the level, at the level or below the level of injury). While our understanding of the underlying causes of neuropathic and nociceptive pain in individuals with a spinal cord injury is limited, there is some evidence to suggest that changes within the central nervous system lead to a heightened sensitivity (or neuronal excitability) and it is this that contributes to the development of pain. [2][4][43][44]
Read more here about the management of Pain.
Nociceptive[edit | edit source]
Nociceptive pain is associated with the activation of peripheral receptive terminals of primary afferent neurons in response to noxious chemical (inflammatory), mechanical or ischemic stimuli. Abnormal posture, gait and overuse of structures such as the arm and shoulder for transfers and wheelchair propulsion result in chronic overuse injuries and musculoskeletal pain, a type of nociceptive pain. Muscle spasm pain is another type of musculoskeletal pain that is more commonly seen in individuals with an incomplete spinal cord injury. Visceral pain, while less common, arises from damage, irritation or distention of internal organs such as the bladder or bowel. [2][4][44][45]
Neuropathic[edit | edit source]
Central neuropathic pain is pain is initiated by a primary lesion or dysfunction in the Central Nervous System (CNS), while peripheral neuropathic pain is initiated or caused by a primary lesion or dysfunction in the Peripheral Nervous System (PNS) and involves numerous pathophysiological mechanisms associated with altered nerve functioning and responsiveness.
In a spinal cord injury neuropathic pain can occur above the level of the injury arising from complex regional pain syndromes and compressive mononeuropathies; at the level of the injury due to central pain secondary to damage to either nerve roots or the spinal cord or below the level of the injury as central dysesthesia syndrome or deafferentation pain characterized by burning, aching, tingling or stabbing sensation.
Spinal cord neuropathic pain is a complex management challenge: frequently the long-term prognosis is poor, and can significantly impair functioning, increase disability and reduce quality of life; and it may be very difficult to achieve adequate pain control. Currently treatment options include, include both pharmacologic (Pregabalin, Gabapentin and Amitriptyline) and non-pharmacologic (Transcranial Direct Current Stimulation, Transcutaneous Electrical Nerve Stimulation) approaches, which target pathophysiologic changes at peripheral, spinal and cerebral levels. [2][4][44][45]
Read more here about Pain Mechanisms
Psychological[edit | edit source]
Spinal cord injury can have a negative impact on mental health and many individuals experience psychological stress and/or psychosocial distress which injury, which for a minority continues after transitioning from rehabilitation back into the community. Recent evidence suggests that the prevalence of depression after a spinal cord injury is between 18.6% to 26.7%, [46] which is substantially greater than that in the general medical population and as such to prevent or minimize the impact of psychological problems physical, pharmacological or psychological interventions should be available both during treatment and long term. [1][4]
Read more here about Psychosocial Considerations in Spinal Cord Injury
References[edit | edit source]
- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 1.16 Hagen EM. Acute Complications of Spinal Cord Injuries. World Journal of Orthopedics. 2015 Jan 18;6(1):17.
- ↑ 2.00 2.01 2.02 2.03 2.04 2.05 2.06 2.07 2.08 2.09 2.10 2.11 2.12 2.13 2.14 2.15 2.16 2.17 2.18 2.19 2.20 2.21 2.22 2.23 2.24 Sezer N, Akkuş S, Uğurlu FG. Chronic Complications of Spinal Cord Injury. World Journal of Orthopedics. 2015 Jan 18;6(1):24.
- ↑ 3.0 3.1 3.2 Biering-Sørensen F, Biering-Sørensen T, Liu N, Malmqvist L, Wecht JM, Krassioukov A. Alterations in Cardiac Autonomic Control in Spinal Cord Injury. Autonomic Neuroscience. 2018 Jan 1;209:4-18.
- ↑ 4.00 4.01 4.02 4.03 4.04 4.05 4.06 4.07 4.08 4.09 4.10 4.11 4.12 4.13 4.14 4.15 4.16 4.17 4.18 4.19 4.20 4.21 4.22 4.23 4.24 Harvey L. Management of Spinal Cord Injuries: A Guide for Physiotherapists. Elsevier Health Sciences; 2008 Jan 10.
- ↑ 5.0 5.1 Ditunno JF, Little JW, Tessler A, Burns AS. Spinal Shock Revisited: A Four-Phase Model. Spinal Cord. 2004 Jul;42(7):383.
- ↑ New Zealand Spinal Trust. Spinal 101 - Spinal Shock. Available from: http://vimeo.com/230390246[last accessed 30/10/87]
- ↑ 7.0 7.1 Krassioukov A, Claydon VE. The Clinical Problems in Cardiovascular Control following Spinal Cord Injury: An Overview. Prog Brain Res. 2006;152:223–229. [PubMed]
- ↑ Ahuja CS, Cadotte DW, Fehlings M. Chapter 33 Spinal Cord Injury. In Principles of Neurological Surgery (Fourth Edition) 2018 (pp. 518-531).
- ↑ Guly HR, Bouamra O, Lecky FE. The Incidence of Neurogenic Shock in Patients with Isolated Spinal Cord Injury in the Emergency Department. Resuscitation. 2008;76:57–62. [PubMed]
- ↑ Koffi M. Kla, Lorri A. Lee. Perioperative Anesthetic and ICU Considerations for Spinal Surgery. In Neurocritical Care Management of the Neurosurgical Patient, 2018
- ↑ Shank CD, Walters BC, Hadley MN. Management of Acute Traumatic Spinal Cord Injuries. In Handbook of Clinical Neurology 2017 Jan 1 (Vol. 140, pp. 275-298). Elsevier.
- ↑ 12.0 12.1 Eldahan KC, Rabchevsky AG. Autonomic Dysreflexia after Spinal Cord Injury: Systemic Pathophysiology and methods of management. Autonomic Neuroscience. 2018 Jan 1;209:59-70.
- ↑ 13.0 13.1 13.2 13.3 Krassioukov A, Warburton DE, Teasell R, Eng JJ, Spinal Cord Injury Rehabilitation Evidence Research Team. A Systematic Review of the Management of Autonomic Dysreflexia after Spinal Cord Injury. Archives of physical Medicine and Rehabilitation. 2009 Apr 1;90(4):682-95.
- ↑ 14.0 14.1 Khastgir J, Drake MJ, Abrams P. Recognition and Effective Management of Autonomic Dysreflexia in Spinal Cord Injuries. Expert Opinion on Pharmacotherapy. 2007 May;8(7):945–56.
- ↑ Consortium for Spinal Cord Injury Medicine. Acute Management of Autonomic Dysreflexia: Individuals with Spinal Cord Injury Presenting to Health Care Facilities. Journal Spinal Cord Med. 2002 Spring; 25 Suppl 1:S67-88.
- ↑ Squair JW, Phillips AA, Harmon M, Krassioukov AV. Emergency Management of Autonomic Dysreflexia with Neurologic Complications. Canadian Medical Association Journal. 2016 Oct 18;188(15):1100-3.
- ↑ Craig Hospital. What is Autonomic Dysreflexia?. Available from: https://youtu.be/3TiYphQVPpU[last accessed 03/03/22]
- ↑ Rick Hansen Institute. Best Practices - Diagnosis and Management of Autonomic Dysreflexia. Available from: https://youtu.be/iau-G2DHVtA[last accessed 30/10/18]
- ↑ 19.0 19.1 19.2 Song YG, Won YH, Park SH, Ko MH, Seo JH. Changes in Body Temperature in Incomplete Spinal Cord Injury by Digital Infrared Thermographic Imaging. Annals of Rehabilitation Medicine. 2015 Oct 1;39(5):696-704.
- ↑ 20.0 20.1 Alibrahim F, McIntyre A, Hsieh JTC, Loh E, Teasell RW, Eng JJ. Venous Thromboembolism Following Spinal Cord Injury. In Eng JJ, Teasell RW, Miller WC, Wolfe DL, Townson AF, Hsieh JTC, Connolly SJ, Noonan VK, Loh E, McIntyre A, editors. Spinal Cord Injury Rehabilitation Evidence. 2016 Version 5.0: p 1-34.
- ↑ Pisano TJ, Joki J, Hon B, Cuccurullo S. Pulmonary Embolism After Acute Spinal Cord Injury and COVID-19. American Journal of Physical Medicine & Rehabilitation. 2020 Nov 1;99(11):982-5.
- ↑ 22.0 22.1 22.2 Krassioukov A, Wecht JM, Teasell RW, Eng JJ. Orthostatic Hypotension Following Spinal Cord Injury. Spinal Cord Injury Rehabilitation Evidence. 2014 Version 5.0. Vancouver: p 1- 26.
- ↑ 23.0 23.1 Kruger EA, Pires M, Ngann Y, Sterling M, Rubayi S. Comprehensive Management of Pressure Ulcers in Spinal Cord Injury: Current Concepts and Future Trends. The Journal of Spinal Cord Medicine. 2013 Nov 1;36(6):572-85.
- ↑ http://emedicine.medscape.com/article/190115-overview
- ↑ https://www.templateroller.com/template/2108688/npuap-pressure-ulcer-stages-categories.html
- ↑ HealthyTomorrow. Skin Breakdown and Pressure Ulcer Prevention in Persons with SCI. Available from: https://youtu.be/b7utewKDqC0[last accessed 03/03/22]
- ↑ 27.0 27.1 Ebert E. Gastrointestinal Involvement in Spinal Cord Injury: A Clinical Perspective. Journal of Gastrointestinal & Liver Diseases. 2012 Mar 1;21(1).
- ↑ 28.0 28.1 28.2 28.3 Krassioukov A, Eng JJ, Claxton G, Sakakibara BM, Shum S. Neurogenic Bowel Management after Spinal Cord Injury: A Systematic Review of the Evidence. Spinal Cord. 2010 Oct;48(10):718.
- ↑ SCIUcourses. Bowel 1.3 - Neurogenic Bowel. Available from: https://youtu.be/AYQo1R-sFHk[last accessed 30/10/18]
- ↑ SCIUcourses. Bowel 2.1 - The Perfect Program. Available from: https://youtu.be/2K7DByoxias[last accessed 30/10/18]
- ↑ 31.0 31.1 31.2 31.3 31.4 Al Taweel W, Seyam R. Neurogenic Bladder in Spinal Cord Injury Patients. Research and Reports in Urology. 2015;7:85.
- ↑ 32.0 32.1 32.2 Dorsher PT, McIntosh PM. Neurogenic Bladder. Advances in Urology. 2012;2012.
- ↑ SCIUcourses. Bladder 1.3 - Neurogenic Bladder. Available from: https://youtu.be/AVYFkgyZv-8[last accessed 30/10/18]
- ↑ SCIUcourses. Bladder 2.2 - Emptying Your Bladder. Available from: https://youtu.be/wR1vJmrZPP8[last accessed 30/10/18]
- ↑ 35.0 35.1 35.2 Trofimenko V, Hotaling JM. Fertility Treatment in Spinal Cord injury and other Neurologic Disease. Translational Andrology and Urology. 2016 Feb;5(1):102.
- ↑ 36.0 36.1 36.2 Alibrahim F, McIntyre A, Serrato J, Mehta S, Loh E, Teasell RW . Heterotopic Ossification Following Spinal Cord Injury. In Eng JJ, Teasell RW, Miller WC, Wolfe DL, Townson AF, Hsieh JTC, Connolly SJ, Noonan VK, Loh E, McIntyre A, editors. Spinal Cord Injury Rehabilitation Evidence. 2016 Version 6.0: p 1-20.
- ↑ Schuetz P, Mueller B, Christ-Crain M, Dick W, Haas H. Amino-biphosphonates in Heterotopic Ossification: First Experience in Five Consecutive Cases. Spinal Cord. 2005;43:604-10.
- ↑ Johnell O and Kanis JA (2006) An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int 17:1726.
- ↑ 39.0 39.1 Craven C, Lynch CL, Eng JJ. Bone Health Following Spinal Cord Injury. In Eng JJ, Teasell RW, Miller WC, Wolfe DL, Townson AF, Hsieh JTC, Connolly SJ, Noonan VK, Loh E, McIntyre A, editors. Spinal Cord Injury Rehabilitation Evidence. 2014 Version 5.0. Vancouver: p 1- 37.
- ↑ Lance JW. Symposium Synopsis. In: Feldman RG,fckLRYoung RR, Koella WP (eds). Spasticity: Disordered Motor Control. Chicago, IL: Year Book 1980:485–94.
- ↑ Pandyan AD, Gregoric M, Barnes MP et al. Spasticity: Clinical Perceptions, Neurological Realities and Meaningful Measurement. Disabil Rehabil 2005;27:2–6.
- ↑ International Association for the Study of Pain. IASP Terminology. Available from: https://www.iasp-pain.org/Education/Content.aspx?ItemNumber=1698. [Accessed 19 July 2020]
- ↑ 43.0 43.1 Moayedi M, Davis KD. Theories of Pain: From Specificity to Gate Control. J Neurophysiol 2013;109:5-12.
- ↑ 44.0 44.1 44.2 44.3 Smart KM, Blake C, Staines A, Doody C. Clinical Indicators of 'Nociceptive', 'Peripheral Neuropathic' and 'Central' Mechanisms of Musculoskeletal Pain. A Delphi Survey of Expert Clinicians. Man Ther 2010;15:80-7
- ↑ 45.0 45.1 Guy SD, Mehta S, Casalino A, Côté I, Kras-Dupuis A, Moulin DE, Parrent AG, Potter P, Short C, Teasell R, Bradbury CL. The CanPain SCI Clinical Practice Guidelines for Rehabilitation Management of Neuropathic Pain after Spinal Cord: Recommendations for Treatment. Spinal Cord. 2016 Jul 22;54(S1):S14.
- ↑ Williams R, Murray A. Prevalence of Depression after Spinal Cord Injury: A Meta-analysis. Archives of Physical Medicine and Rehabilitation. 2015 Jan 1;96(1):133-40.